Magnesium and Vitamin D – recent deficiencies, needed, synergistic - good overview 2017
Magnesium Supplementation in Vitamin D Deficiency
American Journal of Therapeutics 0, 1-9 (2017)
Pramod Reddy, MD and Linda R. Edwards, MD
📄 Download the PDF from Sci-Hub.tw via VitaminDWiki
Background: Vitamin D and magnesium (Mg) are some of the most studied topics in medicine with enormous implications for human health and disease. Majority of the adults are deficient in both vitamin D and magnesium but continue to go unrecognized by many health care professionals.
Areas of Uncertainty: Mg and vitamin D are used by all the organs in the body, and their deficiency states may lead to several chronic medical conditions. Studies described in the literature regarding these disease associations are contradictory, and reversal of any of these conditions may not occur for several years after adequate replacement. One should consider the supplementation therapy to be preventative rather than curative at this time.
Data Sources: PubMed search of several reported associations between vitamin D and Mg with diseases.
Results: Vitamin D and Mg replacement therapy in elderly patients is known to reduce the non- vertebral fractures, overall mortality, and the incidence of Alzheimer dementia.
Conclusions: Vitamin D screening assay is readily available, but the reported lower limit of the normal range is totally inadequate for disease prevention. Based on the epidemiologic studies, ~75% of all adults worldwide have serum 25(OH)D levels of <30 ng/mL. Because of the recent increase in global awareness, vitamin D supplementation has become a common practice, but Mg deficiency still remains unaddressed. Screening for chronic magnesium deficiency is difficult because a normal serum level may still be associated with moderate to severe deficiency. To date, there is no simple and accurate laboratory test to determine the total body magnesium status in humans. Mg is essential in the metabolism of vitamin D, and taking large doses of vitamin D can induce severe depletion of Mg . Adequate magnesium supplementation should be considered as an important aspect of vitamin D therapy.
INTRODUCTION
Magnesium (Mg) and vitamin D directly regulate bone and muscle metabolism throughout the life span of the musculoskeletal system and are also essential for the absorption of dietary calcium and phosphorus. Chronic vitamin D deficiency (VDD) and Mg deficiency are often associated with hypocalcemia. Chronic hypocalcemia may lead to secondary hyperparathyroidism and the resulting elevation in parathyroid hormone (PTH) increases the bone resorption in efforts to restore the serum calcium levels. This process may lead to a generalized decrease in bone mineral density, resulting in osteopenia and osteoporosis (osteodystrophy). Patients may present with bone pain, tenderness, muscle weakness, and difficulty walking with an increased risk of falls and fractures.
In this review article, we briefly discuss the homeostasis and interactions between Mg and vitamin D along with diagnostic and treatment options.
Mg HOMEOSTASIS
Recommended daily allowance (RDA) for men is 5-6 mg/kg body weight (eg, 70 kg male needs 350-400 mg of Mg) and 4-5 mg/kg body weight for women. Dietary intake of Mg is inadequate in most adults because the majority of the Mg is lost during food processing. Although drinking water accounts for ~10% of daily magnesium intake, food (spinach, nuts, and seeds) remain the richest source of Mg.1 Only approximately 30% of the total dietary magnesium is absorbed in the small intestine, but higher absorption is possible in deficiency states. Magnesium excretion is mainly regulated by the kidney, where 70% of the filtered Mg is reabsorbed in the thick ascending limb of the loop of Henle. Mg is critical for adenosine triphosphate (ATP) production, DNA/RNA synthesis, and glucose metabolism. Mg also serves as a cofactor for hundreds of metabolic reactions in the body, including the vitamin D metabolism. Mg is also essential for the regulation of blood pressure, cardiac excitability, nerve transmission, and neuromuscular conduction. 2-4
Normal levels of Mg
The adult human body contains approximately 24 g of magnesium mostly (99%) contained in the bone, muscles, and soft tissues. Only a small fraction of the total body magnesium is present in the serum, which do not accurately reflect the total body stores. A normal serum Mg level (1.5-2.5 meq/L) may still be associated with moderate to severe deficiency.5-7
Causes of magnesium deficiency in general population
Most adult humans do not get their recommended RDA via diet. Patients who are on chronic proton pump inhibitor therapy may develop magnesium deficiency from decreased absorption.8,9 Patients on chronic loop and thiazide diuretics may have increased renal Mg losses. Heavy alcohol consumption impairs the absorption and enhances the excretion of Mg. Consuming large doses of vitamin D products may induce depletion of Mg.
