Inflammatory Bowel Disease associated with low Vitamin D, low Zinc, and low Selenium
Risk Factors for Vitamin D, Zinc, and Selenium Deficiencies in Korean Patients with Inflammatory Bowel Disease.
Gut Liver. 2017 May 15;11(3):363-369. doi: 10.5009/gnl16333.
Han YM1,2, Yoon H3, Lim S3, Sung MK4, Shin CM3, Park YS3, Kim N1,3, Lee DH1,3, Kim JS1,2.
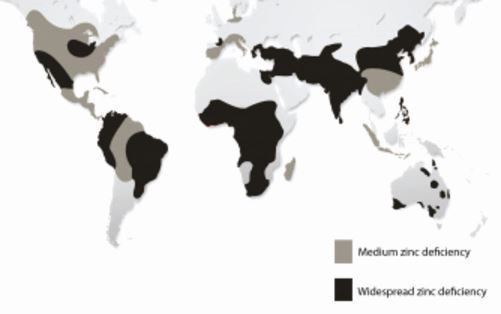 Map from the Zinc category pages suggests that IBD Zinc deficiency is not constant around the world
Note: This 2017 study was from Korea, where they appear to have little Zinc in their crops
1. Overview Gut and vitamin D contains the following summary
{include}
1. Gut category listing contains the following
{include}
---
1. # From the PDF
< 40 years, 3.7 X more likely to have low Zinc
" patients younger than 40 years were at increased risk for zinc deficiency (RR, 3.683; 95% CI, 1.152 to 11.777; p=0.028) "
Females 4.9 X more likely to have low Selenium
"Female sex (RR, 4.871; 95% CI, 1.352 to 17.544; p=0.015) and low serum albumin levels (<3.3 g/dL; RR, 10.346; 95% CI, 1.035 to 103.447; p=0.047) were independent risk factors for selenium deficiency by multivariate logistic regression analysis"
Map from the Zinc category pages suggests that IBD Zinc deficiency is not constant around the world
Note: This 2017 study was from Korea, where they appear to have little Zinc in their crops
1. Overview Gut and vitamin D contains the following summary
{include}
1. Gut category listing contains the following
{include}
---
1. # From the PDF
< 40 years, 3.7 X more likely to have low Zinc
" patients younger than 40 years were at increased risk for zinc deficiency (RR, 3.683; 95% CI, 1.152 to 11.777; p=0.028) "
Females 4.9 X more likely to have low Selenium
"Female sex (RR, 4.871; 95% CI, 1.352 to 17.544; p=0.015) and low serum albumin levels (<3.3 g/dL; RR, 10.346; 95% CI, 1.035 to 103.447; p=0.047) were independent risk factors for selenium deficiency by multivariate logistic regression analysis"
📄 Download the PDF from VitaminDWiki
BACKGROUND/AIMS:
Studies on the micronutrient status of Asian patients with inflammatory bowel disease (IBD) are scarce. We evaluated the prevalence of micronutrient deficiency and verified the risk factors for micronutrient deficiency in Korean patients with IBD.
METHODS:
We measured the serum levels of 25-hydroxyvitamin D3 [25-(OH)D], zinc, and selenium to analyze the clinical risk factors for micronutrient levels below the reference values. In addition, we compared the 25-(OH)D levels of patients with IBD to those of age- and sex-matched healthy controls.
RESULTS:
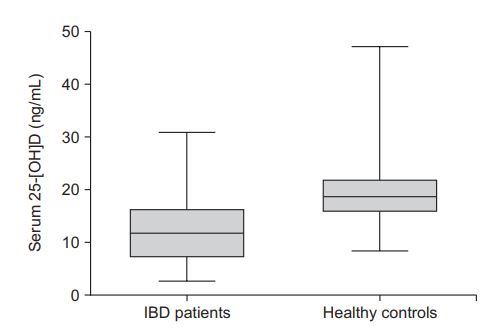
Among the 83 patients, 74 (89.2%) had suboptimal serum 25-(OH)D levels. The mean plasma 25-(OH)D level in patients with IBD was significantly reduced compared to that of the healthy controls (12.3±6.2 ng/mL vs 20.0±6.7 ng/mL; p<0.001).
The proportions of patients with lower serum zinc and selenium levels were 39.0% and 30.9%, respectively. Female sex (p=0.012) and Crohn's disease (p=0.012) were associated with vitamin D deficiency.
Patients younger than 40 years were at increased risk for zinc deficiency (p=0.045).
Female sex (p=0.015) and low serum albumin level (<3.3 g/dL) (p=0.047) were risk factors for selenium deficiency.
CONCLUSIONS:
Many Korean patients with IBD have vitamin D, zinc, and selenium deficiencies, suggesting the necessity for monitoring levels of these micronutrients.
PMID: 28208007 PMCID: PMC5417778 DOI: 10.5009/gnl16333
