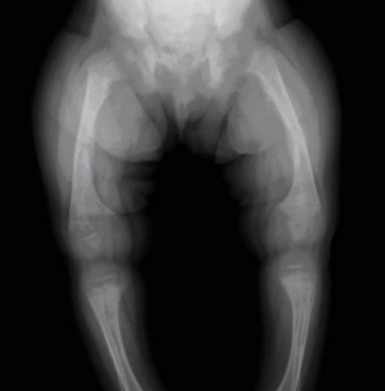
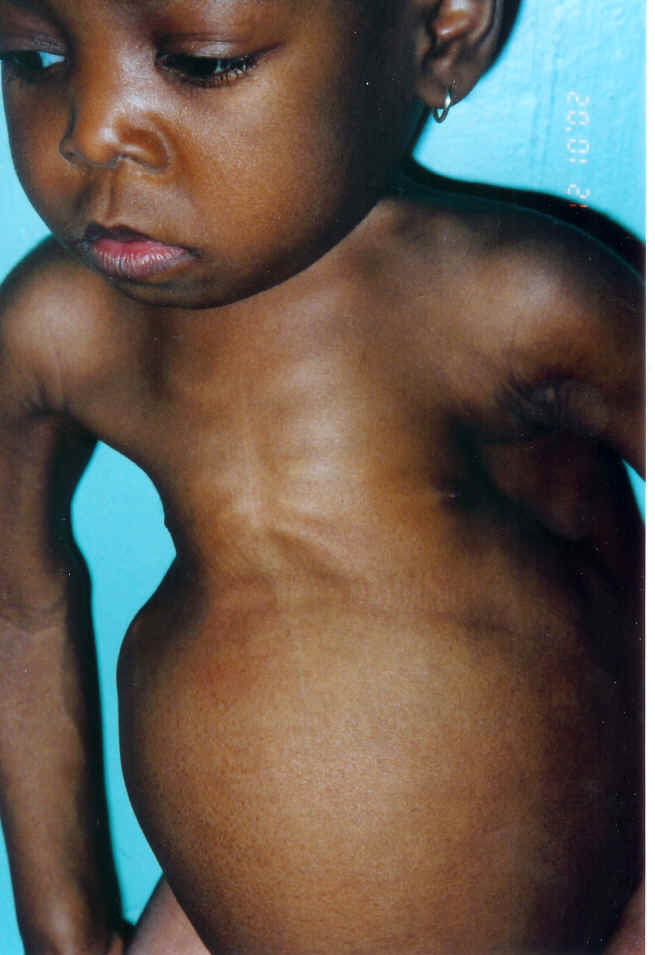
Rickets very prevalent in Mongolia – 1998
Prevalence of rickets in Mongolia
Asia Pacific J Clin Nutr (1998) 7(3/4): 325-328
U Tserendolgor1 MD pubhealth@magicnet.mn, JT Mawson2 MA, AC MacDonald3 MSc and M Oyunbileg1 MD, PhD
1 National Nutrition Research Center, Public Health Institute, National Medical University, Ulaanbaatar, Mongolia
2 Visiting Henry Luce Scholar at the National Nutrition Research Center, Public Health Institute, National Medical University, Ulaanbaatar, Mongolia
3 Department of Family Relations and Applied Nutrition, University of Guelph, Guelph, Ontario, Canada
In order to investigate the current health and nutrition status of mothers and children in Mongolia, a regionally stratified survey of 977 randomly sampled households was conducted during July and August 1997. The prevalence of children aged 6-60 months who demonstrated one or more of three main clinical signs (i.e. rachitic rosary, Harrison's groove and delayed closure of fontanelle) was found to be 69.8%. Although a nationwide supplementation programme exists, caretakers reported only 66.2% of children under 3 years of age had received at least one vitamin D supplement in the 6 months preceding the survey. The lack of adequate UV-B rays during the winter months (i.e. October-April) and traditional swaddling of infants for a minimum of 3 months and a maximum of 9-12 months are likely to contribute to the prevalence of rickets in Mongolia. The high prevalence of rickets in Mongolian children is a serious public health concern. In addition to the adverse effects on growth, development and immune function, it is probably indicative of widespread subclinical vitamin D deficiency.
