Not enough vitamin D during pregnacy in Australia – PHD
Vitamin D Related Behaviours Among Pregnant Women in Australia
Yue Wu, Paediatrician, MMed, BM
Submitted in fulfilment of the requirements for the degree of Doctor of Philosophy
School of Public Health & Social Work Faculty of Health Institute of Health and Biomedical Innovation Queensland University of Technology, October 2013
This is based on web questionare, with no selection of who answered the questionare
Does not appear to consider > 600 IU of vitamin D, the extremely low standard in Austalia
PDF is attached at the bottom of this page
See also VitaminDWiki
National Vitamin D awareness day (Australia, 1000 IU max) - Aug 9 2013
Australian dermatologists had lower vitamin D levels than elderly in hospitals – 2009
Nutrition authorities in Aust and NZ ignoring vitamin D deficiency - July 2012
RCT confirms that Australians need at least 2000 IU vitamin D – Dec 2012
Vitamin D testing in Australia - huge increase in 11 years - July 2012
Black Sudanese children 350X more likely to have rickets than other Australians – April 2012 (Did not notice any mention of dark skin in this PDF dissertation)
2 out of 3 people think that they get enough vitamin D, but only 1 in 3 get even the absolute minimum – Oct 2013 US survey, suspect Australia is similar
Overview Pregnancy and vitamin D which has the following summary
- {include}
Abstract
Maternal vitamin D deficiency during pregnancy has numerous health implications in both the mothers and their offspring, therefore, it is important to prevent women from vitamin D deficiency during this period. Even in Australia, with high levels of sunlight (which is the primary source of vitamin D in human beings), pregnant women have been reported to be at increased risk of vitamin D deficiency.
Because the determinants of vitamin D status are skin exposure to sunlight and oral intake of vitamin D from both foods and supplements, an individual's vitamin D status is affected by his or her sun exposure behaviours, such as time spent outdoors, clothing coverage and sunscreen use, as well as dietary behaviours. However, there is a lack of basic observational data on those sun exposure and dietary behaviours in pregnant women. In consideration of the high prevalence of vitamin D deficiency in pregnant women, and making effective strategies to prevent this issue, it is important to understand how pregnant women behave in regard to sun exposure and vitamin D intake.
This study aims to investigate these vitamin D related behaviours, including time outdoors, clothing, sunscreen use, dietary vitamin D intake and vitamin D supplement ingestion among pregnant women in Australia. One hundred and sixty-four pregnant women throughout Australia participated in web-based questionnaires with regard to their vitamin D related behaviours and the potential influencing factors, such as demographics, obstetrical variables, their knowledge and attitudes to vitamin D. Subsequently, 132 out of the whole 164 women completed a follow-up, online, pilot survey after their delivery to report their pregnancy outcomes, which aimed to explore the potential link between maternal vitamin D related behaviours during pregnancy and pregnancy outcomes.
The mean outdoor time for pregnant women in Australia was 52.46 (95% CI: 45.60 -60.34) minutes per day(median: 60 minutes per day) on weekdays and was 89.12 (95% CI: 77.48 - 102.51) minutes per day (median: 90 minutes per day) on weekends. On average, 78% of their skin was covered by clothing whilst outdoors. Approximately half of the women applied sunscreen in the previous month.
The median dietary intake among these pregnant women was only 1.38 ug per day from foods. Of those who responded, 22.6% did not use of vitamin D supplements, whereas 12.8% reported consuming < 500 IU per day. Women living in a low ambient temperature or ultraviolet radiation environment covered their skin more with clothing, but were less likely to apply sunscreen. Women on > 500 IU per day vitamin D supplements covered their skin more with clothing and tended to have less UV adjusted, outdoor time. No significant differences were found between maternal vitamin D related behaviours and pregnancy outcomes in the follow-up, pilot study.
In conclusion, pregnant women in Australia have low sun exposure and limited vitamin D intake, which may explain why pregnant women are prone to vitamin D deficiency in this country.
Main findings:
• Pregnant women in Australia get limited sun exposure.
• The intake of vitamin D from foods is low in Australian pregnant women who participated in this study.
• The application of vitamin-D-containing supplements in Australian pregnant women is greater than other populations in both proportion and amount, but for the majority of them, the intake amount still does not meet the current recommendations (15 ug per day).
