Strong association of non alcoholic fatty liver disease and low vitamin D
Highlights of this page
- Strong association between them, but perhaps NAFLD ==> low serum level of vitamin D
- Due to the liver not functioning as well when it is fatty
Most patients with NAFLD have few or no symptoms
NAFLD assocatied with obesity, unhealthy dietary pattern, and sedentary lifestyle.
40% of all seniors have NAFLD
See also VitaminDWiki
NAFLD associated with low vitamin D (in children too) – meta-analysis Aug 2019
NAFLD is treated by Vitamin D, Omega-3, Curcumin, Silymarinm, etc. Aug 2018
Non-Alcoholic Fatty Liver Disease treated by Omega-3 – three meta-analysis 2016-2017
More fat in liver associated with lower vitamin D – June 2016
NAFLD in children nicely treated by combination of Vitamin D and Omega-3 – RCT Dec 2016
Liver cancer half as likely if high level of vitamin D – Feb 2014 Recall that NAFLD can lead to Liver cancer
Getting Vitamin D into your blood and cells discusses Calcidiol for people with poor livers
Non-alcoholic Fatty Liver Disease (4 in 10 seniors) and Vitamin D
Non-alcoholic fatty liver disease associated with much lower vitamin D – Aug 2014
Vitamin C reduces liver inflammation, which improves vitamin D production – Dec 2014
Half of obese children had fatty liver and low vitamin D – March 2014
Non-alcoholic fatty liver disease associated with low vitamin D – independent of BMI – June 2014
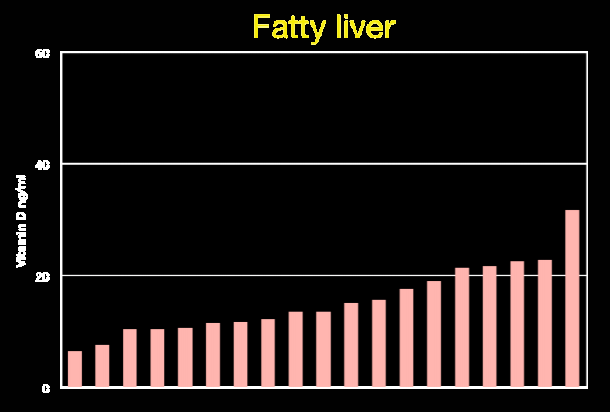
Graphs of diseases vs vitamin D levels - April 2011 All but one person had < 22 ng of vitamin D
NAFLD (MAFLD) and Vitamin D - Oct 2020
Vitamin D and Metabolic Dysfunction-Associated Fatty Liver Disease (MAFLD): An Update
by Ilaria Barchetta,Flavia Agata Cimini andMaria Gisella Cavallo
Department of Experimental Medicine, Sapienza University, Viale Regina Elena 321, 00161 Rome, Italy
Nutrients 2020, 12(11), 3302; https://doi.org/10.3390/nu12113302
📄 Download the PDF from VitaminDWiki
Significant effect if use enough or the right kind
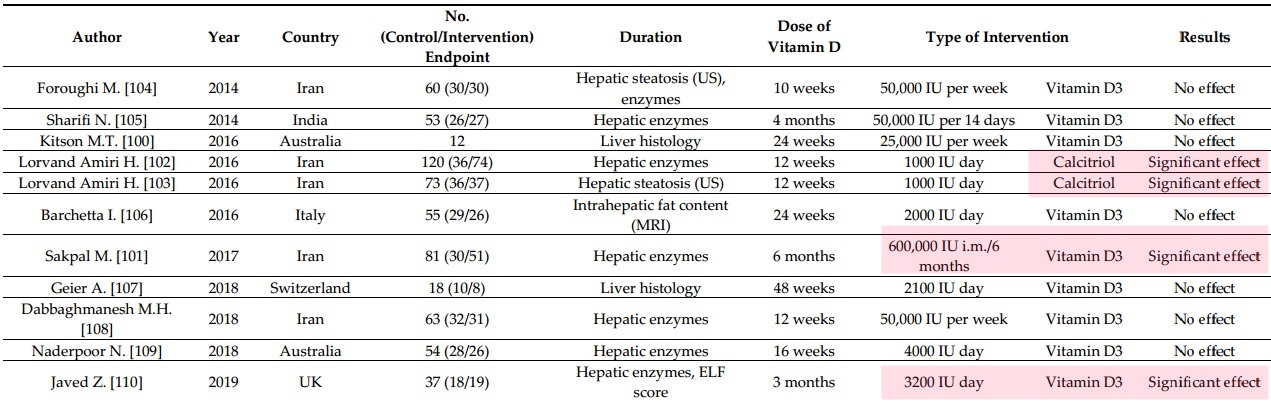
Vitamin D: A new player in non-alcoholic fatty liver disease? - Feb 2015
World J Gastroenterol. 2015 Feb 14;21(6):1718-1727.