VITAMIN D HOMEOSTASIS
Vitamins are by definition organic compounds that cannot be synthesized by an organism but required to maintain good health. Vitamin D has been misclassified as a fat-soluble vitamin since its discovery in 1928, but it should be considered as a hormone because dermal synthesis is the major natural source.
Vitamin D is known to be utilized by the earliest life forms throughout the evolution for nearly a billion years.10 Vitamin D supplements are available in 2 natural inactive forms. Vitamin D2 (ergocalciferol) is not synthesized naturally in the body and fortified milk, and supplements are the main source. Vitamin D3 (cholecalciferol) is produced endogenously in human skin by ultraviolet (UV) radiation after sunlight exposure. Certain dietary sources (dried mushrooms, salmon) and vitamin supplements are also the sources of vitamin D3. Caucasians can generate approximately 20,000 IU of vitamin D3 after full-body exposure for 10-15 minutes. Prolonged exposure to sunlight does not produce toxic amounts of vitamin D3 because the excess precursors convert into biologically inactive compounds. The amount of vitamin D3 production varies with the amount of skin pigmentation, body mass, the amount of skin exposed, and the extent of UV protection, including clothing and sunscreens.
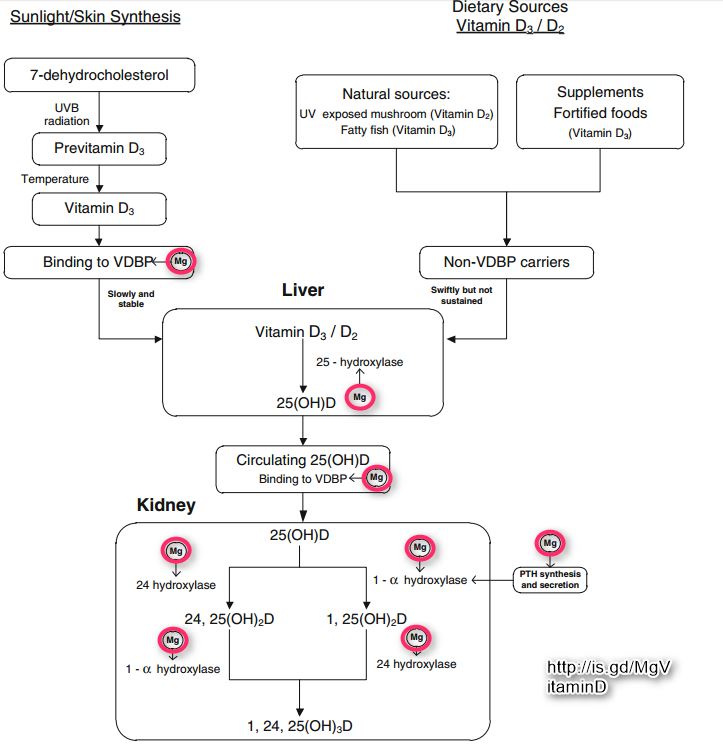
Absorbed inactive vitamin D is bound to vitamin D binding proteins in the circulation and requires 2 hydroxylations in the liver and kidney to become the active form of vitamin D (Figure 1). 25(OH)D serves as vitamin D reserve (4 weeks of half-life) in the body, and the 1,25(OH)2D is considered the active form of vitamin D (15 hours of half-life), which functions via the activation of the vitamin D receptors (VDRs) in the target tissues.11-13
Extrahepatic and extrarenal hydroxylations can occur in a number of tissues (pancreas, prostate, colon, skin, and osteoblasts), where intact vitamin D can be metabolized directly to the active hormone; for example, prostate cells and dermal keratinocytes are capable of both 25 and 1-alpha hydroxylation of the intact vitamin D.14-16 This local tissue ability to metabolize vitamin D is considered vital for the maintenance of tissue health, and VDD is implicated in the development of various diseases and cancers (Table 1). Most of these associations are unproven at this point, and there is a need for larger, randomized, multicenter studies.17
Vitamin D and Mg interactions
Several steps in the vitamin D metabolism depend on magnesium as a cofactor, such as vitamin D binding to vitamin D binding protein, 25(OH)D synthesis, 1,25 (OH)2D synthesis, 25-hydroxylase synthesis, and VDR expression for cellular effects (Figure 1). Mg deficiency can also decrease PTH synthesis and secretion and also the number of available VDRs in target cells.18-21 Serum 1,25(OH)2D concentrations frequently remain low in patients with Mg deficiency despite vitamin D intake22-24 Mg deficiency is also known to cause vitamin D-resistant hypocalcaemia, which can only be corrected after the proper replacement of Mg.
