Hypothesis: Some Mental Illness could be treated or prevented with vitamin D
Started reading Anatomy of an Epidemic: Magic Bullets, Psychiatric Drugs, and the Astonishing Rise of Mental Illness in America
I observe that
People with mental illness often have diseases associated with low vitamin D
Mental Illness gets worse when person must stay indoors (away from vitamin D)
Depression is associated with low vitamin D
Cognitive health in the elderly is associated with low vitamin D
Mental Illness has apparently increased in the past 40 years - at the same time that Vitamin D has increased
It will be interesting how many other factors to point to health problems associated with low vitamin D such as:
Seasonality
Month of birth (see table near the bottom of this page)
Gets worse when further from the equator
Is worse in those groups which are typically vitamin D deficient, such as:
- pregnant, seniors, dark skins, overweight, stay indoors a lot
Vitamin D levels of psychiatric out-patients did not vary much with season
Low serum levels of 25-hydroxyvitamin D (25-OHD) among psychiatric out-patients in Sweden
Relations with season, age, ethnic origin and psychiatric diagnosis
The Journal of Steroid Biochemistry and Molecular Biology
Volume 121, Issues 1–2, July 2010, Pages 467–470
Proceedings of the 14th Vitamin D Workshop
Mats B. Humblea, , , Sven Gustafssonb, Susanne Bejerota
a Department of Clinical Neuroscience, Division of Psychiatry, St. Göran, Karolinska Institutet, Stockholm, Sweden
b Department of Laboratory Medicine, Section for Clinical Chemistry, Karolinska Institutet, Stockholm, Sweden
In a chart review at a psychiatric out-patient department, latitude 59.3°N, a sample of patients with tests of serum 25-hydroxy-vitamin D (25-OHD) and plasma intact parathyroid hormone (iPTH) was collected, together with demographic data and psychiatric diagnoses. During 19 months, 117 patients were included. Their median 25-OHD was 45 nmol/l; considerably lower than published reports on Swedish healthy populations. Only 14.5% had recommended levels (over 75). In 56.4%, 25-OHD was under 50 nmol/l, which is related to several unfavourable health outcomes.
Seasonal variation of 25-OHD was blunted. Patients with ADHD had unexpectedly low iPTH levels. Middle East, South-East Asian or African ethnic origin, being a young male and having a diagnosis of autism spectrum disorder or schizophrenia predicted low 25-OHD levels. Hence, the diagnoses that have been hypothetically linked to developmental (prenatal) vitamin D deficiency, schizophrenia and autism, had the lowest 25-OHD levels in this adult sample, supporting the notion that vitamin D deficiency may not only be a predisposing developmental factor but also relate to the adult patients’ psychiatric state. This is further supported by the considerable psychiatric improvement that coincided with vitamin D treatment in some of the patients whose deficiency was treated.
Clinical Trial using 50,000 IU of vitamin D weekly to treat Schizophrenia Completion date Dec 2012
Vitamin D: Is It Ready for Psychiatric Prime Time?
Psychopharm Review: September 2010 - Volume 45 - Issue 9 - p 67–73
Very provocative title, no abstract
Vitamin D: Does it play a role in psychiatry?
Journal of Pakistan Medican Association, February, 2012
Mukesh Mohan Bhimani ( Department of Psychiatry, Aga Khan University, Karachi. )
Brief answer – possibly
PDF is attached at the bottom of this page
Seasonal Distribution of Psychiatric Births in England
Plos1 April 2012
Giulio Disanto1,2, Julia M. Morahan1,2, Melanie V. Lacey3, Gabriele C. DeLuca1,2, Gavin Giovannoni4, George C. Ebers1,2, Sreeram V. Ramagopalan1,2,3,4*
1 Wellcome Trust Centre for Human Genetics, University of Oxford, Oxford, United Kingdom, 2 Department of Clinical Neurology, University of Oxford, Oxford, United Kingdom, 3 London School of Hygiene and Tropical Medicine, London, United Kingdom, 4 Blizard Institute of Cell and Molecular Science, Queen Mary University of London, Barts and The London School of Medicine and Dentistry, London, United Kingdom
There is general consensus that season of birth influences the risk of developing psychiatric conditions later in life .
