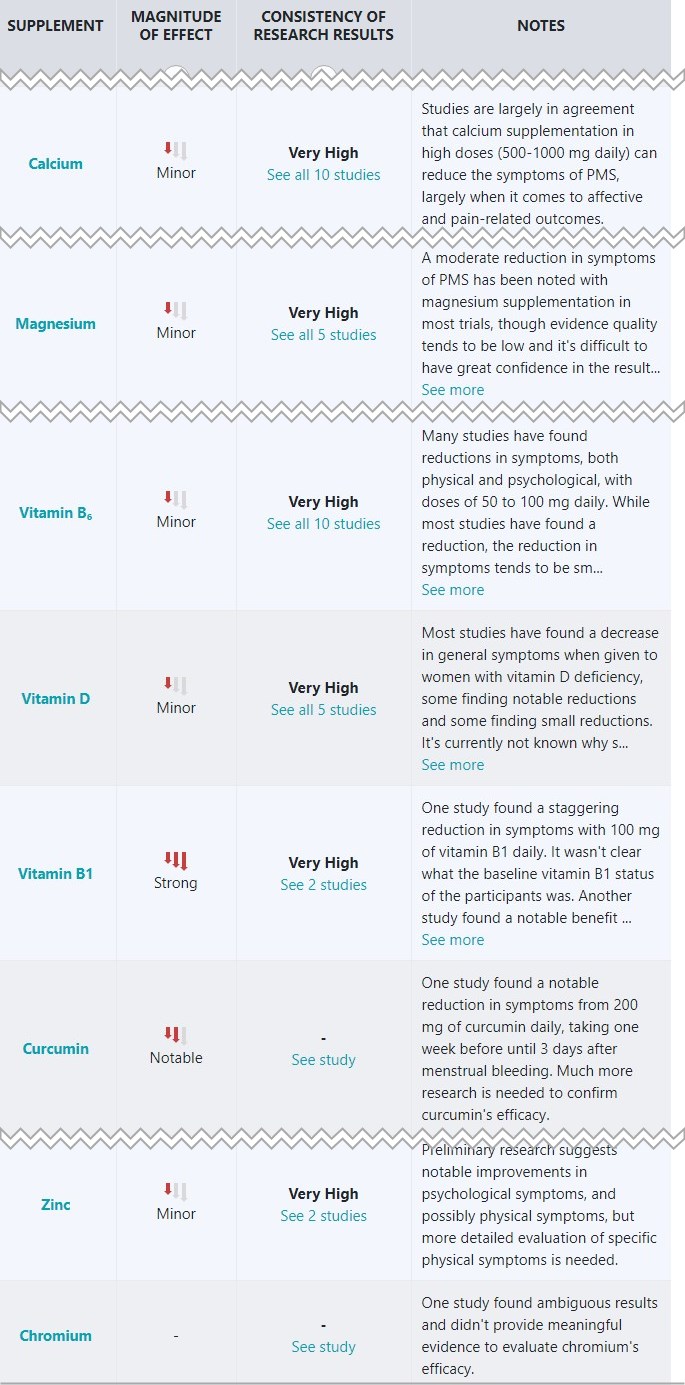
PMS decreased when Vitamin D was added
9 VitaminDWiki pages with PMS in title as of Sept 2021
VitaminDWiki pages containing PREMENSTRUAL or PMS in title
PMS significantly reduced by 50,000 IU of vitamin D every two weeks – RCT Oct 2019
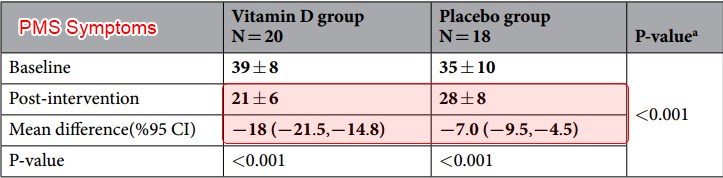
PMS reduced by Vitamin D intervention - meta-analysis May 2019
PMS reduced by Vitamin D intervention - meta-analysis May 2019
PMS in teens reduced 3X by 50,000 IU vitamin D weekly – Jan 2018
PMS in teens reduced 3X by 50,000 IU vitamin D weekly – Jan 2018
Menstrual Pain reduced by vitamin D – RCT 2012, 2014, 2016
Menstrual Pain (PMS) reduced by vitamin D – RCT 2012, 2014, 2016 some content overlap with this page
Vitamin D Supplementation for Premenstrual Syndrome-Related Mood Disorders in Adolescents with Severe Hypovitaminosis D Aug 2016
Clinical trial of women who initially had very low vitamin D (< 10ng)
Loading dose of 200,000IU and 25,000 IU every 2 weeks for 4 months
| Score | Before | After |
| Anxiety | 51 | 20 |
| Irritability | 130 | 70 |
| Crying easily | 41 | 30 |
| Crying | 51 | 31 |
| Disturbed relationships | 150 | 70 |
13% higher risk of PMS for each 4 ng lower level of Vitamin D - Aug 2014
Vitamin D Supplementation for Premenstrual Syndrome-Related Mood Disorders in Adolescents with Severe Hypovitaminosis D. 📄 Download the PDF from VitaminDWiki **---
Dietary vitamin D intake, 25-hydroxyvitamin D3 levels and premenstrual syndrome in a college-aged population - 2010
by: Elizabeth R. Bertone-Johnson, Patricia O. Chocano-Bedoya, Sofija E. Zagarins, Ann E. Micka, Ronnenberg
The Journal of Steroid Biochemistry and Molecular Biology (14 April 2010)
High dietary intake of vitamin D may reduce the risk of premenstrual syndrome (PMS), perhaps by affecting calcium levels, cyclic sex steroid hormone fluctuations, and/or neurotransmitter function. Only a small number of previous studies have evaluated this relationship and none have focused on young women. We assessed this relationship in a cross-sectional analysis within the UMass Vitamin D Status