Lung cancer treated by Vitamin D (1200 IU early stage) – RCT
Vitamin D supplementation and survival of patients with non-small-cell lung cancer: A randomized, double-blind, placebo-controlled trial.
Clin Cancer Res. 2018 Jul 17. pii: clincanres.0483.2018. doi: 10.1158/1078-0432.CCR-18-0483. [Epub ahead of print]
 years
It is amazing that such a small amount of Vitamin D would help.
Suspect that the Japanese patients were very light-weight
Would need larger doses for standard-weight adults
Larger doses would likely also provide more benefits
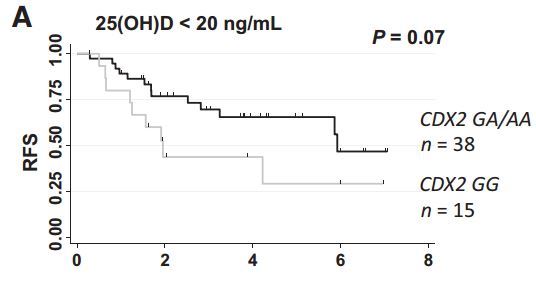
1. Releapse-Free-Survival vs genes (not Vitamin D)
years
It is amazing that such a small amount of Vitamin D would help.
Suspect that the Japanese patients were very light-weight
Would need larger doses for standard-weight adults
Larger doses would likely also provide more benefits
1. Releapse-Free-Survival vs genes (not Vitamin D)
 years
* Lung Cancer death 60 percent less likely if high level of vitamin D – 2 meta-analysis 2017
* Lung cancer and inhaled emulsions (wonder about inhaled Vitamin D) – 2018
* Live longer with lung cancer if have good vitamin D genes (or perhaps lots of vitamin D) – Dec 2017
* Lung Cancer death 60 percent less likely if high level of vitamin D – 2 meta-analysis 2017
* Lung cancer death reduction: CT scan or Vitamin D – which is 40X less expensive
* Cancer patients 64% less likely to die if have high level of vitamin D – Dec 2011 has the following chart
*
years
* Lung Cancer death 60 percent less likely if high level of vitamin D – 2 meta-analysis 2017
* Lung cancer and inhaled emulsions (wonder about inhaled Vitamin D) – 2018
* Live longer with lung cancer if have good vitamin D genes (or perhaps lots of vitamin D) – Dec 2017
* Lung Cancer death 60 percent less likely if high level of vitamin D – 2 meta-analysis 2017
* Lung cancer death reduction: CT scan or Vitamin D – which is 40X less expensive
* Cancer patients 64% less likely to die if have high level of vitamin D – Dec 2011 has the following chart
* 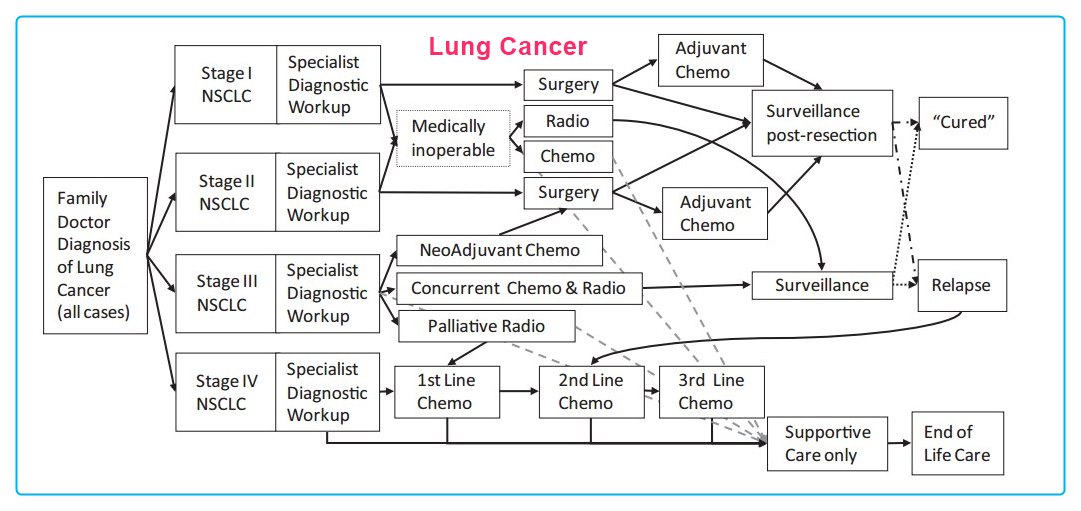 ---
Vitamin D both prevents and treats many cancers
Cancer category starts with the following
{include}
---
Vitamin D both prevents and treats many cancers
Cancer category starts with the following
{include}
PDF is available free at Sci-Hub 10.1158/1078-0432.CCR-18-0483
Akiba T1, Morikawa T2, Odaka M2, Nakada T2, Kamiya N3, Yamashita M2, Yabe M2, Inagaki T2, Asano H2, Mori S2, Tsukamoto Y2, Urashima M4.
1 Thoracic Surgery, Jikei University School of Medicine University Hospital.
2 Thoracic Surgery, Tokyo Jikei University of Medicine.
3 Thoracic Surgery, Kitasato University Kitasato institute hospital.
4 Molecular Epidemiology, Jikei University School of Medicine urashima@jikei.ac.jp.
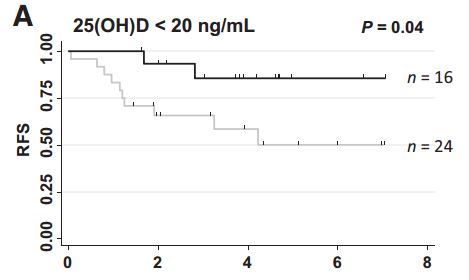
Higher serum 25-hydroxyvitamin D (25(OH)D) levels are reportedly associated with better survival in early-stage non-small-cell lung cancer (NSCLC). Therefore, whether vitamin D supplementation can improve the prognosis of NSCLC patients was examined (UMIN000001869). Experimental
Design: A randomized, double-blind trial comparing vitamin D supplements (1,200 IU/day) with placebo for 1 year after operation was conducted. The primary and secondary outcomes were relapse-free survival (RFS) and overall survival (OS) , respectively. Pre-specified subgroup analyses were performed with stratification by stage (early vs. advanced), pathology (adenocarcinoma vs. others), and 25(OH)D levels (<20 ng/ml vs. high, ≥20 ng/ml). Polymorphisms of vitamin D receptor (VDR) and vitamin D binding protein (DBP) and survival were also examined.
Results: NSCLC patients (n=155) were randomly assigned to receive vitamin D (n=77) or placebo (n=78) and followed for a median of 3.3 years. Relapse and death occurred in 40 (28%) and 24 (17%) patients, respectively. In the total study population, no significant difference in either RFS or OS was seen with vitamin D compared to the placebo group.
However, by restricting the analysis to the subgroup with early-stage adenocarcinoma with low 25(OH)D, the vitamin D group showed significantly better
5-year RFS (86% vs. 58%, P=0.04) and
OS (92% vs. 56%, P=0.02)
than the placebo group. Among the examined polymorphisms, DBP1 (rs7041) TT and CDX2 (rs11568820) AA/AG genotypes were markers of better prognosis, even with multivariate adjustment.
Conclusions: In NSCLC patients, vitamin D supplementation may improve survival of early-stage lung adenocarcinoma patients with lower 25(OH)D levels.