We aimed to investigate whether the risk of
schizophrenia (SC),
bipolar affective disorder (BAD) and
recurrent depressive disorder (RDD)
is influenced by month of birth in England to a similar extent as other countries using the largest cohort of English patients collected to date (n=57,971). When cases were compared to the general English population (n=29,183,034) all diseases showed a seasonal distribution of births (SC p=2.48E-05; BAD p=0.019; RDD p=0.015). This data has implications for future strategies of disease prevention.
PDF is attached at the bottom of this page
Why are Mental Illness patients extremely low on vitamin D?
They were low and got the mental illness
They became lower due to the drugs
They became lower due to being indoors most of the time
The Best Vitamins for People Taking Psychiatric Drugs Livesgtrong Nov 2010
Makes reference to "Human Psychopharmacology." Research published in "BMC Research Notes"
Vitamin D Deficiency Among Psychiatric Inpatients
Prim Care Companion CNS Disord. 2012; 14(2): PCC.11m01230.
Published online 2012 April 19. doi: 10.4088/PCC.11m01230
PMCID: PMC3425463
Robert E. McCue, MD, Richard A. Charles, DO, Geraldine C. M. Orendain, MD, Michel D. Joseph, MD, and James O. Abanishe, MD
Objective: Previous studies in northern Europe and Australia have indicated that vitamin D deficiency is common in psychiatric patients. This study aimed to determine the prevalence of vitamin D deficiency among psychiatric inpatients in a large North American city. The association of vitamin D status with clinical characteristics was also explored, and subgroups of patients that are more vulnerable to vitamin D deficiency were identified.
Method: This descriptive study looked at 107 unselected consecutive admissions to a psychiatric inpatient service in New York City between September and early December 2010. All patients were aged 18 years and older. Psychiatric diagnoses were established by attending psychiatrists as part of the routine assessment using criteria from the DSM-IV. Serum levels of 25-hydroxyvitamin D were measured by high-performance liquid chromatography, tandem mass spectrometry. A vitamin D–deficient state was defined as serum 25-hydroxyvitamin D level ? 20 ng/mL.
Results: Fifty-six (52.3%) patients were classified as deficient in vitamin D. Age and 25-hydroxyvitamin D level were significantly correlated (P = .001). Seventy-one percent of patients from age 18 to 34 years were deficient in vitamin D; this rate was significantly higher than the rate of deficiency in older patients (P = .017). No significant relationships were found between 25-hydroxyvitamin D level and gender, race/ethnicity, glycosylated hemoglobin, body mass index, and major psychiatric diagnostic categories.
Conclusions: A high percentage of psychiatric inpatients are deficient in vitamin D. Younger patients were more at risk for deficiency. Screening for vitamin D deficiency should be part of the health assessment of patients with major psychiatric illnesses.
PDF is attached at the bottom of this page
Vitamin D status of psychiatric inpatients in New Zealand’s Waikato region
David B Menkes1*, Kaye Lancaster2, Michael Grant2, Reginald W Marsh1, Peter Dean2 and Stephen A du Toit2
- Corresponding author: David B Menkes david.menkes@waikatodhb.health.nz
1 Waikato Clinical School, Private Bag 3200, Hamilton, 3240, New Zealand
2 Waikato District Health Board, Pembroke Street, Hamilton, 3240, New Zealand
BMC Psychiatry 2012, 12:68 doi:10.1186/1471-244X-12-68
Received: 25 October 2011, Accepted: 26 June 2012, Published: 26 June 2012
Background: Vitamin D deficiency is widespread in New Zealand, confers multiple health risks, and may be particularly common among people with psychiatric illness. We studied vitamin D status in an unselected sample of adult psychiatric inpatients in Hamilton (latitude 37.5?S) during late winter.