FIGURE 1. Vitamin D metabolism and Mg interaction.

Taking large doses of vitamin D without Mg replacement has been shown to induce atherosclerosis in swine coronary arteries.25
Causes of VDD in general population
Caucasians can generate approximately 20,000 IU of vitamin D3 after full-body exposure for 10-15 minutes. But, wearing a sunscreen (protection factor of 30) reduces vitamin D synthesis in the skin by more than 95%. Certain Caucasians have variable responsiveness to UV-B radiation, resulting in VDD despite abundant sun exposure. Cutaneous production of vitamin D also declines with age.26 Individuals with darker skin pigmentation may require 5-10 times more exposure to generate vitamin D compared with Caucasians. Obese patients may have decreased cutaneous synthesis of vitamin D. In chronic kidney disease (CKD) patients, active vitamin D production progressively declines with the course of the disease. Patients with malabsorption syndromes are often unable to absorb the fat-soluble vitamin D. Patients on anticonvulsants (eg, phenytoin) and antiretroviral medications enhance the catabolism of 25(OH)D and 1,25(OH)2D. Patients with chronic granulomatous disorders (sarcoidosis, tuberculosis, and chronic fungal infections), lymphomas, and primary hyperparathyroidism have increased metabolism of 25(OH)D to 1,25(OH)2D, which may lead to VDD.
ASSESSMENT OF VITAMIN D STATUS
Clinicians typically obtain vitamin D levels while evaluating patients with metabolic syndrome and fasting hyperglycemia. It is also a common practice to assess the vitamin D status in pregnancy, elderly patients, and patients with chronic medical conditions (diabetes, hypertension, chronic renal failure, and dyslipidemia). Diagnosing and treating VDD is beneficial in patients with statin myopathy because the majority of patients (87%-95%) may tolerate a statin rechallenge.27,28
The 25-hydroxy vitamin D level should always be the initial screening test in patients suspected to have VDD, which typically reflects the sum of 25 (OH)-D2 and 25(OH2)-D3, irrespective of the form of supplementation used by the patients. Results are reported either in nanograms/milliliter or nanomoles/liter, and the conversion factor from nanograms/milliliter to nanomoles/liter is about 2.5. For example, if patient's level is 30 ng/mL, multiplying it by 2.5 will convert to 75 in nanomoles per liter.
Serum vitamin D levels are typically reported by the laboratories with a range of 10-30 ng/mL. The lower limit of normal range reflects the necessary level to prevent the skeletal manifestations (eg, rickets), but it is totally inadequate for disease prevention.29,30 Based on the epidemiologic studies, approximately 75% of all adults worldwide have serum 25(OH)D levels of <30 ng/mL. A level of 30-40 ng/mL seems to be ideal for the prevention of premature mortality, depression, diabetes, metabolic syndrome, dyslipidemia, and cardiovascular disease. Much higher levels (50-80 ng/mL) are necessary to prevent dementia and certain malignancies. Most advantageous serum level for 25(OH)Dfor disease prevention is 60 ng/mL, which is the highest amount generated by the sun.31-33
Vitamin D replacement in general population
Oral dosing of vitamin D depends upon the nature and severity of the deficiency. Increase in serum 25(OH)D levels may occur more efficiently with D3 therapy compared with D2. Serum 25(OH)D levels may fall rapidly (14 days) to the baseline in patients treated with D2.34-36 Using vitamin D at intermittent mega doses (eg, 3,00,000 IU every 3 months) should be avoided because of increased fall and fracture risk in elderly patients.37-39 Daily doses of vitamin D3 starting at 5000 IU is widely available over the counter (OTC), which should be recommended for the patients. Vitamin D levels should be rechecked in 3-4 months, and the dose should be adjusted to achieve the most beneficial serum levels (60-80 ng/mL) for disease prevention. Once properly replenished, it is important to maintain the serum 25 (OH)D level without fluctuations. Noncompliance leading to sharp decline in tissue 1,25(OH)2D levels could increase the risk of certain cancers.40
