ALS fought by vitamin D - many studies
Amyotrophic Lateral Sclerosis = ALS = Lou Gehrig's Disease
Highlights
ALS 4X worse if low vitamin D
Die sooner if low Vitamin D
2,000 IU of vitamin D helped all 20 ALS patients - back in 2013
Vitamin D has been recommended by Global ALS group since 2015
2 studies have found that Omega-3 also helps ALS patients
Vitamin D Receptor Activators (Resveratrol and Curcumin) treat ALS
📄 Perplexity AI report of ALS and Vitamin D - June 2025
You might want to see instead: Ankylosing spondylitis and low vitamin D – many studies
13 pages have ALS etc, in their title on VitaminDWiki
This list is automatically updated
{LIST()}
60,00+ items in Google Scholar contain ALS and Vitamin D - Dec 2025
Vitamin D in Neurological Diseases: From Pathophysiology to Therapy- July 2020 FREE PDF
Vitamin D in Neurological Diseases - Dec 2022 FREE PDF
Use of Off-Label Drugs and Nutrition Supplements among Patients with Amyotrophic Lateral Sclerosis in Norway - April 2022 https://doi.org/10.1155/2022/1789946 FREE PDF
Complementary and alternative medicine for treating amyotrophic lateral sclerosis: a narrative review - Dec 2019 doi: 10.1016/j.imr.2019.08.003 FREE PDF
Are the protective benefits of vitamin D in neurodegenerative disease dependent on the route of administration? A systematic review - 2020 https://doi.org/10.1080/1028415X.2018.1493807
Some ALS outbreaks not associated with genetics - March 2025
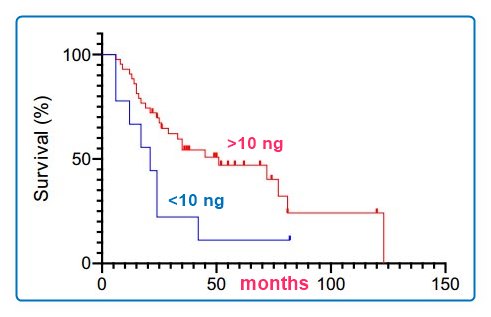
Die sooner of ALS if <10 ng Vitamin D - March 2023
Potential Role of Vitamin D Levels in amyotrophic lateral sclerosis cognitive impairment
See also Amyotrophic lateral sclerosis has 4X faster decline if severely low Vitamin D – Nov 2013
📄 Download the PDF from VitaminDWiki
Speculation: ALS poor gut may need probiotics and/or gut-friendly Vitamin D
Many other health problems with poor guts are poorly treated by standard Vitamin D
A healthy gut needs Vitamin D and a good vitamin D receptor – Sept 2022
Vitamin D is aided by probiotics (review of RCTs) – Dec 2020
Probiotics - New Naturally Occurring Inhibitor Of ALS Progression mentions Buturate - a VDR activator (2020?)
Lessons to Learn from the Gut Microbiota: A Focus on Amyotrophic Lateral Sclerosis - May 2022 📄 PDF_
-
- Diseases with poor guts include Cystic Fibrosis, IBS, Diabetes, and Parkinson's. ALS
Omega-3 fatty acids may reduce the risk of Lou Gehrig’s disease
URL 2014
Note: ALS associated with sports, Omega-3 reduces traumatic brain injury
Worse ASL at diagnosis associated with low Vitamin D - May 2020
Low 25OH Vitamin D Blood Levels Are Independently Associated With Higher Amyotrophic Lateral Sclerosis Severity Scores: Results From a Prospective Study
Raul Juntas-Morales1, Nicolas Pageot1, Gregory Marin2, Anne-Marie Dupuy3, Sébastien Alphandery1, Laura Labar1, Florence Esselin1, Marie Christine Picot2 and William Camu1*
1Clinique du Motoneurone, Explorations Neurologiques, CHU Gui de Chauliac, Montpellier, France
2Département d'Information Médicale, CHU de la Colombière, Montpellier, France
3Laboratoire de Biochimie et Hormonologie, CHU Lapeyronie, Montpellier, France
Background: Amyotrophic lateral sclerosis (ALS) is a fatal neurodegenerative disorder characterized by progressive degeneration of upper and lower motor neurons. Prognosis is highly variable, ranging from a few months to more than 30 years. 25OH vitamin D (25OH VD) blood levels have been associated with a worse prognosis of ALS, but these results remain in dispute. We addressed this controversy with a prospective study and multivariate analysis to study the influence of known clinical prognostic factors of the disease and 25OH VD levels on Revised Amyotrophic Lateral Sclerosis Functional Rating Scale (ALSFRS-R) severity score (ALS-SS), as defined by the monthly rate of decline of ALSFRS-R score, to identify the factors most closely linked to the risk of worsening of the disease.
Results: This prospective cohort of ALS patients recruited 127 individuals, and 105 of them met the inclusion criteria. The mean age of onset was 62.2 ± 12.1 years, 32% of subjects had bulbar onset, and the gender ratio was 1.44 (male/female). Mean 25OH VD level was 26.8 ± 10.8 ng/ml and was similar between males and females.
