Backache strongly associated with low vitamin D
LEVELS OF VITAMIN D IN PATIENTS WITH LOW BACKACHE
Gomal Journal of Medical Sciences July-September 2014, Vol. 12, No. 3
Sardar Sohail Afsar, Mohammad Idrees, Mohammad Gulzar
Department of Orthopaedic Surgery, Pakistan International Medical College, Peshawar, Pakistan
Corresponding Author: Dr. Sardar Sohail Afsar Senior Registrar Orthopaedics Pak International Medical College Hayatabad, Peshawar, Pakistan. E-mail: dr_sardarsohail@yahoo.co.uk
Background: Along with many factors vitamin D is considered to have role in lower backache.
The objective of this study was to determine the levels of vitamin D in patients of low backache.
Material & Methods: This descriptive study was conducted at Pakistan Institute of Medical Sciences, Peshawar over a period of 10 months in 2013. Five hundred patients having low backache were included in the study through non-probability consecutive sampling. A performa including the demographic information, color of skin, veil observation practice, menstrual history and BMI was recorded. Blood was taken and vitamin D levels measured. Levels <20 ng/dl were taken as deficient, 20-30 ng/dl insufficient and >30 ng/dl as normal.
Results: Mean age of patients was 41.13+15.22 years with 237(47.4%) males and 263(52.6%) females. Vitamin D levels were below normal in 442( 88.4% ) and normal in 50( 10% ) cases. On BMI basis 91.66% with BMI >25 Kg/m2 had low vitamin D levels as compared to 86.56% with BMI <25 kg/m2. Among females 89.19% were of reproductive-age and had lower vitamin D levels as compared to 88.76% of menopausal females. Regarding veil observation 6.49% of veil observing females had normal level as compared to 19.28% of non-veil observing females. In respect to skin complexion 27(13.86%) had normal levels among dark complexion as compared to 23(9.67%) with fair complexion.
Conclusion: Vitamin D deficiency is present in majority of patients with idiopathic lower back pain and should be considered a contributing factor.
INTRODUCTION
Pain localized to the area below the costal margins and above the inferior gluteal folds is defined as low back pain and there is consensus internationally on this definition.12 Backache is one of the common symptoms everywhere in the world and everybody does experience it sometime in lifetime.3 It is only possible in 20% of time to know the exact cause of lower back pain as it is regarded as a problem with multiple factors affecting it.45 Along with many other possible factors, vitamin D is considered to have role in the lower backache.2,6,7 Vitamin D is a major player that is involved in calcium haemostasis along with other factors. It is well documented fact that for healthy development of bones sufficient serum levels of vitamin D are mandatory.8 Vitamin D deficiency is associated with osteoporosis, rickets and osteomalacia.910 Along with these conditions which can lead to lower backache, vitamin D deficiency is also linked with myopathy, aches and pains.11 Few studies have shown a relationship between vitamin D levels and inflammatory /life style related diseases. It functions as a hormone in the body.610 It is shown that vitamin D is directly related to anti-inflammatory cytokines and inversely related to pro-inflammatory cytokines thus giving it anti-inflammatory characteristics.612 Few studies have shown vitamin D deficiency to be a possible cause of idiopathic chronic musculoskeletal pain.610 Vitamin D is essential for development and maintenance of musculoskeletal system not only in the early part of life but also throughout life and is also required for the best function of the muscles and nervous system.6
Vitamin D deficiency is a global issue.27,101314 It is reported in populations presenting with a variety of chronic musculoskeletal disorders like osteoarthritis, arthralgia, rheumatoid arthritis and lower backache.2367 15
There can be two possible reasons for relation between vitamin D deficiency and lower backache.
First possible reason is that vitamin D deficiency in lower backache patients causes diffuse pain in muscle and bone, weakness with paraesthesia.610
Second reason may be because of decreased vitamin D levels there is decrease in anti-inflammatory cytokines and increase in pro-inflammatory cytokines which leads to increased chances of inflammation in end plates of vertebrae.61216
Keeping in mind the above mentioned literature we hypothesise that people from Peshawar having non-specific lower backache may have vitamin D deficiency as reported in Danish, Egyptian and Saudi Arabian lower back ache population.2715
The objective of this study was to determine the levels of vitamin D in patients of non-specific low backache in our population.
