Calcium can create heart problems - vitamin D neutral
Vitamin D, Calcium, and Cardiovascular Mortality: A Perspective from a Plenary Lecture given at the Annual Meeting of the American Association of Clinical Endocrinologists.
Endocr Pract. 2011 Aug 19:1-30.
Miller PD. MillerCCBR@aol.com
ColoradoCenter for Bone Research, University of Colorado Health Sciences Center.
Objectives: To examine the data showing any associations between the serum levels of 25(OH) vitamin D, calcium intake and cardiovascular mortality.
Methods: The articles reviewed from the literature that form the basis of this authors opinion include published articles from 1992-2011 derived from search engines (PubMed; Scopus; MedScape) using search terms-vitamin D, calcium, cardiovascular events, cardiovascular mortality, all-cause mortality, vascular calcification, chronic-kidney disease, renal stones, hypercalciuria. Because these articles were not weighted (graded) on the level of evidence, this review reflects my own perspective on the data and how it should be applied in clinical management.
Results: Vitamin D and calcium replacement are fundamental nutrients. For skeletal health they are both needed to insure proper skeletal growth (modeling) and repair (remodeling). Nutritional deficiencies of either Vitamin D or calcium may lead to a spectrum of metabolic bone disorders. Excessive consumption of either nutrient has been linked to a variety of medical disorders, such as hypercalcemia or renal stones.
There have also been associations between Vitamin D or calcium intake and cardiovascular disease.
However, neither of these associations have established evidence nor known causality for increasing cardiovascular risk or all-cause mortality in patients with creatinine clearances > 60 ml/minute.
In patients with more severe chronic kidney disease, there is stronger data linking excess calcium (or phosphorus) intake and increase in vascular calcification but not mortality.
The upper safe level of intake for Vitamin D at least 4,000 IU/day and probably 10,000 IU/day and that for calcium are between 2,000 mg to 3,000 mg/day.
(VitaminDWiki has lots of data that disagrees, see below)
Conclusion: While there is no s olid scientific evidence validating that serum Vitamin D levels between 15-70 ng/ml are associated with any increased risk of CV disease , there is stronger but inconsistent evidence for an association between calcium supplementation greater than 500 mg/day and an increase in the risk for CV disease.
These data need validation by prospective, randomized, placebo-controlled trials. The "VITAL" randomized prospective study may provide more definitive answers to this question. Most professional societies, including AACE, suggest that replacement levels of these nutrients be individualized and to try to obtain and maintain a 25 (OH) D between 30-50 ng/mL and a calcium intake of 1200 mg/day including the consistent daily nutritional intake.
PMID: 21856593
[tiki-download_file.php?fileId=1966] if registered
See also VitaminDWiki
IoM again fails to look at interactions - Nov 2010 which has the following chart
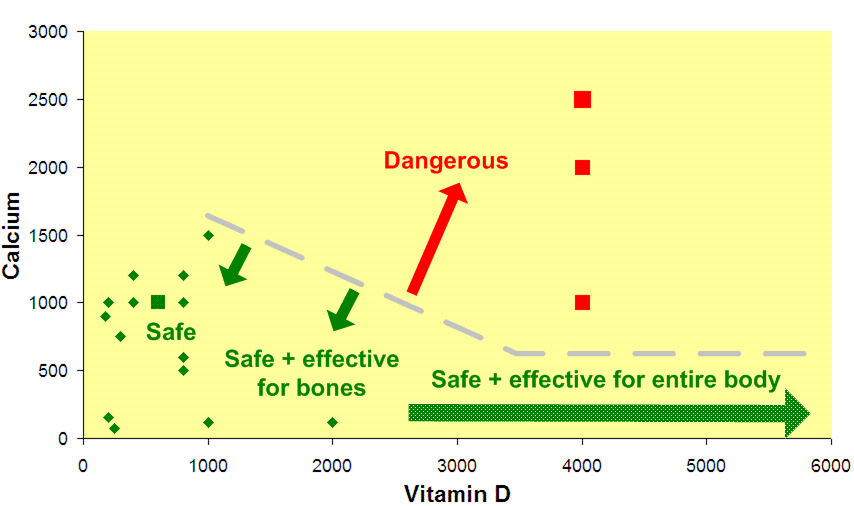
Supplements which combine vitamin D and Calcium (as of Jan-2010) = green diamonds
RDA of Vitamin D and Calcium is safe = green square
The Upper Limit for Vitamin D along with Calcium RDA or Upper Limit are dangerous
The problem: Increasing vitamin D increases the availability of Calcium to the body.
Various studies at the VitaminDWiki show problems with Calcium and Vitamin D above the dashed gray line
Large amount of vitamin D basically multiply the effect of the Calcium in the body by about 4X.
That is, the effect of 2,500 mg of Calcium with 4,000 IU of vitamin D is like taking 4X as much Calcium = 10,000 mg.
The excess Calcium is deposited in artery walls, kidney stones, and other places in the body.
2010 article by Miller PD
"Supplementation with calcium and vitamin D is recommended for all women aged 50 years and older."
