Bone marrow fat is suppressed by Vitamin D
It appears that
1) Bone Marrow is the 3rd largest fat store in the body
2) Vitamin D decreases Bone Marrow Fat
3)Bone Marrow Fat is associated with Osteoporosis
The Regulation of Marrow Fat by Vitamin D - Nov 2019
The Regulation of Marrow Fat by Vitamin D: Molecular Mechanisms and Clinical Implications - Nov 2019
Current Osteoporosis Reports, pp 1–11 DOI https://doi.org/10.1007/s11914-019-00546-6
Hanel Sadie-Van Gijsen
Purpose of Review
To review the available literature regarding a possible relationship between vitamin D and bone marrow adipose tissue (BMAT), and to identify future avenues of research that warrant attention.
Recent Findings
Results from in vivo animal and human studies all support the hypothesis that vitamin D can suppress BMAT expansion. This is achieved by antagonizing adipogenesis in bone marrow stromal cells, through inhibition of PPARγ2 activity and stimulation of pro-osteogenic Wnt signalling. However, our understanding of the functions of BMAT is still evolving, and studies on the role of vitamin D in modulating BMAT function are lacking. In addition, many diseases and chronic conditions are associated with low vitamin D status and low bone mineral density (BMD), but BMAT expansion has not been studied in these patient populations.
Summary: Vitamin D suppresses BMAT expansion, but its role in modulating BMAT function is poorly understood.
Bone Marrow Fat and production of blood cells (Hematopoiesis) - 2018
Front Endocrinol (Lausanne). 2018; 9: 694. doi: 10.3389/fendo.2018.00694
Huifang Wang,† Yamei Leng,† and Yuping Gong*
Bone marrow fat cells comprise the largest population of cells in the bone marrow cavity, a characteristic that has attracted the attention of scholars from different disciplines. The perception that bone marrow adipocytes are “inert space fillers” has been broken, and currently, bone marrow fat is unanimously considered to be the third largest fat depot, after subcutaneous fat and visceral fat . Bone marrow fat (BMF) acts as a metabolically active organ and plays an active role in energy storage, endocrine function, bone metabolism, and the bone metastasis of tumors. Bone marrow adipocytes (BMAs), as a component of the bone marrow microenvironment, influence hematopoiesis through direct contact with cells and the secretion of adipocyte-derived factors. They also influence the progression of hematologic diseases such as leukemia, multiple myeloma, and aplastic anemia, and may be a novel target when exploring treatments for related diseases in the future. Based on currently available data, this review describes the role of BMF in hematopoiesis as well as in the development of hematologic diseases.
📄 Download the PDF from VitaminDWiki
Hematopoiesis in Wikipedia__
Location of Blood cell production changes with age
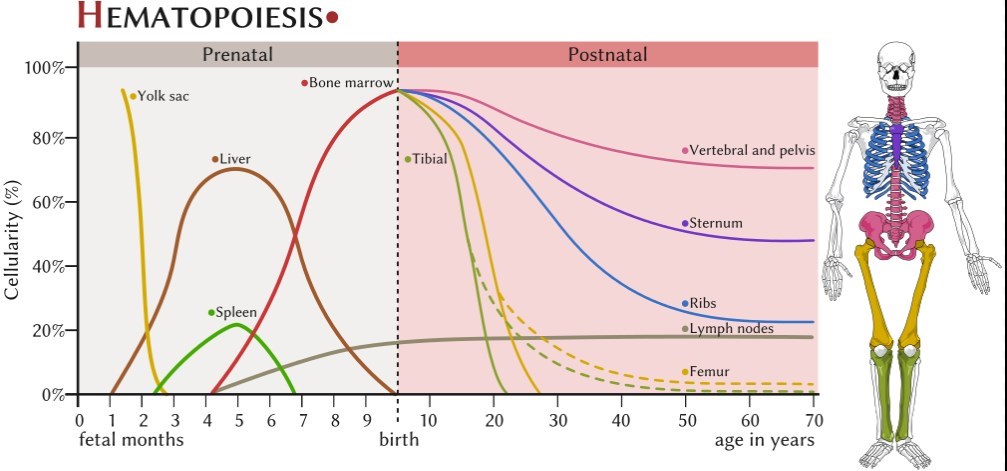
Bone marrow fat - July 2014
Joint Bone Spine, Volume 81, Issue 4, July 2014, Pages 313-319, https://doi.org/10.1016/j.jbspin.2014.02.013
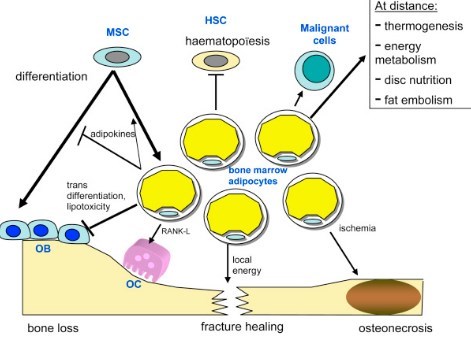
Bone marrow fat (BMF) results from an accumulation of fat cells within the bone marrow. Fat is not a simple filling tissue but is now considered as an actor within bone microenvironment. BMF is not comparable to other fat depots, as in subcutaneous or visceral tissues. Recent studies on bone marrow adipocytes have shown that they do not appear only as storage cells, but also as cells secreting adipokines, like leptin and adiponectin. Moreover bone marrow adipocytes share the same precursor with osteoblasts, the mesenchymal stem cell. It is now well established that high BMF is associated with weak bone mass in osteoporosis, especially during aging and anorexia nervosa. But numerous questions remain discussed: what is the precise phenotype of bone marrow adipocytes? What is the real function of BMF, and how does bone marrow adipocyte act on its environment? Is the increase of BMF during osteoporosis responsible for bone loss? Is BMF involved in other diseases? How to measure BMF in humans? A better understanding of BMF could allow to obtain new diagnostic tools for osteoporosis management, and could open major therapeutic perspectives.