Patients with 25OH VD levels <15 ng/ml had significantly higher ALS-SS at inclusion (ALS-SSi) than those with normal levels (>30 ng/ml), p = 0.011. The study of ALS-SS as calculated at the end of follow-up (ALS-SSe) was not found to correlate to initial 25OH VD levels (r = −0.19; p = 0.084). Univariate analysis showed that ALS-SSe correlated with 25OH VD levels, ALS duration at inclusion, slow vital capacity (SVC) at inclusion, and SVC loss. The multivariate model showed that 25OH VD levels were independently associated with ALS-SSe: r = −0.0125, p = 0.033. Log-rank test with Kaplan–Meier curves did not show significant differences in survival between the groups defined by 25OH VD levels: <15, >15 and <30, and > 30 ng/ml, p = 0.88.
Conclusions: This prospective study in ALS patients confirmed previous retrospective results: ALS-SSi is significantly higher in patients with severe VD deficiency. For the first time, multivariate analysis showed that 25OH VD level was an independent prognostic factor correlated to ALS-SSe, suggesting that discrepancies between previous works could be due to confounders. It would be important that the present work be replicated in larger samples to confirm the present findings.
📄 Download the PDF from VitaminDWiki
The meta-analysis did not find a correlation between ALS with Low Vitamin D - July 2020
Is There a Role for Vitamin D in Amyotrophic Lateral Sclerosis? A Systematic Review and Meta-Analysis
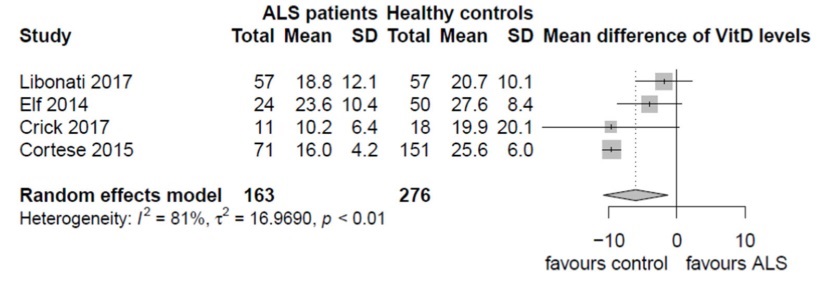
Note by VitaminDWiki - their conclusions do not appear to agree with their data or with other studies.
Conclusion
Our analyses suggest that there is a tendency for ALS patients to have lower levels of vitamin D than controls, but most of the studies did not adjust for the mean vitamin D of the country population and failed to report important factors of variability for vitamin D levels (for example, lack of sun exposure). When studies presented enough data to be analyzed, our meta-analyses did not find strong evidence for a relationship between vitamin D levels and prognosis, nor did vitamin D supplementation induce an improvement in motor function. Our study does not
support any particular positive link between vitamin D and ALS. Furthermore, the risk of bias analysis raised some concerns about the quality of these studies. ALS patients should receive vitamin D supplementation for other health issues related to vitamin D deficiency, but there is not enough evidence to support vitamin D as a therapy for ALS.
📄 Download the PDF from VitaminDWiki
Zinc + Copper might be a Cure for ALS - 2017
Do We Have A Cure For Lou Gehrig's Disease? (Amyotrophic Lateral Sclerosis)
"The recommended dosage is 90-100 mg of zinc and 2-3 mg of copper, taken twice daily."
"As a report published at Atlas of Science points out, the lack of zinc (or balance of zinc with copper) is at the heart of autoimmune disorders. We are talking here about multiple sclerosis, psoriasis, lupus, rheumatoid arthritis, Type I diabetes, Hashimoto's thyroiditis."
Zinc and Vitamin D category listing has
items along with related searches
Vitamin D and ALS: genetics and Signaling - 2013
Roles of vitamin D in amyotrophic lateral sclerosis: possible genetic and cellular signaling mechanisms
📄 Download the PDF from VitaminDWiki
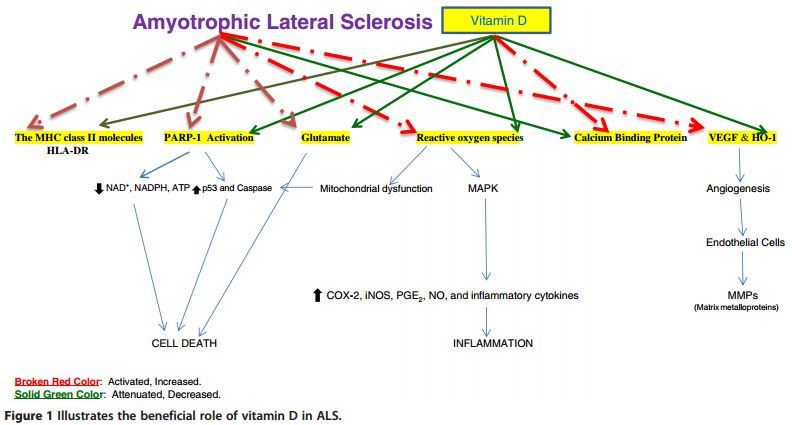
ALS 4X worse if severely low Vitamin D - Nov 2013
Amyotrophic lateral sclerosis has 4X faster decline if severely low Vitamin D – Nov 2013 has the following chart.
