Vitamin D reduces chance of a second heart attack and death
Vitamin D and acute myocardial infarction
World J Cardiol. Jan 26, 2017; 9(1): 14-20 doi: 10.4330/WJC.v9.i1.14
Valentina Milazzo giancarlo.marenzi@ccfm.it, Monica De Metrio, Nicola Cosentino, Giancarlo Marenzi, Elena Tremoli, Centro Cardiologico Monzino, I.R.C.C.S., 20138 Milan, Italy
📄 Download the PDF from VitaminDWiki
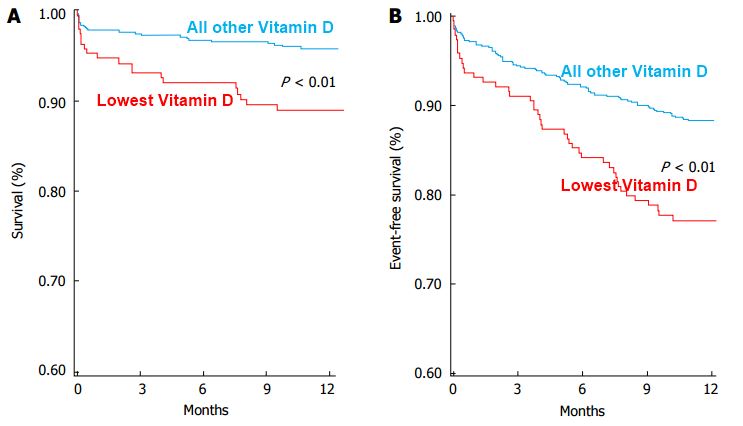
Chart was copied from Acute Coronary Syndrome twice as bad if low vitamin D – May 2015
Low Vitamin D = 9 nanograms
Vitamin D deficiency is a prevalent condition, cutting across all ethnicities and among all age groups, and occurring in about 30%-50% of the population. Besides vitamin D established role in calcium homeostasis, its deficiency is emerging as a new risk factor for coronary artery disease. Notably, clinical investigations have suggested that there is an association between hypovitaminosis D and acute myocardial infarction (AMI). Not only has it been linked to incident AMI, but also to increased morbidity and mortality in this clinical setting.
Moreover, vitamin D deficiency seems to predispose to recurrent adverse cardiovascular events, as it is associated with post-infarction complications and cardiac remodeling in patients with AMI.
Several mechanisms underlying the association between vitamin D and AMI risk can be involved. Despite these observational and mechanistic data, interventional trials with supplementation of vitamin D are controversial. In this review, we will discuss the evidence on the association between vitamin D deficiency and AMI, in terms of prevalence and prognostic impact, and the possible mechanisms mediating it. Further research in this direction is warranted and it is likely to open up new avenues for reducing the risk of AMI.
Core tip : Vitamin D deficiency is a prevalent condition and it is emerging as a new risk factor for coronary artery disease. Notably, hypovitaminosis D has been reported to be common in patients with acute myocardial infarction, and preliminary studies indicate a possible association with short-term and long-term morbidity and mortality. Although these observational initial proofs, interventional trials with supplementation of vitamin D have yielded controversial results. We herein discuss the current evidence suggesting an association between acute myocardial infarction and vitamin D deficiency, in terms of prevalence and prognostic impact, and the possible underlying mechanisms.