Eliades M1, Spyrou E1.

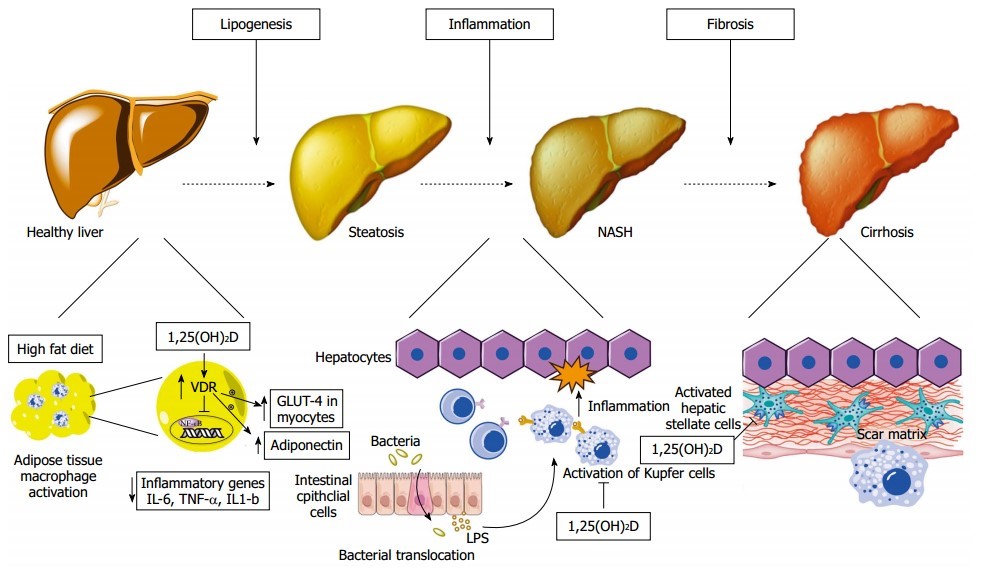
Vitamin D through its active form 1a-25-dihydroxyvtamin D [1,25(OH)2D] is a secosteroid hormone that plays a key role in mineral metabolism. Recent years have witnessed a significant scientific interest on vitamin D and expanded its actions to include immune modulation, cell differentiation and proliferation and inflammation regulation. As our understanding of the many functions of vitamin D has grown, the presence of vitamin D deficiency has become one of the most prevalent micronutrient deficiencies worldwide. Concomitantly, non-alcoholic fatty liver disease (NAFLD) has become the most common form of chronic liver disease in western countries. NAFLD and vitamin D deficiency often coexist and epidemiologic evidence has shown that both of these conditions share several cardiometabolic risk factors. In this article we provide an overview of the epidemiology and pathophysiology linking NAFLD and vitamin D deficiency, as well as the available evidence on the clinical utility of vitamin D supplementation in NAFLD.
PMID: 25684936 📄 Download the PDF from VitaminDWiki.