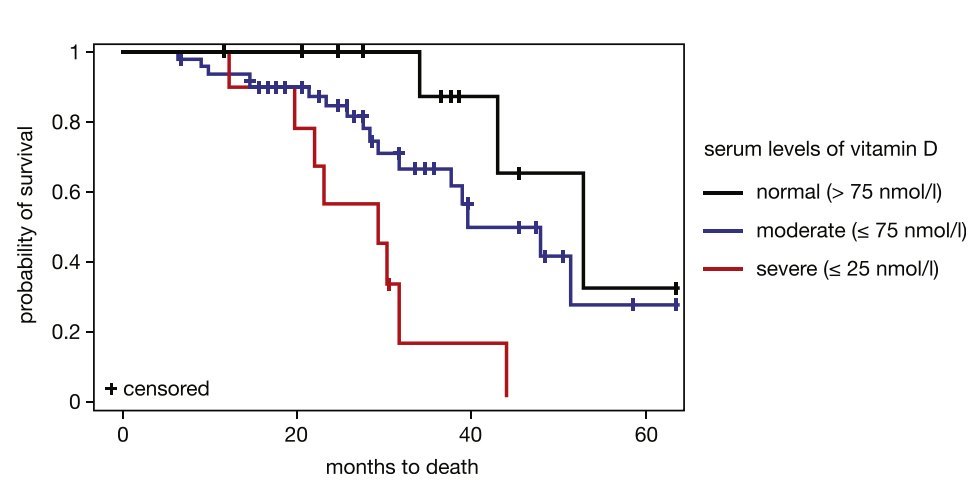
Red line: < 25 nmol = <10 ng
Even 2,000 IU helped all 20 ALS patients in the clinical trial - in 2013
Vitamin D deficiency and its supplementation in patients with amyotrophic lateral sclerosis.
J Clin Neurosci. 2013 Jun 28. pii: S0967-5868(13)00149-5. doi: 10.1016/j.jocn.2013.01.011.
Karam C, Barrett MJ, Imperato T, Macgowan DJ, Scelsa S.
Department of Neurology, Mayo Clinic College of Medicine, 200 First Street SW, Rochester, MN 55905, USA. Electronic address: chafickaram@gmail.com.
We studied 25-hydroxyvitamin D (vitamin D) levels in patients with amyotrophic lateral sclerosis (ALS) and the effect of vitamin D supplementation. Vitamin D levels were checked in 37 consecutive patients with ALS. Demographic data, vitamin D supplementation, change in Amyotrophic Lateral Sclerosis Functional Rating Scale (ALSFRS-R) score, and side effects from vitamin D were noted over a 9-month follow-up period. ALSFRS-R scores were compared between patients who took vitamin D and those who did not. The median age was 55 years, and the median time since symptom onset was 61 months. The mean vitamin D level was 22.3ng/mL (normal range, 30-80ng/mL). Eighty-one percent of patients had a vitamin D level lower than 30ng/mL, and 43% had a vitamin D level lower than 20ng/mL.
Twenty patients took 2000 international units of vitamin D daily . After adjustment for age and baseline vitamin D levels in a linear regression model, the ALSFRS-R score decline was smaller in patients taking vitamin D at 9 months (p=0.02) but was not significantly different at 3 or 6 months. Median vitamin D levels rose from 18.5 to 31.0ng/mL at 6 months in the group taking vitamin D. No side effects secondary to vitamin D supplementation were reported. Vitamin D supplementation at 2000 international units daily was safe over a period of 9 months and may have a beneficial effect on ALSFRS-R scores. Further studies are warranted to determine whether there is a benefit in vitamin D supplementation for all ALS patients.
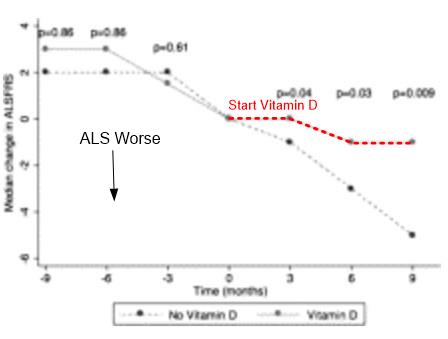
Fig. 1. Graph showing the change in median Amyotrophic Lateral Sclerosis Functional Rating Scale (ALSFRS) score before and after initiation of vitamin D supplementation, with Time 0 being the commencement of supplements for the vitamin D group.
Comment by VitaminDWiki
2,000 IU of vitamin D took over 6 months to restore vitamin D levels - then the benefits could start
It would have been much faster if they had used a loading dose
Publisher sells PDF for $31.50
ALSFRS-R score Calculator is calculated on the following aspects
Speech, 2. Salivation, 3. Swallowing, 4. Handwriting, 5. Cutting food with gastrostomy, 6. Dressing and Hygiene
Turning in bed, 8. Walking, 9. Climbing stairs, 10. Dyspnea, 11. Orthopnea (sleeping), 12. Respiratory insufficiency
Number many years since the onset of symptoms
Vitamin D as a potential therapy in amyotrophic lateral sclerosis (mouse ALS) – Feb 2014
CNS Neurosci Ther. 2014 Feb;20(2):101-11. doi: 10.1111/cns.12204.
