Lung and Vitamin D – Special Issue
Current Respiratory Medicine Reviews; Volume 7, Number 6, December 2011
(Thanks to Vitamin D Council for pointing out this issue)
Editorial from Guest Editor - Hot Topic:Vitamin D and Respiratory Health Pp.394-395
Adrian R. Martineau - Editorial from Guest Editor Vitamin D and Respiratory Health
Adrian R. Martineau'1'2
'Queen Mary University of London, Barts and The London School of Medicine and, Dentistry, Blizard Institute, London E1 2AB, UK
2Division of Mycobacterial Research, National Institute of Medical Research, Mill Hill, NW7 1AA, UK
This Hot Topic edition of Current Respiratory Medicine Reviews considers the literature suggesting that vitamin D status is a key determinant of respiratory health.
At first sight' the proposition that deficiency of a single micronutrient could be implicated in the pathogenesis of conditions as diverse as asthma' allergy' respiratory infection and lung cancer may seem biologically implausible . However' a large and growing body of evidence from both the laboratory and the clinic suggests that associations between vitamin D deficiency and susceptibility to these conditions may well be causal.
Humans acquire vitamin D via cutaneous synthesis as a result of the action of solar ultraviolet B radiation on 7-dehydrocholesterol in the skin' or from the diet' principally by consumption of oily fish or dietary supplements. Vitamin D from either source is metabolised by the liver to form 25-hydroxyvitamin D (25[OH]D), the major circulating vitamin D metabolite whose serum concentration defines vitamin D status. 25(OH)D is metabolised by the enzyme 25(OH)D-1oc-hydroxylase (CYP27B1) to form 1'25-dihydroxyvitamin D (1'25[OH]2D)' the steroid hormone and active metabolite of vitamin D. 1'25(OH)2D induces biological actions by ligating vitamin D receptor (VDR)' which acts as a transcription factor' regulating the expression of vitamin D-responsive genes [1].
The clinical features of vitamin D deficiency were first described in 1651 , when Glisson, Bate and Regemorter published 'A treatise of the rickets: being a disease common to children' [2]. For many years, bone disease was regarded as the only clinical manifestation of inadequate vitamin D status; CYP27B1 was thought to be expressed predominantly in the kidney and 1,25(OH)2D was regarded primarily as a hormone of calcium homeostasis. This perception changed in 1981, when Barbour and colleagues reported a case of hypercalcaemia in an anephric patient with sarcoidosis who was found to have an elevated serum 1,25(OH)2D concentration [3]; this observation provided the first evidence that 1-alpha hydroxylation of 25(OH)D could occur extra-renally. CYP27B1 activity has subsequently been demonstrated in macrophages [4], dendritic cells [5], lymphocytes [5] and pulmonary epithelial cells [6]. In the same year, Abe and colleagues reported expression of VDR in a murine myeloid leukaemia cell line [7], raising the possibility that vitamin D might possess immunomodulatory activity. VDR has subsequently been shown to be expressed in human monocytes, macrophages, B and T lymphocytes [8], in dendritic cells [9] and in both normal and malignant lung tissue [10]; moreover, 1,25(OH)2D has been shown to exert antimicrobial, anti-inflammatory and anti-proliferative actions on these cells in vitro [11]. Taken together, these observations indicate that 1,25(OH)2D3 can be synthesised by, and can exert biological activity in, many cell populations in the lung.
The articles presented here encompass the effects of vitamin D status on respiratory health throughout the lifespan.
Steven Goldring, John Warner, Seif Shaheen and Robert Boyle open with a review of the clinical evidence linking antenatal vitamin D status with subsequent risk of asthma and atopy.
Virender Rehan and John Torday proceed to enlarge on the molecular mechanisms by which perinatal vitamin D deficiency may contribute to asthma pathogenesis in the developing lung, before
Graham Devereux and James Wagner discuss insights into the actions of vitamin D provided by animal models and consider the evidence that vitamin D status may influence incidence and severity of asthma in children and adults.
Abigail Jackson and Nicholas Hopkinson then review the potential implications of vitamin D deficiency for respiratory, musculoskeletal and cardiovascular health in patients with COPD.
Emerging evidence of the potential importance of vitamin D deficiency in susceptibility to acute respiratory infection is then reviewed by Yasmeen Hanifa and
Robert Walton, before Kirsten Mitchell, Chris Griffiths and myself provide an update of the evidence linking vitamin D deficiency and susceptibility to tuberculosis.