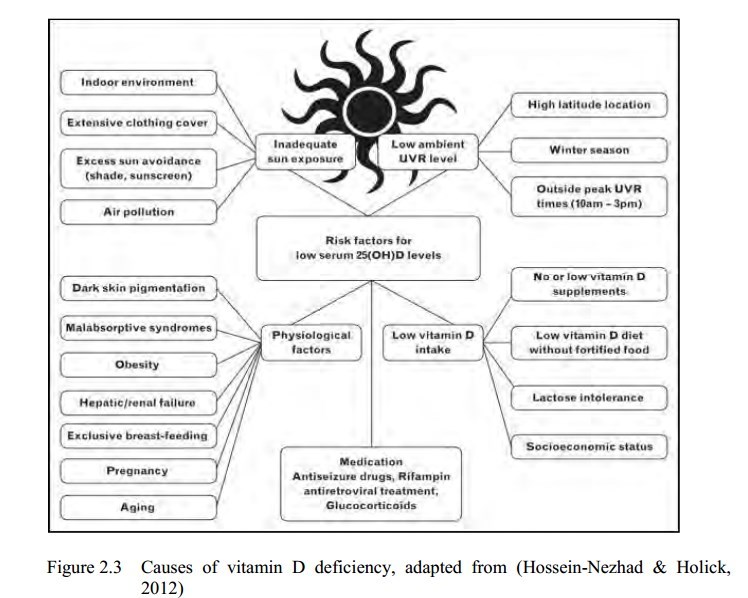
Table of Contents
KEYWORDS .......I
ABSTRACT ......II
TABLE OF CONTENTS...IV
LIST OF TABLES....VII
LIST OF FIGURES...IX
LIST OF ABBREVIATIONS......X
STATEMENT OF ORIGINAL AUTHORSHIP.....XI
ACKNOWLEDGEMENTS......XII
CHAPTER 1: INTRODUCTION.......1
1.1 BACKGROUND AND RATIONALE FOR THE STUDY.....1
1.1.1 Background.1
1.1.2 Rationale for this Study......8
1.2 RESEARCH AIM, OBJECTIVES AND RESEARCH QUESTIONS.....8
1.3 SIGNIFICANCE.......9
1.4 THESIS OUTLINE.10
CHAPTER 2: LITERATURE REVIEW.11
2.1 INTRODUCTION ..11
2.2 BACKGROUND OF VITAMIN D12
2.2.1 Sources of Vitamin D12
2.2.2 Metabolism of Vitamin D.13
2.2.3 Assessment of Vitamin D Status.......14
2.2.4 Classification of Vitamin D Status....15
2.2.5 Function of Vitamin D......16
2.2.6 Epidemiology of Vitamin D Deficiency...19
2.2.7 Causes of Vitamin D Deficiency......19
2.2.8 Prevention and Treatment for Vitamin D Deficiency.......21
2.2.9 Vitamin D in Australia......23
2.3 VITAMIN D IN PREGNANCY.....24
2.3.1 Adaptations of Vitamin D Metabolism in Pregnancy.......25
2.3.2 Prevalence of Vitamin D Deficiency in Pregnancy...26
2.3.3 Maternal Health Consequences of Vitamin D Deficiency in Pregnancy..27
2.3.4 Offspring Health Consequences of Maternal Vitamin D Deficiency in Pregnancy.29
2.4 STUDIES OFBEHAVIOURS IN RELATION TO VITAMIN D..33
2.5 SUMMARY ....35
CHAPTER 3: RESEARCH DESIGN.......37
3.1 RESEARCH DESIGN....37
3.2 SAMPLE.38
3.2.1 Inclusion Criteria......38
3.2.2 Sample Size Calculation...38
3.3 QUESTIONNAIRE DEVELOPMENT..39
3.3.1 The Baseline Survey .40
3.3.2 The Follow-up Survey......41
3.4 SURVEY TEST AND ACTIVATION...42
3.5 RECRUITMENT ....42
3.6 RESEARCH ADMINSTRATION..43
3.7 DATA COLLECTION....44
3.8 THE MAJOR VARIABLES IN THIS THESIS......46
3.8.1 Dependent Variables .46
3.8.2 Independent Variables.......51
3.8.3 Pregnancy Outcome Variables..53
3.9 DATA ANALYSIS.54
3.9.1 Data Coding ......54
3.9.2 Data Cleaning....55
3.9.3 Data Analysis Plan ....56
3.10 ETHICAL CONSIDERATIONS ....58
CHAPTER 4: RESULTS...61
4.1 DEMOGRAPHIC CHARACTERISTICS ......61
4.2 OBSTETRICAL VARIABLES......65
4.3 KNOWLEDGE AND ATTITUDES TO VITAMIN D..66
4.3.1 Knowledge66
4.3.2 Attitudes....70
4.4 SUN EXPOSURE AND PROTECTIVE BEHAVIOURS......72
4.4.1 Outdoor Time....72
4.4.2 Clothing ....83
4.4.3 Sunscreen Use ...87
4.5 VITAMIN D INTAKE....95
4.5.1 Dietary Vitamin D Intake..95
4.5.2 Vitamin D Supplement......98
4.6 ASSOCIATIONS BETWEEN KNOWLEDGE/ATTITUDE AND BEHAVIOURS...102
4.6.1 The Associations between Knowledge and Behaviours..102
4.6.2 The Associations between Attitude and Behaviours.......103
4.7 RELATIONSHIPS BETWEEN VITAMIN D RELATED BEHAVIOURS104
4.7.1 Relationships between Sun Exposure and Sun Protective Behaviours...104
4.7.2 Relationship between Dietary Vitamin D Intake and Vitamin D Supplement104
4.7.3 Relationships between Sun Related Behaviours and Vitamin D Intake Behaviours......104
