Postoperative problems are reduced if sufficient Vitamin D (Bunion in this case)
Association of Vitamin D Deficiency With Adverse Postoperative Outcomes Following Hallux Valgus Correction
Foot Ankle Orthop. 2026 Mar 11;11(1):24730114261422228. doi: 10.1177/24730114261422228
Eve R Glenn 1, David Ryu 1, Eric Mao 1, Daniel Badin 1, Nigel Hsu 1, John M Thompson 1, Amiethab Aiyer 1
Background: Hallux valgus (HV) is a common forefoot deformity treated surgically. Vitamin D is essential for bone and soft tissue health, but its role in postoperative outcomes after HV is unclear. This study evaluated whether low preoperative vitamin D is associated with increased complications.
Methods: Adults undergoing HV correction were analyzed retrospectively using the TriNetX Research Network. Patients were categorized as vitamin D deficient (≤20 ng/mL), subsufficient (≤30 ng/mL), or sufficient (≥30 ng/mL). Secondary analyses examined outcomes by surgical setting (inpatient vs ambulatory) and procedure type among subsufficient patients. Propensity score matching controlled for demographics and comorbidities. Ninety-day outcomes included wound complications, health care visits, opioid use, and thromboembolic events. Significance was set at P <.05.
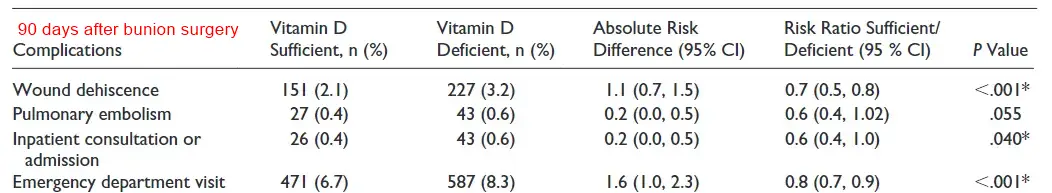
Results: After matching, 7041 deficient and 8150 subsufficient patients were compared with equal numbers of sufficient controls. Vitamin D deficiency and subsufficiency were associated with higher rates of wound dehiscence, postoperative infection, inpatient consultation/admission, emergency department (ED) visits, and opioid use (all P < .05). In secondary analyses, 1286 inpatient and 6346 ambulatory subsufficient and sufficient patients were matched. Vitamin D subsufficiency was associated with higher ED visits in inpatients and increased wound dehiscence, inpatient encounters, ED visits, and opioid use in ambulatory patients (all P < .05). Among 3600 vitamin D-subsufficient patients per cohort, metatarsophalangeal (MTP) fusion had higher wound dehiscence than HV correction (P = .033).
Conclusion: Low preoperative vitamin D is associated with increased postoperative complications after HV, including wound dehiscence, infection, health care utilization, and opioid use. Subsufficient vitamin D was linked to higher ED visits in inpatients and increased wound dehiscence, inpatient encounters, ED visits, and opioid use in ambulatory patients. Among subsufficient patients, MTP fusion had higher wound dehiscence than HV correction, likely due to greater soft tissue disruption. These findings highlight that both vitamin D status and procedure type are associated with postoperative complications; however, given the modest absolute risk differences, preoperative vitamin D screening should be viewed as a possible risk-stratification tool.
Hallux Valgus Correction = bunion correction
Hallux valgus (commonly known as a bunion) is a deformity of the big toe joint where the big toe angles toward the second toe, causing a bony prominence to develop on the inner edge of the foot. "Correction" refers to the surgical or conservative treatments used to address it.
Types of Correction
Conservative (Non-surgical):
- Wider, better-fitting footwear
- Padded shoe inserts / orthotics
- Splints or toe spacers
- Anti-inflammatory medications for pain
- Physical therapy
These don't reverse the deformity but manage symptoms.
Surgical (Hallux Valgus Surgery / Bunionectomy):
There are over 150 described surgical techniques, but the most common include:
- Osteotomy – cutting and realigning the bone (e.g., Chevron, Scarf, or Lapidus procedures)
- Arthrodesis – fusing the joint for severe cases
- Exostectomy – shaving down the bony bump (rarely done alone)
- Minimally invasive / percutaneous surgery – a growing trend using small incisions and specialized tools
Recovery typically takes 6–12 weeks of limited weight-bearing, with full recovery in 3–6 months.
23% of adults need it
- Hallux valgus affects an estimated 23% of adults aged 18–65 and up to 36% of those over 65, making it one of the most common foot deformities worldwide.
- It is significantly more common in women (roughly 2–4x more than men), largely attributed to narrow, pointed, or high-heeled footwear.
- In the United States alone, approximately 150,000–200,000 bunion surgeries are performed each year.
- Globally, it's one of the most frequently performed elective orthopedic foot procedures.
- Not everyone with the condition requires surgery — many manage with conservative care. Surgery is generally recommended when pain significantly interferes with daily activity and conservative measures have failed.
Risk Factors
- Female sex
- Tight or ill-fitting footwear (especially high heels)
- Family history / genetics
- Rheumatoid arthritis or hypermobility
- Flat feet or certain foot shapes
It's a very common quality-of-life issue, particularly among older women, and surgical correction has a high success rate — around 85–90% patient satisfaction in well-selected cases.
Releated in VitaminDWiki
- Hand surgery complications 43% less likely if have good Vitamin D level
- Death after surgery for chronic kidney disease 2.3 X more likely if low Vitamin D
- Vitamin D is needed before many surgeries – many studies and RCTs
- Foot and Ankle Surgeries should benefit from Vitamin D
- Orthopaedic surgeries need Vitamin D – many studies
