How I Treat Vitamin D Deficiency - for Cancer
the following is most of the text and graphics from the PDF. Extracted so that it can be Google-translated into 50+ other languages
- [tiki-download_file.php?fileId=1434]
By Qamar J. Khan, MD, and Carol J. Fabian, MD
Department of Internal Medicine, Division Hematology and Oncology, University of Kansas Medical Center, Kansas City, KS
Copyright © 2010 by American Society of Clinical Oncology MARCH 2010 jop.ascopubs.org
Importance of Vitamin D
Vitamin D is important in a number of physiologic processes, including calcium absorption, innate and adaptive immunity, and homeostasis of a number of organs. Chronic vitamin D deficiency in adults results in osteoporosis, osteomalacia, muscle weakness, and increased risk of falls.1-4 Poor vitamin D intake and low blood levels of vitamin D metabolites are associated with increased incidence and severity of several autoimmune diseases involving the T helper type 1 lymphocyte,5,6 including multiple sclerosis,7 rheumatoid arthritis,8 type I diabetes,9 systemic lupus erythematosis,10 and psoriasis.11,12 Lower levels of vitamin D, adjusted for body mass index, are also associated with increased risk of hypertension, myocardial infarction, and death as a result of cardiovascular disease.13-16
Of particular interest to oncologists is the reduced incidence of some epithelial malignancies, particularly breast and colon, with higher intake or blood levels of vitamin D.17-23
In some observational studies, higher levels of vitamin D have also been associated with reduced recurrence and mortality from breast, colon, and ovarian cancers.24-28 Although there is evidence that vitamin D supplementation can improve muscle strength and reduce the number of falls among the elderly and fractures resulting from osteoporosis,1,29-32 there is little direct evidence that low-dose vitamin D supplementation can significantly reduce cancer incidence or recurrence. Reduction in cancer incidence was observed in a small placebocontrolled trial for calcium and vitamin D (1,100 IU/d), and this reduction seemed greater than that seen with calcium alone, when cancers arising in the first year of the trial were censored.33 However, no reduction in breast or colon cancer was observed for the calcium and vitamin D arm in the Women’s Health Initiative trial, in which the dose of vitamin D for the treatment arm was only 400 IU, and both the placebo and treatment arms were allowed to ingest nonstudy vitamin D up to 1,000 IU/d.34-36
Regardless of whether vitamin D helps prevent cancer or its recurrence, the high frequency of vitamin D inadequacy in the US population37,38 and the adverse impact on bone health of both vitamin D depletion and many of today’s systemic cancer treatments makes it important for oncologists to understand vitamin D physiology and recognize, treat, and prevent vitamin D deficiency.
Vitamin D Metabolism and Its Role in Breast and Colon Homeostasis
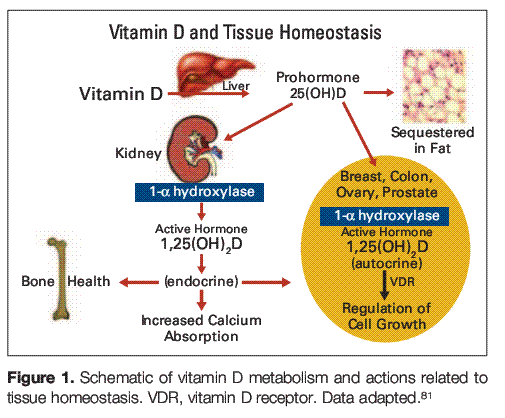
Cholecalciferol (vitamin D3), either ingested or manufactured in the skin in response to sun exposure, must first be converted to the prohormone 25(OH)D in the liver and then to the active hormone 1,25(OH)2D by tissues containing the 1hydroxylase enzyme. The active form of vitamin D—
1,25(OH)2D—may function in an endocrine fashion, as in the case of 1,25(OH)2D produced in the kidney, or an autocrine/ paracrine manner, as in the case of 1,25(OH)2D produced in several other organs in which vitamin D plays an important role in homeostasis (Fig 1). The breast and colon are two of these organs, and epithelial cells from both make 1,25(OH)2D from circulating precursors. In the breast, vitamin D seems to be important in limiting proliferation and neoangiogenesis in response to hormones and growth factors and promoting differentiation.39-47 In the colon, vitamin D limits proliferation in response to bile acids and other carcinogens and promotes differentiation and expression of adhesion and cell-junction proteins.48-50