Vitamin D replacement in patients with CKD and end-stage renal disease
Majority of end-stage renal disease (ESRD) patients suffer from both 25(OH)D deficiency and 1,25 (OH)2 D deficiency. Traditional vitamin D2/D3 agents can be used as the first therapy to treat secondary hyperparathyroidism associated with low circulating levels of 25-hydroxy vitamin D in stage-3 CKD patients. But, their use in patients with stage-4 CKD and ESRD may not significantly lower the PTH levels. The administration of active vitamin D (calcitriol or synthetic vitamin D analogs) is known to significantly lower the PTH levels and increase the survival in patients with ESRD. Calcitriol has a narrow therapeutic window because of the increased intestinal absorption of calcium and phosphorus, resulting in calciphylaxis. To counteract this effect, several synthetic analogues of active vitamin D have been developed that effectively suppresses PTH with minimal VDR activity in the intestine. All the synthetic vitamin D compounds are either D2 based (paricalcitol and doxercalciferol) or D3 based (maxacalcitol, alfacalcidol). It is considered beneficial to also elevate the 25(OH)D levels in patients taking active forms of vitamin D to facilitate the paracrine production in various tissues.40-42
ASSESSMENT OF THE Mg STATUS
Serum and red blood cell assays
Mg in the circulation exists in different compartments of the body (serum, erythrocytes, leukocytes, and thrombocytes). In the serum, magnesium circulates in either a free ionized form or protein/anion bound form. Ionized Mg is the biologically active form of Mg in the body, which can be measured either in the serum or within the red blood cells (RBC).
Total serum Mg assay
Serum Mg assays evaluate the protein bound fraction of Mg and levels are reported as 0.7-1.0 mmol/L (range, 1.7-2.4 mg/dL). Patients with normal serum Mg levels can be still intracellularly deficient.5-7 In patients with hypoalbuminemia, serum Mg assays may overestimate hypomagnesemia. Although serum calcium level can be corrected for hypoalbuminemia, there is no such calculation available for Mg correction.
Ionized serum Mg assay
Ionized magnesium in the serum has been studied extensively in critically ill patients with hypoalbumi- nemia. Hypomagnesemia in general is known to be associated with higher intensive care unit mortality.43
Total RBC Mg assay
RBC Mg levels are known to correlate with Mg levels in both the peripheral tissues and brain. Low RBC Mg levels (despite normal serum Mg levels) may negatively correlate with acute asthma exacerbation.44-46
Ionized RBC magnesium assay
This assay may provide reliable information on the functional magnesium status but not widely available.47
Intracellular Electrolytes and Magnesium test
Tissue scrapings from sublingual epithelial cells are tested for magnesium in this assay. Although the assay is noninvasive, it is not covered by health insurance and is expensive for out-of-pocket payments.
Magnesium tolerance test
Urinary magnesium levels are tested after an infused magnesium loading dose, and the patient is considered deficient when <80% of the magnesium is excreted into the urine. False positives are common in patients with malnutrition, diuretic use, diarrhea, CKD, and cirrhosis.
RECOMMENDATION
It is difficult to reliably diagnose chronic Mg deficiency with any of the currently available assays.48 It is easier to treat the patients with supplements when Mg deficiency is suspected.
CLINICALLY AVAILABLE Mg COMPOUNDS
Magnesium supplements are available as magnesium oxide, magnesium chloride, magnesium citrate, magnesium taurate, magnesium orotate, and amino acid chelates (Table 2).
Importance of elemental Mg
It may seem easy to meet the Mg daily allowance with a single tablet of magnesium oxide 400 mg, which is widely available OTC. But, RDA is based on absorbed quantity of elemental magnesium; for example, magnesium oxide 400 mg has only 241 mg of elemental Mg, out of which only 4%-20% is absorbed. Because only approximately 50 mg elemental Mg is absorbed even with the best possible absorption, patients may need to take 8 tablets to meet the daily requirements.