Gianforcaro A1, Hamadeh MJ.
1School of Kinesiology and Health Science, Faculty of Health, and Muscle Health Research Centre, York University, Toronto, ON, Canada.
Vitamin D has been demonstrated to influence multiple aspects of amyotrophic lateral sclerosis (ALS) pathology.
Both human and rodent central nervous systems express the vitamin D receptor (VDR) and/or its enzymatic machinery needed to activate the hormone fully.
Clinical research suggests that vitamin D treatment can improve compromised human muscular ability and increase muscle size, supported by the loss of motor function and muscle mass in animals following VDR knockout, as well as increased muscle protein synthesis and ATP production following vitamin D supplementation.
Vitamin D has also been shown to reduce the expression of biomarkers associated with oxidative stress and inflammation in patients with
multiple sclerosis,
rheumatoid arthritis,
congestive heart failure,
Parkinson's disease and
Alzheimer's disease;
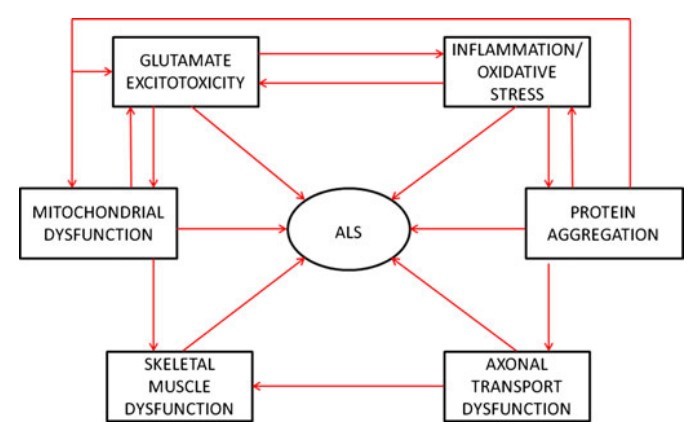
diseases that share common pathophysiologies with ALS.
Furthermore, vitamin D treatment greatly attenuates hypoxic brain damage in vivo and reduces neuronal lethality of glutamate insult in vitro, a hallmark trait of ALS glutamate excitotoxicity.
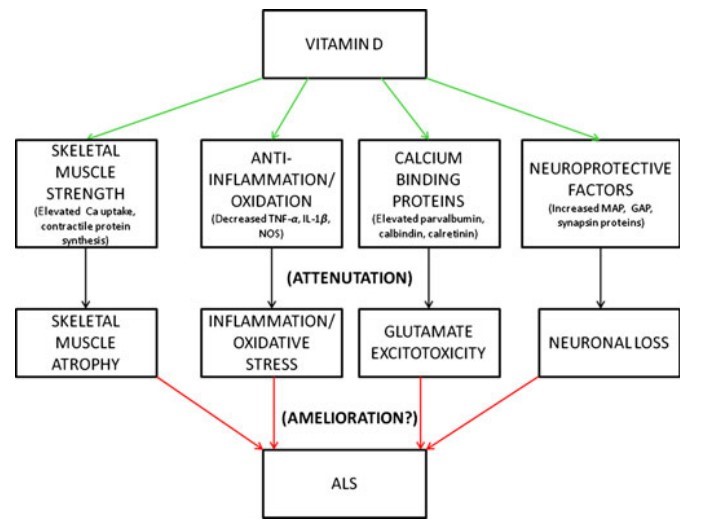
We have recently shown that high-dose vitamin D3 supplementation improved, whereas vitamin D3 restriction worsened functional capacity in the G93A mouse model of ALS .
In sum, evidence demonstrates that vitamin D, unlike the anti glutamatergic agent Riluzole, affects multiple aspects of ALS pathophysiology and could provide a greater cumulative effect.
PMID: 24428861
📄 Download the PDF from VitaminDWiki
ALS varies with latitude - similar to most vitamin D-related diseases
Amyotrophic Lateral Sclerosis: A Synthesis of Research and Clinical Practice
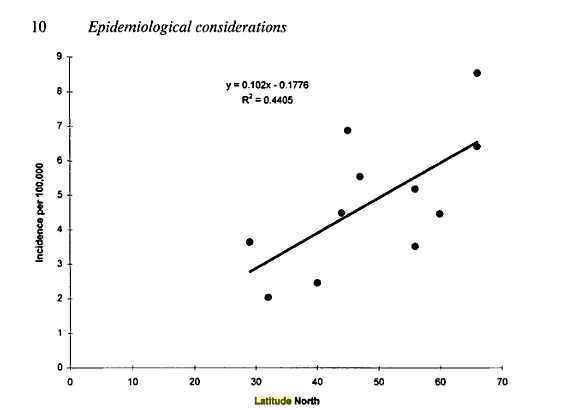
ALS worse if a lower level of vitamin D - June 2015
Vitamin D is Not a Protective Factor in ALS
CNS Neurosci Ther. 2015 Jun 20. doi 10.1111/cns.12423
Blasco H1,2, Madji Hounoum B1, Dufour-Rainfray D1,3, Patin F1, Maillot F4,5, Beltran S6, Gordon PH7, Andres CR1,2, Corcia P1,6.
