Middle ear infection (Otitis Media) and Vitamin D – many studies
Better results following Otitis Media surgery in those having higher levels of Vitamin D - Sept 2025
Vitamin D: A Factor affecting the Success of Type 1 Tympanoplasty
Ear Nose Throat J. 2025 Sep;104(9):NP638-NP642. doi: 10.1177/01455613221137224
Mehmet Kelleş 1, Yavuz Guler 2, Rukiye Guler 3
ObjectivesVitamin D (VD) plays role in wound healing and protection against infections. The relationship between plasma VD level and the outcomes of Type 1 tympanoplasty (T1T) has not been studied before.
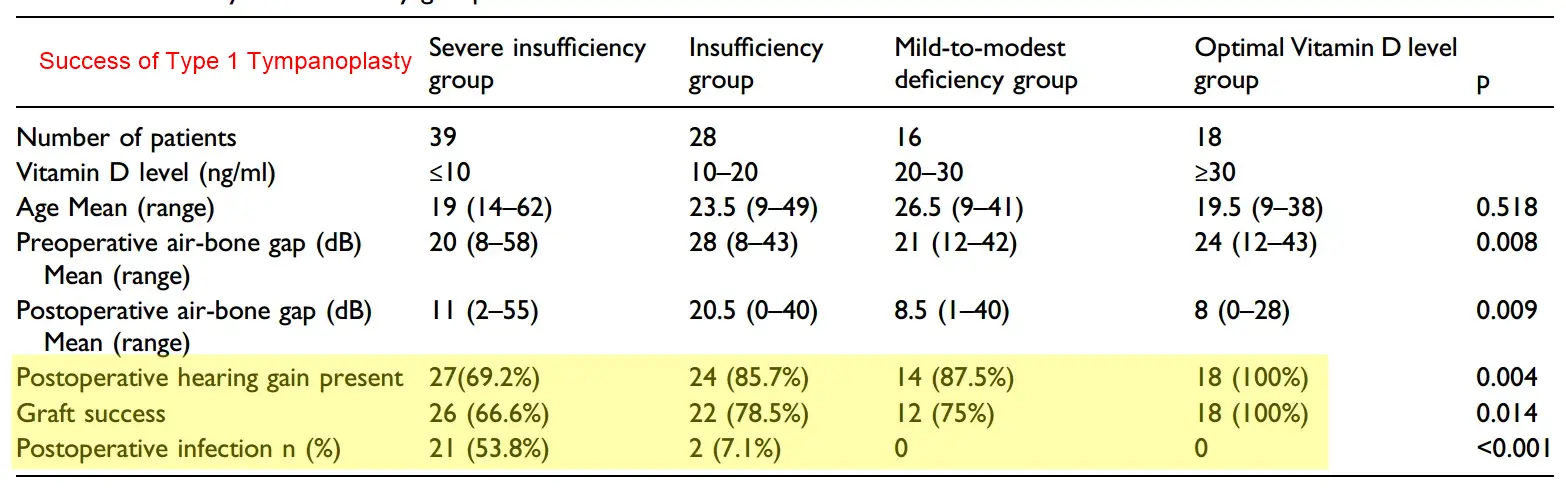
MethodsA total of 101 patients with chronic otitis media scheduled for T1T were divided into four groups in relation with their VD levels as severe insufficiency, insufficiency, mild-to-modest deficiency and optimal VD level groups. Graft success, hearing improvement and postoperative infection rates were compared among the groups in 12-month follow-up period.
ResultsThe graft success rate (P = 0.014) and air-bone gap gain (P = 0.004) were significantly higher, and postoperative infection rate was significantly lower (P < 0.001) in optimal VD level group.
Conclusion25-OH VD deficiency should be considered as a factor for failure in T1T. VD replacement may increase success of tympanoplasty in patients with low preoperative serum VD levels.
📄 Download the PDF from VitaminDWiki
--
Association between vitamin D and ear disease: a meta-analysis and systematic review - Feb 2022
The Egyptian Journal of Otolaryngology (2022) 38:27 https://doi.org/10.1186/s43163-022-00199-w
Marzouqi Salamah, Abdullah Alghamdi, Khalid Mania, Rawan Almahyawi, Haya Alsubaie, Mohamad Alfarghal & Mohammed Algarni
Background
Vitamin D deficiency is a suggested cause and risk factor for various ear diseases. This review assessed the role of vitamin D in ear diseases such as otitis media (OM); this study aimed to assess potential relationships between serum vitamin D level and OM risk; and determined the usefulness of vitamin D supplementation for ear disease prevention and treatment.