Introduction
In modern times, it is unusual for populations to display a high prevalence of rickets, typically found only in high latitude northern countries without vitamin D fortification of food products. Few nutrition surveys have been performed in Mongolia, a sparsely populated (2 347 068 people) landlocked country with a severe continental climate (temperatures fluctuate from -45°C to +30°C annually). A high prevalence of rickets was noted, however, in the 1992 child nutrition survey conducted by the United Nations Children's Fund and the Ministry of Health and Social Welfare (MOHSW) in 1992.1 Among children under 5 years of age, 44.7% displayed craniotabes and/or bowed legs or knocked knees. In that study, children aged 13-24 months demonstrated a higher prevalence of rickets than other age groups.1 Biochemical analysis for rickets is not currently available in Mongolia and rickets must be evaluated using clinical signs.
There are many possible contributors to the high prevalence of rickets in the Mongolian population. The northern latitude limits exposure to UV-B rays during the winter months and cold weather for the majority of the year limits skin exposure. Cultural emphasis on infant swaddling limits sunlight exposure throughout the year in young infants. Consistent vitamin D supplementation is limited and few vitamin D-rich foods are available. There is no vitamin D food fortification at present. Exclusive breast-feeding is nearly universal up to 4 months of age, with more than 80% of mothers breast-feeding up to 2 years. Other factors may contribute to the high prevalence of rickets: these include seasonally low calcium intakes and factors inhibiting calcium absorption.
Before 1993, the national vitamin D supplementation programme was based upon daily doses of 400-800 IU, but parent compliance was low and this regimen was rarely followed. A programme for preventive and treatment stoss-therapy began in 1993. The programme strategy was to distribute supplements (50 000 IU) to children from birth to 2 years of age in order to prevent vitamin D deficiency. In most cases, supplements were distributed once or twice during this period and supplies to health centres were inconsistent. The current goals of the Mongolian government, as specified in the 1992 National Child Development Programme, include increasing the supply of vitamin D supplements to 80% of children under 3 years of age and decreasing the cases of rickets by 20% by the year 2000.2
To investigate the current prevalence of clinical signs of rickets among children in Mongolia, a regionally stratified nutrition survey of 977 randomly sampled households was conducted during July and August 1997. The survey included an evaluation of the clinical signs of rickets in 441 children under 5 years of age and also investigated possible risk factors for rickets.
Methods
A regionally representative survey was carried out by the Nutrition Research Centre (NRC) and World Vision Mongolia (WVM) during July and August 1997. The main survey covered the province of Bulgan (population 64 000, located in the northern part of Mongolia), the province of Dundgobi (population 53 400, located in the mid-southern part of the country), and the main central city of Ulaanbaatar (population 633 900). Prior to the main survey, a pilot survey of 96 households was carried out in Amgalan, a ger (traditional dwelling) sub-district of Ulaanbaatar.
The main survey covered 977 households randomly sampled by cluster sampling methodology (41 clusters), resulting in the evaluation of 454 children under 5 years of age. Household cluster survey sampling procedures were followed, stratified to represent urban and rural provinces. In Ulaanbaatar, four districts were randomly selected and the khoroos (districts) served as clusters. Twenty clusters were randomly chosen in proportion to population from the four districts. In each of the two rural provinces, the provincial capital and three sums (districts) were chosen randomly. These were divided into bags (regions), which were defined as clusters. Eleven clusters were chosen from Bulgan and 10 from Dundgobi.
At the household stage of sampling, 24 households were randomly selected in each cluster by the segmentation (urban) and the EPI INFO (Centers for Disease Control and Prevention, Atlanta, USA) methods (rural). The survey was conducted by a 17-member team including one survey coordinator (a paediatrician from the NRC), four supervisors (researchers from the NRC), four experienced laboratory technicians/nurses, four interviewers (from MOHSW) and four paediatricians.