Helga Rhein presents the case for conducting trials to determine whether vitamin D supplementation may prolong survival in patients with lung cancer, before
Anna Coussens wraps up the issue with an overview of vitamin D metabolism and of the immunomodulatory actions of 1,25(OH)2D that underpin its many functions.
The evidence reviewed above is tantalising, but much of it comes from in vitro studies and observational epidemiology; randomised clinical trials are now needed to determine whether this scientific promise will translate into a clinical benefit. The challenges in conducting trials of vitamin D supplementation are significant: prevention trials, in particular, will require large sample sizes and prolonged follow-up in order to demonstrate clinically plausible effect sizes. Even modest effects are worthy of detection however: vitamin D supplementation is safe, simple to administer and inexpensive, and if it is eventually shown to benefit patients with common and debilitating respiratory disease then the benefits to public health will be very significant.
REFERENCES
[1] Holick MF. Vitamin D deficiency. N Engl J Med 2007; 357(3): 266-81.
[2] Glisson F, Bate G, Regemorter A. A treatise of the rickets: being a disease common to children. London: P. Cole; 1651.
[3] Barbour GL, Coburn JW, Slatopolsky E, Norman AW, Horst RL. Hypercalcemia in an anephric patient with sarcoidosis: evidence for extrarenal generation of 1,25-dihydroxyvitamin D. N Engl J Med 1981; 305(8): 440-3.
[4] Adams JS, Sharma OP, Gacad MA, Singer FR. Metabolism of 25-hydroxyvitamin D3 by cultured pulmonary alveolar macrophages in sarcoidosis. J Clin Invest 1983; 72(5): 1856-60.
[5] Baeke F, Takiishi T, Korf H, Gysemans C, Mathieu C. Vitamin D: modulator of the immune system. Curr Opin Pharmacol 2010; 10(4): 482-96.
[6] Hansdottir S, Monick MM, Hinde SL, Lovan N, Look DC, Hunninghake GW. Respiratory epithelial cells convert inactive vitamin D to its active form: potential effects on host defense. J Immunol 2008; 181(10): 7090-9.
[7] Abe E, Miyaura C, Sakagami H, et al. Differentiation of mouse myeloid leukemia cells induced by 1 alpha,25-dihydroxyvitamin D3. Proc Natl Acad Sci USA 1981; 78(8): 4990-4.
[8] Provvedini DM, Tsoukas CD, Deftos LJ, Manolagas SC. 1,25-dihydroxyvitamin D3 receptors in human leukocytes. Science 1983; 221(4616): 1181-3.
[9] Brennan A, Katz DR, Nunn JD, et al. Dendritic cells from human tissues express receptors for the immunoregulatory vitamin D3 metabolite, dihydroxycholecalciferol. Immunology 1987; 61(4):457-61.
[10] Menezes RJ, Cheney RT, Husain A, et al. Vitamin D receptor expression in normal, premalignant, and malignant human lung tissue. Cancer Epidemiol Biomarkers Prev 2008; 17(5): 1104-10.
[11] Hughes DA, Norton R. Vitamin D and respiratory health. Clin Exp Immunol 2009; 158(1): 20-5.
Early Life Vitamin D Status and Lung Development Pp.396-403
Stephen Goldring, John O. Warner, Seif O. Shaheen and Robert J. Boyle
There is evidence of an association between early life vitamin D insufficiency and future risk of developing asthma. Given the high prevalence of vitamin D insufficiency in women during pregnancy when developmental programming is occurring, this may be of critical public health importance. There are plausible biological mechanisms for an association. Vitamin D is the pro-hormone of calcitriol, a secosteroid hormone with widespread pleiotropic actions. It is a powerful immune modulator and has been shown in animal and in vitro work to have a role in early lung development. Calcitriol may influence lung development through expression of the vitamin D receptor on lung and immune cells, and through epigenetic mechanisms. If the association between early life vitamin D status and childhood respiratory disease is shown to be causal, then this could have significant implications for public health policy. This hypothesis is currently being tested in a number of prospective intervention trials. The aim of this article is to review the evidence that vitamin D status influences early lung development, with a focus on early life mechanisms.