Good, Bad, or Ugly: the Biological Roles of Bone Marrow Fat - Feb 2018
Current Osteoporosis Reports, April 2018, Volume 16, Issue 2, pp 130–137
Lakshman SinghSonia TyagiDamian MyersGustavo Duque Email author
Bone marrow fat expresses mixed characteristics, which could correspond to white, brown, and beige types of fat. Marrow fat could act as either energy storing and adipokine secreting white fat or as a source of energy for hematopoiesis and bone metabolism, thus acting as brown fat. However, there is also a negative interaction between marrow fat and other elements of the bone marrow milieu, which is known as lipotoxicity. In this review, we will describe the good and bad roles of marrow fat in the bone, while focusing on the specific components of the negative effect of marrow fat on bone metabolism.
Download the PDF from VitaminDWiki
References for 2019 study
1.
•• Hardouin P, Rharass T, Lucas S. Bone marrow adipose tissue: tTo be or not to be a typical adipose tissue? Front Endocrinol (Lausanne). 2016;7:85 This is the first formal description of bone marrow adipose tissue (BMAT) as a distinct adipose depot.
2.
Ambrosi TH, Schulz TJ. The emerging role of bone marrow adipose tissue in bone health and dysfunction. J Mol Med (Berl). 2017;95:1291–301.
3.
•• Craft CS, Li Z, MacDougald OA, Scheller EL. Molecular differences between subtypes of bone marrow adipocytes. Curr Mol Biol Rep. 2018;4:16–23 This paper provides a comprehensive description of the two subtypes of bone marrow adipocytes identified in animal models, and highlights future research questions.
4.
Sebo ZL, Rendina-Ruedy E, Ables GP, Lindskog DM, Rodeheffer MS, Fazeli PK, et al. Bone marrow adiposity: basic and clinical implications. Endocr Rev. 2019. https://doi.org/10.1210/er.2018-00138.
5.
Suchacki KJ, Cawthorn WP. Molecular interaction of bone marrow adipose tissue with energy metabolism. Curr Mol Biol Rep. 2018;4:41–9.
6.
Veldhuis-Vlug AG, Rosen CJ. Clinical implications of bone marrow adiposity. J Intern Med. 2018;283:121–39.
7.
Scheller EL, Khandaker S, Learman BS, Cawthorn WP, Anderson LM, Pham HA, et al. Bone marrow adipocytes resist lipolysis and remodeling in response to β-adrenergic stimulation. Bone. 2019;118:32–41.
8.
Horowitz MC, Berry R, Holtrup B, Sebo Z, Nelson T, Fretz JA, et al. Bone marrow adipocytes. Adipocyte. 2017;6:193–204.
9.
Li Y, Meng Y, Yu X. The unique metabolic characteristics of bone marrow adipose tissue. Front Endocrinol (Lausanne). 2019;10:69.
10.
Wang H, Leng Y, Gong Y. Bone marrow fat and hematopoiesis. Front Endocrinol (Lausanne). 2018;9:694.
11.
Luo G, He Y, Yu X. Bone marrow adipocyte: an intimate partner with tumor cells in bone metastasis. Front Endocrinol (Lausanne). 2018;9:339.
12.
Gimble JM, Zvonic S, Floyd ZE, Kassem M, Nuttall ME. Playing with bone and fat. J Cell Biochem. 2006;98:251–66.
13.
Sadie-Van Gijsen H, Crowther NJ, Hough FS, Ferris WF. The interrelationship between bone and fat: from cellular see-saw to endocrine reciprocity. Cell Mol Life Sci. 2013;70:2331–49.
14.
Sadie-Van Gijsen H, Hough FS, Ferris WF. Determinants of bone marrow adiposity: the modulation of peroxisome proliferator-activated receptor-γ2 activity as a central mechanism. Bone. 2013;56:255–65.
15.