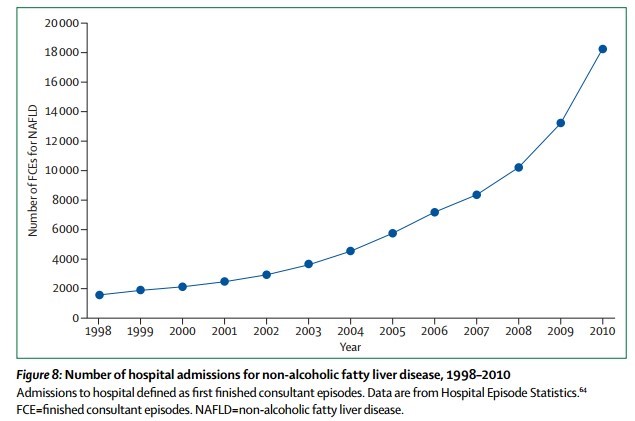
Large recent increases in NAFLD - 2014
📄 Download Lancet nov 2014 PDF from VitaminDWiki.
8X increase in a decade
Nonalcoholic Fatty Liver Disease: America’s Greatest Health Risk of 2015? Scientific American
- Today, up to 25 % of people in the U.S. are living with NAFLD
Fatty livers (determined by ultasound, not enzymes) had lower levels of vitamin D - Aug 2014
Serum vitamin D is associated with non-alcoholic fatty liver disease in Chinese males with normal weight and liver enzymes
Acta Pharmacologica Sinica , (4 August 2014) | doi:10.1038/aps.2014.48
Ya-ping Hao, Xiao-jing Ma, Yu-qi Luo, Jie Ni, Jian-xin Dou, Ya-qin Hu, Jia-an Zhu, Yu-qian Bao and Wei-ping Jia
Aim: Considering the characterization of vitamin D deficiency as a risk factor of ectopic fat deposition, the association of serum 25-hydroxy vitamin D3 [25(OH)D3] levels with non-alcoholic fatty liver disease (NAFLD) was evaluated in Chinese men with normal body mass index (BMI) and enzyme markers of liver function.
Methods: A total of 514 participants (22 to 79 years old) with normal BMI and liver enzymes were identified for analysis. Abdominal ultrasound was performed to diagnose NAFLD , and the fatty liver index (FLI) was calculated to quantify liver steatosis. Serum 25(OH)D3 levels were determined by an electrochemiluminescence immunoassay.
Results: Among the entire study population, the mean levels of serum 25(OH)D3 were 15.32±5.77 ng/mL. However, when serum 25(OH)D3 levels were compared between non-NAFLD subjects (n=438) and NAFLD subjects (n=76), the latter showed significantly lower levels ( 15.65 ±5.89 ng/mL vs 13.46 ±4.65 ng/mL, P=0.002). In addition, serum 25(OH)D3 levels were found to be significantly correlated with FLI after adjustment for age and BMI (r=−0.108, P=0.014). Logistic regression showed that serum 25(OH)D3 levels were independently correlated with NAFLD (OR: 0.937, 95% CI: 0.884–0.993, P=0.028). Furthermore, stepwise regression analysis revealed that serum 25(OH)D3 levels were inversely associated with FLI (β=−0.055, P=0.040).
Conclusion: The present study demonstrated that serum 25(OH)D3 levels were inversely associated with NAFLD, even in subjects with normal total body fat, suggesting a potential role of lower levels of vitamin D in the occurrence and development of NAFLD.
Non-alcoholic fatty liver disease 2.5X more likely (Dec 2013)
2.4X more likely if vitamin D in range of 15 to 30 ng
2.5X more likely if vitamin D <15 ng
Low 25-hydroxyvitamin D level is independently associated with non-alcoholic fatty liver disease.
Nutr Metab Cardiovasc Dis. 2013 Feb 13. pii: S0939-4753(12)00286-4. doi: 10.1016/j.numecd.2012.12.006.
Jablonski KL, Jovanovich A, Holmen J, Targher G, McFann K, Kendrick J, Chonchol M.
