Spinal fusion and Vitamin D - several studies
5+ VitaminDWiki pages have both SPINAL and FUSION in the title
This list is automatically updated
{LIST()}
Spinal Fusion 2.5 X more likely if low vitamin D – meta-analysis June 2024
Risk factors affecting spinal fusion: A meta-analysis of 39 cohort studies
PLoS One. 2024 Jun 7;19(6):e0304473. doi: 10.1371/journal.pone.0304473. eCollection 2024.
Shudong Yang 1, Beijun Zhou 2, Jiaxuan Mo 2, Ruidi He 2, Kunbo Mei 2, Zhi Zeng 2, Gaigai Yang 2, Yuwei Chen 2, Mingjiang Luo 3, Siliang Tang 4, Zhihong Xiao 3
Purpose: We performed a meta-analysis to identify risk factors affecting spinal fusion.
Methods: We systematically searched PubMed, Embase, and the Cochrane Library from inception to January 6, 2023, for articles that report risk factors affecting spinal fusion. The pooled odds ratios (ORs) and 95% confidence intervals (CIs) were estimated using fixed-effects models for each factor for which the interstudy heterogeneity I2 was < 50%, while random-effects models were used when the interstudy heterogeneity I2 was ≥ 50%. Using sample size, Egger's P value, and heterogeneity across studies as criteria, we categorized the quality of evidence from observational studies as high-quality (Class I), moderate-quality (Class II or III), or low-quality (Class IV). Furthermore, the trim-and-fill procedure and leave-one-out protocol were conducted to investigate potential sources of heterogeneity and verify result stability.
Results: Of the 1,257 citations screened, 39 unique cohort studies comprising 7,145 patients were included in the data synthesis.
High-quality (Class I) evidence showed that patients with a
smoking habit (OR, 1.57; 95% CI, 1.11 to 2.21) and
without the use of bone morphogenetic protein-2 (BMP-2) (OR, 4.42; 95% CI, 3.33 to 5.86)
were at higher risk for fusion failure.
Moderate-quality (Class II or III) evidence showed that fusion failure was significantly associated with
vitamin D deficiency (OR, 2.46; 95% CI, 1.24 to 4.90),
diabetes (OR, 3.42; 95% CI, 1.59 to 7.36),
allograft (OR, 1.82; 95% CI, 1.11 to 2.96),
conventional pedicle screw (CPS) fixation (OR, 4.77; 95% CI, 2.23 to 10.20) and
posterolateral fusion (OR, 3.63; 95% CI, 1.25 to 10.49).
Conclusions: Conspicuous risk factors affecting spinal fusion include three patient-related risk factors (smoking, vitamin D deficiency, and diabetes) and four surgery-related risk factors (without the use of BMP-2, allograft, CPS fixation, and posterolateral fusion). These findings may help clinicians strengthen awareness for early intervention in patients at high risk of developing fusion failure.
📄 Download the PDF from VitaminDWiki
After Spinal Fusion 800 IU of Vitamin D helped some, more was needed - Nov 2022 RCT
The efficacy of oral vitamin D supplements on fusion outcome in patients receiving elective lumbar spinal fusion—a randomized control trial
Hu et al. BMC Musculoskeletal Disorders (2022) 23:996 https://doi.org/10.1186/s12891-022-05948-9
Ming-Hsien Hu, Yu-Kai Tseng, Yu-Hsuan Chung, Nai-Yuan Wu, Chi-Huan Li & Pei-Yuan Lee
Background
Previous studies have reported that vitamin D supplement could improve fracture healing, but evidence regarding the role of vitamin D supplements in spinal fusion was limited. Thus, this study aimed to evaluate the effectiveness of oral vitamin D supplements on fusion outcomes in patients undergoing lumbar spinal fusion.
Methods
This randomized, double-blind, parallel-designed, active-control trial included the patients who planned for elective lumbar spinal fusion. Eligible patients were randomly assigned to receive either daily vitamin D3 (cholecalciferol) 800 IU and daily calcium citrate 600 mg (experimental group) or only daily calcium citrate 600 mg (control group). All supplements were given from postoperative day 1 and lasted for 3 months. Primary outcome was postoperative 1-year fusion rate, and secondary outcomes included time to fusion, Oswestry Disability Index (ODI), and visual analogue scale (VAS) for pain.
Results
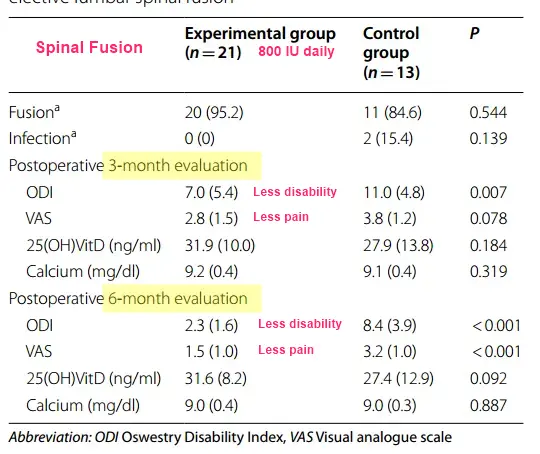
Among the included 34 patients (21 in the experimental group and 13 in the control group), baseline 25-hydroxyvitamin D (25[OHVitD) level was 26.7 (10.4) ng/ml. Preoperative prevalence of vitamin D deficiency and insufficiency were 23.5% and 47.1%, respectively. Postoperative 1-year fusion rate was not significantly different between the two groups (95.2% vs. 84.6%, P = 0.544). The experimental group had significantly shorter time to fusion (Kaplan–Meier estimated: 169 days vs. 185 days [interquartile range: 88–182 days vs. 176–324 days], log-rank test: P = 0.028), lower postoperative 6-month ODI (P < 0.001), and lower postoperative 6-month VAS (P < 0.001) than the control group. Time to fusion was significantly and negatively correlated with preoperative, postoperative 3-month, and 6-month 25(OH)VitD levels (all P < 0.01).
Conclusion
The patient with vitamin D supplements had shorter time to fusion, better spinal function and less pain after elective spinal fusion. Further research is warranted to identify the patients who can benefit the most from vitamin D supplements and the appropriate dose of vitamin D supplements.
Trial registration
ClinicalTrials.gov, NCT05023122. Registered 20 August 2021. Retrospectively registered, http://clinicaltrials.gov/ct2/show/NCT03793530.
📄 Download the PDF from VitaminDWiki
Anticipate much more benefit if use 4,000 IU daily and start 3 months before surgery
Alternately, use 50,000 IU once every 2 weeks and still start 3 months before surgery