Methods: We recruited 102 consenting subjects and measured 25-hydroxy vitamin D3 levels in venous blood using a competitive electrochemiluminescence immunoassay. In addition to descriptive statistics, we used one-sample t-tests to determine the extent to which ethnic and diagnostic subgroups fell below the vitamin D deficiency threshold of 50 nM.
Results: 75 subjects (74%) had vitamin D levels <50 nM and thus had at least mild deficiency, while 19 (19%) were severely deficient with levels <25 nM. Rates of deficiency were comparable for men and women; only the former showed a correlation of vitamin D levels with age (r?=?0.45, p?PDF is attached at the bottom of this page**
Feasibility of screening for and treating vitamin D deficiency in forensic psychiatric inpatients.
J Forensic Leg Med. 2012 Nov;19(8):457-64. doi: 10.1016/j.jflm.2012.04.003. Epub 2012 May 4.
Murie J, Messow CM, Fitzpatrick B.
NHS Scotland State Hospital and NHS Education for Scotland, 2 Central Quay, Glasgow G3 8BW, United Kingdom. Electronic address: jillmurie@aol.com.
Neuroleptic and anti-epileptic medication, inadequate vitamin D intake and limited solar exposure increase the risk of vitamin D deficiency in high security psychiatric environments. Of the 33 inpatients (40% selected; 21% of hospital population) completing this cross-sectional study, 36% had insufficient and 58% deficient vitamin D. Five patients with vitamin D deficiency had secondary hyperparathyroidism, two of whom had osteopenia on dual-emission X-ray absorptiometry. At 1-year follow up, of the 31 patients eligible, 15 had accepted and continued supplements. Systematic screening is therefore necessary due to mental health and consent issues. Implications of supplementation and grounds access are discussed.
Copyright © 2012 Elsevier Ltd and Faculty of Forensic and Legal Medicine. All rights reserved.
PMID: 23084309
Vitamin d deficiency among psychiatric inpatients.
Prim Care Companion CNS Disord. 2012;14(2). pii: PCC.11m01230. Epub 2012 Apr 19.
McCue RE, Charles RA, Orendain GC, Joseph MD, Abanishe JO.
Department of Psychiatry, Woodhull Medical and Mental Health Center, New York University School of Medicine, Brooklyn, New York.
Objective: Previous studies in northern Europe and Australia have indicated that vitamin D deficiency is common in psychiatric patients. This study aimed to determine the prevalence of vitamin D deficiency among psychiatric inpatients in a large North American city. The association of vitamin D status with clinical characteristics was also explored, and subgroups of patients that are more vulnerable to vitamin D deficiency were identified.
Method: This descriptive study looked at 107 unselected consecutive admissions to a psychiatric inpatient service in New York City between September and early December 2010. All patients were aged 18 years and older. Psychiatric diagnoses were established by attending psychiatrists as part of the routine assessment using criteria from the DSM-IV. Serum levels of 25-hydroxyvitamin D were measured by high-performance liquid chromatography, tandem mass spectrometry. A vitamin D-deficient state was defined as serum 25-hydroxyvitamin D level ? 20 ng/mL.
Results: Fifty-six (52.3%) patients were classified as deficient in vitamin D. Age and 25-hydroxyvitamin D level were significantly correlated (P = .001). Seventy-one percent of patients from age 18 to 34 years were deficient in vitamin D ; this rate was significantly higher than the rate of deficiency in older patients (P = .017). No significant relationships were found between 25-hydroxyvitamin D level and gender, race/ethnicity, glycosylated hemoglobin, body mass index, and major psychiatric diagnostic categories.