Height and weight were measured in all children under 5 years of age, according to World Health Organization (WHO) guidelines. Standard deviation (Z scores) was calculated using comparisons with the WHO/NCHS international growth database (EPI INFO). Birthweights were reported by the mothers. Each child under 5 years of age was examined for clinical symptoms of rickets, using a 13-symptom checklist. The child's caretaker was shown a vitamin D capsule and asked whether the child had ever received a vitamin D supplement. Caretakers were also asked whether the child had suffered any illnesses in the previous 4 weeks. Questionnaires covered exposure of children to direct sunlight and swaddling time in months, as well as household characteristics, coping mechanisms, breast-feeding and complementary feeding practices.
Due to the lack of an established international classification system for clinical signs of rickets, several groupings were used.
Clinical evidence of at least one of three main signs (
rachitic rosary,
Harrison's groove or
delayed closure of fontanelle)
or at least one of nine signs (
craniotabes,
rachitic rosary,
Harrison's groove,
delayed closure of fontanelle,
muscular hypotonia,
abdomen of a frog,
spinal deformation,
pigeon chest or
bowed legs),
were used to establish rickets.
Children were classified as having more severe rickets when they demonstrated two or more of nine clinical signs.
The prevalence of at least one of four 'active' signs of rickets (
excessive perspiration,
smell of urine,
muscular hypotonia or
abdomen of a frog),
was also computed on a smaller sample.
The 'active' signs may have been more appropriate for younger infants. Certain signs and symptoms (excessive perspiration, smell of urine, occipital alopecia and Olympic forehead), were omitted from the majority of statistical analysis due to clinical unreliability, subjectivity or reliance upon information reported by the child's caretaker. Data were analysed using SPSS software, while correlations were established using the Chi-squared test and the ANOVA technique.
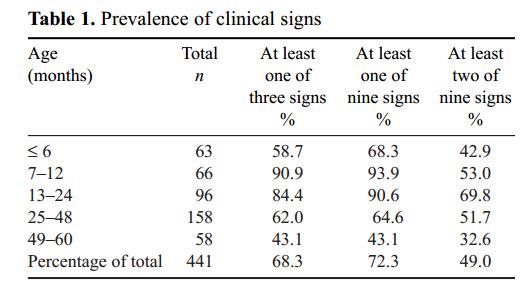
Table 1. Prevalence of clinical signs
Results
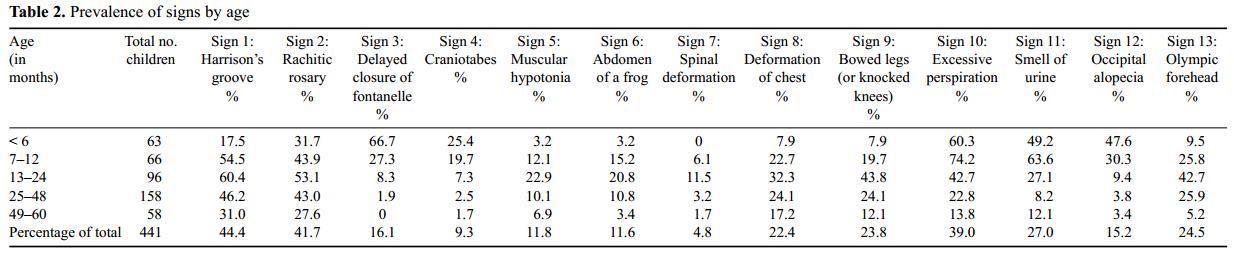
In our survey, 31.1% of children (137 of 441) demonstrated craniotabes and/or bowed legs and knocked knees. The prevalence of children under 5 years of age demonstrating at least one of three main clinical signs (rachitic rosary, Harrison's groove or delayed closure of fontanelle) was found to be 67.4% (69.8% among children 6-60 months). The prevalence of children displaying at least one of four 'active' signs of rickets (excessive perspiration, smell of urine, muscular hypotonia or abdomen of a frog) was found to be 48% (155 of 323; compiled data were only available for a smaller sample). A slightly larger number of children under 5 years of age, 72.3%, displayed at least one of nine clinical signs (craniotabes, rachitic rosary, Harrison's groove, delayed closure of fontanelle, muscular hypotonia, abdomen of a frog, spinal deformation, pigeon chest or bowed legs), with 49.0% (216 of 441) demonstrating at least two of the nine symptoms (Table 1), and 28.9% (133 of 441) displaying at least three of nine clinical signs. The percentage of the population displaying each clinical sign is reported in Table 2.