Material and methods
This systematic review searched the PubMed, EMBASE, Google Scholar, Web of Science, and the Cochrane Database for studies on vitamin D deficiency as a risk factor for ear diseases.
A total of 55 articles were screened based on their titles.
The abstracts were then reviewed to identify the 11 articles analyzed in the present study.
Results
Statistical heterogeneity was observed among the 11 studies for subgroup analysis of plasma vitamin D level according to disease type (
acute otitis media [AOM], P < 0.00001;
chronic otitis media [COM], P = 0.00001) and
age (≤ 5 years, P < 0.00001; > 5 years, P < 0.00001).
Heterogeneity was also observed in the frequency of participants with sufficient plasma vitamin D levels according to disease type (AOM, P < 0.00001; COM, P = 0.00001) and age (≤ 5 years, P < 0.00001; > 5 years, P = 0.003; I2 = 70%: substantial heterogeneity).
Conclusion
Vitamin D deficiency is common in otolaryngology patients, for which supplementation showed promising results. Vitamin D deficiency was associated with the etiopathology of ear diseases in adults and children. We recommend empirical supplementation of vitamin D in otolaryngology patients and further studies investigating this supplementation .
📄 Download the PDF from VitaminDWiki
Vitamin D seems promising for Otitis Media - Review July 2019
Vitamin D and Otitis Media
Current Allergy and Asthma Reports, July 2019, https://doi.org/10.1007/s11882-019-0866-2
Rebecca E. Walker Email author Jim Bartley Carlos A. Camargo Jr Edwin A. Mitchell
Purpose of Review: To examine the relationship between vitamin D and otitis media.
Recent Findings” Vitamin D deficiency has been associated with several respiratory diseases, including otitis media. Vitamin D supplementation may reduce the risk of otitis media. This relationship may be explained by vitamin D supporting the immune system by upregulating antimicrobial peptides which are effective against otopathogens and biofilm formation, supporting a less inflammatory immune response, or promoting beneficial commensal bacteria.
Summary” This review will explore risk factors of both otitis media and vitamin D deficiency, the evidence of vitamin D being beneficial for various forms of otitis media, and possible mechanisms of action.
Conclusion
Several studies have found that low concentrations of serum 25(OH)D are a risk factor for COME, AOM, and RAOM. However, studies to date do not indicate that low 25(OH)D concentration is a risk factor for CSOM. There has only been one RCT of vitamin D supplementation, which reported that it may be beneficial for AOM, but did not help reduce the risk of suppuration.
These findings place vitamin D as having a promising, but far from definitive, link with OM. In particular, more RCTs on the effects of vitamin D supplementation on the risk of thevarious forms of OM are needed, especially in at-risk children. Vitamin D supplementation alone is unlikely to present a “cure” for OM, but it could form part of a programme of treatment to improve the immune response against URI and pathogen overgrowth, in addition to existing interventions such as antibiotics, vaccines, and surgery.

📄 Download the PDF from Sci-Hub via VitaminDWiki
Vitamin D Supplementation Reduces the Risk of Acute Otitis Media in Otitis-Prone Children - 2013
Pediatr Infect Dis J. 2013 May 20.
Marchisio P, Consonni D, Baggi E, Zampiero A, Bianchini S, Terranova L, Tirelli S, Esposito S, Principi N.
1 Pediatric Clinic 1, Dept of Pathophysiology and Transplantation, Università degli Studi di Milano, Fondazione IRCCS Ca' Granda Ospedale Maggiore Policlinico, Milan, Italy;
2 Epidemiology Unit, Dept of Preventive Medicine, Fondazione IRCCS Ca' Granda Ospedale Maggiore Policlinico, Milan, Italy;
3 Laboratory Medicine Unit, Fondazione IRCCS Ca' Granda Ospedale Maggiore Policlinico, Milan, Italy.
BACKGROUND: The aim of this study was to evaluate whether a deficit in vitamin D (VD) is associated with an increased risk of recurrent acute otitis media (rAOM), and whether VD supplementation is effective in reducing the number of AOM episodes in otitis-prone children.
METHODS: A total of 116 children with a history of rAOM (≥3 episodes in preceding six months, or ≥4 episodes in preceding 12 months) were prospectively and blindly randomized to receive oral VD 1,000 IU/day or placebo for 4 months. Episodes of AOM were monitored for 6 months.
