Prostate cancer risk increase with Vitamin D (other studies disagree) – meta-analysis
Circulating vitamin D concentration and risk of prostate cancer: a dose–response meta-analysis of prospective studies
Therapeutics and Clinical Risk Management, 9 January 2018 Vol 2018:14 Pages 95—104, DOI https://doi.org/10.2147/TCRM.S149325
Gao JL, Wei W, Wang G, Zhou HL, Fu YW, Liu N
Department of Urology, The First Hospital of Jilin University, Changchun, People’s Republic of China
📄 Download the PDF from VitaminDWiki
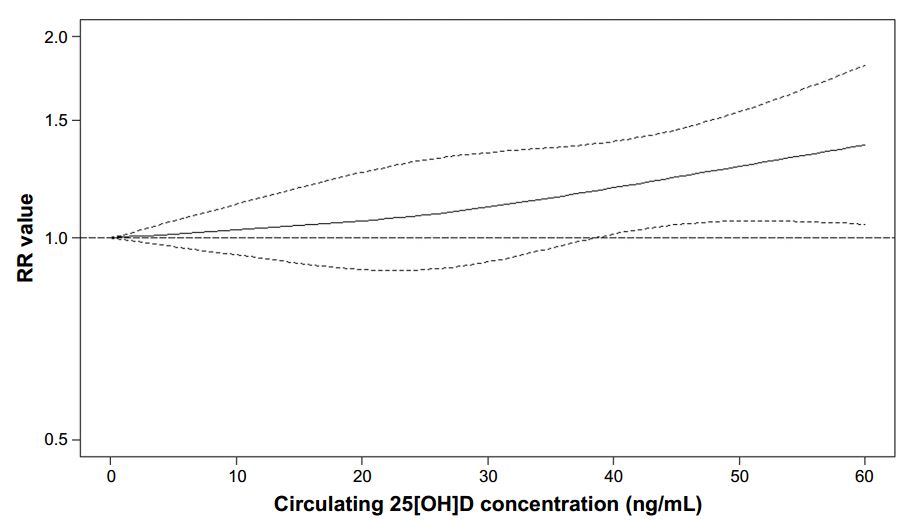
Risk for all studies (not adjusted for excess Calcium)
Background: Though many studies have been performed to elucidate the association between circulating vitamin D and prostate cancer, no conclusive result is available. We carried out a dose–response meta-analysis to quantitatively examine the association of circulating 25-hydroxyvitamin D (25[OH]D) concentration with prostate cancer.
Methods: Only prospective studies examining the associations of circulating 25[OH]D concentration with prostate cancer were eligible for the meta-analysis. A random-effect meta-analysis was done first, to calculate the summary relative risk (RR) and 95% confidence intervals (CIs) comparing the higher concentration with the lower concentration of 25[OH]D. A dose–response meta-analysis using random-effects model was then carried out to evaluate the nonlinearity and calculate the summary RR caused per 10 ng/mL increment.
Results: Nineteen prospective cohort or nested case–control studies were included. Higher 25[OH]D concentration was significantly correlated with elevated risk of prostate cancer (RR =1.15, 95% CI 1.06–1.24). No nonlinear relationship was found between 25[OH]D concentration and risk of prostate cancer (P=0.654). Dose–response meta-analysis showed that the summary RR caused per 10 ng/mL increment in circulating 25[OH]D concentration was 1.04 (95% CI 1.02–1.06). Subgroup analysis also found a modest dose–response relationship. Funnel plot and Egger’s test did not detect publication bias.
Conclusion: The findings suggest that highest 25[OH]D concentration is correlated with elevated risk of prostate cancer and a modest dose–response effect exists in this association; however, more studies are needed.
