Indoor workers have lower vitamin D levels than outdoor workers, unless lead smelter
Vitamin D levels and deficiency with different occupations: a systematic review.
BMC Public Health. 2017 Jun 22;17(1):519. doi: 10.1186/s12889-017-4436-z.
 click on image for details
click on image for details
📄 Download the PDF from VitaminDWiki
Sowah D1, Fan X1, Dennett L2, Hagtvedt R3, Straube S4.
1 Division of Preventive Medicine, Department of Medicine, University of Alberta, 5-30 University Terrace, 8303-112 Street, Edmonton, AB, T6G 2T4, Canada.
2 JW Scott Health Sciences Library, University of Alberta, Edmonton, Canada.
3 Department of Accounting, Operations and Information Systems, School of Business, University of Alberta, Edmonton, Canada.
4 Division of Preventive Medicine, Department of Medicine, University of Alberta, 5-30 University Terrace, 8303-112 Street, Edmonton, AB, T6G 2T4, Canada. straube@ualberta.ca.
BACKGROUND:
Vitamin D deficiency is prevalent worldwide, but some groups are at greater risk. We aim to evaluate vitamin D levels in different occupations and identify groups vulnerable to vitamin D deficiency.
METHODS:
An electronic search conducted in Medline, Embase, the Cochrane Central Register of Controlled Trials, and CINAHL Plus with Full Text generated 2505 hits; 71 peer-reviewed articles fulfilled the inclusion criteria. Occupations investigated included outdoor and indoor workers, shiftworkers, lead/smelter workers, coalminers, and healthcare professionals. We calculated the pooled average metabolite level as mean ± SD; deficiency/insufficiency status was described as % of the total number of subjects in a given category.
RESULTS:
Compared to outdoor workers, indoor workers had lower 25-hydroxyvitamin D (25-(OH)D) levels (40.6 ± 13.3 vs. 66.7 ± 16.7 nmol/L; p < 0.0001). Mean 25-(OH)D levels (in nmol/L) in shiftworkers, lead/smelter workers and coalminers were 33.8 ± 10.0, 77.8 ± 5.4 and 56.6 ± 28.4, respectively. Vitamin D deficiency (25-(OH)D < 50 nmol/L), was high in shiftworkers (80%) and indoor workers (78%) compared to outdoor workers (48%). Among healthcare professionals, medical residents and healthcare students had the lowest levels of mean 25-(OH)D, 44.0 ± 8.3 nmol/L and 45.2 ± 5.5 nmol/L, respectively. The mean 25-(OH)D level of practising physicians, 55.0 ± 5.8 nmol/L, was significantly different from both medical residents (p < 0.0001) and healthcare students (p < 0.0001). Nurses and other healthcare employees had 25-(OH)D levels of 63.4 ± 4.2 nmol/L and 63.0 ± 11.0 nmol/L, respectively, which differed significantly compared to practising physicians (p = 0.01), medical residents (p < 0.0001) and healthcare students (p < 0.0001). Rates of vitamin D deficiency among healthcare professionals were: healthcare students 72%, medical residents 65%, practising physicians 46%, other healthcare employees 44%, and nurses 43%. Combined rates of vitamin D deficiency or insufficiency (25-(OH)D < 75 nmol/L) were very high in all investigated groups. Potential confounders such as gender and body composition were not consistently reported in the primary studies and were therefore not analyzed. Furthermore, the descriptions of occupational characteristics may be incomplete. These are limitations of our systematic review.
CONCLUSIONS:
Our review demonstrates that shiftworkers, healthcare workers and indoor workers are at high risk to develop vitamin D deficiency, which may reflect key lifestyle differences (e.g. sunlight exposure). This may help target health promotion and preventive efforts.
PMID: 28637448 PMCID: PMC5480134 DOI: 10.1186/s12889-017-4436-z
Interestingly - Outdoor workers Vitamin D levels peaked in the winter
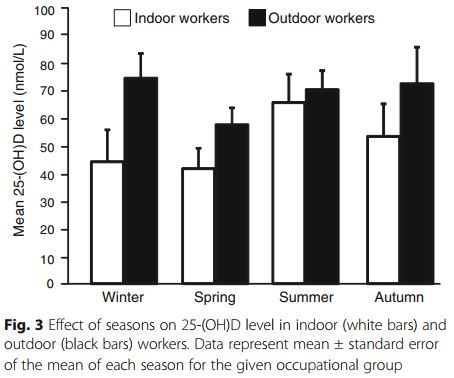
Clipped from PDF
Lead exposure, either short- or long-term, has the potential to influence the metabolism of vitamin D [77, 78]. The impact of lead on serum 1α, 25-(OH)2D levels is attributed to the inhibitory effect of lead on cytochrome P450 in the proximal tubules of the kidney, which mediates the hydroxylation of 25-(OH)D to the dihydroxy metabolite. In adults occupationally exposed to lead [78], Mason et al. demonstrated increased serum 1α, 25-(OH)2D levels in lead-exposed workers compared with a referent group who were not occupationally exposed to lead. In contrast, Greenberg et al. [79] did not demonstrate any effect of lead exposure on serum 1α, 25-(OH)2D levels.
Supplemental files such as the following chart
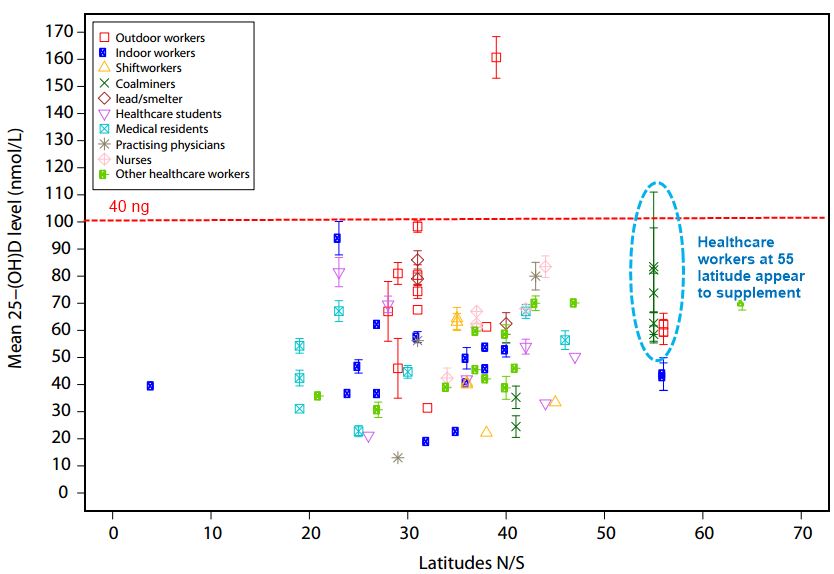
It appears that healthcare workers at 55 N latitude supplement
Perhaps it is in Edmonton Canada, where a philantropist has been promoting the use of vitamin D
