Helicobacter pylori associated with low Vitamin D, treated much better if high Vitamin D
Helicobacter pylori treatment success improved 1.2X when activated Vitamin D was added – RCT Sept 2021
Influence of adding vitamin D3 to standard clarithromycin-based triple therapy on the eradication rates of Helicobacter pylori infection
Arab J Gastroenterol . 2021 Sep 11;S1687-1979(21)00066-6. doi: 10.1016/j.ajg.2021.08.002
Mohamed S El Shahawy 1, Zakarya M Shady 2, Abdullah Gaafar 3
Background and study aims: The successful eradication rates with standard clarithromycin-based triple therapy are declining concerning the high antibiotic resistance rate and adverse drug reactions. This study aims to evaluate the effect of adding 1,25-hydroxyvitamin D3 on the eradication rates of the standard clarithromycin-based triple therapy for Helicobacter pylori infection.
Patients and methods: This is a randomized prospective comparative study of 150 patients diagnosed with H. pylori gastritis using magnifying narrow-band imaging endoscopy and supported by a stool antigen test. Patients were divided into two groups: group A (n = 75) treated with amoxicillin, clarithromycin, and esomeprazole for 2 weeks; group B (n = 75) treated with 1,25-hydroxyvitamin D3 for 1 month plus amoxicillin, clarithromycin, and esomeprazole for 2 weeks. The H. pylori eradication rates were assessed using stool antigen test conducted 4 weeks after the end of therapy. Furthermore, the H. pylori eradication rates were assessed with per-protocol (PP) and intention-to-treat (ITT) analyses.
Results: The current results showed that H. pylori eradication was achieved in 46 of 62 (74.19%) and 46 of 75 (61.33%) patients via PP and ITT analyses, respectively, in group A. However, eradication was achieved in 60 of 68 (88.23%) and 60 of 75 (80%) patients via PP and ITT analyses, respectively, in group B. Therefore, the H. pylori eradication rates in the group where vitamin D3 was added to the clarithromycin-based triple therapy were significantly higher than in the other groups (p = 0.012 and p = 0.029 in ITT and PP analyses, respectively).
Conclusions: Adding vitamin D3 to the standard clarithromycin-based triple therapy could provide an additional advantage to achieve significantly higher eradication rates for H. pylori infection.
People with lLow Vitamin D associated 11X less likely to eradicate Helicobacter pylori - meta-analysis Aug 2019
**Effect of vitamin D on Helicobacter pylori infection and eradication: A meta‐analysis
Liping Yang Xinjue He Lan Li Chao Lu
First published: 14 August 2019 https://doi.org/10.1111/hel.12655
Background
Various studies reported the relationship between Helicobacter pylori (H pylori) and vitamin D, but there is some controversy around that. This study aimed to conduct a meta‐analysis to clarify the relationship between vitamin D and H pylori infection, and vitamin D and H pylori eradication.
Methods
Articles published until June 1, 2019, in the PubMed, MEDLINE, and EMBASE databases with English‐language medical studies were searched. According to the inclusion criteria, relevant statistical data were extracted to Microsoft Excel and analyzed by STATA15.1.
Results
Ten articles were finally included. It was demonstrated that average 25(OH)D level in H pylori‐positive patients was lower than H pylori‐negative (SMD = −0.53 ng/mL, 95% CI = (−0.91, −0.16 ng/mL)). For H pylori eradication individuals, the result showed that average 25(OH)D level in H pylori successful eradication individuals was higher than unsuccessful (SMD = 1.31 ng/mL, 95% CI = [0.60, 2.02 ng/mL]).
In addition, individuals with vitamin D deficiency had lower H pylori eradicate rate (* OR = 0.09 *, 95% CI = [0.02, 0.41]).
Sensitivity analysis showed that the meta‐analysis results were stable and reliable.
Conclusions
Vitamin D was a protective factor to H pylori infection. Moreover, vitamin D can improve the success rate of H pylori eradication.