Conclusions: A high percentage of psychiatric inpatients are deficient in vitamin D . Younger patients were more at risk for deficiency. Screening for vitamin D deficiency should be part of the health assessment of patients with major psychiatric illnesses.
PMID: 22943031 Full text online
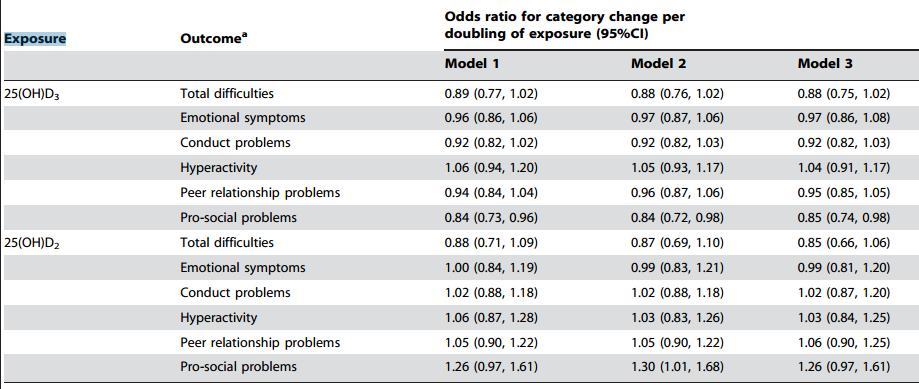
The association of 25-hydroxyvitamin D3 and D2 with behavioural problems in childhood.
PLoS One. 2012;7(7):e40097. Epub 2012 Jul 10.
Tolppanen AM, Sayers A, Fraser WD, Lewis G, Zammit S, Lawlor DA.
Medical Research Council Centre for Causal Analyses in Translational Epidemiology, School of Social and Community Medicine, University of Bristol, Bristol, United Kingdom.
BACKGROUND:Higher serum concentrations of 25-hydroxyvitamin D (25(OH)D), an indicator of vitamin D synthesis and intake, have been associated with better mental health and cognitive function. Concentrations of 1,25-dihydroxyvitamin D(3) (the active vitamin D(3) metabolite) have been associated with openness and extrovert behaviour, but 25(OH)D concentrations have not been associated with behavioural problems in humans.
METHODS:We investigated the prospective association between the different forms of 25(OH)D - 25(OH)D(3) and 25(OH)D(2)- and childhood behavioural problems in Avon Longitudinal Study of Parents and Children (ALSPAC). Serum 25(OH)D(3) and 25(OH)D(2) concentrations were assessed at mean age 9.9 years. Incident behavioural problems were assessed with Strengths and Difficulties Questionnaire (SDQ; emotional symptoms, conduct problems, hyperactivity-inattention problems, peer relationship problems and pro-social behaviour subscales and total difficulties score) at mean age 11.7. Sample sizes varied between 2413-2666 depending on the outcome.
RESULTS:Higher 25(OH)D(3) concentrations were weakly associated with lower risk of prosocial problems (fully adjusted odds ratio: OR (95% confidence interval: CI) 0.85 (0.74, 0.98)). Serum 25(OH)D(3) or 25(OH)D(2) concentrations were not associated with other subscales of SDQ or total difficulties score after adjusting for concfounders and other measured analytes related to vitamin D.
CONCLUSIONS:
Our findings do not support the hypothesis that 25-hydroxyvitamin D status in childhood has important influences on behavioural traits in humans.
PMID: 22808099 Full text online
Note by VitaminDWiki
Table shows a weak association between behaviorial problems and low vitamin D3, but not D2
Vitamin D deficiency and psychotic features in mentally ill adolescents: A cross-sectional study.
BMC Psychiatry. 2012 May 9;12:38.
Gracious BL, Finucane TL, Friedman-Campbell M, Messing S, Parkhurst MN.
Center for Innovation in Pediatric Practice, The Research Institute at Nationwide Children's Hospital and The Ohio State University, Columbus, OH, USA. Barbara.gracious@nationwidechildrens.org.