RESULTS: Fifty-eight children received placebo and 58 with similar characteristics were treated with VD. The number of children experiencing ≥1 AOM episode during the study period was significantly lower in the treatment group (26 vs 38; p=0.03). There was a marked difference in the number of children who developed uncomplicated AOM (p<0.001), but no difference in the number of children with ≥1 episode of spontaneous otorrhea. The likelihood of AOM was significantly reduced in the patients whose serum VD concentrations were ≥30 ng/mL.
CONCLUSIONS: VD hypovitaminosis is common in children with rAOM and associated with an increase in the occurrence of AOM when serum 25(OH)D levels are <30 ng/mL. The administration of VD in a dosage of 1,000 IU/day restores serum values of ≥30 ng/mL in most cases and is associated with a significant reduction in the risk of uncomplicated AOM.
8 minute video by one of the authors
Summary 2013 study by VitaminDWiki
58 pairs of children who tended to get middle ear infection
26 got infection with vitamin D
38 got infection with placebo
Thus ~ 30% reduction in middle ear infection with 1,000 IU of vitamin D
Comment on 2013 study by VitaminDWiki: Even fewer ear infections if had
Started with a loading dose, thus eliminating about 3 months of ear infections. (guess 45% instead of 30%)
Used a large dose of vitamin D (guess 70% if had used 2,000 IU of vitamin D)
Focused on high-risk children: dark skins. high latitude, etc. (guess 70% instead of 30%)
121 publications referred to this study as of Oct 2022
See also VitaminDWiki
Vitamin D Deficiency associated with Eardrum Perforation Risk – May 2012
Many infant infections avoided with supplementation with 400 IU of vitamin D – Oct 2012
Ear category listing has items
Third study found that Infants needed 1600 IU of vitamin D – JAMA RCT May 2013
Infants receiving 1600 IU of vitamin D were safe and healthy – RCT Aug 2012
Proof that Vitamin D Works this study was the 28th health problem proof
See also web
Association between vitamin D and ear disease: a meta-analysis and systematic review - Feb 2022 - https://doi.org/10.1186/s43163-022-00199-w FREE PDF
Vitamin D levels in children with otitis media with effusion - Oct 2021 - https://doi.org/10.1093/qjmed/hcab094.017 FREE PDF
Serum vitamin D levels in children with recurrent otitis media March 2013
- Added vitamin D, dropped from 4+ per year for 84 children (the definition of recurrent) to only 5 children with 1 and 1 child with 2
- Preview does not indicate amount of vitamin D, ut it appears that they were trying to have a level > 30 ng
- Acute Otitis Media Medscape Update, Dec 2013
- Describes diagnosis then treatment by antibiotics, No mention of vitamin D
- Medical prevention of recurrent acute otitis media: an updated overview March 2014
- Image from the web

- Influence of Vitamin D Deficiency on Progression of Experimental Otitis Media in Rats June 2018
- Confirmed in rats - free PDF online
13% less likely to get chronic otitis media for each 4 ng higher level of Vitamin D - Sept 2017
Higher serum 25(OH)D concentration is associated with lower risk of chronic otitis media with effusion: a case-control study.
Acta Paediatr. 2017 Sep;106(9):1487-1492. doi: 10.1111/apa.13908
Walker RE1, Bartley J2, Camargo CA Jr3,4, Flint D2, Thompson JMD1, Mitchell EA1.
More likely to get otitis media with effusion as well as less likely to recover if low vitamin D - Feb 2018
Clinical role of vitamin D in prognosis of otitis media with effusion.
Int J Pediatr Otorhinolaryngol. 2018 Feb;105:1-5. doi: 10.1016/j.ijporl.2017.11.030
Akcan FA1, Dündar Y2, Akcan HB3, Uluat A4, Cebeci D5, Sungur MA6, Ünlü İ5.
OBJECTIVE: To investigate the clinical role of Vitamin D in prognosis of Otitis media with effusion.
METHODS:
This prospective-controlled study was conducted at otolaryngology department in Duzce University, Turkey. The study group comprised children who were diagnosed with Otitis media with effusion between September 2016 and February 2017. Control group was conducted with children underwent circumcision or inguinal hernia repair operations that confirmed with ENT examination they do not have any sign of otitis media. After 3 months of follow-up without any treatment, unresolved cases who were accepted as chronic otitis media with effusion were operated under general anesthesia for ventilation tube application. Study and control groups were assessed depending on the serum 25(OH)Vitamin D levels at the end of 3 months; < 15 ng/mL was accepted as vitamin D deficiency. The results were compared with the control group in terms of vitamin D levels. Also, subgroup analysis was performed addressing to the complete recovery otitis media with effusion and chronic otitis media with effusion.