Perinatal Vitamin D Deficiency and Childhood Asthma: A Molecular Perspective Pp.404-407
Virender K. Rehan and John S. Torday
There is a large body of literature suggesting that the recent increase in the incidence of childhood asthma might be associated with vitamin D deficiency during lung development. There are also strong experimental animal data showing that vitamin D is one of the local alveolar paracrine factors that spatiotemporally modulates perinatal pulmonary maturation. However, the mechanistic link between vitamin D deficiency during pregnancy and childhood asthma is not known. In this review, we demonstrate how perinatal vitamin D deficiency could mechanistically drive both the proximal and distal airways to a myogenic phenotype, molecularly and structurally, predisposing the offspring to asthma. More specifically, we will review how perinatal vitamin D deficiency results in an increased abundance of mesenchymal myofibroblasts, a feature that is highly consistent with the pathophysiology of asthma. We also provide evolutionary insights as to how vitamin D deficiency might (re)activate the atavistic host defense mechanisms that could precipitate a lung phenotype consistent with asthma. Since vitamin D deficiency seems to alter the normal homeostatic epithelialmesenchymal signaling pathways in the developing lung, it offers a distinct translational opportunity to prevent this process through targeted molecular manipulations. While we wait for the results of on-going trials of vitamin D supplementation during pregnancy to get some definitive answers on its role in the pathogenesis of childhood asthma, we advocate studies to discover new vitamin D analogs and/or metabolites with optimal respiratory effects and without any significant side effects.
Vitamin D and Asthma: Scientific Promise and Clinical Reality Pp.408-413
Graham Devereux and James G. Wagner
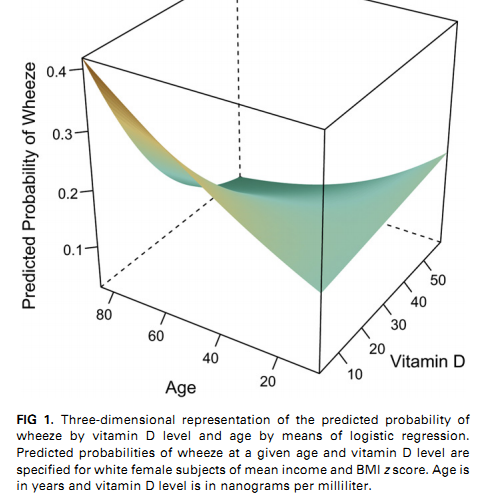
Widespread vitamin D insufficiency and vitamin D supplementation (even low dose rickets prophylaxis) have been hypothesised as contributory factors to the recent increase in asthma. These hypotheses are supported by reports of immunomodulatory effects of vitamin D on antigen presenting cells, regulatory T cells and T-helper cells and evidence that vitamin D influences fetal lung differentiation and epithelial-mesenchymal function. Studies of vitamin D in animal models confirm complex effects of vitamin D on asthma immunopathogenesis. In humans a majority of epidemiological studies support the hypothesis that vitamin D insufficiency during pregnancy increases the likelihood of childhood wheeze and possibly asthma, although some studies do report the converse. In children and adults with asthma, reduced serum vitamin 25-hydroxyvitamin D levels have been associated with parameters of increased asthma severity. Clinical trials are underway addressing whether maternal vitamin D supplementation during pregnancy reduces the likelihood of childhood asthma and if there is a role for vitamin D supplementation in established asthma.
Vitamin D in COPD - A Pleiotropic Micronutrient in a Multisystem Disease Pp.414-420
Abigail S. Jackson and Nicholas S. Hopkinson
Chronic Obstructive Pulmonary Disease (COPD) is a debilitating disease affecting an estimated 3 million people in the United Kingdom. It is characterised by progressive and irreversible airway obstruction and lung parenchymal damage, and by multisystem involvement including skeletal muscle impairment, systemic inflammation, and an increased prevalence of osteoporosis, cardiovascular disease and lung cancer.
Patients with COPD have reduced dietary intake of vitamin D, spend a reduced amount of time outdoors and have been shown to have lower levels of 25-hydroxyvitamin D (25[OH]D) than age-matched subjects without COPD. The active metabolite of vitamin D, 1,25-dihydoxyvitamin D (1,25[OH]2D), is a pleiotropic hormone with effects on lung development and function, the immune system and musculoskeletal function; vitamin D deficiency also associates with increased prevalence of cardiovascular disease and cancer. This article focuses on the evidence that vitamin D deficiency is highly prevalent in patients with COPD and reviews associations between vitamin D status and lung function, muscle function and risk of osteoporosis, cardiovascular disease and cancer. The potential pathological mechanisms which may be involved are also discussed.