MATERIAL AND METHODS
This was hospital based descriptive study conducted on 500 adult males and females of age between 16-80 years complaining of lower back pain of idiopathic nature for less than 6 month duration at Peshawar Institute of Medical Sciences from April 2013 to December 2013. Non-probability consecutive sampling technique was used. Both CT scanning and MRI of lower spine were performed to exclude disc prolapse, spinal stenosis, and degenerative disease of the spine when needed. Patients who had a mechanical cause for the back pain or with clinical features suggestive of neurologic involvement were excluded. Patients with known renal impairment, chronic liver disease or osteoporosis were excluded from the study. Those taking vitamins supplements, using sun blocks, known hypocalcemic patients, metabolic bone disease patients and pregnant & lactating women were also excluded from the study. All those who were fulfilling the inclusion criteria were explained the objective of study and written informed consent was then obtained. A semi structured questionnaire was filled for each participant which included variables like height (cm), weight (kg), BMI (kg/m2) age (years), and skin color for both genders, while observation of veil for pardha and menstrual history from female participants. Patients were also asked about the symptom of paraesthesia.
Blood (5 cc) was drawn from each subject; serum was separated and stored at -20°C. Samples were analyzed within 48 hours of collection. As per protocol of Clinical practice guidelines by Endocrine Society the vitamin D levels were classified vitamin D deficient when serum 25(OH) vitamin D levels were <20 ng/dL, insufficient when 20-30 ng/dL. Serum levels greater than 30 ng/dL were deemed sufficient and levels of >100ng/dL were considered to be in toxic range.
All records were entered into Statistical Package for Social Sciences (SPSS) version 16.0; SPSS Inc., Chicago, IL, USA, for analysis. The quantitative variables like age and BMI were presented as mean and standard deviation. The qualitative variables like gender, skin color, veil observation, and menopause were presented as frequency and percentages. P-value was calculated where applicable.
RESULTS
Our study included 500 patients with low back pain. The mean age was 41.13+15.22 years. Among these 263 (52.6%) were males and 237 (47.4%) females. (Table 1)
The mean vitamin D level of sample was 21.93+21.56. Among the males 231 (87.83%) had vitamin D levels below normal range while 28 (10.64%) had normal vitamin D levels with 4 (1.52%) having levels in the toxic range. Among females 22 (9.28%) had vitamin D levels in normal range, 211 (89.02%) below normal and 4 (1.68%) in the toxic range.
Table-2 represents the vitamin D levels of the patients. It shows that 442 (88.4%) people have below normal vitamin D levels with 315 (63%) having vitamin D deficiency i.e. <20 ng/dL and 127 (25.4%) having vitamin D insufficiency i.e. 20-30 ng/dL. Only 50 (10%) people had vitamin D levels within normal range. Eight (1.6%) people had vitamin-D levels in toxic level i.e. >100 ng/dL. Table-4 represents the vitamin-D levels of patients with lower backache in correlation with BMI. Out of 237 females, 148 were in reproductive age. 132 (89.19%) of these 148 had vitamin-D levels below normal and only 13 (8.78%) had normal vitamin D levels where as 3 (2.02%) had levels in toxic range. In 89 menopausal females, 9 (10.11%) had normal vitamin D levels and 79 (88.76%) had below normal levels. Table 5 shows the vitamin-D level distribution among veil observer and non-veil observer females. Regarding complexion 269 (53.8%) of the patients were of fair complexion while 231 (46.2%) were having dark complexion. Twenty-seven (11.68%) had normal levels among dark complexion group as compared to 23 (8.55%) among fair complexion group
Table 3: Age-wise distribution of vitamin D levels in patients with low backache (n=500).
Table 4: Body Mass Index wise distribution of vitamin D levels in patients with low backache (n=500).
Table 5: Vitamin D levels in veil observer and non-veil observer females in patients with low backache (n=237).
(rounding by VitaminDWiki)
|| |<20 ng/dL| 20-30 ng/dL| 31-100 ng/dL| >100 ng/dL
Veil observer| 80%|14%|6%| 1%
Non-veil observer|48%|33%|16%|4%||
In 215 (43%) of patients with low backache there were paraesthesiae and out of these 191 (88.84%) had vitamin D levels below normal range.