Division of Renal Diseases and Hypertension, University of Colorado Denver, Anschutz Medical Center, Aurora, CO 80045, USA. Electronic address: kristen.nowak@ucdenver.edu.
BACKGROUND AND AIMS: We sought to explore associations between serum 25-hydroxyvitamin D [25(OH)D] levels and non-alcoholic fatty liver disease [NAFLD] in an integrated healthcare delivery system in the U.S.
METHODS AND RESULTS: Six hundred and seven NAFLD cases were randomly matched 1:1 with controls for age, sex, race and season of measurement. Conditional logistic regression was used to evaluate if serum 25(OH)D levels were associated with increased odds of NAFLD (diagnosed by ultrasound) after adjusting for body mass index and history of diabetes, renal, peripheral vascular and liver diseases (model 1) and also for hypertension (model 2). Mean (SD) serum 25(OH)D level was significantly lower in the group with NAFLD as compared with that in the matched control group (75±17 vs. 85±20nmol/L [30±7 vs. 34±8ng/mL], P<0.001).
Inadequate 25(OH)D status progressively increased the odds of NAFLD when classified categorically as sufficient (25(OH)D 75nmol/L >30ng/mL, reference group), insufficient (37-75nmol/L 15-30ng/mL; adjusted odds ratio [OR]: 2.40, 95% confidence interval [CI]: 0.90-6.34) or deficient (<37nmol/L [<15ng/mL](<15ng/mL); adjusted OR: 2.56 , 95% CI: 1.27-5.19).
When modeled as a continuous variable, increased log(10) 25(OH)D was inversely associated with the risk of prevalent NAFLD (adjusted OR: 0.25, 95% CI: 0.064-0.96, P=0.02).
CONCLUSION: Compared with matched controls, patients with NAFLD have significantly decreased serum 25(OH)D levels, suggesting that low 25(OH)D status might play a role in the development and progression of NAFLD.
Fatty liver disease in 16 percent of teens, most of whom had low vitamin D levels – Feb 2014
Low serum 25-hydroxyvitamin D concentrations are associated with non-alcoholic fatty liver disease in adolescents independent of adiposity
Journal of Gastroenterology and Hepatology, DOI: 10.1111/jgh.12541
Lucinda J. Black 1, Peter Jacoby 1, Wendy Chan She Ping-Delfos 2, Trevor A. Mori 2, Lawrence J. Beilin2, John K. Olynyk2,3,4,5, Oyekoya T. Ayonrinde2,3,4, Rae Chi Huang1,2, Patrick G. Holt1,6, Prue H. Hart1, Wendy H. Oddy1,†, Leon A. Adams2,7,†,*
Background and aims
Non-alcoholic fatty liver disease (NAFLD) and serum 25-hydroxyvitamin D (s25(OH)D) concentrations are both associated with adiposity and insulin resistance (IR) and thus may be pathogenically linked. We aimed to determine the prevalence of vitamin D deficiency in adolescents with NAFLD and to investigate the longitudinal and cross-sectional associations between s25(OH)D concentrations and NAFLD.
Methods
Participants in the population-based West Australian Pregnancy (Raine) Cohort had seasonally-adjusted s25(OH)D concentrations determined at ages 14 and then 17 years. NAFLD was diagnosed at 17 years using liver ultrasonography. Associations were examined after adjusting for potential confounders. Odds ratios (OR) and confidence intervals (CI) are reported per standard deviation in s25(OH)D concentrations.
Results
NAFLD was present in 16% (156/994) of adolescents.
The majority of participants with NAFLD had either
insufficient (51%) or
deficient (17%) vitamin D status.
Lower s25(OH)D concentrations at 17 years were significantly associated with increased risk of NAFLD (OR 0.74, 95%CI 0.56,0.97; p=0.029), after adjusting for sex, race, physical activity, television/computer viewing, body mass index and IR. The effect of s25(OH)D concentrations at 17 years was minimally affected after further adjusting for s25(OH)D concentrations at 14 years (OR 0.76, 95%CI 0.56,1.03; p=0.072).