Caretakers reported that only 66.2% of children under 3 years had received at least one vitamin D supplement in the 6 months preceding the survey (however, 27.8% of the entire sample did not respond). Children with one or more of nine signs were more likely to be reported by their mothers as having been ill in the past month (Chi-squared test, P < 0.01).
The prevalence of more severe rickets (children with two or more of nine clinical signs) varied significantly by location. The highest prevalence was in Ulaanbaatar ( 58.1% ; 125 out of 215) followed by Dundgobi (45.5%; 46 out of 101), while the lowest was in Bulgan (37.9%; 50 out of 132) (Chi-squared test, P < 0.01).
In addition, children with severe rickets (two or more clinical signs) were more likely to have been born in winter (Chi-squared test, P < 0.05), more likely to have been low birthweight babies (less than 2500 g at birth; Chi-squared test, P <0.01), and more likely to have been born either early (6-8 months) or late (greater than 9.5 months; anova, P <0.01). Spinal deformation was found only in the most severe cases, that is, in children demonstrating at least four other signs of rickets.
There was a trend (P = 0.077) for stunted children to be more likely than normal children to show one or more of nine clinical signs.
Many of the clinical signs were found to correlate significantly with stunting: Olympic forehead (P < 0.01), chest deformation (pigeon chest; P < 0.01), muscular hypotonia (P <0.01), abdomen of a frog (P <0.01) and spinal deformation (P < 0.01) (all Chi-squared test).
Underweight children were more likely to have signs of rickets (one or more of nine signs) than normal weight children (Chi-squared test, P < 0.05). In addition, several symptoms correlated significantly with underweight children: Olympic forehead (P <0.01), chest deformation (pigeon chest; P < 0.01), muscular hypotonia (P < 0.01), spinal deformation (P < 0.05), bowed legs (P < 0.01) and a trend to correlate with Harrison's groove (P = 0.061).
There was no difference in rickets prevalence between male and female children. Although all caretakers reported swaddling their children, reported duration of swaddling time did not correlate with signs of rickets. There was no correlation between anaemia and signs of rickets. There was also no correlation found between monthly household income or percentage of monthly income spent on food and signs of rickets. Children with one or more of nine signs of rickets were less likely to have dental caries (as reported by caretaker) than normal children (Chi-squared test, P < 0.01).
Discussion
Following political and economic transition in Mongolia in 1989, changes in the healthcare sector led to both decreases and variability in the supplementation programme, possibly leading to a greater incidence of rickets . Using the prevalence of one or more of three main clinical signs (rachitic rosary, Harrison's groove or enlarged size of fontanelle), the overall prevalence was almost 70%. Among children aged 13-24 months, 90% show one of three clinical signs. This prevalence warrants further investigation.
Applying the assessment model (the presence of craniotabes and/or bowed legs or knocked knees) used by the 1992 UNICEF/MOHSW nutrition survey to our data, indicates a lower prevalence in our study than in 1992, 30.6% as compared with 44.7%. These signs may not be the most appropriate measures of active rickets, however, and this model may mask more acute deficiency. Craniotabes can result from other causes, and normal children can demonstrate craniotabes (JM Pettifor, pers. comm., 1998). In addition, bowed legs can persist in children with healed rickets, and may also vary due to genetic differences in populations.
Children in Ulaanbaatar are more likely than their rural counterparts
to live in apartments,
to spend more time inside, and
to live in a more polluted area.
These factors may contribute to a higher prevalence of rickets. The higher prevalence of rickets among children born during the winter months could be due to the seasonal swaddling period and possibly to low maternal stores of vitamin D.
It is also important to note the
significant relationship between length of pregnancy and clinical signs of rickets, and the
relationship between birthweight and rickets.