BACKGROUND: Vitamin D deficiency is a re-emerging epidemic, especially in minority populations. Vitamin D is crucial not only for bone health but for proper brain development and functioning. Low levels of vitamin D are associated with depression, seasonal affective disorder, and schizophrenia in adults, but little is known about vitamin D and mental health in the pediatric population.
METHODS: One hundred four adolescents presenting for acute mental health treatment over a 16-month period were assessed for vitamin D status and the relationship of 25-OH vitamin D levels to severity of illness, defined by presence of psychotic features.
RESULTS: Vitamin D deficiency (25-OH D levels <20?ng/ml) was present in 34%; vitamin D insufficiency (25-OH D levels 20-30?ng/ml) was present in 38%, with a remaining 28% in the normal range. Adolescents with psychotic features had lower vitamin D levels (20.4?ng/ml vs. 24.7?ng/ml; p?=?0.04, 1 df). The association for vitamin D deficiency and psychotic features was substantial (OR 3.5; 95% CI 1.4-8.9; p <0.009). Race was independently associated with vitamin D deficiency and independently associated with psychosis for those who were Asian or biracial vs. white (OR?=?3.8; 95% CI 1.1?13.4; p?Full text online** ](http://www.ncbi.nlm.nih.gov/pubmed/22571731%20)
Vitamin D status of psychiatric inpatients in New Zealand's Waikato region.
BMC Psychiatry. 2012 Jun 26;12:68.
Menkes DB, Lancaster K, Grant M, Marsh RW, Dean P, du Toit SA.
Waikato Clinical School, Private Bag 3200, Hamilton, 3240, New Zealand. david.menkes@waikatodhb.health.nz
BACKGROUND: Vitamin D deficiency is widespread in New Zealand, confers multiple health risks, and may be particularly common among people with psychiatric illness. We studied vitamin D status in an
METHODS: We recruited 102 consenting subjects and measured 25-hydroxy vitamin D3 levels in venous blood using a competitive electrochemiluminescence immunoassay. In addition to descriptive statistics, we used one-sample t-tests to determine the extent to which ethnic and diagnostic subgroups fell below the vitamin D deficiency threshold of 50 nM.
RESULTS: 75 subjects (74%) had vitamin D levels <50 nM and thus had at least mild deficiency, while 19 (19%) were severely deficient with levels <25 nM. Rates of deficiency were comparable for men and women; only the former showed a correlation of vitamin D levels with age (r?=?0.45, p?Full text online** ](http://www.ncbi.nlm.nih.gov/pubmed/22734499%20)
Vitamin D deficiency and depression: Causal relationship or artifact?
Biofactors. 2012 Sep;38(5):317-9. doi: 10.1002/biof.1028. Epub 2012 Jun 2.
Rastmanesh R, Beauchet O, Annweiler C.
Human Nutrition and Dietetics Department, Shahid Beheshti University of Medical Sciences, National Nutrition and Food Sciences Technology Research Institute, Tehran, Iran.
PMID: 22674822
Vitamin D: a potential role in reducing suicide risk?
Int J Adolesc Med Health. 2011;23(3):157-65.
Tariq MM, Streeten EA, Smith HA, Sleemi A, Khabazghazvini B, Vaswani D, Postolache TT.
Mood and Anxiety Program, Department of Psychiatry, University of Maryland School of Medicine, Baltimore, MD 21201, USA.
Suicide attempts are known to peak in the spring , overlapping with the time of year when 25-hydroxyvitamin D [25(OH)D] levels are at their nadir in the northern hemisphere because of negligible skin production of vitamin D owing to low levels of ultraviolet B radiation. Low levels of 25(OH)D, the vitamin D metabolite used to diagnose vitamin D deficiency, have been associated with certain pro-suicidal factors such as exacerbation of depression, anxiety, psychosis, and certain medical conditions. Therefore, we hypothesize that vitamin D deficiency could also be associated with increased risk of completed suicides. Here, we briefly review the literature on vitamin D, its deficiency, and its reported association with certain risk factors for suicide.