Conclusions
Lower s25(OH)D concentrations are significantly associated with NAFLD, independent of adiposity and IR. Screening for vitamin D deficiency in adolescents at risk of NAFLD is appropriate, and clinical trials investigating the effect of vitamin D supplementation in the prevention and treatment of NAFLD may be warranted.
Note by VitaminDWiki:Insufficient level of Vitamin D is not defined in the abstract. It may be <20 ng or might be <30 ng
Several PubMed papers
- Patients with Nonalcoholic Fatty Liver Disease Have a Low Response Rate to Vitamin D Supplementation Aug 2017
- "Daily supplementation with 2000 IU cholecalciferol for 6 mo did not correct hypovitaminosis D in the majority of patients with NASH"
- Publisher wants $25 to access all of their publications
- VitaminD Council review of the study
- " 26 individuals were considered nonresponders and 16 were considered responders."
- "Nonresponders had a greater fat mass and lower fat-free mass scores compared to responders (p < 0.001)."
- "Nonresponders had higher disease severity scores than nonresponders, indicating a greater disease severity (p = 0.02)"
- Comment by VitaminDWiki - people with poor livers (non-responsers) probably need Calcidiol
- The Association between Vitamin D Insufficiency and Nonalcoholic Fatty Liver Disease: A Population-Based Study No association - July 2017
- Full text online
- Vitamin D and histologic severity of nonalcoholic fatty liver disease: A systematic review and meta-analysis June 2017
- "Despite evidence implicating vitamin D in NAFLD pathogenesis, serum 25-hydroxyvitamin D may not be associated with NAFLD histologic severity"
High serum vitamin D levels reduce the risk for nonalcoholic fatty liver disease in healthy men independent of metabolic syndrome. Endocr J.. Feb 2013 full text online
Why vitamin D status should be checked in patients with nonalcoholic fatty liver disease Mayo Clin Proc, Aug 2012 full text online
- Mascitelli L, Goldstein MR, Grant WB.
D-livering the message: the importance of vitamin D status in chronic liver disease J Hepatol. 2012 Oct full text online
Nutrition and physical activity in NAFLD: an overview of the epidemiological evidence World J Gastroenterol. 2011 Aug full text online
- The high prevalence of NAFLD is probably due to the contemporary epidemics of obesity, unhealthy dietary pattern, and sedentary lifestyle.
- Nutritional recommendations for patients with non-alcoholic fatty liver diseases World J Gastroenterol. 2011 Aug full text online
- Among the dietary constituents, combination of vitamin D, vitamin E, and omega-3 fatty acids shows promise for the treatment of NAFLD.
Non-alcoholic fatty liver disease and mortality among US adults: prospective cohort study BMJ. 2011 Nov full text online
Low vitamin D levels are associated with increased risk for fatty liver disease among non-obese adults. Dec 2013 59% more likely if low vitamin D
-
- doubled over the past 20 years and currently affects nearly 11% of adolescents
See also web
Nonalcoholic Fatty Liver Disease Chris Masterjohn W.A,Price, April 2011, provides excellent understanding of fatty liver
NAFLD by American Liver foundation
- WHO IS LIKELY TO HAVE NAFLD? NAFLD tends to develop in people who are overweight or obese or have diabetes, high cholesterol or high triglycerides.
- Rapid weight loss and poor eating habits also may lead to NAFLD.
- However, some people develop NAFLD even if they do not have any risk factors. NAFLD affects up to 25% of people in the United States.
- SYMPTOMS: NAFLD often has no symptoms.
- When symptoms occur, they may include fatigue, weakness, weight loss, loss of appetite, nausea, abdominal pain, spider-like blood vessels, yellowing of the skin and eyes (jaundice), itching, fluid build up and swelling of the legs (edema) and abdomen (ascites), and mental confusion.
- Wikipedia
- Most patients with NAFLD have few or no symptoms. Patients may complain of fatigue, malaise, and dull right-upper-quadrant abdominal discomfort.