• Tencerova M, Kassem M. The bone marrow-derived stromal cells: commitment and regulation of adipogenesis. Front Endocrinol (Lausanne). 2016;7:127 This review provides an update on the cellular and molecular mechanisms involved in regulating the competitive selection between adipogenesis and osteoblastogenesis in BMSCs.
16.
Justesen J, Stenderup K, Ebbesen EN, Mosekilde L, Steiniche T, Kassem M. Adipocyte tissue volume in bone marrow is increased with aging and in patients with osteoporosis. Biogerontology. 2001;2:165–71.
17.
He J, Fang H, Li X. Vertebral bone marrow fat content in normal adults with varying bone densities at 3T magnetic resonance imaging. Acta Radiol. 2019;60:509–15.
18.
Cortes ARG, Cohen O, Zhao M, Aoki EM, Ribeiro RA, Abu Nada L, et al. Assessment of alveolar bone marrow fat content using 15 T MRI. Oral Surg Oral Med Oral Pathol Oral Radiol. 2018;125:244–9.
19.
Bani Hassan E, Demontiero O, Vogrin S, Ng A, Duque G. Marrow adipose tissue in older men: association with visceral and subcutaneous fat, bone volume, metabolism, and inflammation. Calcif Tissue Int. 2018;103:164–74.
20.
Zhu L, Xu Z, Li G, Wang Y, Li X, Shi X, et al. Marrow adiposity as an indicator for insulin resistance in postmenopausal women with newly diagnosed type 2 diabetes—an investigation by chemical shift-encoded water-fat MRI. Eur J Radiol. 2019;113:158–64.
21.
Lips P, van Schoor NM. The effect of vitamin D on bone and osteoporosis. Best Pract Res Clin Endocrinol Metab. 2011;25:585–91.
22.
Topor LS, Melvin P, Giancaterino C, Gordon CM. Factors associated with low bone density in patients referred for assessment of bone health. Int J Pediatr Endocrinol. 2013;2013(1):4.
23.
Swanson CM, Srikanth P, Lee CG, Cummings SR, Jans I, Cauley JA, et al. Associations of 25-hydroxyvitamin D and 1,25-dihydroxyvitamin D with bone mineral density, bone mineral density change, and incident nonvertebral fracture. J Bone Miner Res. 2015;30:1403–13.
24.
Arunabh S, Pollack S, Yeh J, Aloia JF. Body fat content and 25-hydroxyvitamin D levels in healthy women. J Clin Endocrinol Metab. 2003;88:157–61.
25.
Parikh SJ, Edelman M, Uwaifo GI, Freedman RJ, Semega-Janneh M, Reynolds J, et al. The relationship between obesity and serum 1,25-dihydroxy vitamin D concentrations in healthy adults. J Clin Endocrinol Metab. 2004;89:1196–9.
26.
•• Pino AM, Miranda M, Figueroa C, Rodríguez JP, Rosen CJ. Qualitative aspects of bone marrow adiposity in osteoporosis. Front Endocrinol (Lausanne). 2016;7:139 This review discusses the emerging concept of the impact of marrow fat lipid composition, rather than marrow fat volume per se, on bone fragility.
27.
• Cordes C, Baum T, Dieckmeyer M, Ruschke S, Diefenbach MN, Hauner H, et al. MR-based assessment of bone marrow fat in osteoporosis, diabetes, and obesity. Front Endocrinol (Lausanne). 2016;7:74 This paper describes how MR-based methods can be applied to quantify BMAT lipid composition.
28.
Singhal V, Bredella MA. Marrow adipose tissue imaging in humans. Bone. 2019;118:69–76.
29.
Xu K, Sigurdsson S, Gudnason V, Hue T, Schwartz A, Li X. Reliable quantification of marrow fat content and unsaturation level using in vivo MR spectroscopy. Magn Reson Med. 2018;79:1722–9.
30.
Martel D, Leporq B, Bruno M, Regatte RR, Honig S, Chang G. Chemical shift-encoded MRI for assessment of bone marrow adipose tissue fat composition: pilot study in premenopausal versus postmenopausal women. Magn Reson Imaging. 2018;53:148–55.
31.
Martel D, Leporq B, Saxena A, Belmont HM, Turyan G, Honig S, et al. 3T chemical shift-encoded MRI: detection of altered proximal femur marrow adipose tissue composition in glucocorticoid users and validation with magnetic resonance spectroscopy. J Magn Reson Imaging. 2019;50:490–6.
32.
Zhu M, Hao G, Xing J, Hu S, Geng D, Zhang W, et al. Bone marrow adipose amount influences vertebral bone strength. Exp Ther Med. 2019;17:689–94.
PubMedPubMedCentralGoogle Scholar
33.
Scheller EL, Troiano N, Vanhoutan JN, Bouxsein MA, Fretz JA, Xi Y, et al. Use of osmium tetroxide staining with microcomputerized tomography to visualize and quantify bone marrow adipose tissue in vivo. Methods Enzymol. 2014;537:123–39.
