Diets lack micronutrients such as vitamin D
Note: This wiki page has 3 items. The original peer-reviewed paper and two papers which it referenced
Prevalence of micronutrient deficiency in popular diet plans
Jayson B Calton email
Department of Nutritional Research and Education, Calton Nutrition, North Venice, FL, USA
Journal of the International Society of Sports Nutrition 2010, 7:24doi:10.1186/1550-2783-7-24
The electronic version of this article is the complete one and can be found online at: http://www.jissn.com/content/7/1/24
Received: 26 April 2010; Accepted: 10 June 2010; Published: 10 June 2010; © 2010 Calton; licensee BioMed Central Ltd.
Background
Research has shown micronutrient deficiency to be scientifically linked to a higher risk of overweight/obesity and other dangerous and debilitating diseases. With more than two-thirds of the U.S. population overweight or obese, and research showing that one-third are on a diet at any given time, a need existed to determine whether current popular diet plans could protect followers from micronutrient deficiency by providing the minimum levels of 27 micronutrients, as determined by the U.S. Food and Drug Administrations (FDA) Reference Daily Intake (RDI) guidelines.
Methods
Suggested daily menus from four popular diet plans (Atkins for Life diet, The South Beach Diet, the DASH diet, the DASH diet) were evaluated. Calorie and micronutrient content of each ingredient, in each meal, were determined by using food composition data from the U.S. Department of Agriculture Nutrient Database for Standard Reference. The results were evaluated for sufficiency and total calories and deficient micronutrients were identified. The diet plans that did not meet 100% sufficiency by RDI guidelines for each of the 27 micronutrients were re-analyzed; (1) to identify a micronutrient sufficient calorie intake for all 27 micronutrients, and (2) to identify a second micronutrient sufficient calorie intake when consistently low or nonexistent micronutrients were removed from the sufficiency requirement.
Results
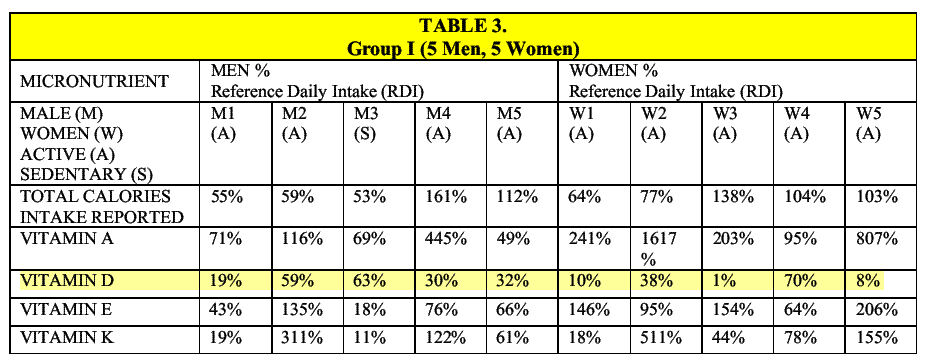
Analysis determined that each of the four popular diet plans failed to provide minimum RDI sufficiency for all 27 micronutrients analyzed. The four diet plans, on average, were found to be RDI sufficient in (11.75 ± 2.02; mean ± SEM) of the analyzed 27 micronutrients and contain (1748.25 ± 209.57) kcal. Further analysis of the four diets found that an average calorie intake of (27,575 ± 4660.72) would be required to achieve sufficiency in all 27 micronutrients. Six micronutrients (vitamin B7, vitamin D, vitamin E, chromium, iodine and molybdenum) were identified as consistently low or nonexistent in all four diet plans. These six micronutrients were removed from the sufficiency requirement and additional analysis of the four diets was conducted. It was determined that an average calorie content of (3,475 ± 543.81) would be required to reach 100% sufficiency in the remaining 21 micronutrients.
Conclusion
These findings are significant and indicate that an individual following a popular diet plan as suggested, with food alone, has a high likelihood of becoming micronutrient deficient; a state shown to be scientifically linked to an increased risk for many dangerous and debilitating health conditions and diseases.