Sources of Vitamin D and Standard Doses of Vitamin D Supplements
Vitamin D sufficiency is defined in terms of the serum level of the prohormone 25(OH)D required for bone health, which is 30 to 32 ng/mL. Maintenance of a 30 to 32 ng/mL serum level requires approximately 2,200 to 3,000 IU/d of vitamin D from all sources, including ultraviolet light exposure, food, and supplements.20,51,52 Recommendations from the Institute of Medicine for vitamin D supplementation suggest 200 IU of vitamin D daily from birth through age 50 years, 400 IU/d for individuals age 51 to 70 years, and 600 IU/d for those age 70 years or older.53 These recommendations presume some sun exposure and vitamin D intake from food and are not adequate to treat vitamin D deficiency.54,55 Historically, the source of most vitamin D has been ultraviolet light–induced skin manufacture of cholecalciferol. A single whole-body dose of ultraviolet radiation associated with minimal erythema produces 10,000 IU of vitamin D.55 Thus, 15 to 20 minutes of daily sun exposure without sunscreen in lower midwestern and southern latitudes between 10:00 AM and 3:00 PM is usually sufficient to ensure adequate synthesis of vitamin D metabolites. Large excesses of vitamin D3 from prolonged sun exposure are destroyed in the skin, making vitamin D toxicity from sun
exposure improbable.54,55 In contrast, with the exception of coldwater ocean fish, food is a poor source of vitamin D.54
Three ounces of herring, which few individuals eat, provides 1,300 IU of vitamin D, 3.5 oz of the more commonly ingested salmon provides 350 IU, and 1 teaspoon of cod liver oil provides approximately 400 IU. However, the amount of vitamin D in 1 cup of fortified milk or orange juice is only 100 IU, with 50-100 IU per cup of breakfast cereal or tablespoon of margarine.54,56,57 Today, with more time spent indoors and increased use of sunscreen, higher basal intakes of 1,000 to 2,000 IU/d from supplements are recommended to avoid vitamin D deficiency.23,58-60 Multiple vitamins generally contain 400 IU of vitamin D, and calcium supplements provide 200 to 400 IU of vitamin D. Vitamin D3 supplements without other additives are readily available over the counter in 400, 1,000, and 2,000 IU strengths at pharmacies and most grocery stores. These supplements are much smaller in size than pills containing calcium and vitamin D and generally cost $10 or less for a 3-month supply. At similar doses, vitamin D3 may be more potent than vitamin D2 (ergocalciferol), which is obtained from plants.61 The Institute of Medicine lists 2,000 IU/d as the upper tolerable limit, but in fact, there is little evidence of toxicity unless doses of 10,000 IU of vitamin D3/d are exceeded.53,62
Definition of Vitamin D Deficiency and Incidence in US Population
Vitamin D adequacy is currently defined as a function of calcium homeostasis, with lower vitamin D levels resulting in reduced absorption of calcium from the gut and/or elevations of parathyroid hormone (PTH) considered inadequate. Blood levels of the prohormone 25(OH)D, with a half-life of 2 to 3 weeks, are used to describe vitamin D sufficiency rather than levels of 1,25(OH)2D, which has a half-life of only 3 to 4 hours.54,58 Furthermore, in early vitamin D depletion, blood levels of 1,25(OH)2D can be misleading because they may rise initially in response to elevations in PTH, which is sensitive to til 25(OH)D reaches a minimum of 30 ng/mL, and PTH continues to decrease until this level is reached,64,65 a 25(OH)D serum level of 30 to 32 ng/mL is considered sufficient and levels of 20 to 29 ng/mL insufficient.