- Mild jaundice may be noticed although this is rare. More commonly NAFLD is diagnosed following abnormal liver function tests during routine blood tests
- Pediatric Nonalcoholic Fatty Liver Disease (NAFLD) was first reported in 1983. It is currently the primary form of liver disease among children
- VitaminDWiki comment: The first report was just about when vitamin D levels started falling.
New 10 year data shows non-alcoholic fatty liver disease will reach epidemic status in the U.S. March 2011
The Epidemiology and Natural History of Non-alcoholic Fatty Liver Disease and Non-alcoholic Steatohepatitis in Adults Medscape 2011, extensive article
Comorbid diseases in nonalcoholic fatty liver diseaseNov 2010
- Diseases associated with NAFLD are ALL also associated with low vitamin D:
- cardiovascular disease, chronic kidney disease, type 2 diabetes, obesity, metabolic syndrome.
-
- In many cases, doctors are not exactly sure what causes fatty liver in people who aren’t alcoholics,
- but it has been associated with high blood cholesterol, obesity, and type 2 diabetes.
- Fatty liver develops when the body creates too much fat or cannot metabolize fat fast enough.
- As a result, the leftover is stored in liver cells where it accumulates to become fatty liver disease.
- Eating a high-fat diet does not directly result in fatty liver.
Note: Most NAFLD associations are also associated with low vitamin D
Strong association between non alcoholic fatty liver disease (NAFLD) and low 25(OH) vitamin D levels in an adult population with normal serum liver enzymes - 2011
**BMC Med. 2011 Jul 12;9(1):85.** Barchetta I, Angelico F, Del Ben M, Baroni MG, Pozzilli P, Morini S, Cavallo MG; gisella.cavallo@uniroma1.it BACKGROUND: Hypovitaminosis D has been recently recognized as a worldwide epidemic. Since vitamin D exerts significant metabolic activities, comprising free fatty acids (FFA) flux regulation from the periphery to the liver, its deficiency may promote fat deposition into the hepatocytes. Aim of our study was to test the hypothesis of a direct association between hypovitaminosis D and the presence of NAFLD in subjects with various degree of insulin-resistance and related metabolic disorders. METHODS: We studied 262 consecutive subjects referred to the Diabetes and Metabolic Diseases clinics for metabolic evaluation. NAFLD (non-alcoholic fatty liver disease) was diagnosed by upper abdomen ultrasonography, metabolic syndrome was identified according to the Third Report of National Cholesterol Education Program/Adult Treatment Panel (NCEP/ATPIII) modified criteria. Insulin-resistance was evaluated by means of HOMA-IR. Fatty-Liver-Index, a recently identified correlate of NAFLD, was also estimated. Serum 25(OH)vitamin D was measured by colorimetric method. RESULTS: Patients with NAFLD (n=162, 61.8%) had reduced serum 25(OH) vitamin D levels compared to subjects without NAFLD ( **14.8** +/- 9.2 vs **20.5** +/- 9.7 ng/ml, p<0.001, **OR 0.95** , IC 95% 0.92-0.98). The relationship between NAFLD and reduced 25(OH)vitamin D levels was independent from age, sex, triglycerides, high density lipoproteins (HDL) and glycaemia (p<0.005) and Fatty Liver Index inversely correlated with low 25(OH) vitamin D regardless sex, age and HOMA-IR (p<0.007). CONCLUSIONS: Low 25(OH)vitamin D levels are associated with the presence of NAFLD independently from metabolic syndrome, diabetes and insulin-resistance profile. PMID: 21749681 PDF is attached at the bottom of this pageVitamin D and NAFLD: Is it more than just an association? (Sept 2013)
Hepatology Vol. 57 Issue 3 Ryan M. Kwok MD1, Dawn M. Torres MD1, Stephen A. Harrison MD2,§,* † Disclaimer The view(s) expressed herein are those of the author(s) and do not reflect the official policy or position of San Antonio Military Medical Center, the U.S. Army Medical Department, the