Knee osteoarthritis: Vitamin D is the 4th best treatment – meta-analysis
Symptomatic Efficacy of Pharmacological Treatments for Knee Osteoarthritis: A Systematic Review and a Network Meta-Analysis with a 6-Month Time Horizon
Drugs, . 2020 Oct 19, doi: 10.1007/s40265-020-01423-8
C Beaudart 1, L Lengelé 2, V Leclercq 2, A Geerinck 2, D Sanchez-Rodriguez 2 3, O Bruyère 2, J Y Reginster 2 4
📄 Download the PDF from VitaminDWiki
Introduction: Several pharmacological treatments aiming at a better symptomatic control of osteoarthritis (OA) are used in daily practice but their efficacy is often disputed. The purpose of this network meta-analysis (NMA) is to assess the efficacy on pain and function of the drugs that are most widely prescribed against knee OA.
Methods: Medline, Scopus, and Cochrane database of systematic reviews were searched for randomized controlled trials published up to August 2019 and assessing the efficacy of knee OA treatments using a 6-month time horizon. Pain and function changes from baseline were the primary outcomes. A Bayesian network meta-analysis was run and standardized mean differences (SMDs) with 95% credibility intervals (95% CrIs) were calculated.
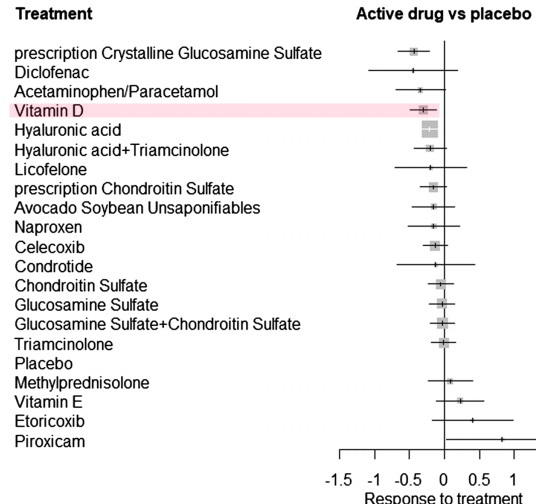
Results: 9697 references were identified and 80 RCTs were concordant with our inclusion criteria (79 studies involving 15,609 individuals reported pain outcomes and 55 studies involving 13,655 individuals reported function outcomes). A significant decrease in pain was observed for the intra-articular (IA) combination of hyaluronic acid (HA) and triamcinolone (SMD - 0.49, 95% CrI - 0.78; - 0.19), vitamin D (SMD - 0.31, 95% CrI - 0.56; - 0.06), IA HA (SMD - 0.29, 95% CrI - 0.40; - 0.17), prescription-grade crystalline glucosamine sulfate (pCGS) (SMD - 0.29, 95% CrI - 0.58; - 0.004), and prescription-grade chondroitin sulfate (pCS) (SMD - 0.26, 95% CrI - 0.44; - 0.08). Significant improvements in physical function were found with pCGS (SMD - 0.44, 95% CrI - 0.66; - 0.21), vitamin D (SMD - 0.30, 95% CrIs - 0.49; - 0.11) and IA HA (SMD - 0.21, 95% CrIs - 0.31; - 0.11).
Conclusion: Six months of treatment with IA HA, pCGS, pCS, vitamin D and the combination of IA HA and triamcinolone improve pain and/or physical function in patients suffering from knee OA.