34.
DeLuca HF. Overview of general physiologic features and functions of vitamin D. Am J Clin Nutr. 2004;80:1689S–96S.
35.
Geng S, Zhou S, Bi Z, Glowacki J. Vitamin D metabolism in human bone marrow stromal (mesenchymal stem) cells. Metabolism. 2013;62:768–77.
36.
Heaney RP, Recker RR, Grote J, Horst RL, Armas LA. Vitamin D(3) is more potent than vitamin D(2) in humans. J Clin Endocrinol Metab. 2011;96:E447–52.
37.
Romagnoli E, Pepe J, Piemonte S, Cipriani C, Minisola S. Management of endocrine disease: value and limitations of assessing vitamin D nutritional status and advised levels of vitamin D supplementation. Eur J Endocrinol. 2013;169:R59–69.
38.
Christakos S, Dhawan P, Liu Y, Peng X, Porta A. New insights into the mechanisms of vitamin D action. J Cell Biochem. 2003;88:695–705.
39.
Norman AW. Minireview: vitamin D receptor: new assignments for an already busy receptor. Endocrinology. 2006;147:5542–8.
PubMed
40.
Langub MC, Reinhardt TA, Horst RL, Malluche HH, Koszewski NJ. Characterization of vitamin D receptor immunoreactivity in human bone cells. Bone. 2000;27:383–7.
41.
Geng S, Zhou S, Glowacki J. Effects of 25-hydroxyvitamin D(3) on proliferation and osteoblast differentiation of human marrow stromal cells require CYP27B1/1α-hydroxylase. J Bone Miner Res. 2011;26:1145–53.
42.
Whitfield GK, Hsieh JC, Nakajima S, MacDonald PN, Thompson PD, Jurutka PW, et al. A highly conserved region in the hormone-binding domain of the human vitamin D receptor contains residues vital for heterodimerization with retinoid X receptor and for transcriptional activation. Mol Endocrinol. 1995;9:1166–79.
PubMedPubMedCentralGoogle Scholar
43.
Suda T, Ueno Y, Fujii K, Shinki T. Vitamin D and bone. J Cell Biochem. 2003;88:259–66.
44.
Atkins GJ, Anderson PH, Findlay DM, Welldon KJ, Vincent C, Zannettino AC, et al. Metabolism of vitamin D3 in human osteoblasts: evidence for autocrine and paracrine activities of 1 alpha,25-dihydroxyvitamin D3. Bone. 2007;40:1517–28.
45.
• Zhou S, LeBoff MS, Glowacki J. Vitamin D metabolism and action in human bone marrow stromal cells. Endocrinology. 2010;151:14–22 This article first demonstrated that BMSCs possess all of the molecular machinery required to produce and respond to calcitriol.
46.
Beresford JN, Joyner CJ, Devlin C, Triffitt JT. The effects of dexamethasone and 1,25-dihydroxyvitamin D3 on osteogenic differentiation of human marrow stromal cells in vitro. Arch Oral Biol. 1994;39:941–7.
47.
Piek E, Sleumer LS, van Someren EP, Heuver L, de Haan JR, de Grijs I, et al. Osteo-transcriptomics of human mesenchymal stem cells: accelerated gene expression and osteoblast differentiation induced by vitamin D reveals c-MYC as an enhancer of BMP2-induced osteogenesis. Bone. 2010;46:613–27.
48.
Kelly KA, Gimble JM. 1,25-Dihydroxy vitamin D3 inhibits adipocyte differentiation and gene expression in murine bone marrow stromal cell clones and primary cultures. Endocrinology. 1998;139:2622–8.
49.
Ding J, Nagai K, Woo JT. Insulin-dependent adipogenesis in stromal ST2 cells derived from murine bone marrow. Biosci Biotechnol Biochem. 2003;67:314–21.
50.
Kong J, Li YC. Molecular mechanism of 1,25-dihydroxyvitamin D3 inhibition of adipogenesis in 3T3-L1 cells. Am J Physiol Endocrinol Metab. 2006;290:E916–24.
51.
Atmani H, Chappard D, Basle MF. Proliferation and differentiation of osteoblasts and adipocytes in rat bone marrow stromal cell cultures: effects of dexamethasone and calcitriol. J Cell Biochem. 2003;89:364–72.
52.
Mahajan A, Stahl CH. Dihydroxy-cholecalciferol stimulates adipocytic differentiation of porcine mesenchymal stem cells. J Nutr Biochem. 2009;20:512–20.
53.
Zarei A, Hulley PA, Sabokbar A, Javaid MK, Morovat A. 25-hydroxy- and 1α,25-dihydroxycholecalciferol have greater potencies than 25-hydroxy- and 1α,25-dihydroxyergocalciferol in modulating cultured human and mouse osteoblast activities. PLoS One. 2016;11(11):e0165462.
54.