4.8 PREGNANCY OUTCOMES.......107
4.9 VITAMIN D STATUS DURING PREGNANCY108
4.10 MATERNAL VITAMIN D RELATED BEHAVIOURS DURING PREGNANCY
AND PREGNANCY OUTCOMES ......109
4.10.1 Maternal Vitamin D Related Behaviours and Delivery Type.111
4.10.2 Maternal Vitamin D Related Behaviours and Weight Gain....112
4.10.3 Maternal Vitamin D Related Behaviours and Gestational Age.......113
4.10.4 Maternal Vitamin D Related Behaviours and Birth Weight...114
4.10.5 Maternal Vitamin D Related Behaviours and Birth Length....115
4.10.6 Maternal Vitamin D Related Behaviours and Head Circumference.......116
4.11 MATERNAL ATITUDES AND PRACTICE OF SUN EXPSOURE AND VITAMIN
D REGARDING THE NEW INFANT.118
4.11.1 Maternal Attitudes and Practice for the New Infant118
4.11.2 Associations between Maternal Behaviours to Themselves and Their Attitudes and Practice to Their New Infants Regarding Vitamin D and Sun Exposure .119
CHAPTER 5: DISCUSSION...123
5.1 SAMPLE CHARACTERISTICS..123
5.2 SUN EXPOSURE AND PROTECTIVE BEHAVIOURS...124
5.2.1 Outdoor Time..125
5.2.2 Clothing ..127
5.2.3 Sunscreen Use.128
5.2.4 Summary .130
5.3 VITAMIN D INTAKE..131
5.3.1 Dietary Vitamin D Intake132
5.3.2 Vitamin D Supplement...134
5.3.3 Summary.137
5.4 KNOWLEDGE AND ATTITUDES TO VITAMIN D139
5.4.1 Knowledge of Vitamin D139
5.4.2 Attitudes to Vitamin D....141
5.4.3 Associations between Knowledge/Attitude and Behaviours...141
5.5 RELATIONSHIPS BETWEEN VITAMIN D RELATED BEHAVIOURS142
5.6 MATERNAL VITAMIN D RELATED BEHAVIOURS DURING PREGNANCY AND PREGNANCY OUTCOMES......143
5.7 MATERNAL VITAMIN D RELATED BEHAVIOURS DURING PREGNANCY, AND ATTITUDES AND PRACTICES TOWARDS THE NEW INFANTS REGARDING VITAMIN D AND SUN EXPOSURE .145
5.8 COMPARISONS WITH AUSTRALIAN NORMATIVE DATA146
CHAPTER 6: CONCLUSION151
6.1 SUMMARY OF FINDINGS151
6.2 STUDY STRENGTHS AND LIMITATIONS.....152
6.3 IMPLICATIONS FOR PRACTICE .....154
6.4 IMPLICATIONS FOR FUTURERESEARCH ....155
BIBLIOGRAPHY.....157
APPENDICES...173
Appendix A Survey One (the initial survey).173
Appendix B Survey Two (the follow-up survey)..219
Appendix C Ethical Application Approval Letter.225
Appendix D Ethics Variation Approval Letter.....226
Appendix E Recruitment Advertisement in Newspapers......227
Appendix F Recruitment Advertisement at QUT Website....239
Appendix G Recruitment Advertisement at Other Websites240
Appendix H Follow-up Invitation Letter......241
List of Tables
Table 1. 1 Worldwide prevalence of vitamin D deficiency during pregnancy..4
Table 1.2 Australia nationwide prevalence of vitamin D deficiency during pregnancy...4
Table 1.3 Observational studies of vitamin D intake from foods and supplements in pregnant women ....... 7
Table 2.1 Vitamin D Recommendations by the IOM and Dr.Holick.....23
Table 3. 1 UV weight at different time period.48
Table 4.1 Demographic characteristics for sample (N=164)..63
Table 4.2 Obstetrical variables for sample (N=164).......65