Table 2. Properties of commonly available magnesium supplements.

Mg supplements differ in the content of elemental Mg and bioavailability, but there is not sufficient evidence to suggest one form of Mg over another at this time.49-56 It is also important not to consume large quantities of Mg to meet the daily requirements. Patients should be encouraged to take 2-4 pills of any Mg preparation they can afford and tolerate along with a diet rich in Mg. Magnesium supplementation should be done cautiously in patients with moderate CKD with 50%-75% dose reductions. Mg supplementation should be avoided in patients with advanced CKD and ESRD.57
ADVERSE EFFECTS OF VITAMIN D AND Mg REPLACEMENT THERAPY
Early adverse effects
Most patients tolerate the vitamin D and Mg supplemental therapy without adverse effects. But, a small number of patients may develop new symptoms within the first week of initiating the therapy. Palpitations, low-grade fever, heat intolerance, dizziness, dry eyes, conjunctival erythema, coated tongue, dry mouth, and significantly increased thirst are reported by some patients. Patients report increased tendency for dehydration and may drink large quantities of water but without primary polyuria. Severe muscle cramps and tendon stiffness may occur in previously asymptomatic patients. Pain at the sites of old, healed, musculoskeletal injuries and tingling sensation of nerves are sometimes reported. Musculoskeletal symptoms are more pronounced in patients with statin myopathy who started the supplemental therapy.
Most of these clinical manifestations are not adequately explained by the current medical knowledge. One possible explanation is that human body adopts to vitamin D and Mg deficiency by downregulating several metabolic reactions, which are rapidly resumed after the replacement therapy. There is minimal correlation between the serum levels and clinical symptoms. For example, a patient with severe VDD (<10 ng/L) may remain asymptomatic before and after the replacement therapy, whereas patients with only mild deficiency (20 ng/L) may develop these symptoms. Some patients report recurrence of symptoms when new Mg supplements are added to isolated vitamin D therapy.
It can be frightening to the affected patients when muscle pains and fatigue occurs along with palpitations.58 They commonly undergo vigorous laboratory testing (eg, creatinine kinase, renal function panel), which usually reveal normal results. Screening tests for diabetes mellitus frequently reveal elevated fasting glucose levels and hemoglobin A1C levels up to 5.9, without postprandial hyperglycemia.
Physicians should have an open mind when patients report any new symptoms during the prescribed therapy. It is also a useful practice to inquire about the use of OTC vitamin D and Mg supplements when evaluating these patients. Symptoms gradually resolve in 3-6 months, and physicians should assure the patients about the benign nature of the condition. Patients should be encouraged to do daily walking and stretching of the affected limbs and gradual weight lifting exercises to avoid the tendon injury. Replacement therapy can be continued at lower doses, which is advised over completely stopping the therapy. Recurrence of these symptoms is common if patient chooses to stop the therapy and resume it at a later time.
Late adverse effects
Vitamin D toxicity
Serum 25(OH)D level of >150 ng/mL is a good threshold for identifying patients at the risk for developing toxicity.59,60 Toxicity is typically associated with hypercalcemia, hyperphosphatemia, low PTH, and hypercalciuria. Patients may manifest with severe bone pains and nephrolithiasis due to bone demineralization. When the serum calcium concentration exceeds 14 mg/dL, patients may present with confusion, polyuria, polydipsia, anorexia, vomiting, and muscle weakness. Emergent medical intervention is necessary to rapidly correct hypercalcemia to prevent mortality. Treatment typically includes aggressive saline hydration, calcitonin, bisphosphonates, and corticosteroids. Because the excess vitamin D is stored in adipose tissues, effects of toxicity may last for few months, and weekly monitoring of serum calcium levels are recommended.
Mg toxicity
Hypermagnesemia from Mg supplements is extremely rare but possible in patients with advanced CKD. Neuromuscular symptoms (muscle weakness, decreased tendon reflexes) occur commonly when the serum Mg level is more than 4.8 mg/dL. Severe hypermagnesemia can cause hypotension, complete heart block, and cardiac arrest. Administration of intravenous calcium along with cardiorespiratory support is needed until magnesium levels are reduced by hemodialysis.