Duque G, Rivas D. Alendronate has an anabolic effect on bone through the differentiation of mesenchymal stem cells. J Bone Miner Res. 2007;22:1603–11.
55.
Duque G, Li W, Vidal C, Bermeo S, Rivas D, Henderson J. Pharmacological inhibition of PPARγ increases osteoblastogenesis and bone mass in male C57BL/6 mice. J Bone Miner Res. 2013;28:639–48.
56.
• Cianferotti L, Demay MB. VDR-mediated inhibition of DKK1 and SFRP2 suppresses adipogenic differentiation of murine bone marrow stromal cells. J Cell Biochem. 2007;101:80–8 This article identified stimulation of Wnt signalling as a mechanism whereby calcitriol could inhibit marrow adipogenesis.
57.
Nicolas V, Prewett A, Bettica P, Mohan S, Finkelman RD, Baylink DJ, et al. Age-related decreases in insulin-like growth factor-I and transforming growth factor-beta in femoral cortical bone from both men and women: implications for bone loss with aging. J Clin Endocrinol Metab. 1994;78:1011–6.
PubMedPubMedCentralGoogle Scholar
58.
Gómez JM. The role of insulin-like growth factor I components in the regulation of vitamin D. Curr Pharm Biotechnol. 2006;7:125–32.
59.
Wei S, Tanaka H, Seino Y. Local action of exogenous growth hormone and insulin-like growth factor-I on dihydroxyvitamin D production in LLC-PK1 cells. Eur J Endocrinol. 1998;139:454–60.
60.
Ameri P, Giusti A, Boschetti M, Bovio M, Teti C, Leoncini G, et al. Vitamin D increases circulating IGF1 in adults: potential implication for the treatment of GH deficiency. Eur J Endocrinol. 2013;169:767–72.
61.
Bredella MA, Gerweck AV, Barber LA, Breggia A, Rosen CJ, Torriani M, et al. Effects of growth hormone administration for 6 months on bone turnover and bone marrow fat in obese premenopausal women. Bone. 2014;62:29–35.
62.
Duque G, Macoritto M, Kremer R. 1,25(OH)2D3 inhibits bone marrow adipogenesis in senescence accelerated mice (SAM-P/6) by decreasing the expression of peroxisome proliferator-activated receptor gamma 2 (PPARgamma2). Exp Gerontol. 2004;39:333–8.
63.
Duque G, Rivas D, Li W, Li A, Henderson JE, Ferland G, et al. Age-related bone loss in the LOU/c rat model of healthy ageing. Exp Gerontol. 2009;44:183–9.
64.
Ambrosi TH, Scialdone A, Graja A, Gohlke S, Jank AM, Bocian C, et al. Adipocyte accumulation in the bone marrow during obesity and aging impairs stem cell-based hematopoietic and bone regeneration. Cell Stem Cell. 2017;20:771–84.
65.
Holick MF, Smith E, Pincus S. Skin as the site of vitamin D synthesis and target tissue for 1,25-dihydroxyvitamin D3. Use of calcitriol (1,25-dihydroxyvitamin D3) for treatment of psoriasis. Arch Dermatol. 1987;123:1677–83a.
66.
Montero-Odasso M, Duque G. Vitamin D in the aging musculoskeletal system: an authentic strength preserving hormone. Mol Asp Med. 2005;26:203–19.
67.
Geng S, Zhou S, Glowacki J. Age-related decline in osteoblastogenesis and 1α-hydroxylase/CYP27B1 in human mesenchymal stem cells: stimulation by parathyroid hormone. Aging Cell. 2011;10:962–71.
68.
Skversky AL, Kumar J, Abramowitz MK, Kaskel FJ, Melamed ML. Association of glucocorticoid use and low 25-hydroxyvitamin D levels: results from the National Health and Nutrition Examination Survey (NHANES): 2001-2006. J Clin Endocrinol Metab. 2011;96:3838–45.
69.
Mazziotti G, Formenti AM, Adler RA, Bilezikian JP, Grossman A, Sbardella E, et al. Glucocorticoid-induced osteoporosis: pathophysiological role of GH/IGF-I and PTH/VITAMIN D axes, treatment options and guidelines. Endocrine. 2016;54:603–11.
70.
Ghali O, Al Rassy N, Hardouin P, Chauveau C. Increased bone marrow adiposity in a context of energy deficit: the tip of the iceberg? Front Endocrinol (Lausanne). 2016;7:125.
71.
Veronese N, Solmi M, Rizza W, Manzato E, Sergi G, Santonastaso P, et al. Vitamin D status in anorexia nervosa: a meta-analysis. Int J Eat Disord. 2015;48:803–13.
72.
Pereira-Santos M, Costa PR, Assis AM, Santos CA, Santos DB. Obesity and vitamin D deficiency: a systematic review and meta-analysis. Obes Rev. 2015;16:341–9.
73.