RESULTS:
One-hundred-seventy-four children with otitis media with effusion and 80 control patients were included to the study. One-hundred-eight (62%) out of 174 patients with otitis media with effusion was completely recovered after a 3-months follow up. Of those 66 out of 174 children, they had persistent diseases, underwent ventilation tube insertion after a 3-months follow-up. The mean 25(OH)Vitamin D level was 18.98 ± 10.60 in otitis media with effusion group and 28.07 ± 14.10 in control group and the difference was statistically significant between the study and control group (p < 0.001). Vitamin D deficiency was observed in 33 out of 66 patients (50.0%) in chronic otitis media with effusion group whilst 35 out of 108 patients (32.4%) in complete recovery otitis media with effusion group (p = 0.021). The rate of 25(OH)Vitamin D deficiency was 25% in control group which was statistically different from chronic otitis media with effusion and recovery chronic otitis media with effusion groups (p = 0.006).
CONCLUSIONS:
This study not only shows the relationship between Vitamin D and otitis media with effusion development, but also demonstrates the effects of Vitamin D on otitis media with effusion prognosis. There is a significant association between 25(OH)Vitamin D deficiency and follow-up outcomes of otitis media with effusion.
AIM:
Vitamin D supplementation and higher 25(OH)-vitamin D concentration are associated with reduced risk of acute respiratory infection. This study examined whether there is a similar association between higher serum 25(OH)D concentration and lower risk of chronic otitis media with effusion (COME).
METHODS:
In a case-control study, serum 25(OH)D concentration in children referred for tympanostomy tube placement for COME (n = 178) was compared to that of healthy children randomly sampled from primary care practices (n = 179). Subjects aged three and four years were recruited in Auckland, New Zealand between May 2011 and November 2013. Blood samples were collected from the children, and their guardians were interviewed. Odds ratios were calculated using logistic regression.
RESULTS:
In a multivariable analysis, higher serum 25(OH)D concentration was associated with a lower risk of COME (OR: 0.86 per 10 nmol/L; 95% CI 0.77-0.97) after adjusting for age, sex, deprivation index, ethnicity, tobacco smoke exposure, duration of breastfeeding and season of blood sampling. Further adjustment for eight additional risk factors did not change the result.
CONCLUSION:
This finding supports further investigation into whether the risk of COME could be reduced by increasing serum 25(OH)D concentration through increased sun exposure, higher dietary intake or vitamin D supplementation.
International Consensus on otitis media with effusion does not contain the word VITAMIN - Feb 2018
International consensus (ICON) on management of otitis media with effusion in children
". There was a clear international recommendation against using steroids, antibiotics, decongestants or antihistamines to treat OME, because of side-effects, cost issues and no convincing evidence of long-term effectivenes"
Meta-analysis of 5 studies failed to find a strong association between low Vit D and OM (did not look at VDBP) - Oct 2016
Association between vitamin D and development of otitis media: A PRISMA-compliant meta-analysis and systematic review
Medicine (Baltimore). 2016 Oct;95(40):e4739.
Li HB1, Tai XH, Sang YH, Jia JP, Xu ZM, Cui XF, Dai S.
BACKGROUND:
Nutrients related to serum vitamin D level were previously shown to be significantly associated with the risk of many chronic diseases. This study aimed to assess potential relationships between serum vitamin D level and otitis media (OM) risk.
METHODS:
PubMed, EMBASE, and Cochrane Library databases were searched till Aug 18, 2015 for studies of quantitative OM risk estimates in relation to serum vitamin D level. The odds ratio and weighted mean difference, with 95% confidence intervals (CIs), were used to measure the relationship between serum vitamin D level and OM risk.
RESULTS:
Of the 89 articles identified by database search, 5 studies reported data of 16,689 individuals were included in our meta-analysis. We noted participants with OM was associated with lower level of plasma vitamin D when compared with patients without OM (weighted mean difference -5.67; 95% CI -8.08 to -3.26, P < 0.001). Furthermore, as compared with control group, serum vitamin D level was not associated with the risk of OM (odds ratio 0.80, 95% CI 0.47-1.38, P = 0.425). Subgroup analyses suggested that participants with acute OM might associate with lower serum vitamin D level.
CONCLUSIONS:
Plasma vitamin D level might play an important role on the progression of acute OM, whereas no significant impact in patients with chronic OM.
