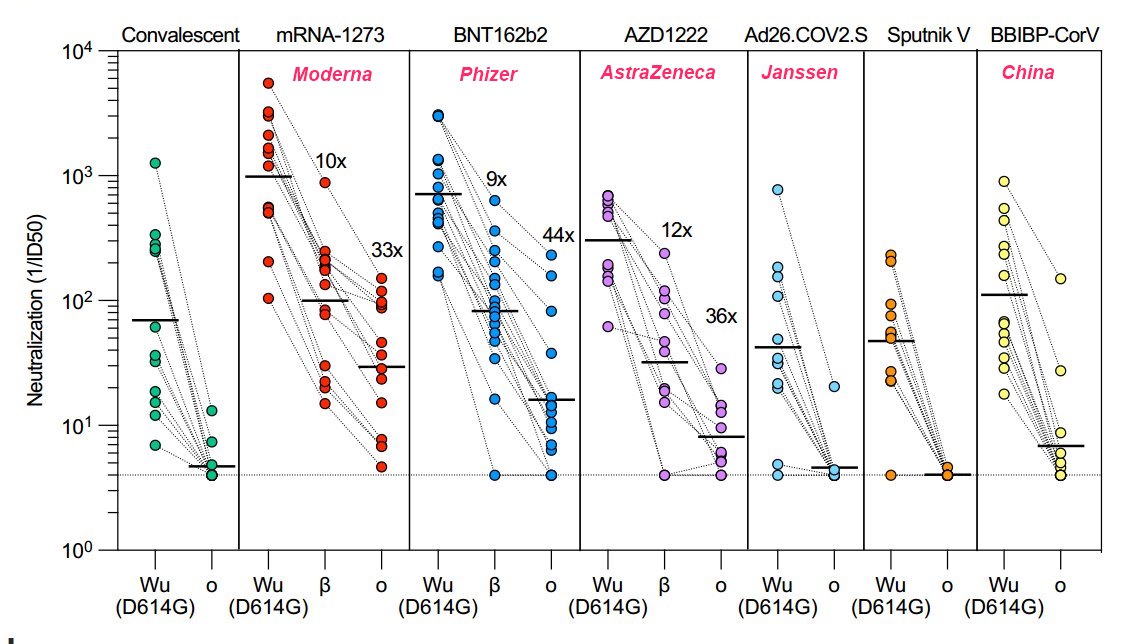
Far fewer vaccination antibodies against Omicron
Broadly neutralizing antibodies overcome SARS-CoV-2 Omicron antigenic shift
Preprint https://doi.org/10.1101/2021.12.12.472269
Elisabetta Cameroni1, Christian Saliba1, John E. Bowen2, Laura E. Rosen3, Katja Culap1, Dora Pinto1, Anna De Marco1, Samantha K. Zepeda2, Julia di Iulio3, Fabrizia Zatta1, Hannah Kaiser3, Julia Noack3, Nisar Farhat3, Nadine Czudnochowski3, Colin Havenar-Daughton3, Kaitlin R. Sprouse2, Josh R. Dillen3, Abigail E. Powell3, Alex Chen3, Cyrus Maher 3, Li Yin3, David Sun3, Leah Soriaga3, Claes Gustafsson4, Nicholas M. Franko5, Jenni Logue5, Najeeha Talat Iqbal6, Ignacio Mazzitelli7, Jorge Geffner7, Renata Grifantini8, Helen Chu5, Andrea Gori9, Agostino Riva10, Olivier Giannini11,12, Alessandro Ceschi11,13,14,15, Paolo Ferrari11,16,17, Alessandra Franzetti-Pellanda18, Christian Garzoni19, Christy Hebner3, Lisa A. Purcell3, Luca Piccoli1, Matteo Samuele Pizzuto1, Alexandra C. Walls2,20, Amalio Telenti2, Herbert W. Virgin3,21,22,23, Antonio Lanzavecchia1,8,23, David Veesler2,20,23, Gyorgy Snell3,23, Davide Corti1,23
1Humabs Biomed SA, a subsidiary of Vir Biotechnology, 6500 Bellinzona, Switzerland
2Department of Biochemistry, University of Washington, Seattle, WA 98195, USA
3Vir Biotechnology, San Francisco, California 94158, USA
4ATUM, Newark, California 94560, USA
5Division of Allergy and Infectious Diseases, University of Washington, Seattle, WA 98195, USA.