Greco EA, Lenzi A, Migliaccio S. Role of hypovitaminosis D in the pathogenesis of obesity-induced insulin resistance. Nutrients. 2019:11(7).
Google Scholar
74.
Bouillon R, Bex M, Van Herck E, Laureys J, Dooms L, Lesaffre E, et al. Influence of age, sex, and insulin on osteoblast function: osteoblast dysfunction in diabetes mellitus. J Clin Endocrinol Metab. 1995;80:1194–202.
PubMedPubMedCentralGoogle Scholar
75.
Reichrath J. Dermatologic management, sun avoidance and vitamin D status in organ transplant recipients (OTR). J Photochem Photobiol B. 2010;101:150–9.
76.
Lai CY, Yang JY, Rayalam S, Della-Fera MA, Ambati S, Lewis RD, et al. Preventing bone loss and weight gain with combinations of vitamin D and phytochemicals. J Med Food. 2011;14:1352–62.
77.
• Duque G, Macoritto M, Kremer R. Vitamin D treatment of senescence accelerated mice (SAM-P/6) induces several regulators of stromal cell plasticity. Biogerontology. 2004;5:421–9 Combined, references 65 and 66 demonstrate that vitamin D suppress BMAT formation through upregulation of IGF-1 and downregulation of pro-adipogenic genes, including PPARγ2.
78.
Yang YJ, Zhu Z, Wang DT, Zhang XL, Liu YY, Lai WX, et al. Tanshinol alleviates impaired bone formation by inhibiting adipogenesis via KLF15/PPARγ2 signaling in GIO rats. Acta Pharmacol Sin. 2018;39:633–41.
79.
Maurice F, Dutour A, Vincentelli C, Abdesselam I, Bernard M, Dufour H, et al. Active Cushing syndrome patients have increased ectopic fat deposition and bone marrow fat content compared to cured patients and healthy subjects: a pilot 1H-MRS study. Eur J Endocrinol. 2018;179:307–17.
80.
Pereira RC, Delany AM, Canalis E. Effects of cortisol and bone morphogenetic protein-2 on stromal cell differentiation: correlation with CCAAT-enhancer binding protein expression. Bone. 2002;30:685–91.
81.
Compston J. Glucocorticoid-induced osteoporosis: an update. Endocrine. 2018;61:7–16.
82.
Badr S, Legroux-Gérot I, Vignau J, Chauveau C, Ruschke S, Karampinos DC, et al. Comparison of regional bone marrow adiposity characteristics at the hip of underweight and weight-recovered women with anorexia nervosa using magnetic resonance spectroscopy. Bone. 2019;127:135–45.
83.
Bredella MA, Torriani M, Ghomi RH, Thomas BJ, Brick DJ, Gerweck AV, et al. Vertebral bone marrow fat is positively associated with visceral fat and inversely associated with IGF-1 in obese women. Obesity (Silver Spring). 2011;19:49–53.
84.
Baum T, Yap SP, Karampinos DC, Nardo L, Kuo D, Burghardt AJ, et al. Does vertebral bone marrow fat content correlate with abdominal adipose tissue, lumbar spine bone mineral density, and blood biomarkers in women with type 2 diabetes mellitus? J Magn Reson Imaging. 2012;35:117–24.
85.
Yu EW, Greenblatt L, Eajazi A, Torriani M, Bredella MA. Marrow adipose tissue composition in adults with morbid obesity. Bone. 2017;97:38–42.
86.
De Araújo IM, Salmon CE, Nahas AK, Nogueira-Barbosa MH, Elias J Jr, de Paula FJ. Marrow adipose tissue spectrum in obesity and type 2 diabetes mellitus. Eur J Endocrinol. 2017;176:21–30.
87.
Tencerova M, Figeac F, Ditzel N, Taipaleenmäki H, Nielsen TK, Kassem M. High-fat diet-induced obesity promotes expansion of bone marrow adipose tissue and impairs skeletal stem cell functions in mice. J Bone Miner Res. 2018;33:1154–65.
88.
Tencerova M, Frost M, Figeac F, Nielsen TK, Ali D, Lauterlein JL, et al. Obesity-associated hypermetabolism and accelerated senescence of bone marrow stromal stem cells suggest a potential mechanism for bone fragility. Cell Rep. 2019;27:2050–62.
89.
• Mangan A, Le Roux CW, Miller NG, Docherty NG. Iron and vitamin D/calcium deficiency after gastric bypass: mechanisms involved and strategies to improve oral supplement disposition. Curr Drug Metab. 2019;20:244–52 This article provides evidence for increased prevalence of vitamin D deficiency after gastric bypass surgery, which is of clinical concern in an era where such surgery is increasingly used to treat morbid obesity.
90.
Kim TY, Schwartz AV, Li X, Xu K, Black DM, Petrenko DM, et al. Bone marrow fat changes after gastric bypass surgery are associated with loss of bone mass. J Bone Miner Res. 2017;32:2239–47.
91.