AIMS: Vitamin D deficiency has been associated with poorer prognosis in ALS. A better understanding of the role of vitamin D in ALS is needed to determine whether trials of systematic supplementation are justified. Our aim was to report vitamin D levels during the course of ALS and to evaluate its relationship with clinical parameters at diagnosis and with disease progression.
METHODS: We prospectively collected vitamin D serum concentrations from 125 consecutive ALS patients. Cox proportional hazard models analyzed the relationship between vitamin D concentrations, clinical parameters, and survival.
RESULTS: The mean vitamin D concentration was below our laboratory's lower limit of normal (P < 0.0001) and did not change during the course of the disease. The concentrations were higher in patients with bulbar onset (P = 0.003) and were negatively associated with body mass index (BMI) (P = 0.0095). Models with ALSFRS-R (ALS Functional Rating Scale-Revised) and BMI as covariates showed that vitamin D concentrations predicted a worse prognosis.
CONCLUSION: .Our cohort's distribution of vitamin D concentrations was consistent with previous reports. Surprisingly, we noted a negative effect of higher vitamin D levels on prognosis in ALS . More detailed research is warranted to determine whether vitamin D manipulation could benefit patients. PMID: 26096806
ALS Worldwide continues to recommend high dose Vitamin D - Feb 2015
Vitamin D3 BenefitsALS Wordlwide
"ALS Worldwide has been recommending the use of Vitamin D (specifically Vitamin D3, a more powerful isomer) for several years, based largely on instinct and the realization that many ALS/MND patients are unable to get sufficient vitamin D through sunshine."
"Based on our own usage of D3 and guidelines established by Mayo Clinic, we recommend a trial dose of 6,000 to 10,000 IU daily by mouth."
Life Extension Foundation - Many supplements prevent or treat ALS
Includes Vitamin B12, Zinc, CoQ10,Creatine, Glutathione and N-acetyl-cysteine (NAC), etc
ALS "Ice Washing" "nonprofit" executives each have an average salary of $173,000
Details at |60+ Natural ALS Cures the "Ice Washing" Campaign Isn't Funding! GreenMedInfo
GreenMedInfo points out that ALS "non-profit" focuses on patentable treatments of ALS rather than natural supplements.
GreenMedInfo gives details on proven ALS treatments by Vitamins D, E, and B-12
ALS 5 X more likely if exposed to pesticides - JAMA May 2016
Association of Environmental Toxins With Amyotrophic Lateral Sclerosis JAMA Neurology
Questionnaire to 60-year-olds - comparing ALS and non-ALS
5X any pesticide exposure in 30 years
pentachlorobenzene: OR = 2.21;
cis-chlordane: OR = 5.74;
PCB 175: OR = 1.81;
PCB 202: OR = 2.11;
BFR (polybrominated diphenyl ether 47: OR = 2.69;
Military: OR = 2.31;
Sources of pesticides (from PDF)

📄 Download the PDF from VitaminDWiki
Note: Pesticides lower Vitamin D. Vitamin D supplementation cancels some of the problem
See also VitaminDWiki Pesticides increase risk of Cancers, Alz, ALS, Asthma, ADHD, etc. (all related to low vitamin D) – Oct 2016
ALS 4X more likely in professional football players- June 2016
- The Complicated Connection Between Football and ALS Atlantic
- "professional football players are 4 X more likely to die of ALS than the general population."
- "Hereditary factors explain only a small percentage of ALS cases."
- "The head trauma hypothesis is bolstered by the fact that veterans appear to be more likely to develop ALS, as are soccer players."
- Note by VitaminDWiki: many professional football players have low levels of vitamin D due to covered stadiums (lack of sun)
ALS survival does not vary with vitamin D level (greater or less than 10 nanograms) - Aug 2016
Vitamin D levels are not predictors of survival in a clinic population of patients with ALS.
J Neurol Sci. 2016 Aug 15;367:83-8. doi: 10.1016/j.jns.2016.05.007. Epub 2016 May 7.
Yang J1, Park JS2, Oh KW2, Oh SI3, Park HM4, Kim SH5.
OBJECTIVE:
This study aimed to measure serum 25-hydroxyvitamin D [25(OH)D] concentrations, bone mineral density (BMD), and the parameters of bone metabolism in amyotrophic lateral sclerosis (ALS) patients and their correlation with survival.
METHODS:
We retrospectively analyzed data from 100 ALS patients who consecutively visited a single referral ALS clinic between January and December 2011. Sex, age, and site of symptom onset and death were recorded. Serum 25(OH)D concentration was dichotomized as <10ng/ml and ≥10ng/ml.
RESULTS:
There was absent relationship between serum 25(OH)D and concentration of bone turnover parameters or between 25(OH)D and BMD. According to the results of the Kaplan-Meier analysis with log-rank test, the survival rates of patients without (≥10ng/ml) and of those with severe vitamin D deficiency (< 10ng/ml) were not significantly different. Cox regression analysis showed that a poor prognosis was most correlated with older age at onset and bulbar onset after adjustment for all the clinical factors.