Study. Between 2006 and 2008, 186 women aged 18–30 (mean age = 21.6 years) completed a validated food frequency questionnaire, additional questionnaires to assess menstrual symptoms and other health and lifestyle factors, and provided a fasting blood sample collected during the late luteal phase of their menstrual cycle. Among all study participants, results suggested the possibility of an inverse association between intake of vitamin D from food sources and overall menstrual symptom severity, though were not statistically significant; mean intakes in women reporting menstrual symptom severity of none/minimal, mild, and moderate/severe were 253, 214, and 194 IU/day, respectively ( P = 0.18). From among all study participants, 44 women meeting standard criteria for PMS and 46 women meeting control criteria were included in additional case–control analyses. In these women, after adjustment for age, body mass index, smoking status and total calcium intake, higher intake of vitamin D from foods was associated with a significant lower prevalence of PMS.
Women reporting vitamin D intake from* food sources of <100 IU/day had a prevalence odds ratio of 0.31 *compared to those reporting <100 IU/day (95% confidence interval = 0.10–0.98). Late luteal phase 25-hydroxyvitamin D 3 levels were not associated with prevalent PMS.
Results from this pilot study suggest that a relationship between vitamin D and PMS is possible, though larger studies are needed to further evaluate this relationship and to investigate whether 25-hydroxyvitamin D 3 levels in the follicular or early luteal phases of the menstrual cycle may be related to PMS risk.
Here's why periods can get worse in winter Jan 2018* PMS lasted 0.9 days longer in the winter *---
PMS reduced by half in girls who had low levels of vitamin D – RCT Dec 2015
Vitamin D supplementation reduced PMS pain (does not quantify) - July 2018* The impact of circulating 25-hydroxyvitamin and oral cholecalciferol treatment on menstrual pain in dysmenorrheic patients. *Gynecol Endocrinol. 2018 Jul 25:1-5. doi: 10.1080/09513590.2018.1490407.