Bredella MA, Greenblatt LB, Eajazi A, Torriani M, Yu EW. Effects of Roux-en-Y gastric bypass and sleeve gastrectomy on bone mineral density and marrow adipose tissue. Bone. 2017;95:85–90.
92.
Patsch JM, Li X, Baum T, Yap SP, Karampinos DC, Schwartz AV, et al. Bone marrow fat composition as a novel imaging biomarker in postmenopausal women with prevalent fragility fractures. J Bone Miner Res. 2013;28:1721–8.
93.
Woods GN, Ewing SK, Sigurdsson S, Kado DM, Ix JH, Hue TF, et al. Chronic kidney disease is associated with greater bone marrow adiposity. J Bone Miner Res. 2018;33:2158–64.
94.
Hernandez MJ, Dos Reis LM, Marques ID, Araujo MJ, Truyts CAM, Oliveira IB, et al. The effect of vitamin D and zoledronic acid in bone marrow adiposity in kidney transplant patients: a post hoc analysis. PLoS One. 2018;13(5):e0197994.
95.
Stein EM, Cohen A, Freeby M, Rogers H, Kokolus S, Scott V, et al. Severe vitamin D deficiency among heart and liver transplant recipients. Clin Transpl. 2009;23:861–5.
96.
Anastasilakis AD, Tsourdi E, Makras P, Polyzos SA, Meier C, McCloskey EV, et al. Bone disease following solid organ transplantation: a narrative review and recommendations for management from The European Calcified Tissue Society. Bone. 2019;127:401–18.
97.
Kühne CA, Heufelder AE, Hofbauer LC. Bone and mineral metabolism in human immunodeficiency virus infection. J Bone Miner Res. 2001;16:2–9.
98.
Ahmad AN, Ahmad SN, Ahmad N. HIV infection and bone abnormalities. Open Orthop J. 2017;11:777–84.
99.
Cotter EJ, Ip HS, Powderly WG, Doran PP. Mechanism of HIV protein induced modulation of mesenchymal stem cell osteogenic differentiation. BMC Musculoskelet Disord. 2008;9:33.
100.
Butler JS, Dunning EC, Murray DW, Doran PP, O'Byrne JM. HIV-1 protein induced modulation of primary human osteoblast differentiation and function via a Wnt/β-catenin-dependent mechanism. J Orthop Res. 2013;31:218–26.
101.
Noe S, Moeckel CI, Schwerdtfeger C, Oldenbuettel C, Jaeger H, Wolf E, et al. Monthly or weekly supplementation with cholecalciferol 20,000 IU in people living with HIV: results from a nested cohort study. Interdiscip Perspect Infect Dis. 2018;2018:7502127.
102.
Haug CJ, Aukrust P, Haug E, Mørkrid L, Müller F, Frøland SS. Severe deficiency of 1,25-dihydroxyvitamin D3 in human immunodeficiency virus infection: association with immunological hyperactivity and only minor changes in calcium homeostasis. J Clin Endocrinol Metab. 1998;83:3832–8.
103.
Mayur N, Lewis S, Catherwood BD, Nanes MS. Tumor necrosis factor alpha decreases 1,25-dihydroxyvitamin D3 receptors in osteoblastic ROS 17/2.8 cells. J Bone Miner Res. 1993;8:997–1003.
104.
Fernandez-Martin JL, Kurian S, Farmer P, Nanes MS. Tumor necrosis factor activates a nuclear inhibitor of vitamin D and retinoid-X receptors. Mol Cell Endocrinol. 1998;141:65–72.
105.
• Nylén H, Habtewold A, Makonnen E, Yimer G, Bertilsson L, Burhenne J, et al. Prevalence and risk factors for efavirenz-based antiretroviral treatment-associated severe vitamin D deficiency: a prospective cohort study. Medicine (Baltimore). 2016;95(34):e4631 This article discusses the risk of vitamin D deficiency associated with efavirenz and TDF use, which is of clinical concern in a population that already presents with an infection-related burden of vitamin D deficiency.
PubMedCentral
106.
•• Conradie MM, van de Vyver M, Andrag E, Conradie M, Ferris WF. A direct comparison of the effects of the antiretroviral drugs Stavudine, Tenofovir and the combination Lopinavir/Ritonavir on bone metabolism in a rat model. Calcif Tissue Int. 2017;101:422–32 This article is the only study to date to provide evidence that certain ARVs may cause BMAT expansion in vivo.
107.
Hernandez-Vallejo SJ, Beaupere C, Larghero J, Capeau J, Lagathu C. HIV protease inhibitors induce senescence and alter osteoblastic potential of human bone marrow mesenchymal stem cells: beneficial effect of pravastatin. Aging Cell. 2013;12:955–65.
108.
Gaudio A, Morabito N, Catalano A, Rapisarda R, Xourafa A, Lasco A. Pathogenesis of thalassemia major-associated osteoporosis: a review with insights from clinical experience. J Clin Res Pediatr Endocrinol. 2019;11:110–7.