CONCLUSIONS:
In conclusion, vitamin D levels were not correlated to other bone markers and survival in a clinic population of ALS patients.
ALS is not helped by 25,000 IU every 15 days (no surprise). RCT Jan 2017
Vitamin D in amyotrophic lateral sclerosis.
Funct Neurol. 2017 Jan/Mar;32(1):35-40.
Libonati L, Onesti E, Gori MC, Ceccanti M, Cambieri C, Fabbri A, Frasca V, Inghilleri M.
Vitamin D supplementation has been proposed as a potential treatment to delay amyotrophic lateral sclerosis (ALS) progression. The aims of this study were to retrospectively compare vitamin D blood levels in ALS patients with those in healthy subjects, correlate vitamin D blood levels with clinical functions in patients, and evaluate whether vitamin D administration could modify the disease's clinical progression. Vitamin D blood levels were evaluated in 57ALS patients and in 57 healthy subjects. In the ALS patients, the following clinical variables were evaluated every 3 months: Medical Research Council scale (MRC) score, revised ALS functional rating scale (ALSFRS-R) score and forced vital capacity (FVC). Twenty-four patients were treated with high doses of cholecalciferol. No significant differences were found between the vitamin D blood levels in the ALS patients (18.8 ± 12.2) and the healthy subjects (20.7 ± 10.1). The vitamin D levels in ALS patients did not correlate with recorded clinical parameters. No clinical differences in terms of ALSFRS-R, MRC, or FVC were found between the treated and the untreated patients over time. In ALS, as in other chronic neurological diseases, vitamin D levels in blood appeared reduced, but no difference was found between the levels in ALS patients and healthy subjects. Oral vitamin D supplementation in ALS patients was not associated with a better prognosis than in untreated ALS patients. Further prospective controlled studies are needed to clarify the effect of vitamin D on the progression of ALS disease.
📄 Download the PDF from VitaminDWiki
The study does not appear to have measured the vitamin D levels after treatment
Wonder why they consider a 1,700 IU daily average to be a "high dose."
$145,000+/year ALS drugs approved by 2017, 2022. Cancelled March 2024 (=placebo)
A Second Drug Is Approved to Treat A.L.S. New York Times
" . . Radicava or edaravone, slowed the progression of the degenerative disease in a six-month study in Japan."
“The effect is modest but significant.”
"The first round of treatment requires a one-hour infusion every day for 14 days, followed by 14 days off. After that, the infusions are given daily for 10 out of 14 days, with 14 days off."
"He added that the drug will not make patients feel better or stronger. It does not improve symptoms. It can slow the decline, but that is not something a patient will notice."
NYT Sept 2022 - Relyvrio $158,000/year
This $158,000 Drug Likely Doesn’t Work. Why Was It Approved? Bloomberg March 2024
When Amylyx Pharmaceuticals Inc. snagged US approval for a $158,000-a-year drug to treat amyotrophic lateral sclerosis, it was a controversial decision. The company had completed only one small efficacy trial in 137 patients. The first time the drug went before a Food and Drug Administration advisory panel in March 2022, the panel voted 6-4 that the drug had not been proven to be effective.
The FDA, under pressure from patient groups to approve the medicine, took the unusual move of convening a second panel hearing on the same drug less than six months later. At the second hearing, Amylyx co-founder Justin Klee promised to take the drug off the market if it was approved and later studies failed to confirm the medicine’s effectiveness.
New York Times Jane Brody on new drug for ALS - May 2017 (nothing about Vitamin D)
A New Drug for A.L.S., but the Diagnosis Remains Dire
- "Over the course of a lifetime, one person in about 400 is likely to develop it, a risk not unlike that of multiple sclerosis."
- Note by admin of VitaminDWiki - I checked, and yes, ALS and MS have similar incidence rates.
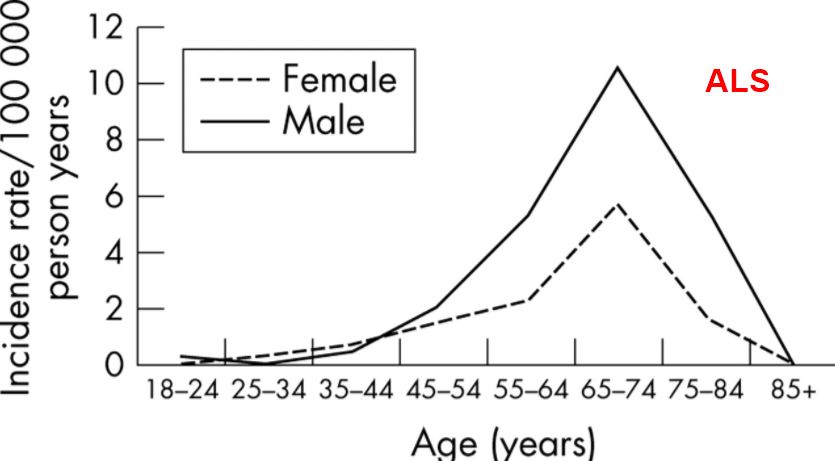
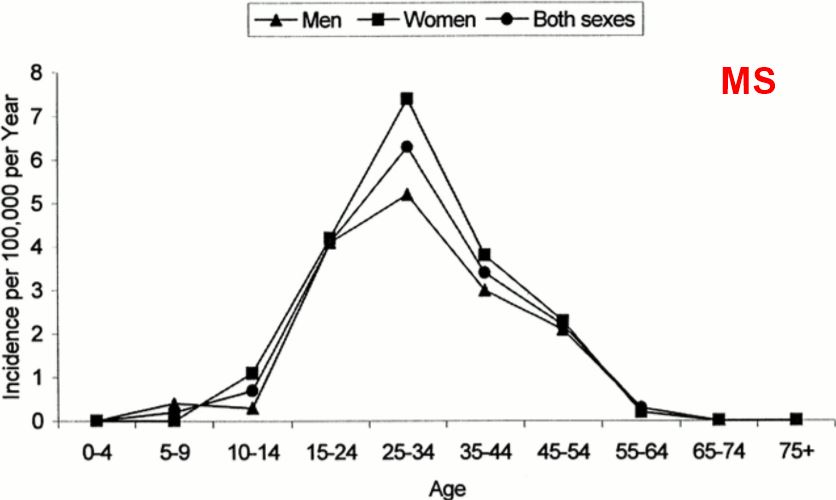
- Note by admin of VitaminDWiki - I checked, and yes, ALS and MS have similar incidence rates.