Table4.3 Knowledge of health problems among 164 participants.67
Table 4.4 Knowledge of symptoms and signs among 164 participants..68
Table 4.5 Knowledge of how to get vitamin D among 164 participants69
Table 4.6 Knowledge of main strategy to get vitamin D among 164 participants..70
Table 4.7 Attitudes toward vitamin D of 164 participants N (%)...71
Table 4.8 Comparison of outdoor time per hour at three time periods (minute/hour)....73
Table 4.9 Comparison of outdoor time on weekdays and weekends......74
Table 4.10 Factors and daily UV adjusted outdoor time..76
Table 4.11 General linear model for UV adjusted outdoor time.......82
Table 4.12 Clothing patterns.....83
Table 4.13 Factors and total clothing score......84
Table 4.14 General linear model for total clothing score..87
Table 4.15 Description of sunscreen use for whole sample (N = 164).....88
Table 4.16 Factors and sunscreen use.......89
Table 4.17 Binary logistic regression for sunscreen use (N=164)....94
Table 4.18 Factors and daily dietary vitamin D intake.....95
Table 4.19 Binary logistic regression for daily dietary vitamin D intake (N=164)..97
Table 4.20 Factors and daily vitamin D supplements.......99
Table 4.21 Binary logistic regression for vitamin D supplement (N=164).....101
Table 4.22 Correlations of vitamin D knowledge score and behaviours102
Table 4.23 Correlations of vitamin D attitude score and behaviours......103
Table 4.24 Pregnancy outcomes.....108
Table 4.25 Thirteen participants' vitamin D statuses.....109
Table 4.26 Descriptions of six pregnancy outcomes for 132 mother-child pairs....110
Table 4.27 Maternal vitamin D related behaviours and delivery type (N=132).....112
Table 4.28 Maternal vitamin D related behaviours and weight gain (N=129)113
Table 4.29 Maternal vitamin D related behaviours and gestational age (N=132)..114
Table 4.30 Maternal vitamin D related behaviours and birth weight (N= 132).......115
Table 4.31 Maternal vitamin D related behaviours and birth length (N= 132)116
Table 4.32 Maternal vitamin D related behaviour and head circumference (N=132)....117
Table 4.33 Associations between maternal vitamin D related behaviours to themselves and their attitudes and practices towards the new infant.....120
Chapter 6: Conclusion
The purpose of this final chapter is to summarise and integrate the main findings from previous chapters of this study.
A discussion of strengths and limitations of the research is offered, followed by implications for public health and future research.
6.1 SUMMARY OF FINDINGS
This study has identified possible explanations that may prevent women in Australia from obtaining adequate vitamin D during pregnancy.
Pregnant women in Australia spend limited time outside. When in the sun, they would like to cover, on average, 78% of the body surface.
Half of them use sunscreen to protect their skin, and 30+ is the universal SPF in use.