Optimal Vitamin D Status
At the present time, 25(OH)D levels in the range of 30 to 60 ng/mL are considered optimal, but higher levels up to 100 ng/mL are often seen in individuals with outdoor occupations receiving intense sun exposure without ill effects.55
Correlative studies of 25(OH)D with muscle strength or risk of breast or colon cancer have prompted several investigators to suggest that the optimal 25OHD target for multiple health outcomes is 40 to 50 ng/mL.19,20 Garland et al23 suggest that increasing 25(OH)D to a range of 40 to 60 ng/mL from the current US average could reduce risk of breast cancer by 25% and colon cancer by 27%. Intakes of at least 4,000 IU daily from all sources would be needed to maintain 25(OH)D levels of 40 to 60 ng/mL. Practically speaking, supplements of 2,000 IU daily plus some sun exposure would probably be required to maintain a 25(OH)D level of 40 to 60 ng/mL year round.23
Vitamin D Toxicity
Vitamin D intoxication with renal stones and hypercalcemia may be observed when serum levels of 25(OH)D are greater than 150 ng/mL (374 nmol/L). For a good margin of safety, levels greater than 100 ng/mL should probably be avoided.
Prevalence of Vitamin D Deficiency
The incidence of vitamin D deficiency (ie, 25(OH)D 20 ng/ mL) in US adults is approximately 25% for men and approximately 35% for women.38 Postmenopausal women with osteoporosis are especially likely to exhibit deficiency.1,63 The problem is not limited to older women. Seventy-four percent of a cohort of newly diagnosed premenopausal patients with breast cancer from the New York City area66 and 50% of a cohort of premenopausal women from the Kansas City area at high risk for the disease were reported as exhibiting vitamin D deficiency.67
Who Should Have Serum 25(OH)D Levels Assessed?
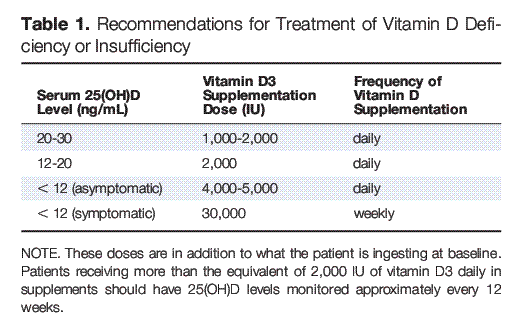
Table 1. Recommendations for Treatment of Vitamin D Deficiency or Insufficiency
Frequency of Vitamin D Supplementation
We suggest obtaining a baseline 25(OH)D level in all individuals who are initiating therapy that could impact bone mineralization. This means that premenopausal women undergoing chemotherapy or medical or surgical ovarian ablation and postmenopausal women beginning aromatase-inhibitor therapy should be tested. Estrogen upregulates both the 1hydroxylase enzyme that converts 25(OH)D to 1,25(OH)2D and increases levels of vitamin D receptor protein.68,69 Thus, depletion of estrogen may unmask a subclinical vitamin D deficiency, which may increase the severity of muscle and joint symptoms experienced by women entering menopause or undergoing aromatase-inhibitor therapy. For cancer survivors, 25(OH)D levels drawn in late winter or early spring will provide an estimation of trough levels of vitamin D.