PMID: 22191178
Effects of vitamin D supplementation on cognitive and emotional functioning in young adults--a randomised controlled trial.
PLoS One. 2011;6(11):e25966. Epub 2011 Nov 4.
Dean AJ, Bellgrove MA, Hall T, Phan WM, Eyles DW, Kvaskoff D, McGrath JJ.
Queensland Brain Institute, The University of Queensland, St Lucia, Australia. a.dean@uq.edu.au
BACKGROUND: Epidemiological research links vitamin D status to various brain-related outcomes. However, few trials examine whether supplementation can improve such outcomes and none have examined effects on cognition. This study examined whether Vitamin D supplementation led to improvements in diverse measures of cognitive and emotional functioning, and hypothesised that supplementation would lead to improvements in these outcomes compared to placebo.
METHODS/PRINCIPAL FINDINGS: Healthy young adults were recruited to a parallel-arm, double-blind trial conducted at The University of Queensland. Participants were randomly allocated to receive Vitamin D (one capsule daily, containing 5000 IU cholecalciferol) or identical placebo capsule for six weeks. All participants and outcome assessors were blinded to group assignment. Primary outcome measures assessed at baseline and 6 weeks were working memory, response inhibition and cognitive flexibility. Secondary outcomes were: hallucination-proneness, psychotic-like experiences, and ratings of depression, anxiety and anger. 128 participants were recruited, randomised and included in primary analyses (vitamin D n = 63; placebo n = 65). Despite significant increases in vitamin D status in the active group, no significant changes were observed in working memory (F = 1.09; p = 0.30), response inhibition (F = 0.82; p = 0.37), cognitive flexibility (F = 1.37; p = 0.24) or secondary outcomes. No serious adverse effects were reported.
CONCLUSIONS: Our findings indicate that vitamin D supplementation does not influence cognitive or emotional functioning in healthy young adults . Future controlled trials in targeted populations of interest are required to determine whether supplementation can improve functioning in these domains. Australian and New Zealand Clinical Trials Registry; ACTRN12610000318088.
PMID: 22073146 Full text online
'D' for depression: any role for vitamin D? 'Food for Thought' II.
Acta Psychiatr Scand. 2011 Oct;124(4):243-9. doi: 10.1111/j.1600-0447.2011.01705.x. Epub 2011 Apr 12.
Parker G, Brotchie H.
School of Psychiatry, University of New South Wales, Randwick, Sydney, NSW, Australia. g.parker@unsw.edu.au
OBJECTIVE: While there has long been interest in any nutritional contribution to the onset and treatment of mood disorders, there has been increasing scientific evaluation of several candidate nutritional and dietary factors in recent years. In this paper, we overview research into any vitamin D insufficiency and deficiency contribution to depression.
METHOD: The relevant literature was reviewed.
RESULTS: Cross-sectional studies have identified associations between depression and low vitamin D levels, but studies have failed to clarify whether vitamin D deficiency is an antecedent cause, correlate or consequence of depression. While vitamin D deficiency and insufficiency have been linked with seasonal affective disorder, suggested associations have not been rigorously tested. There has been insufficient research to establish whether and when vitamin D supplementation should be considered as an augmentation strategy with antidepressant drugs.
CONCLUSION: There is currently insufficient evidence to argue strongly for vitamin D supplementation in patients with depression, but such a strategy is worthy of consideration in depressed patients whose lifestyle and geographical residence may indicate a risk of vitamin D insufficiency--or where low vitamin D levels have been quantified.
© 2011 John Wiley & Sons A/S.
PMID: 21480836
Vitamin D and depression.
J Psychosoc Nurs Ment Health Serv. 2011 Feb;49(2):15-8. doi: 10.3928/02793695-20110111-02. Epub 2011 Jan 21.