Kucukceran H1, Ozdemir O2, Kiral S3, Berker DS4, Kahveci R5, Ozkara A5, Atalay CR2, Ates İ6.
This study aims to determine Vitamin-D level in patients with primary dysmenorrhea and investigate the effect of Vitamin-D replacement on symptoms. About 100 patients in the 18-30 age group followed-up with primary dysmenorrhea diagnosis were included in this observational study. The pain severity was assessed using the visual analog scale (VAS). 25-hydroxy vitamin D(25(OH)D) levels of the patients were measured and the replacement therapy was applied according to measurement results. The patients were followed for three months in total. At the end of the three-month period, the 25(OH)D level was measured and the VAS score was assessed once more after the therapy. 25(OH)D level was insufficient in 23.0%, deficient in 45.0%, and severely deficient in 32.0% of the patients.
It was found that the VAS score increased as the 25(OH)D level decreased (r = -0.320; p = .002). A significant reduction was observed in VAS scores after Vitamin-D treatment in all three groups; the amount of reduction in VAS score was determined to be higher in the patients with severely deficient levels of 25(OH)D, compared to the patients with deficient or insufficient levels (p < .001). A significant and negative correlation was found between Vitamin-D and symptoms associated with dysmenorrhea in our study. The Vitamin-D replacement therapy led to a significant decrease in symptoms.
50,000 IU Vitamin D weekly reduced menstrual problems, dysmenorrhea, and premenstrual syndrom - Aug 2018* High dose vitamin D supplementation can improve menstrual problems, dysmenorrhea, and premenstrual syndrome in adolescents. *Gynecol Endocrinol. 2018 Aug;34(8):659-663. doi: 10.1080/09513590.2017.1423466. Epub 2018 Feb 15.
Bahrami A1,2, Avan A2,3, Sadeghnia HR4, Esmaeili H5, Tayefi M6, Ghasemi F7, Nejati Salehkhani F8, Arabpour-Dahoue M8, Rastgar-Moghadam A2, Ferns GA9, Bahrami-Taghanaki H10, Ghayour-Mobarhan M3.
Vitamin D has a crucial role in female reproduction, possibly through its effects on calcium homeostasis, cyclic sex steroid hormone fluctuations, or neurotransmitter function. We have assessed the effects of vitamin D supplementation on dysmenorrhea and premenstrual syndrome (PMS) in adolescents. In this study, 897 adolescent girls living in Mashhad and Sabzevar, Iran, received nine high-dose vitamin D supplements (as 50,000 IU/week of cholecalciferol) and were followed up over 9 weeks. We evaluated the effect of vitamin D supplementation on individuals in four categories: those with only PMS; individuals with only dysmenorrhea; subjects with both PMS and dysmenorrhea and normal subjects. The prevalence of PMS after the intervention fell from 14.9% to 4.8% (p < .001). Similar results were also found for the prevalence of subjects with dysmenorrhea (35.9% reduced to 32.4%), and in subjects with both PMS and dysmenorrhea (32.7% reduced 25.7%). Vitamin D supplementation was associated with a reduction in the incidence of several symptoms of PMS such as backache and tendency to cry easily as well as decrement in pain severity of dysmenorrhea (p < .05). High dose vitamin D supplementation can reduce the prevalence of PMS and dysmenorrhea as well as has positive effects on the physical and psychological symptoms of PMS.
PMS pain greatly reduced with 50,000 IU weekly - RCT 2016* RCT discovers vitamin D may alleviate painful menstrual cramps Vitamin D Council, May 2016 *50 women, 31 had severe vitamin D deficiency (< 10 ng/ml) and 19 had moderate vitamin D deficiency (10-19 ng/ml).
50,000 IU weekly for 8 weeks
| Before | After | |
| Mild pain | 13 % | 96 % |
| Moderate pain | 70 % | 4 % |
| Severe pain | 17 % | 0 |
PMS supplements at Examine.com Jan 2020** The following is summary of a subset of their data. You must be a member to see the details__