Individuals at High Risk for Vitamin D Deficiency
Individuals most likely to have vitamin D deficiency are those who do not take supplements, are elderly,54 are darkly pigmented,70 are obese,71 have osteoporosis or osteopenia,1 avoid any sun exposure without sunscreen,72,73 are typically veiled,74 live in a highly polluted environment,75 or have Crohn’s disease or other reasons for fat malabsorption.54
Individuals With Symptoms of Vitamin D Deficiency
Symptoms of vitamin D deficiency can be rather nonspecific and include fatigue, altered mood and depression, insomnia, nonradicular back pain, arthralgias (particularly of the wrists, ankles, shoulders, and shins), proximal muscle weakness, headache, and hair loss.76,77 Symptoms are uncommon with 25(OH)D levels greater than 20 ng/mL, and even individuals with mild to moderate deficiency may not spontaneously complain of symptoms unless they are undergoing treatment that results in reduced formation of 1,25(OH)2D or decreased vitamin D receptor activation, such as estrogen depletion as the result of aromatase-inhibitor therapy. In a pilot study, we found that 50,000 IU of vitamin D3 weekly for 12 weeks was effective in treating vitamin D insufficiency in women receiving the aromatase inhibitor letrozole, and higher levels of 25(OH)D were associated with reduced disability from aromatase inhibitor–associated joint pain.78
How to Treat Vitamin D Deficiency
The first step in treating vitamin D deficiency is to obtain a baseline 25(OH)D blood level and then decide on the target replacement level and how quickly that target must be reached (Table 1). Each 1,000 IU of vitamin D3 daily in addition to what the patient is currently ingesting will raise the level of 25(OH)D by 10 ng/mL after a few weeks. Note that more may be required for individuals who are obese, because vitamin D is sequestered in adipose tissue.79
NOTE. These doses are in addition to what the patient is ingesting at baseline. Patients receiving more than the equivalent of 2,000 IU of vitamin D3 daily in supplements should have 25(OH)D levels monitored approximately every 12 weeks.
A common example encountered by an oncologist would be that of an asymptomatic postmenopausal woman about to begin aromatase-inhibitor therapy who is found to have mild osteopenia. Her 25(OH)D level is 20 ng/mL. In addition to ensuring adequate calcium intake, if the target 25(OH)D serum level is 40 ng/mL, the simplest treatment is to ask her to take an extra 2,000 IU of over-the-counter vitamin D3, checking the 25(OH)D level again at 3 months. It should be cautioned that 1% of the population may have occult primary hyperparathyroidism, which may be unmasked by vitamin D and calcium supplementation, resulting in hypercalcemia.80
For individuals of average weight with insufficiency only during the winter months who get appreciable sun exposure during the summer, we usually suggest vitamin D3 supplementation only during the late fall, winter, and early spring.
A different scenario might involve a woman with a body mass index of 35 kg/m2 ready to begin antihormonal therapy who already complains of fatigue, weakness, and diffuse arthralgias. A 25(OH)D level of 9 ng/mL shows evidence of severe vitamin D deficiency and is likely responsible for some or all of her symptoms. In this case, the 25(OH)D level should be increased as quickly as possible with either 4,000 IU vitamin D3 daily or 30,000 IU weekly, checking the level again at 6 and 12 weeks. When the desired level is achieved, maintenance of 40 ng/mL is usually possible with 2,000 IU per day, but in the case of obese women, higher doses may be needed.79
The importance of educating patients, checking compliance, and monitoring 25(OH)D levels every 3 months during treatment of deficiency and early maintenance phases cannot be overstressed. Patients easily get confused. We have observed situations in which weekly high-dose vitamin D was taken daily by mistake. In summary, vitamin D plays an important role in the homeostasis of a variety of organ systems. The precise roles that vitamin D plays in prevention of cancer and recurrence— along with the blood levels necessary to carry out those roles— have yet to be defined. In the meantime, oncologists are encouraged to check vitamin D levels in individuals about to undergo treatment that could impact bone and muscle health, replace deficiencies, and maintain 25(OH)D at levels optimum for musculoskeletal health.