Howland RH.
Psychiatry, University of Pittsburgh School of Medicine, Western Psychiatric Institute and Clinic, Pittsburgh, PA 15213, USA. HowlandRH@upmc.edu
Vitamin D is an essential nutrient proven to be important for bone health. It has other physiological functions, and there are plausible reasons for investigating vitamin D in depressive disorders. Some cross-sectional clinical and epidemiologic studies, but not all studies, have found that low levels of vitamin D are significantly associated with higher levels of depressive symptoms or with a depression diagnosis. However, cross-sectional studies cannot establish causality, and the methodology of these studies has been criticized. Due to the poor quality of the treatment studies, the effectiveness of vitamin D for depression cannot be adequately assessed. Current evidence does not definitively demonstrate that vitamin D deficiency is a cause of or risk for developing depression or that vitamin D is an effective therapy for depression.
Copyright © 2011, SLACK Incorporated. PMID: 21261225
5700 IU of vitamin D not enough to decrease depression
Effect of vitamin D supplement on depression scores in people with low levels of serum 25-hydroxyvitamin D:
nested case-control study and randomised clinical trial.
Br J Psychiatry. 2012 Jul 12.
Kjærgaard M, Waterloo K, Wang CE, Almås B, Figenschau Y, Hutchinson MS, Svartberg J, Jorde R.
MD, Medical Clinic, University Hospital of North Norway and Endocrine Research Group, Department of Clinical Medicine, University of Tromsø; Knut Waterloo, PsyD, Department of Neurology, University Hospital of North Norway and Department of Psychology, University of Tromsø; Catharina E. A. Wang, PsyD, Department of Neurology, University Hospital of North Norway and Department of Psychology, University of Tromsø; Bjørg Almås, MD, PhD, Hormone Laboratory, Haukeland University Hospital and Institute of Medicine, University of Bergen; Yngve Figenschau, MD, PhD, Department of Medical Biochemistry, University Hospital of North Norway and Institute of Medical Biology, University of Tromsø; Moira S. Hutchinson, MD, Johan Svartberg, MD, PhD, Rolf Jorde, MD, PhD, Medical Clinic, University Hospital of North Norway and Endocrine Research Group, Department of Clinical Medicine, University of Tromsø, Norway.
AIMS: To compare depressive symptoms in participants with low and high serum 25-hydroxyvitamin D (25(OH)D) levels and to examine whether supplementation with vitamin D(3) would improve symptoms in those with low serum 25(OH)D levels.
METHOD: Participants with low 25(OH)D levels were randomised to either placebo or 40 000 IU vitamin D(3) per week for 6 months. Individuals with high serum 25(OH)D levels were used as nested controls. Depressive symptoms were evaluated with the Beck Depression Inventory, Hospital Anxiety and Depression Scale, Seasonal Pattern Assessment Scale and Montgomery-Åsberg Depression Rating Scale. The study was registered at ClinicalTrials.gov (NCT00960232).
RESULTS: Participants with low 25(OH)D levels (n = 230) at baseline were more depressed (P<0.05) than participants with high 25(OH)D levels (n = 114). In the intervention study no significant effect of high-dose vitamin D was found on depressive symptom scores when compared with placebo.
CONCLUSIONS: Low levels of serum 25(OH)D are associated with depressive symptoms, but no effect was found with vitamin D supplementation.
PMID: 22790678
Children and adolescents with severe mental illness need vitamin D supplementation regardless of disease or treatment.
Child Adolesc Psychopharmacol. 2011 Apr;21(2):157-61. Epub 2011 Apr 12.
Bonnot O, Inaoui R, Raffin-Viard M, Bodeau N, Coussieu C, Cohen D.
