Less bone loss if take 100,000 IU vitamin D monthly – RCT
Effect of monthly high-dose vitamin D on bone density in community-dwelling older adults substudy of a randomized controlled trial.
J Intern Med. 2017 Nov;282(5):452-460. doi: 10.1111/joim.12651. Epub 2017 Jul 26.
Reid IR1,2, Horne AM1, Mihov B1, Gamble GD1, Al-Abuwsi F1, Singh M1, Taylor L1, Fenwick S1, Camargo CA3, Stewart AW4, Scragg R4.
1 Department of Medicine, Faculty of Medical and Health Sciences, University of Auckland, Auckland, New Zealand.
2 Department of Endocrinology, Auckland District Health Board, Auckland, New Zealand.
3 Department of Emergency Medicine, Massachusetts General Hospital, Harvard Medical School, Boston, MA, USA.
4 School of Population Health, University of Auckland, Auckland, New Zealand.
📄 Download the PDF from VitaminDWiki
BACKGROUND:
Severe vitamin D deficiency causes osteomalacia, yet trials of vitamin D supplementation in the community have not on average demonstrated benefit to bone mineral density (BMD) or fracture risk in adults.
OBJECTIVE:
To determine whether monthly high-dose vitamin D supplementation influences BMD in the general population and in those with low 25-hydroxyvitamin D levels.
METHODS:
Two-year substudy of a trial in older community-resident adults. A total of 452 participants were randomized to receive monthly doses of vitamin D3 100 000 IU, or placebo. The primary end-point was change in lumbar spine BMD. Exploratory analyses to identify thresholds of baseline 25-hydroxyvitamin D for vitamin D effects on BMD were prespecified.
RESULTS:
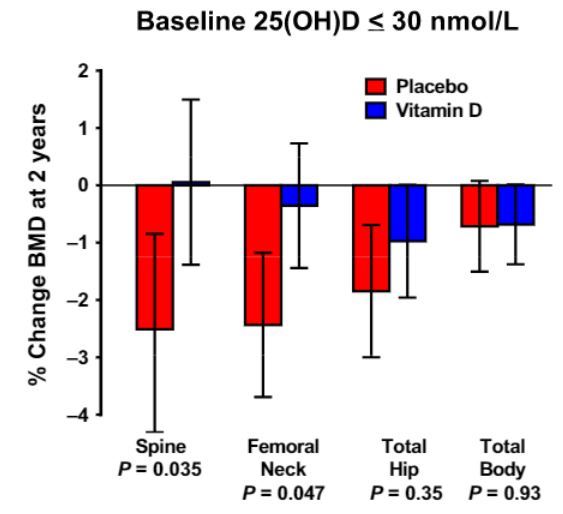
Intention-to-treat analyses showed no significant treatment effect in the lumbar spine (between-groups difference 0.0071 g cm-2 , 95%CI: -0.0012, 0.0154) or total body but BMD loss at both hip sites was significantly attenuated by ~1/2% over 2 years. There was a significant interaction between baseline 25-hydroxyvitamin D and treatment effect (P = 0.04). With baseline 25-hydroxyvitamin D ≤ 30 nmol L-1 (n = 46), there were between-groups BMD changes at the spine and femoral sites of ~2%, significant in the spine and femoral neck, but there was no effect on total body BMD. When baseline 25-hydroxyvitamin D was >30 nmol L-1 , differences were ~1/2% and significant only at the total hip.
CONCLUSIONS:
This substudy finds no clinically important benefit to BMD from untargeted vitamin D supplementation of older, community-dwelling adults. Exploratory analyses suggest meaningful benefit in those with baseline 25-hydroxyvitamin D ≤ 30 nmol L-1 . This represents a significant step towards a trial-based definition of vitamin D deficiency for bone health in older adults.
PMID: 28692172 DOI: 10.1111/joim.12651
