Preterm births reduced in half if 40 ng of vitamin D in 3rd trimester
Post-hoc comparison of vitamin D status at three timepoints during pregnancy demonstrates lower risk of preterm birth with higher vitamin D closer to delivery.
J Steroid Biochem Mol Biol. 2014 Nov 13. pii: S0960-0760(14)00268-4. doi: 10.1016/j.jsbmb.2014.11.013. [Epub ahead of print]
Wagner CL1, Baggerly C2, McDonnell SL2, Baggerly L2, Hamilton SA3, Winkler J3, Warner G3, Rodriguez C3, Shary JR4, Smith PG4, Hollis BW4.
1Medical University of South Carolina Children's Hospital, Charleston, SC, USA. Electronic address: wagnercl@musc.edu.
2 GrassrootsHealth, Encinitas, CA, USA.
3 Eau Claire Cooperative Health Centers, Columbia, SC, USA.
4 Medical University of South Carolina Children's Hospital, Charleston, SC, USA.
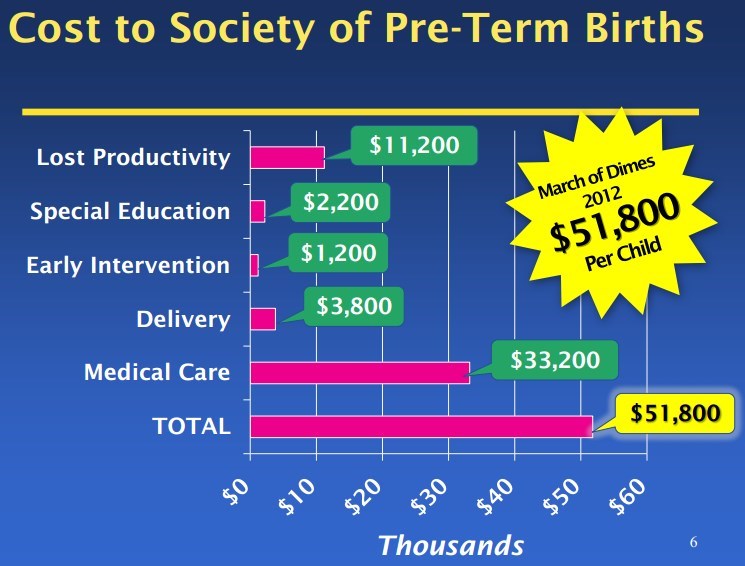 Click on chart for details by some of the coauthors of this study
📄 Download the PDF from VitaminDWiki.
Click on chart for details by some of the coauthors of this study
📄 Download the PDF from VitaminDWiki.
Highlights
Association between serum 25(OH)D and preterm birth during 3 timepoints was examined.
25(OH)D value closest to delivery more strongly correlated with preterm birth.
Findings most notable in Hispanic women.
47% lower preterm birth rate associated with 25(OH)D >100 nmol/L at 27 weeks.
Later intervention as rescue therapy may positively impact risk of preterm delivery.
There have been observational reports that maternal vitamin D status at baseline and not closest to delivery is a better predictor of pregnancy outcomes, suggesting that a cascade of events is set into motion that is not modifiable by vitamin D supplementation during later pregnancy. To address this issue, in this exploratory post-hoc analysis using correlation and logistic regression, we sought to measure the strength of the association between serum 25(OH)D concentrations at 3 timepoints during pregnancy: baseline, 1st trimester (<16 weeks); 2nd trimester (16–26 weeks); and 3rd trimester (≥27 weeks) and preterm birth. It was hypothesized that the 25(OH)D value closest to delivery would be most significantly associated with preterm birth. To accomplish this objective, the datasets from NICHD (n = 333) and Thrasher Research Fund (n = 154) vitamin D supplementation pregnancy studies were combined.
The results of this analysis were that 25(OH)D values closer to delivery were more strongly correlated with gestational age at delivery than earlier values:
1st trimester: r = 0.11 (p = 0.02);
2nd trimester: r = 0.08 (p = 0.09); and
3rd trimester: r = 0.15 (p = 0.001).
When logistic regression was performed with preterm birth (<37 weeks) as the outcome and 25(OH)D quartiles as the predictor variable, adjusting for study and participant race/ethnicity, as with the correlation analysis, the measurements closer to delivery were more significantly associated and had a higher magnitude of effect.
That is, at baseline, those who had serum concentrations <50 nmol/L (20 ng/mL) had 3.3 times of odds of a preterm birth compared to those with serum concentrations ≥100 nmol/L (40 ng/mL; p = 0.27).
At 2nd trimester, the odds were 2.0 fold (p = 0.21) and at the end of pregnancy, the odds were 3.8 fold (p = 0.01).
The major findings from this exploratory analysis were: (1) maternal vitamin D status closest to delivery date was more significantly associated with preterm birth, suggesting that later intervention as a rescue treatment may positively impact the risk of preterm delivery, and (2) a serum concentration of 100 nmol/L (40 ng/mL) in the 3rd trimester was associated with a 47% reduction in preterm births .
This article is part of a Special Issue entitled '17th Vitamin D Workshop'. (June 2014)
Copyright © 2014 Elsevier Ltd. All rights reserved.
PMID: 25448734
Short url = http://is.gd/preterm2x
