Vitamin D levels have been crashing since 1995 (Polish Children, Elite Military, etc)
25(OH)D Concentration in Neonates, Infants, and Toddlers From Poland—Evaluation of Trends During Years 1981–2011 - Nov 2018
Front. Endocrinol., 08 November 2018 | https://doi.org/10.3389/fendo.2018.00656
Marek Wójcik, Maciej Jaworski and Pawel Pludowski*
Department of Biochemistry, Radioimmunology and Experimental Medicine, The Children's Memorial Health Institute, Warsaw, Poland
 * Reasons for Low Vitamin D and what to do
* Overview Deficiency of vitamin D
---
1. Vitamin D levels have been crashing
* Reasons for Low Vitamin D and what to do
* Overview Deficiency of vitamin D
---
1. Vitamin D levels have been crashing
 * Canada 6% drop in 2 years all ages, about 2X higher % for age 6-11
* 2X more people have less than :30 ng of vitamin D in a decade – Feb 2010
* 4,000 IU of Vitamin D is OK - 19 organizations agree - 2018
* Governments are increasing their Vitamin D recommendations about every decade.
* Their recommendations typically (mistakenly) consider the vitamin D levels to be static
* Dr. Hollick recommended 1000 IU in 2004, but a decade later recommends 3,500 IU
* * Deficiency of Vitamin D category listing has items along with related searches**
* 10 Reasons why children no longer have healthy levels of Vitamin D
* Prediction: Vitamin D levels will continue dropping for decades
* Vitamin D levels continue to fall in Korea– June 2018
*
* Canada 6% drop in 2 years all ages, about 2X higher % for age 6-11
* 2X more people have less than :30 ng of vitamin D in a decade – Feb 2010
* 4,000 IU of Vitamin D is OK - 19 organizations agree - 2018
* Governments are increasing their Vitamin D recommendations about every decade.
* Their recommendations typically (mistakenly) consider the vitamin D levels to be static
* Dr. Hollick recommended 1000 IU in 2004, but a decade later recommends 3,500 IU
* * Deficiency of Vitamin D category listing has items along with related searches**
* 10 Reasons why children no longer have healthy levels of Vitamin D
* Prediction: Vitamin D levels will continue dropping for decades
* Vitamin D levels continue to fall in Korea– June 2018
*  Military
* Military and Vitamin D - many studies special operations forces
* Trial starting for Vitamin D with US soldiers – 2,000 and 5,000 IU for 3 months – Nov 2016
* Need for Routine Vitamin D Screening in Military Personnel – Sept 2016
* No military trainee consumed Vitamin D RDA (most were also low in Magnesium) – July 2018
Incidence of 22 health problems related to vitamin D have doubled in a decade
* but frogs are not noticing the increasing problem
*
Military
* Military and Vitamin D - many studies special operations forces
* Trial starting for Vitamin D with US soldiers – 2,000 and 5,000 IU for 3 months – Nov 2016
* Need for Routine Vitamin D Screening in Military Personnel – Sept 2016
* No military trainee consumed Vitamin D RDA (most were also low in Magnesium) – July 2018
Incidence of 22 health problems related to vitamin D have doubled in a decade
* but frogs are not noticing the increasing problem
* 
📄 Download the PDF from VitaminDWiki
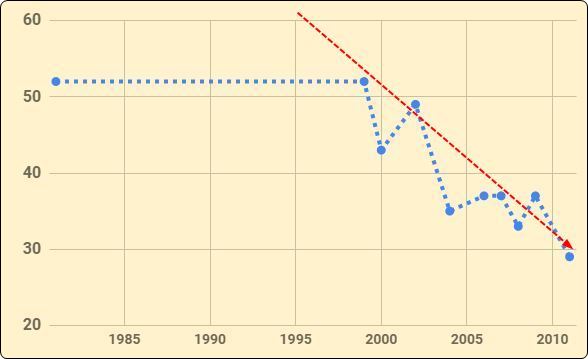
Polish Children ( age 8 months)

Note: Only a single data point for 1981-1999 - unable to see trends during it.

