Inflammatory bowel disease and vitamin D – review
Review article: vitamin D and inflammatory bowel disease
– established concepts and future directions
Alimentary Pharmacology & Therapeutics; Volume 36, Issue 4, pages 324–344, August 2012
M. Garg 1,2,3,*,
J. S. Lubel 1,2,
M. P. Sparrow 4,
S. G. Holt 2,5,
P. R. Gibson 1,2,4
1 Department of Gastroenterology & Hepatology, Eastern Health, Box Hill, Vic, Australia
2 Eastern Health Clinical School, Monash University, Melbourne, Vic, Australia
3 Gastroenterology and Liver Transplant Unit, Austin Hospital, Melbourne, Vic, Australia
4 Department of Gastroenterology & Hepatology, Alfred Hospital, Melbourne, Vic, Australia
5 Department of Nephrology, Eastern Health, Box Hill, Vic, Australia
- Correspondence to: Dr M. Garg, Department of Gastroenterology & Hepatology, Eastern Health, Level 2, 5 Arnold St, Box Hill 3128 Vic, Australia, Mayur.Garg@monash.edu
Background: Understanding of the role of vitamin D in health and disease has increased markedly in the past decade, with its involvement extending well beyond traditional roles in calcium and phosphate homeostasis and musculoskeletal health. This conceptual expansion has been underpinned by identification and exploration of components of this axis including vitamin D-binding protein, key enzymes and receptors in multiple cell types, and a greater recognition of nonclassical autocrine and paracrine effects. Its influence in IBD remains uncertain.
Aim: To review the role of vitamin D in bone health, immune regulation and cancer prevention in IBD, and to outline practical issues and limitations of its use.
Methods: An extensive online literature review including PubMed and Medline.
Results: In patients with IBD, the vitamin D axis provides an important and often underutilised pathway to preserving bone health. Furthermore, an exciting body of clinical and basic science research demonstrates that these pathways may have an integral part to play in regulation of the immune response in IBD, through effects on the intestinal barrier, antigen presenting cells and adaptive T cells. The possibility of chemoprevention requires further study.
The optimal target level of 25-hydroxy vitamin D in patients with IBD is currently uncertain, as is the best therapeutic modality.
Conclusions: Study of vitamin D pathways may result in the development of relatively inexpensive therapeutic options to optimise patient outcomes.
Further prospective clinical research is required to address efficacy and long-term safety.
From PDF
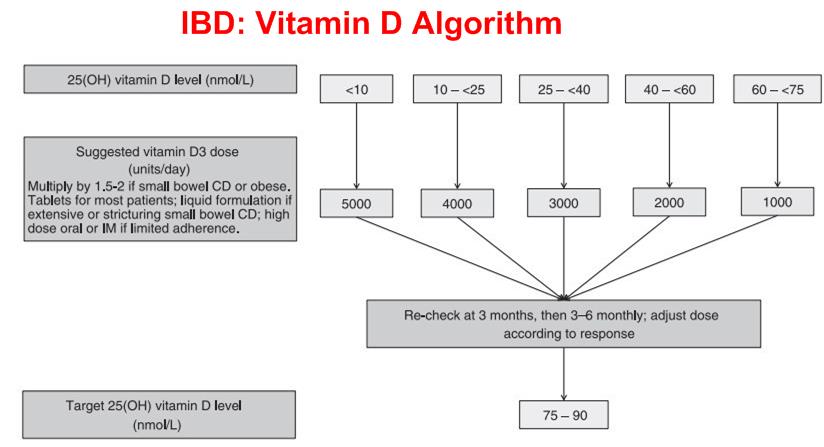
VitaminDWiki notices various failures in suggested treatment
Fails to provide loading dose so as to speed up the treatment
Fails to consider types of vitamin D which are better absorbed with gut problems
Fails to aim for a higher level of vitamin D- which is needed to TREAT a disease (something in the range of 100-200 nmol)
Fails to consider treatment with UV - which provides vitamin D without depending on the gut
Fails to consider cofactors - which are generally important for vitamin D supplementation
- and are especially important for those with poor absorption = IBD
PDF is attached at the bottom of this page
See also VitaminDWiki
Inflammatory bowel diseases are helped by vitamin D – commissioned review Nov 2013 in same journal
Overview Gut and vitamin D contains the following summary
- {include}
Short url = http://is.gd/ibdvitd