U.S. Army Office of the Surgeon General, the Department of the Army, Department of Defense or the U.S. Government. Vitamin D is a secosteroid with known effects on calcium homeostasis that has recently been shown to have other significant functions regarding immune modulation, cell differentiation and proliferation, and the inflammatory response. As our understanding of the many functions of vitamin D has grown, the presence of vitamin D deficiency (VDD) has become more evident in Western populations. Concomitantly, non-alcoholic fatty liver disease (NAFLD) has become the most common cause of chronic liver disease. NAFLD and VDD are often found together, and while this is not unexpected given their similar associations with obesity and sedentary lifestyle, a growing body of evidence points to a closely linked and potentially causative relationship between VDD and NAFLD. The epidemiologic association between VDD and NAFLD as well as the role of VDD in the pathogenesis of NAFLD and the available evidence on the clinical utility of vitamin D replacement in NAFLD populations will be discussed. (HEPATOLOGY 2013.)Clipped from WikiPedia
Non-alcoholic fatty liver disease (NAFLD) is one cause of a fatty liver, occurring when fat is deposited (steatosis) in the liver not due to excessive alcohol use. It is related to insulin resistance and the metabolic syndrome and may respond to treatments originally developed for other insulin-resistant states (e.g. diabetes mellitus type 2) such as weight loss metformin and thiazolidinediones. Non-alcoholic steatohepatitis (NASH) is the most extreme form of NAFLD this being regarded as a major cause of cirrhosis of the liver of unknown cause.The prevalence of non-alcoholic fatty liver disease ranges from 9 to 36.9% of the population in different parts of the world
Approximately 20% of the United States population suffers from non-alcoholic fatty liver, and the prevalence of this condition is increasing.
Symptoms and associations
Most patients with NAFLD have few or no symptoms.
Patients may complain of fatigue, malaise, and dull right-upper-quadrant abdominal discomfort.
Mild jaundice may be noticed although this is rare.
More commonly NAFLD is diagnosed following abnormal liver function tests during routine blood tests.
By definition, alcohol consumption of over 20 g/day (about 25 ml/day) excludes the condition.
NAFLD is associated with insulin resistance and metabolic syndrome (obesity, combined hyperlipidemia, diabetes mellitus (type II) and high blood pressure).
Hypovitaminosis D is associated with increased whole body fat mass and greater severity of non-alcoholic fatty liver disease - 2013
Liver Int. 2013 Sep 5. doi: 10.1111/liv.12312
Dasarathy J, Periyalwar P, Allampati S, Bhinder V, Hawkins C, Brandt P, Khiyami A, McCullough AJ, Dasarathy S.
Department of Family Medicine, MetroHealth Medical Center, Cleveland, OH, USA.
BACKGROUND & AIMS: Hypovitaminosis D is common in obesity and insulin-resistant states. Increased fat mass in patients with non-alcoholic fatty liver disease (NAFLD) may contribute to hypovitaminosis D. To determine the relation among plasma vitamin D concentration, severity of disease and body composition in NAFLD.
METHODS: Plasma vitamin D concentration was quantified in 148 consecutive biopsy-proven patients with NAFLD (non-alcoholic steatohepatitis - NASH: n = 81; and hepatic steatosis: n = 67) and healthy controls (n = 39). NAFLD was scored using the NASH CRN criteria. Body composition was quantified by bioelectrical impedance analysis and abdominal CT image analysis.
RESULTS: Plasma vitamin D concentration was significantly lower in NAFLD ( 21.2 ± 10.4 ng/ml) compared with healthy controls ( 35.7 ± 6.0 ng/ml).
Higher NAFLD activity scores were associated with lower plasma concentration of vitamin D (r2 = 0.29; P < 0.001).