Authors’ Disclosures of Potential Conflicts of Interest
Although all authors completed the disclosure declaration, the following author(s) indicated a financial or other interest that is relevant to the subject matter under consideration in this article. Certain relationships marked with a “U” are those for which no compensation was received;
Author Contributions
Conception and design: Qamar J. Khan, Carol J. Fabian
Manuscript writing: Qamar J. Khan, Carol J. Fabian
Final approval of manuscript: Qamar J. Khan, Carol J. Fabian
those relationships marked with a “C” were compensated. For a detailed description of the disclosure categories, or for more information about ASCO’s conflict of interest policy, please refer to the Author Disclosure Declaration and the Disclosures of Potential Conflicts of Interest section in Information for Contributors.
Employment or Leadership Position: None Consultant or Advisory Role: None Stock Ownership: None Honoraria: None Research Funding: Qamar J. Khan, Novartis Expert Testimony: None Other Remuneration: None
Corresponding author: Carol J. Fabian, MD, University of Kansas Medical Center, 3901 Rainbow Blvd, Kansas City, KS 66160; e-mail: cfabian@kumc.edu.
DOI: 10.1200/JOP.091087
References
Lips P: Vitamin D deficiency and osteoporosis: The role of vitamin D deficiency and treatment with vitamin D and analogues in the prevention of osteoporosisrelated fractures. Eur J Clinic Invest 26:436-442, 1996
Bischoff HA, Stahelin HB, Urscheler N, et al: Muscle strength in the elderly: Its relation to vitamin D metabolites. Arch Phys Med Rehabil 80:54-58, 1999
Bischoff-Ferrari HA, Zhang Y, Kiel DP, et al: Positive association between serum 25-hydroxyvitamin D level and bone density in osteoarthritis. Arthritis Rheum 53:821-826, 2005
Janssen HC, Samson MM, Verhaar HJ: Vitamin D deficiency, muscle function, and falls in elderly people. Am J Clin Nutr 75:611-615, 2002
Adorini L, Penna G: Control of autoimmune diseases by the vitamin D endocrine system. Nat Clin Pract Rheumatol 4:404-412, 2008
Zold E, Szodoray P, Gaal J, et al: Vitamin D deficiency in undifferentiated connective tissue disease. Arthritis Res Ther 10:R123, 2008
Munger KL, Levin LI, Hollis BW, et al: Serum 25-hydroxyvitamin D levels and risk of multiple sclerosis. JAMA 296:2832-2838, 2006
Patel S, Farragher T, Berry J, et al: Association between serum vitamin D metabolite levels and disease activity in patients with early inflammatory polyarthritis. Arthritis Rheum 56:2143-2149, 2007
Mohr SB, Garland CF, Gorham ED, et al: The association between ultraviolet B irradiance, vitamin D status and incidence rates of type 1 diabetes in 51 regions worldwide. Diabetologia 51:1391-1398, 2008
Wu PW, Rhew EY, Dyer AR, et al: 25-hydroxyvitamin D and cardiovascular risk factors in women with systemic lupus erythematosus. Arthritis Rheum 61:1387-1395, 2009
DiSepio D, Chandraratna RA: New drugs in the treatment of psoriasis. Expert Opin Investig Drug 9:79-93, 2000
Tanghetti EA: The role of topical vitamin D modulators in psoriasis therapy. J Drugs Dermatol 8:s4-s8, 2009 (suppl 8)
Pilz S, Tomaschitz A, Ritz E, et al: Vitamin D status and arterial hypertension: A systematic review. Nat Rev Cardiol 6:621-630, 2009
Giovannucci E, Liu Y, Hollis BW, et al: 25-hydroxyvitamin D and risk of myocardial infarction in men: A prospective study. Arch Intern Med 168:1174-1180, 2008