6Department of Paediatrics and Child Health, Aga Khan University, Karachi, 74800, Pakistan
7Instituto de Investigaciones Biomédicas en Retrovirus y SIDA (INBIRS), Facultad de Medicina, Buenos Aires
C1121ABG, Argentina
8National Institute of Molecular Genetics, Milano, Italy
9Infectious Disease Unit, Fondazione IRCCS Ca’ Granda, Ospedale Maggiore Policlinico, Milan, Italy 10Department of Biomedical and Clinical Sciences 'L.Sacco' (DIBIC), Università di Milano, Milan, Italy "Faculty of Biomedical Sciences, Università della Svizzera italiana, Lugano, Switzerland "
11Department of Medicine, Ente Ospedaliero Cantonale, Bellinzona, Switzerland 13Clinical Trial Unit, Ente Ospedaliero Cantonale, Lugano, Switzerland
12Division of Clinical Pharmacology and Toxicology, Institute of Pharmacological Science of Southern Switzerland, Ente Ospedaliero Cantonale, Lugano, Switzerland
13Department of Clinical Pharmacology and Toxicology, University Hospital Zurich, Zurich, Switzerland
"Division of Nephrology, Ente Ospedaliero Cantonale, Lugano, Switzerland
"Clinical School, University of New South Wales, Sydney, Australia
18Clinical Research Unit, Clinica Luganese Moncucco, 6900 Lugano, Switzerland.
19Clinic of Internal Medicine and Infectious Diseases, Clinica Luganese Moncucco, 6900 Lugano, Switzerland. 20Howard Hughes Medical Institute, Seattle, WA 98195, USA.
21Department of Pathology and Immunology, Washington University School of Medicine, Saint Louis MO 63110
22Department of Internal Medicine, UT Southwestern Medical Center, Dallas TX 75390
23These authors contributed equally: Herbert W. Virgin, Antonio Lanzavecchia, David Veesler, Gyorgy Snell and Davide Corti
- These authors contributed equally Correspondence: dcorti@vir.bio. dveesler@uw.edu
The recently emerged SARS-CoV-2 Omicron variant harbors 37 amino acid substitutions in the spike (S) protein, 15 of which are in the receptor-binding domain (RBD), thereby raising concerns about the effectiveness of available vaccines and antibody therapeutics. Here, we show that the Omicron RBD binds to human ACE2 with enhanced affinity relative to the Wuhan-Hu-1 RBD and acquires binding to mouse ACE2. Severe reductions of plasma neutralizing activity were observed against Omicron compared to the ancestral pseudovirus for vaccinated and convalescent individuals. Most (26 out of 29) receptor-binding motif (RBM)-directed monoclonal antibodies (mAbs) lost in vitro neutralizing activity against Omicron, with only three mAbs, including the ACE2-mimicking S2K146 mAb1, retaining unaltered potency. Furthermore, a fraction of broadly neutralizing sarbecovirus mAbs recognizing antigenic sites outside the RBM, including sotrovimab2, S2X2593 and S2H974, neutralized Omicron. The magnitude of Omicron-mediated immune evasion and the acquisition of binding to mouse ACE2 mark a major SARS-CoV-2 mutational shift. Broadly neutralizing sarbecovirus mAbs recognizing epitopes conserved among SARS-CoV-2 variants and other sarbecoviruses may prove key to controlling the ongoing pandemic and future zoonotic spillovers.
📄 Download the PDF from VitaminDWiki
COVID-19 treated by Vitamin D - studies, reports, videos
{include}

- The above image is automatically updated
VItamin D appears to fight all variants of a wide number of viruses
How healthy innate immune systems adapt to viral mutations - Feb 2021
Strong innate immune systems do not get viral symptoms (COVID-19) – April 2021
A virus can mutate to avoid a vaccine, need more than vaccines to fight a virus – July 31, 2021
Omicron may require fourth vaccine dose, Pfizer says - Dec 10, 2021
VitaminDWiki pages with OMICRON in title
This list is automatically updated
{LIST()}
