Radio frequency ablation survival doubled with even modest levels of vitamin D
Prognostic role of 25-hydroxyvitamin d in patients with liver metastases from colorectal cancer treated with radiofrequency ablation.
J Gastroenterol Hepatol. 2016 Feb 20. doi: 10.1111/jgh.13326. [Epub ahead of print]
Facciorusso A1, Del Prete V1, Muscatiello N1, Crucinio N1, Barone M1.
1Gastroenterology Unit, University of Foggia, Italy.
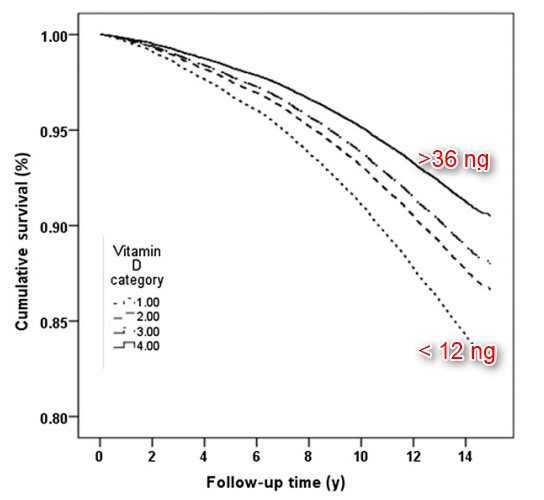 click on chart for details
click on chart for details
BACKGROUND AND AIM:
Vitamin D is implicated in the etiology of several neoplastic diseases but its relationship with colorectal cancer survival is still unclear. Aim of this study was to determine whether vitamin D levels influence survival outcomes in colorectal cancer liver metastases patients treated with percutaneous radiofrequency ablation.
METHODS:
We measured 25-hydroxyvitamin D levels in 143 patients with 215 colorectal liver metastases who underwent radiofrequency ablation between 1999 and 2011 at our Institution. The influence of 25-hydroxyvitamin D levels on overall survival and time to recurrence was evaluated in univariate and multivariate Cox analyses.
RESULTS:
Median age was 68 years (range 41-85) and median number of nodules was 2 (1-3) with a median maximum diameter of 26 mm (10-48). Median survival was 44 months (36-62) and survival rate was 91.4%, 46.5% and 42.2% at 1, 4 and 5 years in the whole cohort.
Median survival was 65 months (52-74) if 25-hydroxyvitamin D > 20 ng/mL and 34 months (24-41) if ≤ 20 ng/mL ( p < 0.001). In the whole cohort median time to recurrence was 34 months (26-47), 50 months (36-62) in the case of 25-hydroxyvitamin D > 20 ng/mL and 24 months (20-32) if ≤ 20 ng/mL (p < 0.001). Nodule size and 25-hydroxyvitamin D resulted as significant predictors of both overall survival and time to recurrence in multivariate analysis.
CONCLUSIONS:
Our study provides support for the use of 25-hydroxyvitamin D as a new predictor of outcome for colorectal liver metastases patients. This article is protected by copyright. All rights reserved.
PMID: 26896637