Half of ALS die within 5 years.
"The Food and Drug Administration just approved a second drug, Radicava (edaravone), said to slow disease progression in a six-month study in Japan, though its effects on survival are not yet known. It must be administered intravenously for 10 days every two weeks at a cost of more than $145,000 a year for the medication alone."
"The risk is higher than expected among military veterans, professional football players, and athletes who took dietary supplements containing branched-chain amino acids. The Department of Veterans Affairs recognizes A.L.S. as a service-connected disease."
ALS patients helped by Omega-3 – RCT Sept 2017
Amyotrophic Lateral Sclerosis patients helped by Omega-3 – RCT Sept 2017
ALS was treated by the right balance of Omega-3 and Omega-6 - mice in 2018
- Omega-3 Hastens and Omega-6 Delays the Progression of Neuropathology in a Murine Model of Familial ALS
- mice live for 2.5-3yrs; the 1.5 to 3-week increase in survival demonstrated herein extrapolates to ≥1yr of human life based on an 80yr human life span."
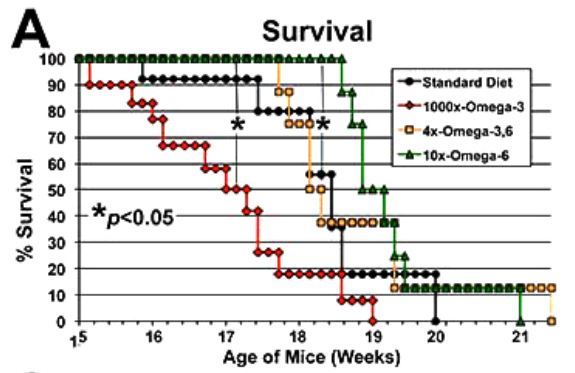
📄 Download the PDF from VitaminDWiki
Vitamin D levels are associated with gross motor function in amyotrophic lateral sclerosis.- April 2017
Muscle Nerve. 2017 Oct;56(4):726-731. doi: 10.1002/mus.25555. Epub 2017 Apr 5.
Paganoni S1,2,3, Macklin EA1,4, Karam C5, Yu H2, Gonterman F2, Fetterman KA2, Cudkowicz M1,2, Berry J1,2, Wills AM1,2.
1 Neurological Clinical Research Institute, Harvard Medical School, Massachusetts General Hospital, 165 Cambridge Street, Suite 600, Boston, Massachusetts, 02114, USA.
2 Department of Neurology, Neurological Clinical Research Institute, Massachusetts General Hospital, Boston, Massachusetts, USA.
3 Department of Physical Medicine and Rehabilitation, Spaulding Rehabilitation Hospital, Cambridge, Massachusetts, USA.
4 Biostatistics Center, Massachusetts General Hospital, Boston, Massachusetts, USA.
5 Department of Neurology, Oregon Health and Science University, Portland, Oregon, USA.
INTRODUCTION: This study aimed to determine whether serum vitamin D [25(OH)D] levels are associated with disease progression in amyotrophic lateral sclerosis (ALS).
METHODS:
25(OH)D was measured in subjects enrolled in a multicenter study to validate ALS biomarkers. Baseline 25(OH)D levels were correlated with baseline ALSFRS-R scores. Average 25(OH)D levels from baseline and month 6 visits (seasonally asynchronous) were used to predict the subsequent rate of change in ALSFRS-R from month 6 to month 18.
RESULTS:
Most subjects had either insufficient or deficient 25(OH)D levels. Lower 25(OH)D was associated with lower ALSFRS-R gross motor scores but not lower ALSFRS-R total scores at baseline. 25(OH)D levels were not predictive of disease progression over the next 12 months.
CONCLUSION:
25(OH)D was associated with baseline gross motor ALSFRS-R scores but did not predict the rate of disease progression. Vitamin D levels may reflect poor mobility in patients with ALS. Muscle Nerve, 2017 Muscle Nerve 56: 726-731, 2017.