Other studies have indicated increased tendencies for low birthweight and preterm babies to display rickets.3
The relationship between possessing one or more of the clinical signs of rickets and having been sick during the past month is also an important finding. Vitamin D deficiency rickets is associated with the lowering of general immune resistance4 and has also been correlated with increased incidence of pneumonia, diarrhoea and other infections.5 The reduction in immune resistance among Mongolian children may be a contributing factor to the high incidence of Acute Respiratory Infection (ARI), the leading cause of death among children under 5 years of age. Rickets affecting pelvic development in female children may be a contributing factor to high maternal mortality in Mongolia (145 per 100 000 births in 19976) by increasing the risk of cephalo-pelvic disproportion (CPD).7
The high prevalence of clinical signs of rickets in Mongolia is a serious public health problem that should be studied further. The situation requires continued investigation into the aetiology of rickets in Mongolian children, an evaluation of possible contributing factors, and an evaluation of the efficacy of vitamin D supplementation and stoss therapy. The contribution of calcium intakes, found to be a main contributor to rickets incidence in Nigeria, as well as inhibitors of calcium absorption, should be examined.8 Although we did not find the duration of swaddling time to correlate with rickets, the fact that all children were swaddled requires further evaluation, and prevention could be integrated into further nutrition information, education and communication programmes. In addition, the role of lactose, which has been found to aid absorption of calcium in the absence of vitamin D,9 as well as the report of low levels of the gene for high intestinal lactase in the Mongolian population, should be integrated into further analysis.7
The authors acknowledge that diagnosis of rickets based solely upon clinical signs can be unreliable. In addition, it is possible that over-diagnosis of signs of rickets could have been a factor in this survey, as has been found among physicians in China.10 It would be prudent to be cautious about designing public health interventions, especially potentially toxic stosstherapy programmes, without further study.11
Although evaluation of clinical signs is the only method available at present, the Nutrition Research Center hopes to have the opportunity to combine this method with biochemical measurements and radiological examination in the future.
Acknowledgements. The authors would like to thank World Vision Mongolia and World Vision Canada for supporting the 1997 Nutrition and Food Security Survey, and for providing technical assistance. We would like extend our gratitude to Dr Tsergelen for her invaluable assistance with statistical analysis. In addition we would like to thank the Henry Luce Foundation and the Luce Scholars Program.
References
1. UNICEF/Ministry of Health. Child Nutrition Survey. Ulaanbaatar: UNICEF/Ministry of Health and Social Welfare, 1993.
2. Ministry of Health and Social Welfare. The 1992 National Child Development Programme. Ulaanbaatar, Mongolia, 1992.
3. Paunier L. Prevention of Rickets. In: FH Glorieux, ed. Rickets. Nestle Nutrition Workshop Series, Vol. 21. New York: Vevey/Raven Press Ltd, 1991.
4. Yener E, Coker C, Cura A, Keskinoglu A, Mir S. Lymphocyte sub-populations in children with vitamin D deficient rickets. Acta Paediatr Jpn 1995; 37: 500-502.
5. Muhe L, Lulseged S, Mason KE, Simoes EA. Case-control study of the role of nutritional rickets in the risk of developing pneumonia in Ethiopian children. Lancet 1997; 349: 1801-1804.
6. National Statistical Office. 1997 Mongolian Statistical Yearbook. Ulaanbaatar, 1998.
7. Strickland SS. Human nutrition in Mongolia: Maternal mortality and rickets. Nomadic Peoples 1993; 33: 231-239.
8. Oginni LM, Worsfold M, Oyelami OA, Sharp CA, Powell DE, Davie MWJ. Etiology of rickets in Nigerian children. J Pediatr 1996; 128: 692-694.
9. Durham WH. Coevolution. Stanford: Stanford University Press 1993; 254-259.
10. Tong L. Prevention of rickets and vitamin D intoxication in China (letter). Acta Paediatr 1995; 84: 940.
11. Wharton BA. Diagnosis and presentation of rickets (letter). Acta Paediatr 1995; 84: 848.
See also VitaminDWiki
See also web
- Harrison's Groove Wikipedia
Harrison's groove, also known as Harrison's sulcus, is a horizontal groove along the lower border of the thorax corresponding to the costal insertion of the diaphragm; It is usually caused by chronic asthma or obstructive respiratory disease. It may also appear in rickets because the patients lack the mineralized calcium in their bones necessary to harden them; thus the diaphragm, which is always in tension, pulls the softened bone inward. During rickets it is due to the indentation of lower ribs at the point of attachment of diaphragm.