The effect of vitamin D deficiency on eradication rates of Helicobacter pylori infection - Dec 2018* Successful if high Vitamin D *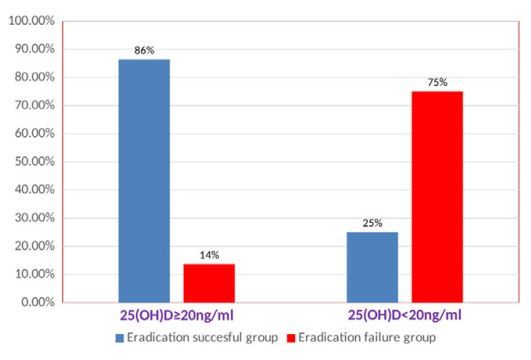
JGH Open. 2018 Aug 2;2(6):270-275. doi: 10.1002/jgh3.12081. eCollection 2018 Dec.
El Shahawy MS1, Hemida MH2, El Metwaly I3, Shady ZM1.
BACKGROUND/AIM:
Many studies have investigated risk factors other than antibiotic resistance linked to Helicobacter pylori (H. pylori) eradication failure. The aim of this study was to study the effect of serum levels of 25-hydroxy-vitamin D (25[OH]D) on eradication rates of H. pylori infection.
METHODS:
This study included 150 patients diagnosed with H. pylori gastritis using magnifying narrow-band imaging endoscopy supported by stool antigen test. Serum 25-OH vitamin D levels were measured via the Enzyme-Linked Immune Sorbent assay (ELISA) method before starting eradication therapy of H. pylori infection. All patients were treated with clarithromycin-based triple therapy for 14 days. H. pylori eradication was determined via a stool antigen test performed 4 weeks after the end of therapy. According to the serum level of 25-OH vitamin D levels, the patients were divided into two groups: group I (sufficient) had a vitamin D level of ≥20 ng/mL, while group II (deficient) had a vitamin D level of <20 ng/mL.
RESULTS:
Our results revealed that eradication was successful in 105 (70%) patients and failed in 45 (30%) patients. The mean 25[OH]D level was significantly lower in the eradication failure group compared to the successful treatment group (14.7 ± 4.5 vs 27.41 ± 7.1; P < 0.001).
Furthermore, there were significantly more patients with deficient 25[OH]D levels in the failed treatment group, 30 (* 66.6% ), compared to the successful group, 10 ( 9.5% *) (P < 0.001).
CONCLUSIONS:
Our results demonstrated that 25-OH vitamin D deficiency may be considered a risk factor related to eradication failure of H. pylori infection. In addition, a further randomized trial to evaluate the effect of vitamin D supplementation in H. pylori eradication is mandatory.{FONT(size="16")}* 📄 Download the PDF from VitaminDWiki *{FONT}
The influence of vitamin D deficiency on eradication rates of Helicobacter pylori - 2017
Adv Clin Exp Med. 2017 Dec;26(9):1377-1381. doi: 10.17219/acem/65430.
Yildirim O1, Yildirim T2, Seckin Y1, Osanmaz P3, Bilgic Y1, Mete R4.