Child and Adolescent Department and Reference Center for Rare Disease with Psychiatric Expression, Groupe Hospitalier Pitié Salpétriere, Assistance Publique Hopitaux de Paris, Paris, France. olivier.bonnot@psl.aphp.fr
BACKGROUND: To protect against osteoporosis, keeping the vitamin D blood level (25[OH]D; VDBL) above 30?ng/mL is recommended. It is established that regular intake of vitamin D, calcium intake, and physical exercise contribute to maximizing bone mineral mass during childhood and adolescence. Recent articles suggest that patients with schizophrenia treated with antipsychotics have low VDBL and may have a higher risk of hip fractures in their later years than the general population.
OBJECTIVES: To evaluate whether adolescent psychiatric inpatient VDBL is lower than the 30-ng/mL optimal threshold and to document low-VDBL risk factors.
METHOD: We determined the VDBL of all consecutive inpatients from three adolescents units in 2009 (N?=?136). Univariate analyses explored the influence on VDBL of (1) well-documented risk factors (e.g., age, gender, ethnic origin, body mass index, or season) and (2) suspected risk factors (e.g., disease type or antipsychotic treatment).
RESULTS: All but six patients had a VDBL <30?ng/mL (mean [?±?SD]: 15.9 [?±?8.4] ng/mL). VDBL was significantly lower for all patients during the first quarter of the year compared to the other three (all p?
See also web
- Hypovitaminosis D in Psychiatric Inpatients: Clinical Correlation with Depressive Symptoms, Cognitive Impairment, and Prescribing Practices. Psychosomatics Journal, Dec 2012
- 37% were low on vitamin D, but no strong correlation between Vitamin D level and depressive symptoms or cognitive function
- Daily Mail article on Birth Month - June 2011 sample table follows

Mental Disorders wikipedia
Acute stress disorder Adjustment disorder Amnesia Anxiety disorder Anorexia nervosa Antisocial personality disorder Asperger syndrome
Attention deficit/hyperactivity disorder Autism Autophagia Avoidant personality disorder Bereavement Bestiality Bibliomania Binge eating disorder, Bipolar disorder Body dysmorphic disorder Borderline personality disorder Brief psychotic disorder Bulimia nervosa Childhood disintegrative disorder , Circadian rhythm sleep disorder Conduct disorder Conversion disorder Cyclothymia Delirium Delusional disorder Dementia Dependent personality disorder, Depersonalization disorder Depression Disorder of written expression Dissociative fugue Dissociative identity disorder Down syndrome Dyslexia Dyspareunia, Dyspraxia Dysthymic disorder Erotomania Encopresis Enuresis Exhibitionism Expressive language disorder Factitious disorder Folie à deux Ganser syndrome, Gender identity disorder Generalized anxiety disorder General adaptation syndrome Histrionic personality disorder Hyperactivity disorder Primary hypersomnia, Hypochondriasis Hyperkinetic syndrome Hysteria Intermittent explosive disorder Joubert syndrome Kleptomania Mania Munchausen syndrome, Mathematics disorder Narcissistic personality disorder Narcolepsy Nightmares Obsessive-compulsive disorder Obsessive-compulsive personality disorder , Oneirophrenia Oppositional defiant disorder Pain disorder Panic attacks Panic disorder Paranoid personality disorder Parasomnia Pathological gambling, Perfectionism Pervasive developmental disorder Pica Postpartum Depression Post-traumatic embitterment disorder Post-traumatic stress disorder, Primary insomnia Psychotic disorder Pyromania Reading disorder Reactive attachment disorder Retts disorder Rumination syndrome Schizoaffective disorder, Schizoid Schizophrenia Schizophreniform disorder Schizotypal personality disorder Seasonal affective disorder Self Injury Separation anxiety disorder, Sadism and masochism Shared psychotic disorder Sleep disorder Sleep terror disorder Sleepwalking disorder Social anxiety disorder Somatization disorder, Stereotypic movement disorder Stuttering Suicide Tourette syndrome Transient tic disorder Trichotillomania