Vitamin D and Acute Respiratory Tract Infection Pp.421-434
Yasmeen Hanifa and Robert Walton
Acute respiratory tract infections (ARTI) generate a major disease burden worldwide, disproportionately affecting the elderly and the very young. A growing body of evidence supports an important immunomodulatory function for the biologically active metabolite of vitamin D,1,25-dihydroxyvitamin D (1,25[OH]2D). Respiratory epithelial cells and leucocytes express both the vitamin D receptor and CYP27B1, the enzyme which converts 25-hydroxyvitamin D to 1,25(OH)2D. Observational and ecological studies report associations between inadequate vitamin D status and susceptibility to ARTI, and vitamin D deficiency has been proposed as the seasonal stimulus for influenza epidemics. In children, associations between profound vitamin D deficiency and susceptibility to lower respiratory tract infection have been reported in a variety of settings. In adults, particularly amongst those with asthma and COPD, inadequate vitamin D status has been reported to be associated with susceptibility to upper respiratory tract infection. Vitamin D supplementation trials for the prevention of ARTI report conflicting results. This may reflect variation in study populations and methodology, or factors such as genetic heterogeneity within the vitamin D metabolic or signalling pathways. Further trials of vitamin D supplementation in different settings, with measurement of participants' vitamin D status and evaluation of genetic factors which might modify the effect of vitamin D supplementation are needed.
Vitamin D and Tuberculosis Pp.435-439
Kirsten Mitchell, Christopher J. Griffiths and Adrian R. Martineau
Tuberculosis is a major global health problem: the World Health Organisation estimates that there were 9.4 million incident cases and 1.8 million deaths from the disease in 2008. The development of new agents to prevent acquisition or reactivation of latent Mycobacterium tuberculosis infection and to allow shortening of antimicrobial therapy regimens for active tuberculosis without loss of efficacy is a research priority. In this article we describe the immunomodulatory actions of vitamin D metabolites in mycobacterial infection and review the growing body of evidence from observational and intervention studies suggesting that vitamin D might have a role in the prevention and treatment of TB.
Vitamin D and Lung Cancer Pp.440-443
Helga Rhein
Lung cancer is one of the most common cancers but treatment has limited success and survival rates remain low. The active metabolite of vitamin D, 1,25-dihydroxyvitamin D, has anti-proliferative and pro-apoptotic actions in lung carcinoma cell lines in vitro. Vitamin D deficiency is associated with poor prognosis in lung cancer, and lung cancer survival varies according to vitamin D receptor genotype. Randomized controlled trials should be performed to determine whether vitamin D supplementation might have a role as an adjunct to conventional treatments for lung cancer.
Immunomodulatory Actions of Vitamin D Metabolites and their Potential Relevance to Human Lung Disease Pp.444-453
Anna K. Coussens
The non-classical role for vitamin D in maintaining immune homeostasis has been recognised for 30 years. A definitive link between vitamin D status and the immune response has now been established by a multitude of association studies which link both vitamin D deficiency and genetic polymorphisms in vitamin D-related genes to susceptibility to respiratory diseases including tuberculosis, upper respiratory tract infection, chronic obstructive pulmonary disease (COPD), asthma and lung cancer. This review considers the mechanisms by which immune cells and lung epithelial cells respond to infection or injury by inducing intracellular metabolism of vitamin D. The effects of vitamin D metabolites on induction of phagocyte antimicrobial responses, modulation of DC maturation and T cell priming, skewing of the cytokine milieu towards a type 2 inflammatory response and promotion of regulatory T (Treg) cell development will also be described.
Treatment of the Cheyne-Stokes Breathing Pattern in Patients with Congestive Heart Failure: State of the Art Pp.454-463
Charles Poon and Jeanne Wallace
Cheyne-Stokes breathing/central sleep apnea (CSB/CSA) commonly occurs in patients with congestive heart failure. Although the clinical significance of this primarily nocturnal breathing disorder is not certain, several studies have reported an association with increased mortality, as well as physiologic and biochemical changes that may lead to further deterioration of cardiac function. Suppression of CSB/CSA can be difficult to achieve and a consistently effective therapeutic strategy has not been identified. Optimizing medical management of the underlying heart failure is a logical initial intervention. In addition, positional therapy, oxygen, carbon dioxide, acetazolamide and theophylline have been associated with improvement of CSB/CSA in some patients. For patients with persistent CSB/CSA, nocturnal application of intrathoracic positive pressure via CPAP and BIPAP has sometimes been successful in attenuating CSB/CSA, but may not improve long-term survival. A newer technique, adaptive servo-ventilation that applies dynamic positive inspiratory pressure support in coordination with the patient's breathing pattern is promising, but more experience is needed to define the efficacy for attenuating CSB/CSA and long-term beneficial effects.