DISCUSSION
Calcium homeostasis in the body involves vitamin D and it is required in sufficient levels for healthy bones.8 Rickets, osteomalacia, osteoporosis are linked with vitamin D deficiency, which is also linked with myopathy, aches and pains. All these conditions in turn can lead to low back pain.69-10 Vitamin D also has anti-inflammatory properties and loss of this can also cause musculoskeletal pain.612 Not enough research is conducted to know the role of vitamin D deficiency in low back pain. Our study showed that 88.4% of patients with low backache had vitamin D levels below normal range with 63% having levels even lower than 20 ng/dL (deficient group). A study in Saudi Arabia7 on chronic low back pain patients showed 83% patients with low back pain had vitamin D deficiency. Similarly a study by Siddique & Malik3 on low backache patients in Islamabad also showed 81% patients having sub-optimal vitamin D levels. An Egyptian study also showed that 81% of low back pain patients had below normal vitamin D levels.16 Similar findings are also observed all around the globe.17-19
Our study also showed that people with BMI <25 kg/m2 had better levels of vitamin D while those with higher BMI had lower levels of vitamin D. Similar findings were noted in many studies across the globe.20-22
In our study fair complexion subjects had lesser vitamin D levels as compared to dark complexion subjects. Only 9.67% among fair complexion group had normal vitamin D levels as compared to 13.86% among dark complexion group. This is in contrast to studies showing that pigmented skin people have more chance of having vitamin D deficiency as increased pigmentation reduces capacity of the skin to manufacture vitamin D from sunlight.20 However, a study conducted in Denmark showed no effect of pigmentation of skin on vitamin D levels.
Sufficient sunlight exposure in term of body surface area and duration for which body is exposed to it is mandatory for manufacturing of vitamin D. Our religious and cultural barriers play important role in this aspect as majority of our female population observe parda and use veil for this purpose. Our study showed that only 6.49% of veil observer females had normal levels as compared to 19.28% of females who don't observe veil. Our study further showed that 79.87% of veil observer females had deficient levels of vitamin D (<20 ng/dL) as compared to 48.19% of non-veil observing females. This finding is in line with studies done by Johansen et al2 and study by Siddique & Malik. Hormonal factors does contribute to metabolism of vitamin D, Calcium and Phosphate suggesting further lower levels of vitamin D in females after their menopause ensues.3 However in our study both reproductive age and menopausal females with low back pain had similar levels of vitamin D. In our study 89.19% of reproductive age females had vitamin D levels below normal as compared to 88.76% of post-menopausal females having lower vitamin D levels. This finding suggests that in our area both reproductive age and post-menopausal women have equally low levels of vitamin D. Our finding was in contrast to few studies which showed that post-menopausal women have even lower levels of vitamin D.32324
In our study 88.83% of patients who had symptom of paraesthesia had lower levels of vitamin D as compared to 88.07% with no such symptoms showing not much difference to associated paraesthesia with vitamin D deficiency. These findings are in line with the finding of Johansen et al.2
CONCLUSION
Vitamin D deficiency is present in majority of patients with low back pain and should be considered a contributing factor in people with idiopathic low back pain.
REFERENCES in PDF
📄 Download the PDF from VitaminDWiki.
See also VitaminDWiki
Back Pain category listing has items along with related searches
Back pain extremely associated with low level of vitamin D – May 2014
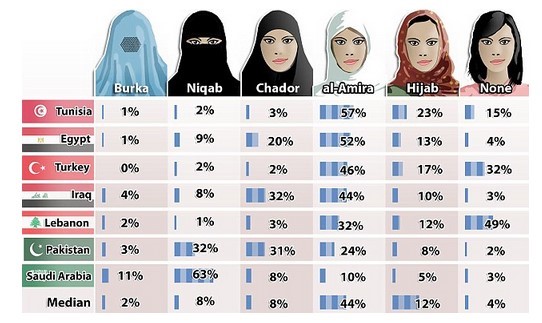
Middle East and Vitamin D category listing has the following graphic