1 Department of Gastroenterology, Faculty of Medicine, Inonu University, Malatya, Turkey.
2 Dept of Physiotherapy and Rehabilitation, Faculty of Medicine, Inonu University, Malatya, Turkey.
3 Department of Internal Medicine, Faculty of Medicine, Namik Kemal University, Tekirdag, Turkey.
4 Department of Gastroenterology, Faculty of Medicine, Namik Kemal University, Tekirdag, Turkey.
{BOX(title=>VitaminDWiki class="border" bg=>#FF9,width= "700px")}* Eradicated: 19 ng of vitamin D
NOT eradicated: 9 ng of vitamin D *---
Helicobacter pylori infection and low vitamin D – many studies
Number of people to treat to prevent 1 case of flu: Vitamin D 4, Vaccination 40 – Feb 2017
8 times less bacteria in blood of HIV patients if Vitamin D levels greater than 30 ng – April 2016
Vitamin D improves a child’s immune system – can now be claimed in Europe – Sept 2016
Inflammatory diseases: review of vitamin D, with many tables – May 2014
Helicobacter pylori infection protection by the body’s increasing Vitamin D receptors – Nov 2013
---* See also PubMed ** Relationship of vitamin D receptor gene polymorphisms in Helicobacter pylori gastric patients Jan 2018 Free PDF online
- The Associations Between Helicobacter pylori Infection, Serum Vitamin D, and Metabolic Syndrome: A Community-Based Study May 2016 Free PDF online
{BOX}
{FONT(size="18")}* 📄 Download the PDF from VitaminDWiki *{FONT}
BACKGROUND:
Helicobacter pylori eradication therapy improves the healing of various gastro-duodenal diseases such as chronic gastritis and peptic ulcer, and also reduces gastric cancer incidence. Several studies have reported on risk factors other than antibiotic resistance related to Helicobacter pylori eradication failure.
OBJECTIVES:
In this study, we aimed to investigate whether or not the serum levels of 25-hydroxy-vitamin D (25(OH)D) influence eradication rates of H.pylori.
MATERIAL AND METHODS:
220 patients diagnosed with H.pylori gastritis using endoscopic biopsy had their 25-OH vitamin D levels measured via the electrochemiluminescence method before beginning eradication therapy of H.pylori. Gastric biopsies obtained at endoscopy were examined for H.pylori strains and histopathologic findings. All patients were treated with bismuth-containing quadruple therapy for 14 days. H.pylori eradication was determined via the 14C-urea breath test performed 4 weeks after the end of therapy. Based on the 25-OH vitamin D levels, the patients were divided into 2 groups: group 1 (deficient) had a vitamin D level of <10 ng/mL, while group 2 (sufficient) had a vitamin D level of ≥10 ng/ mL.
RESULTS:
Eradication was successful in 170 (77.2%) patients and failed in 50 (22.7%) patients. The prevalence of 25(OH)D deficiency was 30.5%. Mean 25(OH)D levels were significantly lower in the eradication failure group compared to the successful treatment group (9.13 ±4.7 vs 19.03 ±8.13; p = 0.001). There were significantly more patients with deficient 25(OH)D levels in the failed treatment group compared to the successful treatment group (p = 0.001).
CONCLUSIONS:
Our findings suggest that 25-OH vitamin D deficiency may be considered a risk factor related to eradication failure of H.pylori, which may lead to a need for supplementation of vitamin D before eradication of H.pylori.
Helicobacter pylori infection 3X higher risk if less than 20 of Vitamin D – Sept 2018* Vitamin D deficiency and risk of Helicobacter pylori infection in older adults: a cross-sectional study. *Aging Clin Exp Res. 2018 Sep 28. doi: 10.1007/s40520-018-1039-1. [Epub ahead of print]
Mut Surmeli D1, Surmeli ZG2, Bahsi R3, Turgut T3, Selvi Oztorun H3, Atmis V4, Varli M3, Aras S3.
1 Department of Geriatrics, Ibni-i Sina Hospital, Ankara University School of Medicine, 06230, Ankara, Turkey. denizmut19@yahoo.com.
2 Department of Medical Oncology, Ankara Medical Park Hospital, 06680, Ankara, Turkey.
3 Department of Geriatrics, Ibni-i Sina Hospital, Ankara University School of Medicine, 06230, Ankara, Turkey.
4 Department of Geriatrics, Bursa Sevket Yilmaz Training and Research Hospital, 16310, Bursa, Turkey.
BACKGROUND:
Vitamin D deficiency is known to cause increased predisposition to various infectious diseases and the addition of vitamin D to antimicrobial treatment may improve treatment responses. However, the relationship between vitamin D and Helicobacter pylori (H. pylori) remains to be determined.