Kendrick J, Targher G, Smits G, et al: 25-hydroxyvitamin D deficiency is independently associated with cardiovascular disease in the Third National Health and Nutrition Examination Survey. Atherosclerosis 205:255-260, 2009
Kilkkinen A, Knekt P, Aro A, et al: Vitamin D status and the risk of cardiovascular disease death. Am J Epidemiol 170:1032-1039, 2009
Garland FC, Garland CF, Gorham ED, et al: Geographic variation in breast cancer mortality in the United States: A hypothesis involving exposure to solar radiation. Prev Med 19:614-622, 1990
John EM, Schwartz GG, Dreon DM, et al: Vitamin D and breast cancer risk: The NHANES I epidemiologic follow-up study 1971-1975 to 1992—National Health and Nutrition Examination Survey. Cancer Epidemiol Biomarkers Prev 8:399-406, 1999
Garland CF, Gorham ED, Mohr SB, et al: Vitamin D and prevention of breast cancer: Pooled analysis. J Steroid Biochem Mol Biol 103:708-711, 2007
Bischoff-Ferrari HA, Giovannucci E, Willett WC, et al: Estimation of optimal serum concentrations of 25-hydroxyvitamin D for multiple health outcomes. Am J Clin Nutr 84:18-28, 2006
John EM, Koo J, Schwartz GG: Sun exposure and prostate cancer risk: Evidence for a protective effect of early-life exposure. Cancer Epidemiol Biomarkers Prev 16:1283-1286, 2007
Tworoger SS, Lee IM, Buring JE, et al: Plasma 25-hydroxyvitamin D and 1,25-dihydroxyvitamin D and risk of incident ovarian cancer. Cancer Epidemiol Biomarkers Prev 16:783-788, 2007
Garland CF, Gorham ED, Mohr SB, et al: Vitamin D for cancer prevention: Global perspective. Ann Epidemiol 19:468-483, 2009
Porojnicu AC, Lagunova Z, Robsahm TE, et al: Changes in risk of death from breast cancer with season and latitude: Sun exposure and breast cancer survival in Norway. Breast Cancer Res Treat 102:323-328, 2007
Freedman DM, Looker AC, Chang SC, et al: Prospective study of serum vitamin D and cancer mortality in the United States. J Natl Cancer Inst 99:1594-1602, 2007
Goodwin PJ, Ennis M, Pritchard KI, et al: Prognostic effects of 25-hydroxyvitamin D levels in early breast cancer. J Clin Oncol 27:3757-3763, 2009
Moan J, Porojnicu AC, Robsahm TE, et al: Solar radiation, vitamin D and survival rate of colon cancer in Norway. J Photochem Photobiol B 78:189-193, 2005
Lefkowitz ES, Garland CF: Sunlight, vitamin D, and ovarian cancer mortality rates in US women. Int J Epidemiol 23:1133-1136, 1994
Gloth FM III, Smith CE, Hollis BW, et al: Functional improvement with vitamin D replenishment in a cohort of frail, vitamin D-deficient older people. J Am Geriatr Soc 43:1269-1271, 1995
Pfeifer M, Begerow B, Minne HW, et al: Effects of a short-term vitamin D and calcium supplementation on body sway and secondary hyperparathyroidism in elderly women. J Bone Miner Res 15:1113-1118, 2000
Chapuy MC, Arlot ME, Duboeuf F, et al: Vitamin D3 and calcium to prevent hip fractures in elderly women. N Engl J Med 327:1637-1642, 1992
Bischoff-Ferrari HA, Dawson-Hughes B, Staehelin HB, et al: Fall prevention with supplemental and active forms of vitamin D: A meta-analysis of randomised controlled trials. BMJ 339:b3692, 2009
Lappe JM, Travers-Gustafson D, Davies KM, et al: Vitamin D and calcium supplementation reduces cancer risk: Results of a randomized trial. Am J Clin Nutr 85:1586-1591, 2007
Hsia J, Heiss G, Ren H, et al: Calcium/vitamin D supplementation and cardiovascular events. Circulation 115:846-854, 2007