109.
Van den Berghe G, Van Roosbroeck D, Vanhove P, Wouters PJ, De Pourcq L, Bouillon R. Bone turnover in prolonged critical illness: effect of vitamin D. J Clin Endocrinol Metab. 2003;88:4623–32.
110.
Klein GL. The interaction between burn injury and vitamin D metabolism and consequences for the patient. Curr Clin Pharmacol. 2008;3:204–10.
111.
Murdaca G, Tonacci A, Negrini S, Greco M, Borro M, Puppo F, et al. Emerging role of vitamin D in autoimmune diseases: an update on evidence and therapeutic implications. Autoimmun Rev. 2019;102350.
Google Scholar
112.
Peterson CA, Heffernan ME. Serum tumor necrosis factor-alpha concentrations are negatively correlated with serum 25(OH)D concentrations in healthy women. J Inflamm (Lond). 2008;5:10.
113.
Fletcher J, Cooper SC, Ghosh S, Hewison M. The role of vitamin D in inflammatory bowel disease: mechanism to management. Nutrients 2019;11(5).
PubMedCentral
114.
Szafors P, Che H, Barnetche T, Morel J, Gaujoux-Viala C, Combe B, et al. Risk of fracture and low bone mineral density in adults with inflammatory bowel diseases. A systematic literature review with meta-analysis. Osteoporos Int. 2018;29:2389–97.
115.
Choi ST, Kwon SR, Jung JY, Kim HA, Kim SS, Kim SH, Kim JM, Park JH, Suh CH. Prevalence and fracture risk of osteoporosis in patients with rheumatoid arthritis: a multicenter comparative study of the FRAX and WHO criteria. J Clin Med. 2018;7(12).
PubMedCentral
116.
Xia J, Luo R, Guo S, Yang Y, Ge S, Xu G, et al. Prevalence and risk factors of reduced bone mineral density in systemic lupus erythematosus patients: a meta-analysis. Biomed Res Int. 2019;2019:3731648.
PubMedPubMedCentralGoogle Scholar
117.
Mutt SJ, Karhu T, Lehtonen S, Lehenkari P, Carlberg C, Saarnio J, et al. Inhibition of cytokine secretion from adipocytes by 1,25-dihydroxyvitamin D3 via the NF-κB pathway. FASEB J. 2012;26:4400–7.
118.
•• Jacobs FA, Sadie-Van Gijsen H, van de Vyver M, Ferris WF. Vanadate impedes adipogenesis in mesenchymal stem cells derived from different depots within bone. Front Endocrinol (Lausanne). 2016;7:108 In this article, we identified two separate MSC populations in the rat femur, with different adipogenic potential, which may have distinct contributions to BMAT expansion.
119.
Li Y, Bäckesjö CM, Haldosén LA, Lindgren U. Species difference exists in the effects of 1alpha,25(OH)(2)D(3) and its analogue 2-methylene-19-nor-(20S)-1,25-dihydroxyvitamin D(3) (2MD) on osteoblastic cells. J Steroid Biochem Mol Biol. 2008;112:110–6.
120.
Wiberg K, Ljunghall S, Binderup L, Ljunggren O. Studies on two new vitamin D analogs, EB 1089 and KH 1060: effects on bone resorption and osteoclast recruitment in vitro. Bone. 1995;17:391–5.
121.
Hou QK, Huang YQ, Luo YW, Wang B, Liu YM, Deng RD, et al. (+)-Cholesten-3-one induces osteogenic differentiation of bone marrow mesenchymal stem cells by activating vitamin D receptor. Exp Ther Med. 2017;13:1841–9.
122.
Peräkylä M, Malinen M, Herzig KH, Carlberg C. Gene regulatory potential of nonsteroidal vitamin D receptor ligands. Mol Endocrinol. 2005;19:2060–73.
123.
• Montazeri-Najafabady N, Ghasemi Y, Dabbaghmanesh MH, Talezadeh P, Koohpeyma F, Gholami A. Supportive role of probiotic strains in protecting rats from ovariectomy-induced cortical bone loss. Probiotics Antimicrob Proteins. 2018. https://doi.org/10.1007/s12602-018-9443-6These findings suggest that specific gut microbiota populations may provide support in maintaining or correcting vitamin D status.
124.
• Fairfield H, Falank C, Harris E, Demambro V, McDonald M, Pettitt JA, et al. The skeletal cell-derived molecule sclerostin drives bone marrow adipogenesis. J Cell Physiol. 2018;233:1156–67 This article identifies sclerostin, another Wnt inhibitor, as a driver of BMAT expansion, similar to the Wnt inhibitors identified in reference 56.
125.
•• Fairfield H, Falank C, Farrell M, Vary C, Boucher JM, Driscoll H, et al. Development of a 3D bone marrow adipose tissue model. Bone. 2019;118:77–88 This model may fundamentally change the way that we study BMAT function in vitro.