AIMS: To assess the association between vitamin D deficiency and H. pylori infection.
METHODS:
This cross-sectional study included patients aged 65 and over, who underwent gastroscopy and had gastric biopsy performed between 2010 and 2017. Of the 441 patients, 254 had available 25-hydroxyvitamin D level results and were included in the analyses. Patients were categorized into H. pylori (+) and H. pylori (-) groups, according to histopathological examination results of gastric biopsies. Serum 25(OH) vitamin D levels less than 20 ng/mL were defined as vitamin D deficiency.
RESULTS:
Of all patients, 43 were H. pylori (+) and 211 were H. pylori (-). More patients had vitamin D deficiency (< 20 ng/mL) in the H. pylori (+) group than the H. pylori (-) group (86% vs 67.3%, p = 0.014). The proportion of H. pylori (+) patients decreased across increasing quartiles of 25(OH) vitamin D levels (p for trend = 0.010). In multivariable logistic regression analysis, vitamin D deficiency was associated with increased odds of H. pylori infection after adjustment for age, gender, and Charlson Comorbidity Index (* OR = 3.02 *, 95% CI 1.19-7.69, p = 0.020).
CONCLUSION:
Vitamin D deficiency can be associated with increased risk of H. pylori infection. The potential protective effect of vitamin D against H. pylori infection and its possible role in the treatment of H. pylori should be evaluated in prospective trials.
Metabolic Syndrome 2.1X more likely if both Helicobacter pylori Infection and <20 ng of Vitamin D – May 2016* The Associations Between Helicobacter pylori Infection, Serum Vitamin D, and Metabolic Syndrome: A Community-Based Study. *Medicine (Baltimore). 2016 May;95(18):e3616. doi: 10.1097/MD.0000000000003616.
Chen LW1, Chien CY, Hsieh CW, Chang LC, Huang MH, Huang WY, Kuo SF, Chien CH, Lin CL, Chien RN.
The associations between Helicobacter pylori infection, serum vitamin D level, and metabolic syndrome (MS) are controversial. The present community-based study aimed to investigate the effect of H pylori infection and serum vitamin D deficiency on MS development.Individuals from the northeastern region of Taiwan were enrolled in a community-based study from March, 2014 to August, 2015. All participants completed a demographic survey and underwent the urea breath test (UBT) to detect H pylori infection as well as blood tests to determine levels of vitamin D, adiponectin, leptin, and high-sensitivity C-reactive protein. The ATP III criteria for MS were used in this study. A total of 792 men and 1321 women were enrolled. The mean age was 56.4 ± 13.0 years. After adjusting for age and sex, the estimated odds of MS development for a UBT-positive subject were 1.503 (95% confidence interval [CI]: 1.206-1.872, P < 0.001) when compared to a UBT-negative subject.
For participants with vitamin D deficiency (<20 ng/mL), the odds of MS development were 1.423 (95% CI: 1.029-1.967, P = 0.033) when compared to those with sufficient vitamin D level (>30 ng/mL).
For participants with both H pylori infection and vitamin D deficiency, the odds of MS development were* 2.140 *(95% CI: 1.348-3.398, P = 0.001) when compared to subjects without H pylori infection and with sufficient vitamin D levels.H pylori infection and vitamin D deficiency could be predictors of MS.
For individuals with both H pylori infection and vitamin D deficiency, the odds of MS development were 2.140 when compared to individuals without H pylori infection and with sufficient vitamin D levels.
{BOX(title=>VitaminDWiki class="border" bg=>#FFFAE2,width= "700px")}* Items in both categories Metabolic Syndrome and Immunity are listed here: *{category}
{BOX}
{FONT(size="18")}* 📄 Download the PDF from VitaminDWiki *{FONT}
This page was renamed in Sept 2018. There have actually been** __ visitors to this page since it was originally made