A portion of one of the tables
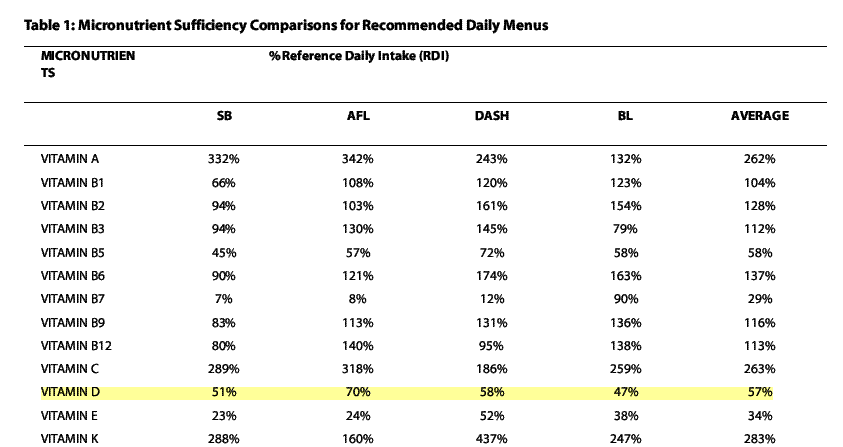
[tiki-download_file.php?fileId=1419]
Reference from the original paper: Obese children are vitamin D insufficient
Prevalence of vitamin D insufficiency in obese children and adolescents.
J Pediatr Endocrinol Metab. 2007 Jul;20(7):817-23.
Smotkin-Tangorra M, Purushothaman R, Gupta A, Nejati G, Anhalt H, Ten S.
Division of Pediatric Endocrinology, Infants and Children's Hospital of Brooklyn at Maimonides, NY 11219, USA. rit37@yahoo.com
OBJECTIVE: Recent studies have shown a broad prevalence of vitamin D deficiency in adults. Serum 25-hydroxyvitamin D (25-OHD) levels were reported to be inversely related to body mass index (BMI) and body fat content and correlated directly with hypertension, degree of insulin resistance and progression to diabetes mellitus. We sought to determine the prevalence of vitamin D insufficiency and markers of metabolic syndrome in an obese pediatric population.
METHODS: Charts of 217 obese (weight >95th percentile for age and sex) children (118 females, 99 males; mean BMI 32.2 +/- 6.4 kg/m2; mean age 12.9 2 5.5; age range 7-18 years) who had received a standard physical examination at the pediatric endocrine clinic of the Infants and Children's Hospital of Brooklyn at Maimonides, Brooklyn, NY, were retrospectively analyzed. Data obtained included age, sex, weight, BMI, height and systolic and diastolic blood pressure. The routine bloodwork panel for obesity at our pediatric endocrine facility includes fasting 25-OHD, total cholesterol, high density lipoprotein-cholesterol (HDL-C), low density lipoprotein-cholesterol (LDL-C), triglycerides, ALT, AST, thyroid stimulating hormone (TSH), total T4, and insulin and glucose. Insulin sensitivity as calculated by quantitative insulin-sensitivity check index (QUICKI = 1/[log(I0) + log(G0)], where I0 is fasting insulin and G0 is fasting glucose) was computed following the visit.
RESULTS: Overall, 55.2% of patients were vitamin D insufficient (25-OHD <20 ng/ml). Severely low vitamin D levels (25-OHD < or =10 ng/ml) were seen in 21.6% of 217 patients, which represents almost half of the insufficient group. In the 25-OHD <20 ng/ml group age, BMI, and SBP were significantly higher than in the 25-OHD 220 ng/ml group, while QUICKI (<0.35 is consistent with insulin resistance) was borderline low in the <20 ng/ml group. HDL-C was significantly lower in the 25-OHD < or =10 ng/ml group. The 25-OHD levels correlated negatively with BMI and positively with HDL-C. No other findings were significant.
CONCLUSION: More than half of the obese children had vitamin D levels <20 ng/ml with equal gender distribution. Vitamin D insufficiency was associated with increased age, BMI, and SBP, and decreased HDL-C. PMID: 17849744
Another reference from the original paper
Food Alone May Not Provide Sufficient Micronutrients for Preventing Deficiency -2006
[tiki-download_file.php?fileId=1421]