Acute Exercise Testing of COPD Patients: The Effect on Systemic Inflammatory Proteins Pp.464-474
Jane Canavan, Ben Linton-Willoughby and Rachel Garrod
Strenuous exercise can cause significant changes in the concentration of several pro- and anti-inflammatory cytokines in healthy people, with wide ranging effects, but research evidence addressing this is limited in COPD. A systematic review was therefore undertaken to clarify whether acute exercise affects circulating inflammatory proteins in stable COPD. Computerised searches were conducted of The Cochrane Database of Systematic Reviews, EMBASE, CINAHL, OVID MEDLINE and NLM gateway to identify relevant articles up to July 2010. Ten published studies using various exercise modes to ascertain the impact of acute exercise tests on systemic inflammation in COPD were retained for the review. Six studies reported significant increases in inflammatory markers, of varying magnitude; four out of five maximal cycling studies reported increased IL-6/TNF-?. There was considerable variance in pre-test conditions/patient characterization, exercise protocols, and assay techniques. The findings indicate that exercise intensity and duration, body composition, individual immunity, hypoxaemia and blood sampling method possibly explain most variations between studies.
See also VitaminDWiki
Lung cancer decreased by 7.5% for every 1260 feet in altitude
- Makes one think that the risk of Lung Cancer might be reduced with vitamin D (since UVB which creates vitamin D increases with altitude)
Prevention of Lung Cancer: Future Perspective with Natural Compounds
Pneumonia elderly death 12X more likely when vitamin D less than 12 ng – 2011
One third of lung disease patients in China had less than 4ng of vitamin D – May 2012
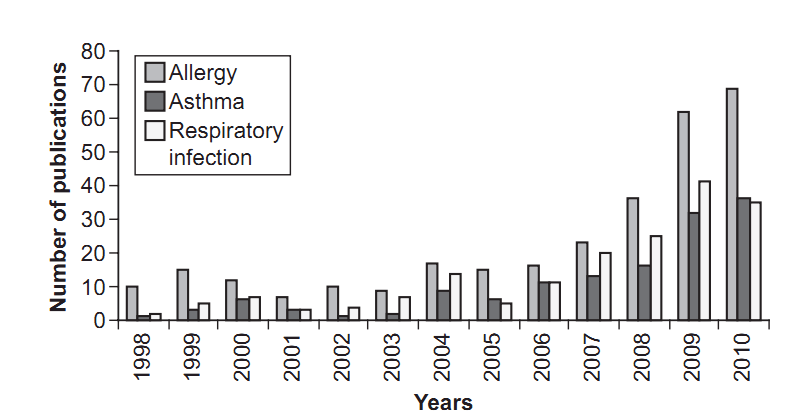
Crescendo of papers on Asthma, Allergy, and Vitamin D – Sept 2011
See also web
Vitamin D Council Respiratory Asthma, Chronic obstructive pulmonary disease, Cystic fibrosis, Pneumonia, Respiratory Tract Infections
Life Extension Magazine March 2007 - Vitamin D and Cancers such as Lung Cancer
Asthma Clinical Trials with Vitamin D Intervention as of Dec 2011
Vitamin and Asthma Study 03/10/2011
Correction of Vitamin D in Asthma Control 29/06/2011
Vitamin D and airway obstruction 2011-07-24
Vitamin D and Chronic Obstructive Lung Disease 12/08/2011
Sleep Apnea Syndrome and Vitamin D 24/03/2011
Vitamin D and Grass Pollen Specific Immunotherapy 01/11/2011
Vit D to Treat Asthma in Children: a Randomized, Double-blind, Placebo-controlled Trial *24/01/2011
The Effect of Vitamin D Replacement on Airway Reactivity, Allergy and Inflammatory Mediators in Exhaled Breath Condensate in Vitamin D Deficient Asthmatic Children 30/01/2011