Subgroup analysis among patients with NAFLD showed that patients with NASH had significantly lower (P < 0.01) vitamin D levels than those with steatosis alone (18.1 ± 8.4 vs. 25.0 ± 11.3 ng/ml). Low concentrations of vitamin D were associated with greater severity of steatosis, hepatocyte ballooning and fibrosis (P < 0.05).On multivariate regression analysis, only severity of hepatocyte ballooning was independently associated (P = 0.02) with low vitamin D concentrations.
Plasma vitamin D (P = 0.004) and insulin concentrations (P = 0.03) were independent predictors of the NAFLD activity score on biopsy.
Patients with NAFLD had higher fat mass that correlated with low vitamin D (r2 = 0.26; P = 0.008).
CONCLUSIONS: Low plasma vitamin D concentration is an independent predictor of the severity of NAFLD.
Further prospective studies demonstrating the impact of vitamin D replacement in NAFLD patients are required.
© 2013 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd. PMID: 24118743
The Silent Epidemic Of Liver Disease - Life Extension April 2015
Increased obestiy ==> Diabetes/Metabolic Syndrome ==>NAFLD
Silymarin found in the milk thistle Prevents And Reverses Liver Disease
Does not mention Vitamin D
📄 Download the PDF from VitaminDWiki
The serum vitamin D level is inversely correlated with nonalcoholic fatty liver disease (25%)- March 2016
Clin Mol Hepatol. 2016 Mar;22(1):146-51. doi: 10.3350/cmh.2016.22.1.146. Epub 2016 Mar 28.
Chung GE1, Kim D1,2, Kwak MS1, Yang JI1, Yim JY1, Lim SH1, Itani M3.
1Department of Internal Medicine, Healthcare Research Institute, Gangnam Healthcare Center, Seoul National University Hospital, Seoul, Korea.
2Division of Gastroenterology and Hepatology, Stanford University School of Medicine, Stanford, California, USA.
3Pulmonary and Critical Care Consultant, Sheikh Khalifa Specialty Hospital, Ras AlKhaimah, UAE.
BACKGROUND/AIMS:
A low vitamin D level has been associated with metabolic syndrome and diabetes. However, an association between a low vitamin D level and nonalcoholic fatty liver disease (NAFLD) has not yet been definitively established. This study aimed to characterize the relationship between a vitamin D level and NAFLD in Korea.
METHODS:
A cross-sectional study involving 6,055 health check-up subjects was conducted. NAFLD was diagnosed on the basis of typical ultrasonographic findings and a history of alcohol consumption.
RESULTS:
The subjects were aged 51.7±10.3 years (mean±SD) and 54.7% were female. NAFLD showed a significant inverse correlation with the vitamin D level after adjusting for age and sex [odds ratio (OR)=0.85, 95% confidence interval (CI)=0.75-0.96]. The age- and sex-adjusted prevalence of NAFLD decreased steadily with increasing vitamin D level [OR=0.74, 95% CI=0.60-0.90, lowest quintile (≤14.4 ng/mL) vs highest quintile (≥28.9 ng/mL), p for trend <0.001]. Multivariate regression analysis after adjusting for other metabolic factors revealed that NAFLD showed a significant inverse correlation with both the vitamin D level (>20 ng/mL) [OR=0.86, 95% CI=0.75-0.99] and the quintiles of the vitamin D level in a dose-dependent manner (p for trend=0.001).
CONCLUSIONS:
The serum level of vitamin D, even when within the normal range, was found to be inversely correlated with NAFLD in a dose-dependent manner. Vitamin D was found to be inversely correlated with NAFLD independent of known metabolic risk factors. These findings suggest that vitamin D exerts protective effects against NAFLD.
PMID: 27044765
📄 Download the PDF from VitaminDWiki
2,000 IU daily did not improve NAFLD (no surprise)- June 2016
Too small of a dose (raised average Vitamin D level to 36 nanograms)
Wrong form of vitamin D for a poor liver
Many vitamins are associated with NAFLD, not just Vitamin D - Review Sept 2021
The Role of Vitamins in Non-Alcoholic Fatty Liver Disease: A Systematic Review
