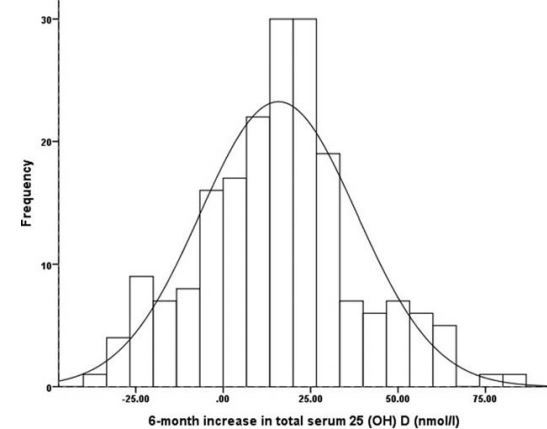
Response to a large dose of vitamin D (80,000 IU) typically varied by 2 X
Molecular evaluation of vitamin D responsiveness of healthy young adults.
J Steroid Biochem Mol Biol. 2017 Nov;174:314-321. doi: 10.1016/j.jsbmb.2016.06.003. Epub 2016 Jun 6.
Seuter S1, Virtanen JK2, Nurmi T2, Pihlajamäki J2, Mursu J2, Voutilainen S2, Tuomainen TP2, Neme A1, Carlberg C3 carsten.carlberg@uef.fi.
1 School of Medicine, Institute of Biomedicine, University of Eastern Finland, Kuopio, Finland.
2 Institute of Public Health and Clinical Nutrition, University of Eastern Finland, Kuopio, Finland.
3 School of Medicine, Institute of Biomedicine, University of Eastern Finland, Kuopio, Finland.
 * Reasons for low response to vitamin D
* How you might double your response to vitamin D
* Includes co-factors, different forms of Vitamin D. time of day it is taken, etc.
* Vitamin D responses to as much as 15,000 IU per day – Feb 2017
* Response to Vitamin D supplementation – July 2015
* How to predict response to a vitamin D dose – RCT April 2014
* Vitamin D injection helped migrants a bit, but some had poor or even negative responses – Dec 2017
* Note: There may be even larger variation in the amount of Vitamin D getting to cells due to poor Genetics
* Response by obese to weekly 50,000 IU of Vitamin D – May 2018
*
* Reasons for low response to vitamin D
* How you might double your response to vitamin D
* Includes co-factors, different forms of Vitamin D. time of day it is taken, etc.
* Vitamin D responses to as much as 15,000 IU per day – Feb 2017
* Response to Vitamin D supplementation – July 2015
* How to predict response to a vitamin D dose – RCT April 2014
* Vitamin D injection helped migrants a bit, but some had poor or even negative responses – Dec 2017
* Note: There may be even larger variation in the amount of Vitamin D getting to cells due to poor Genetics
* Response by obese to weekly 50,000 IU of Vitamin D – May 2018
* 
📄 Download the PDF from Researchgate via VitaminDWiki
3X difference in responses to a single dose of 80,000 IU of Vitamin D
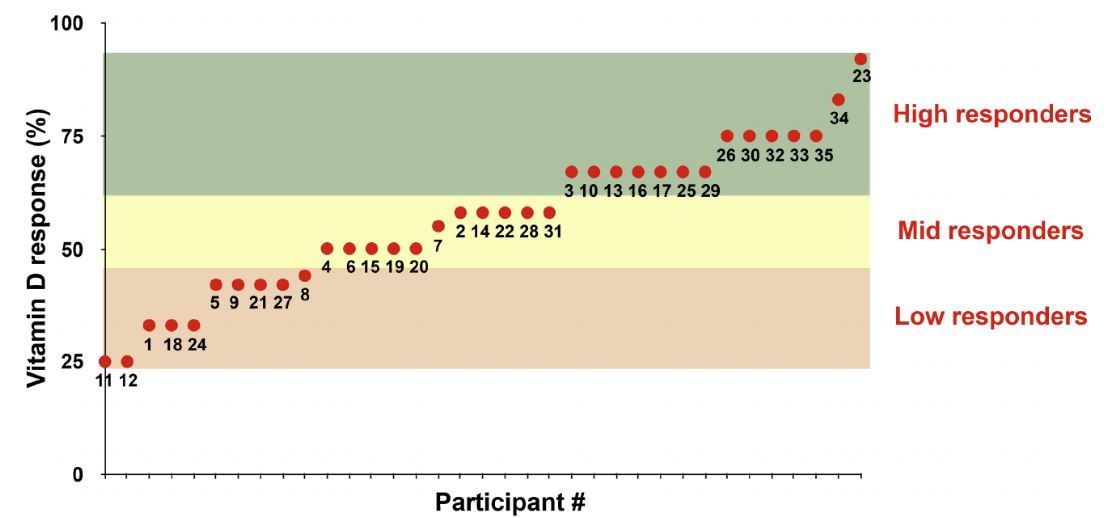
Vitamin D3 has via its metabolites 25-hydroxyvitamin D3 (25(OH)D3) and 1α,25-dihydroxyvitamin D3 (1,25(OH)2D3) direct effects on the transcriptome and the epigenome of most human cells. In the VitDbol study we exposed 35 healthy young adults to an oral vitamin D3 dose (2000μg) or placebo and took blood samples directly before the supplementation as well as at days 1, 2 and 30. Within 24h the vitamin D3 intake raised the average serum levels of both 25(OH)D3 and 1,25(OH)2D3 by approximately 20%.
However, we observed large inter-individual differences in these serum levels, reflected by the average ratios between 25(OH)D3 and 1,25(OH)2D3 concentrations ranging from 277 to 1365. Interestingly, average serum parathyroid hormone (PTH) levels increased at day 1 by some 10% but then decreased within the following four weeks to levels 5% below baseline. In peripheral blood mononuclear cells (PBMCs) that were isolated at the same time points we determined vitamin D-modulated chromatin accessibility by FAIRE-qPCR at selected genomic loci. This method is well suited to evaluate both short-term and long-term in vivo effects of vitamin D on the epigenome of human subjects. The differential vitamin D responsiveness of the VitDbol study participants was determined via individual changes in their PTH levels or chromatin accessibility in relation to alterations in 25(OH)D3 concentrations. This led to the segregation of the subjects into 14 high, 11 mid and 10 low responders. In summary, the vitamin D responsiveness classification provides additional information compared to a vitamin D status assessment based on single 25(OH)D3 serum measurements. The study was registered at Clinicaltrials.gov (NCT02063334).
PMID: 27282116 DOI: 10.1016/j.jsbmb.2016.06.003