PMID: 28044349 DOI: 10.1002/mus.25555 Publisher rents PDF for $6
ALS motor functions not helped by monthly 100,000 IU - June 2019
Vitamin D supplementation has no effects on the progression of motor dysfunction in amyotrophic lateral sclerosis (ALS).
Eur J Clin Nutr. 2019 Jun 13. doi: 10.1038/s41430-019-0448-3
Trojsi F1, Siciliano M2,3, Passaniti C2,3, Bisecco A2, Russo A2, Lavorgna L2, Esposito S2, Ricciardi D2, Monsurrò MR2, Tedeschi G2, Santangelo G3.
OBJECTIVES:
To investigate the effects of cholecalciferol supplementation on the progression of motor disability in a cohort of amyotrophic lateral sclerosis (ALS) patients with low blood 25-hydroxyvitamin D3 [25(OH)D] levels, on the basis of the hypothesis of potential neuroprotective effects of vitamin D supplementation.
METHODS:
Forty-eight ALS patients, 34 with deficient (<20 ng/mL) and 14 with insufficient (20-29 ng/mL) serum levels of 25(OH)D, were randomized and treated by 3 different doses of cholecalciferol [50.000, 75.000 and 100.000 international units (IU) /month] and evaluated after 6-months. Assessment of motor dysfunction at baseline and after 6 months included ALS Functional Rating Scale-Revised (ALFRS-R) and upper motor neuron (UMN) scores and blood samples for 25(OH)D levels.
RESULTS:
Clinical data of 33 patients were available after 6 months. Analysis of Covariance (ANCOVA), with pre-treatment measurements included as a covariate, did not show statistically significant differences in the ALSFRS-R (p > 0.05) and UMN (p > 0.05) among the patient groups who underwent 3 different doses of cholecalciferol. Conversely, the treatment with 75.000 IU/month or 100.000 IU/month induced a significant increase in serum levels of 25(OH)D in comparison with the supplementation with 50.000 IU/month; no significant differences were found between 75.000 IU/month and 100.000 IU/month.
CONCLUSIONS:
Our findings highlighted that 6-month supplementation of vitamin D in ALS patients had no significant effects on motor dysfunction. However, it is recommended to prevent medical complications of vitamin D deficiency in ALS patients as well as in other populations of neurodegenerative patients characterized by low mobility and decreased sun exposure.
📄 Download the PDF from Sci-Hub via VitaminDWiki
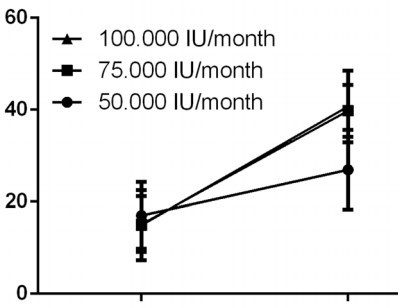
Comment by the founder of VitaminDWiki: Only half of the participants got to a good level of vitamin D (> 40 ng) by the end of the trial, probably due to poor response associated with poor gut function. Anticipate far better results if you use any of the many gut-friendly forms of vitamin D for a longer time and/or use a loading dose.
Asked CHAT-GPT June 2023: What is the commonality of Amyotrophic Lateral Sclerosis with Muscular Dystrophy.
Amyotrophic Lateral Sclerosis (ALS) and Muscular Dystrophy (MD) are both neuromuscular disorders but distinct diseases with different causes and manifestations. However, they do share several similarities:
Neuromuscular Disorders: Both ALS and MD are classified as neuromuscular disorders. This means that they both affect the muscles and the nerves that control them.
Progressive Disease: ALS and MD are progressive diseases, meaning symptoms tend to worsen over time. In both cases, this progression increases muscle weakness and functional disability.
Genetic Factors: Some forms of both ALS and MD can be caused by inherited genetic mutations. However, not all cases are inherited; most ALS cases are sporadic, meaning they occur randomly without a clear cause.
Muscle Weakness: Both diseases lead to muscle weakness, though the progression, distribution, and specific muscles affected can vary. In ALS, muscle weakness often starts in the limbs, while Duchenne Muscular Dystrophy (the most common form of MD in children) usually begins in the hips and pelvis.
No Known Cure: As of my knowledge cutoff in September 2021, there are no known cures for either ALS or MD. Managing both diseases involves treating symptoms, preventing complications, and maintaining the quality of life as much as possible.
Life Expectancy: Both diseases can impact life expectancy, though the degree can vary widely. ALS often progresses more rapidly than most forms of MD, leading to life-threatening complications more quickly.
Research: Both diseases are the focus of intense research efforts aimed at better understanding their causes, finding more effective treatments, and, ultimately, discovering a cure.
- Despite these commonalities, it's important to note that ALS and MD are distinct diseases with different causes and disease processes. If you or someone else has been diagnosed with either condition, it's crucial to speak with a healthcare provider to understand the specific disease and its management.
See also in VitaminDWiki
Muscular Dystrophy probably treated by high-dose Vitamin D plus muscle rehab
Muscular Dystrophies – low vitamin D might be associated with all 9 types – Aug 2018