The amount of vitamin D acquired from food is extremely low among pregnant women in Australia. Even though the proportion of these women taking vitamin D supplements is relatively higher than other populations, there are still over one-fifth going without any vitamin D supplements during pregnancy. In consideration of the dose, according to the latest recommendation from the Institute of Medicine, USA, the daily allowance of vitamin D is 600 IU (15 ug) for people aged one to 70 years, including pregnant women. The participants are short of this recommendation, with only one-third achieving 600 IU per day for vitamin D intake both from foods and supplements.
There are some influencing factors that may affect pregnant women's vitamin D related behaviours, such as educational level, residential region and season. These might be important indicators when screening for pregnant women at risk of vitamin D deficiency in Australia. Furthermore, pregnant women have a relatively good knowledge of vitamin D, even though there is some confusion (knowing of the health problems of vitamin D deficiency, but not being able to cite any symptoms or signs). However, their attitudes to vitamin D are ambiguous, with similar proportions on either positive or negative sides with approximately one-fifth keeping neutral. Additionally, the knowledge and attitudes do not directly result in actual behaviours.
There is a counteraction between sun exposure and vitamin D supplement use among the participants. Pregnant women who take a vitamin D supplement of < 500 IU per day cover themselves less by clothing than women on a dose of > 500 IU per day. Pregnant women taking a vitamin D supplement of < 500 IU per day tend to have longer UV adjusted outdoor times than women on > 500 IU per day. Therefore, only using sun exposure and protective behaviours or vitamin D intake to predict vitamin D status may not be sufficient.
The data lack evidence showing the relationships between maternal vitamin D related behaviours and pregnancy outcomes in this study. However, as mentioned in Chapter 3, the secondary research questions were addressed in an exploratory manner. Taking into account the relatively small sample size, it is likely to be underpowered to detect the relationships. It cannot, therefore, be ruled out that such associations exist. The findings lack the sensitivity needed to fully define the influence of vitamin D status on the course and outcomes of pregnancy. However, as a secondary aim in this study, the interest is in gathering preliminary data, and the resultant data do show some significance to warrant further studies.
6.2 STUDY STRENGTHS AND LIMITATIONS
One of the strengths of this study is that it is believed to be the first study in Australia to investigate pregnant women's vitamin D related behaviours systematically, including sun exposure and protective behaviours, as well as vitamin D intake from both food and supplements. Secondly, by using a web-based survey, a nationwide and diverse group of pregnant women is approached and assessed in this study. Thirdly, UV adjusted outdoor time is applied in the data analysis, which is more accurate when related to vitamin D synthesis. Finally, the study is cost effective, which is suitable for a PhD project.
The study's limitations need to be noted so that the data can be understood correctly.
First, its main limitation is the relatively small sample size. In light of the sample size calculation, as described in Chapter 3, it is sufficient to estimate the mean levels or prevalence of five vitamin D related behaviours with a certain degree of accuracy. However, it is likely to be underpowered in detecting the relationships between these behaviours, influencing factors and other variables. The limited sample size of this study precludes a comprehensive understanding of the factors influencing vitamin D related behaviours, as well as the implications of pregnancy outcomes.
The second limitation is that this study relies on self-reported information. Reports are subject to recall bias and are best thought of as indicating what pregnant women think they did rather than what 'actually happened' last month. It is possible that some individuals incorrectly reported their behaviours, which are subject to recall bias.
Third, the participants of this study generally had a higher educational level, which is not representative of the entire Australian population. It is possible that an awareness of vitamin D benefits might be higher in this particular group. Sun exposure could also be different for this group, as educational levels have been linked to sun exposure (El-Hajj Fuleihan, 2009). Therefore, the generalisability of the study is limited, however, as an exploratory study; the aim to stimulate some attention to this subject has been achieved.
Fourth, a database of all known vitamin D containing diets and supplements in Australia has not been developed. Such a database would enable a more accurate estimate of oral vitamin D intake. Also, the vitamin D amount obtained from food depends on the cooking and feeding methods. However, the latter point is not considered in this study and estimation is relied on, using the mean value of each food type. It is, therefore, uncertain whether the estimated intakes in this study reflect the real intake.
Fifth, there is no control group in this study. Instead the data is compared with that from previous literature. The associations found may have been stronger if this study had been designed as a case control study.
Sixth, the optimal design is to conduct a longitudinal, prospective study and trace women pre-pregnancy to post pregnancy, which could reflect how current vitamin D related behaviours may have changed since the respondents become pregnant.