Introduction: The numerous evidence showing spectrum of vitamin D effects on human health resulted in both updates of vitamin D supplementation guidelines for general population and concerns on potential risk of hypercalcaemia. The aim of this study was to analyse trends in serum 25-hydroxyvitamin D concentration (25(OH)D) change over the 30 years of operation of a single pediatric diagnostic unit.
Materials and methods: Calcium-phosphate metabolism markers and 25(OH)D concentrations were analyzed in a group that consisted of newborns and infants commissioned for diagnostics due to suspected calcium-phosphate metabolic disturbances (n = 3,163; mean age 8.0 ± 3.0 months).
Results: 25(OH)D < 10 ng/ml was noted in 4.5% of patients (n = 163), 10–20 ng/ml in 14.7% (n = 465), 20–30 ng/ml in 23.9% (n = 756) and 30–50 ng/ml in 35.9% (n = 1,136). The mean 25(OH)D concentration in analyzed group was 37.5 ± 24.5 ng/ml. In patients with 25(OH)D concentration < 10 ng/ml a normal calcaemia (2.25–2.65 mmol/l) was noted in 83.4% cases (n = 136). Eighty one patients had 25(OH)D concentrations above 100 ng/ml with co-existing calcaemia in range of 2.6–4.38 mmol/l (mean Ca = 2.69 mmol/l). Hypocalcaemia (Ca < 2.25 mmol/l) was observed in 0.54%, (n = 17). 13.8% patients revealed calcium levels >2.65 mmol/l (n = 435). In general, the mean calcium-phosphate markers values were within the reference range for age. The highest mean 25(OH)D concentration of 51.8 ng/ml ± 38.8 was noted in years 1981–1999 (n = 305). The lowest mean 25(OH)D value was observed in years 2010–2011 (29.0 ng/ml ± 13.6; n = 412). The trend of decreasing 25(OH)D concentration during analyzed time period was significant (r = −0.29, p < 0.0001).
Conclusions: Eighty percent of children aged 0–36 months had 25(OH)D concentration >20 ng/ml, however, during 3 decades a mean 25(OH)D concentrations trended significantly to decrease. A direct relationship between low 25(OH)D concentration and hypocalcaemia was not observed nor between high 25(OH)D concentration and hypercalcemia.
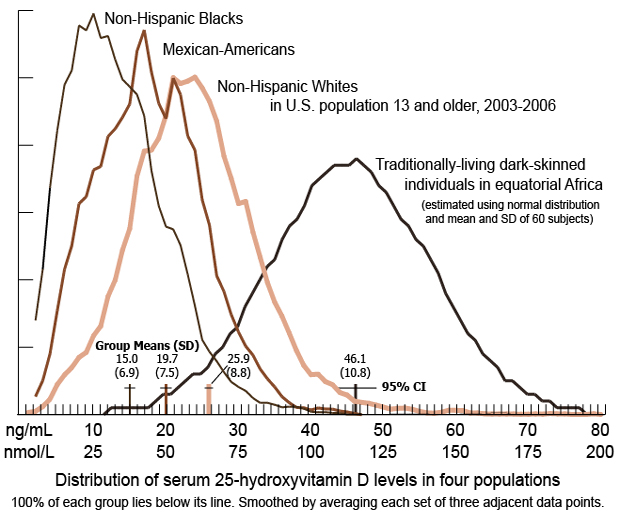
Chart of Vitamin D levels vs race - April 2013 has the following
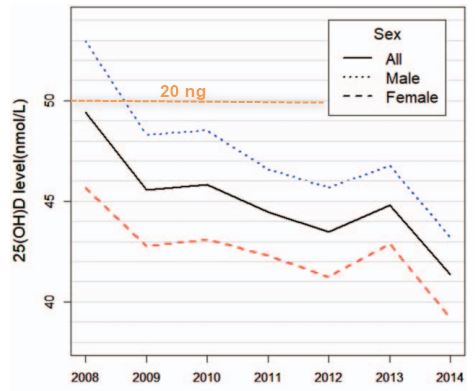
Portuguese Military 25 ng (2014 to 2020)
Vitamin D levels in Portuguese military personnel March 2022
PDF behind a paywall. but first page can be viewed on DeepDyve
Civilians have 24 ng level
sufficiency 25%, insufficiency 40% and deficiency 37%.
short url of this page = is.gd/dcrashing
