Crescendo of papers on Asthma, Allergy, and Vitamin D
Asthma, allergy and respiratory infections: the vitamin D hypothesis
S. Bozzetto1, S. Carraro1, G. Giordano1, A. Boner2, E. Baraldi1 baraldi@pediatria.unipd.it
1 Allergy Unit and Respiratory Medicine, Department of Pediatrics, University of Padova, Padova
2 Department of Pediatrics, University Hospital, Verona, Italy
Allergy & Clinical Immunology , 21 SEP 2011, DOI: 10.1111/j.1398-9995.2011.02711.x
The recent discovery that every tissue in the human body has vitamin D receptors and that vitamin D has pleiotropic effects has prompted an increased interest in this hormone. Vitamin D deficiency is widespread and on the increase. There is no consensus on the serum vitamin D levels to consider appropriate for global health, the cutoffs for its deficiency, or the doses to use for its supplementation. Vitamin D seems to correlate closely with host reactions against various respiratory infections. Epidemiological studies have shown that low serum 25-hydroxyvitamin D levels are associated with a higher risk of upper and lower respiratory infections in children and a shortage of vitamin D may contribute to asthmatic patients’ symptoms and morbidity rates. There are studies highlighting associations between childhood asthma, fetal lung and/or immune development, and maternal vitamin D intake. An insufficiency of this vitamin also seems to be implicated in the onset of childhood atopy and food allergies. The hypothesis is that vitamin D could have a central role in these pathological situations and that it may represent a novel preventive and/or therapeutic strategy. This article reviews and discusses published data on the relationship between vitamin D and asthma and allergy, emphasizing the need for controlled, prospective studies on vitamin D supplementation to clarify whether it has a role in the prevention of and treatment for asthma and allergic conditions.
PDF is attached at the bottom of this page
Increasing number of studies during past 12 years: Hypothesis that low vitamin D causes some breathing problems (graph from PDF)
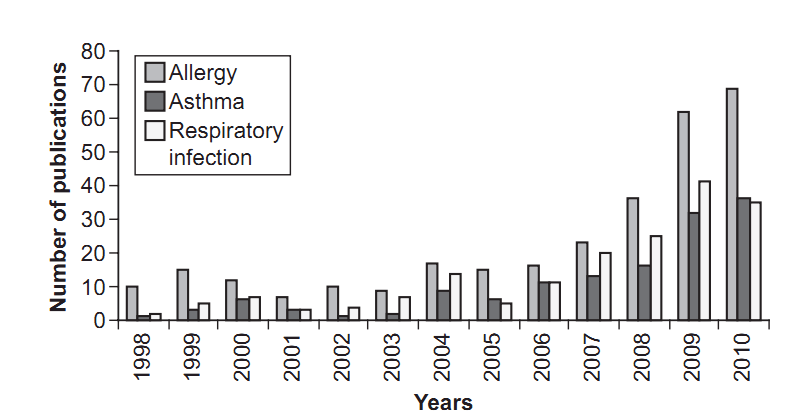
Figure 2: Schematic diagram of vitamin D metabolism
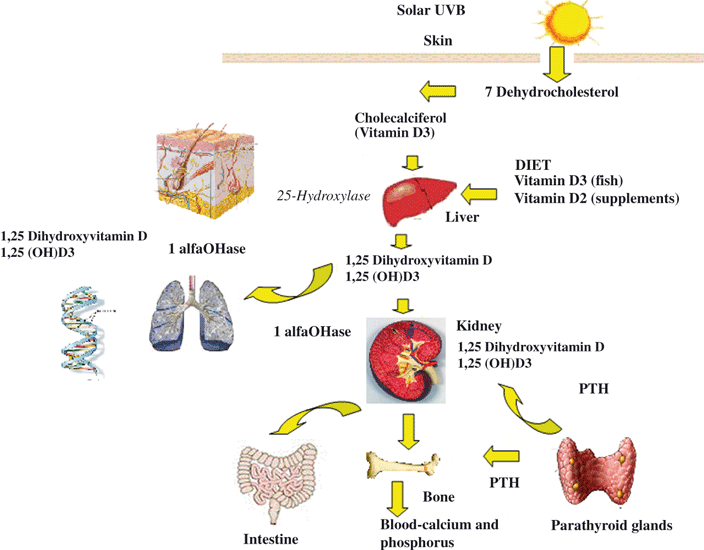
During exposure to sunlight, 7-dehydrocholesterol in the skin absorbs solar UVB radiation and is converted into cholecalciferol (Vit D3). Together with vitamin D originating from the diet, it enters the circulation and is metabolized to 25 hydroxyvitamin D3 (25[OH]D3) in the liver by vitamin D 25-hydroxylase. This is the form that circulates in the highest concentrations and reflects solar and dietary exposure. 25(OH)D3 reenters the circulation and is converted into 1,25(OH)2D3 in the kidney by 25(OH)D3 1 hydroxylase. A variety of factors, including serum phosphorus (Pi) and PTH, regulate the renal production of 1,25(OH)2D, which governs calcium metabolism through interactions with its major target tissues, i.e. bone and intestine. 25(OH)D is also metabolized in other tissues to regulate cell growth (e.g. in the lung and skin) and its expression is controlled by immune signals instead of bone and calcium homeostasis mediators.
Conclusions
In recent years, numerous studies have been published on the effects of vitamin D, which seems to have a role in many different diseases (autoimmune, cardiovascular, allergic disorders, etc.).
Rickets is no longer considered a common disease, but vitamin D deficiency seems to be widespread and may occur without many of the signs of nutritional rickets.
A limit of the present review is that the studies considered sometimes differ somewhat in defining deficient and insufficient vitamin D levels, because there is no general consensus on such definitions.
The variations are small but they may nonetheless constitute an important bias.
It would be important to arrive at definitions of the optimum serum level and the levels coinciding with vitamin D deficiency or insufficiency, not only for osseous outcomes but also for global health.
A crucial issue for any vitamin D intervention concerns its dosage.
The currently recommended vitamin D levels are thought to be the bare minimum needed for its beneficial effects on muscle and skeletal function, but the optimal vitamin D levels for global health (immune system function, possible prevention of atopy and defense against respiratory infections) are still not known. In light of recent literature on the action of vitamin D, and the effects it has demonstrated in vivo and in vitro in asthma and atopic disorders, it seems that this hormone might lead to a new turning point in our understanding and treatment of these increasingly common conditions . Well-designed clinical trials on vitamin D supplementation are needed to provide a definitive answer to the hypothesis that vitamin D could have a role in the prevention of and treatment for asthma, allergic diseases, and respiratory infections in childhood.
See also VitaminDWiki
Breathing category listing has items along with related searches
Allergy medications may be improved by Vitamin D (6X for birch pollen in this case) – Aug 2021