Therefore, a large-sample-sized, representative, case-controlled and longitudinal study is needed to further investigate vitamin D related behaviours among pregnant women, who are prone to vitamin D deficiency. The data collected here are preliminary and can be used to conduct power analyses for future studies.
6.3 IMPLICATIONS FOR PRACTICE
In recent years, vitamin D has been a focus of growing interest in public health nutrition. Vitamin D insufficiency is common around the world. The reasons might be multifactorial, but probably stem from a combination of decreased dietary intake of vitamin D and decreased sun exposure.
There is no doubt that sun exposure causes health issues, especially it being the main reason for the development of skin cancer. Therefore, excessive sun exposure has to be avoided. However, strict sun avoidance may induce the risk of vitamin D deficiency. Pregnant women have a high prevalence of vitamin D deficiency and inadequate sun exposure, at least partially, contributes to this issue. Media campaigns have highlighted the purported harm of sun exposure by the delivery of "slip, slop, slap" and other messages to the population of Australia. However, in light of the benefits of sun exposure, there is a need to find a balance in order to minimise the risk of skin cancer and maximise vitamin D synthesis from sun exposure. Public health and other intervention strategies to facilitate appropriate sun exposure in this vulnerable population should, therefore, be developed.
It has been suggested that pregnancy is a time to motivate women to improve health maximally. While it is important to be sun safe, it is equally as important to ensure the intake of a regular dose of adequate vitamin D. People can increase their vitamin D intake from both food and supplements, alternatively, while sun exposure is unavailable. Generally, of the pregnant women studied in the present investigation, the overall intake of vitamin D from food was not sufficient. Thus, pregnant women should be informed of suitable food sources, and it would be best to recommend taking the correct supplementary amounts to meet their bodily needs under the guidance of their licensed healthcare provider. Considering its safety, low costs and potentially wide, broad-range beneficial effects on both mothers and offspring, it could lead to a structural measurement and use of vitamin D supplementation in pregnancy.
How to improve the vitamin D status of pregnant women in Australia? The strategies might not be only restricted to sun exposure or vitamin D intake. A combination of multiple strategies might be more practical, with consideration of the availability of sun exposure and dietary sources. Furthermore, consideration of the cautionary guidelines to limit sun exposure to prevent skin cancer, and limited food types containing adequate vitamin D, either naturally or by fortification, it seems that vitamin D supplementation prescribed to pregnant women as routine has a high priority. Future research ought to look at sunlight exposure and supplement use, together with dietary intake and the maternal vitamin D status, in order to decipher how much vitamin D needs to be consumed to reach recommendations.
It is also important to detect and treat vitamin D deficiency in this population. Pregnancy is an opportune time for health care providers to give targeted, practical advice that will help women to better understand the risks associated with being vitamin D deficient. At present, vitamin D screening and supplementation are not routinely offered to all pregnant women. Thus, it is important for health care providers to identify those pregnant women at a higher risk of vitamin D deficiency.
6.4 IMPLICATIONS FOR FUTURE RESEARCH
With the mounting evidence that lower levels of vitamin D are associated with an increased risk of adverse pregnancy outcomes, improving the maternal vitamin D status in pregnancy has a tremendous capacity to benefit public health. This study's data adds to the growing body of research supporting the assertion that the current individual lifestyle (low sun exposure and low vitamin D intake) might be directly attributable to the epidemic of vitamin D deficiency during pregnancy in Australia.
Taking into account the limitations of the current study, large-sample-sized, case-controlled studies, with representative populations, are needed in the future to better investigate the potential influencing factors for maternal vitamin D related behaviours during pregnancy and their direct implications for pregnancy outcomes. Meanwhile, an optimal serum vitamin D level during pregnancy has not been determined and remains an area of active research. Additionally, exactly how much sun exposure is needed for maintaining an optimal vitamin D level during pregnancy is not clear. This remains to be elucidated in future studies.
Some pregnant women cannot obtain adequate vitamin D through sun exposure, and limited food sources are available and supplementation seems to be more easily implemented, but how much vitamin D should be recommended to pregnant women is still debated. More studies are needed to provide conclusive evidence on effective, but also safe, doses of vitamin D supplements during pregnancy.
