Breast cancer chemotherapy benefits from highest vitamin D levels
Pretreatment vitamin D level and response to neoadjuvant chemotherapy in women with breast cancer on the I-SPY trial (CALGB 150007/150015/ACRIN6657).
Cancer Med. 2014 Jun;3(3):693-701. doi: 10.1002/cam4.235. Epub 2014 Apr 9.
Clark AS1, Chen J, Kapoor S, Friedman C, Mies C, Esserman L, DeMichele A; I-SPY1 Investigators.
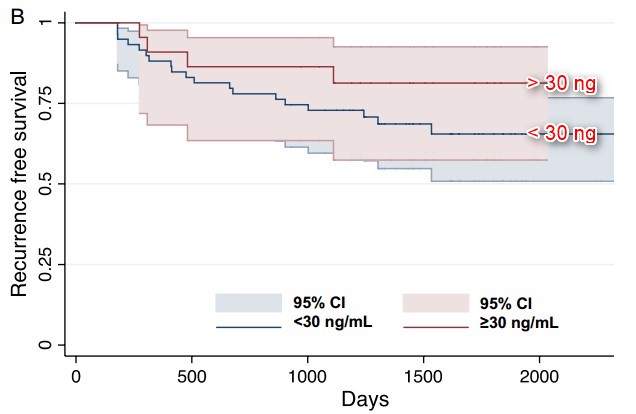 Suspect that there would be a virtually flat survival line for women having > 50 ng of vitamin D
📄 Download the PDF from VitaminDWiki.
See also VitaminDWiki
* 6X less Breast Cancer if have even minimal vitamin D – July 2013
* Vitamin D Might Be Able to Slash Your Breast Cancer Risk by 90 Percent - Baggerly, Mercola: May 2013
* 85 percent less risk of death from Breast Cancer when vitamin D levels higher than 30 ng – May 2012
* Chemotherapy and vitamin D - many studies
* Overview Breast Cancer and Vitamin D
* Chemo drug (Nitrogen Mustard in this study) side effects minimized by vitamin D (mice) – March 2015
* Breast Cancer chemotherapy 2.7 X more likely to be successful if not vitamin D deficient – Dec 2017
Benefits of Vitamin D to Breast Cancer are for levels > 30 ng
Suspect that there would be a virtually flat survival line for women having > 50 ng of vitamin D
📄 Download the PDF from VitaminDWiki.
See also VitaminDWiki
* 6X less Breast Cancer if have even minimal vitamin D – July 2013
* Vitamin D Might Be Able to Slash Your Breast Cancer Risk by 90 Percent - Baggerly, Mercola: May 2013
* 85 percent less risk of death from Breast Cancer when vitamin D levels higher than 30 ng – May 2012
* Chemotherapy and vitamin D - many studies
* Overview Breast Cancer and Vitamin D
* Chemo drug (Nitrogen Mustard in this study) side effects minimized by vitamin D (mice) – March 2015
* Breast Cancer chemotherapy 2.7 X more likely to be successful if not vitamin D deficient – Dec 2017
Benefits of Vitamin D to Breast Cancer are for levels > 30 ng
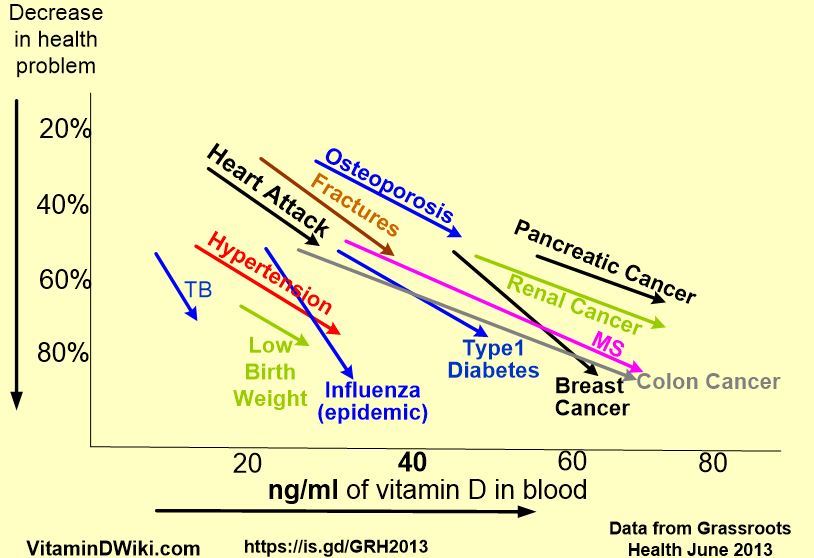 * click on chart for details
* click on chart for details
Laboratory studies suggest that vitamin D (vitD) enhances chemotherapy-induced cell death. The objective of this study was to determine whether pretreatment vitD levels were associated with response to neoadjuvant chemotherapy (NACT) in women with breast cancer. Study patients (n = 82) were enrolled on the I-SPY TRIAL, had HER2-negative tumors, and available pretreatment serum. VitD levels were measured via DiaSorin radioimmunoassay. The primary outcome was pathologic residual cancer burden (RCB; dichotomized 0/1 vs. 2/3). Secondary outcomes included biomarkers of proliferation, differentiation, and apoptosis (Ki67, grade, Bcl2, respectively) and 3-year relapse-free survival (RFS). Mean and median vitD values were 22.7 ng/mL (SD 11.9) and 23.1 ng/mL, respectively; 72% of patients had levels deemed "insufficient" (<30 ng/mL) by the Institute of Medicine (IOM). VitD level was not associated with attaining RCB 0/1 after NACT (univariate odds ratio [OR], 1.01; 95% CI, 0.96-1.05) even after adjustment for hormone receptor status (HR), grade, Ki67, or body mass index (BMI). Lower vitD levels were associated with higher tumor Ki67 adjusting for race (OR, 0.95; 95% CI, 0.90-0.99). VitD level was not associated with 3-year RFS, either alone (hazard ratio [HzR], 0.98; 95% CI, 0.95-1.02) or after adjustment for HR, grade, Ki-67, BMI, or response. VitD insufficiency was common at the time of breast cancer diagnosis among women who were candidates for NACT and was associated with a more proliferative phenotype. However, vitD levels had no impact on tumor response to NACT or short-term prognosis.
© 2014 The Authors. Cancer Medicine published by John Wiley & Sons Ltd.
PMID: 24719175