Chlebowski R, Johnson K, Kooperberg C, et al: Calcium plus vitamin D supplementation and the risk of breast cancer. J Natl Cancer Inst 100:1581-1591, 2008
Neuhouser ML, Wassertheil-Smoller S, Thomson C, et al: Multivitamin use and risk of cancer and cardiovascular disease in the Women’s Health Initiative cohorts. Arch Intern Med 169:294-304, 2009
Zadshir A, Tareen N, Pan D, et al: The prevalence of hypovitaminosis D among US adults: Data from the NHANES III. Ethn Dis 15:97-101, 2005 (suppl 5)
Yetley EA: Assessing the vitamin D status of the US population. Am J Clin Nutr 88:558S-564S, 2008
Mantell DJ, Owens PE, Bundred NJ, et al: 1 alpha,25-dihydroxyvitamin D(3) inhibits angiogenesis in vitro and in vivo. Circ Res 87:214-220, 2000
Welsh J, Wietzke JA, Zinser GM, et al: Impact of the vitamin D3 receptor on growth-regulatory pathways in mammary gland and breast cancer. J Steroid Biochem Mol Biol 83:85-92, 2002
Cheskis B, Freedman LP: Ligand modulates the conversion of DNA-bound vitamin D3 receptor (VDR) homodimers into VDR-retinoid X receptor heterodimers. Mol Cell Biol 14:3329-3338, 1994
Colston KW, Perks CM, Xie SP, et al: Growth inhibition of both MCF-7 and Hs578T human breast cancer cell lines by vitamin D analogues is associated with increased expression of insulin-like growth factor binding protein-3. J Mol Endocrinol 20:157-162, 1998
Rozen F, Yang XF, Huynh H, et al: Antiproliferative action of vitamin D-related compounds and insulin-like growth factor binding protein 5 accumulation. J Natl Cancer Inst 89:652-656, 1997
Swami S, Raghavachari N, Muller UR, et al: Vitamin D growth inhibition of breast cancer cells: Gene expression patterns assessed by cDNA microarray. Breast Cancer Res Treat 80:49-62, 2003
Verlinden L, Verstuyf A, Convents R, et al: Action of 1,25(OH)2D3 on the cell cycle genes, cyclin D1, p21 and p27 in MCF-7 cells. Mol Cell Endocrinol 142:57-65, 1998
Wu G, Fan RS, Li W, et al: Modulation of cell cycle control by vitamin D3 and its analogue, EB 1089, in human breast cancer cells. Oncogene 15:1555-1563, 1997
Campbell FC, Xu H, El-Tanani M, et al: The yin and yang of vitamin D receptor (VDR) signaling in neoplastic progression: Operational networks and tissuespecific growth control. Biochem Pharmacol 79:1-9, 2010
Nagpal S, Na S, Rathnachalam R: Noncalcemic actions of vitamin D receptor ligands. Endocr Rev 26:662-687, 2005
Aguilera O, Pen˜ a C, Garc?´a JM, et al: The Wnt antagonist DICKKOPF-1 gene is induced by 1alpha,25-dihydroxyvitamin D3 associated to the differentiation of human colon cancer cells. Carcinogenesis 28:1877-1884, 2007
Penda´ s-Franco N, Garc?´a JM, Pen˜ a C, et al: DICKKOPF-4 is induced by TCF/beta-catenin and upregulated in human colon cancer, promotes tumour cell invasion and angiogenesis and is repressed by 1alpha,25-dihydroxyvitamin D3. Oncogene 27:4467-4477, 2008
Holick MF: High prevalence of vitamin D inadequacy and implications for health. Mayo Clin Proc 81:353-373, 2006
Dawson-Hughes B, Heaney RP, Holick MF, et al: Estimates of optimal vitamin D status. Osteoporos Int 16:713-716, 2005
Institute of Medicine, Food and Nutrition Board: Dietary Reference Intakes for Calcium, Phosphorus, Magnesium, Vitamin D, and Fluoride. Washington, DC, National Academies Press, 1997
Holick MF: Vitamin D deficiency. N Engl J Med 357:266-281, 2007
Heaney RP: The vitamin D requirement in health and disease. J Steroid Biochem Mol Biol 97:13-19, 2005
Holden JM, Lemar LE, Exler J: Vitamin D in foods: Development of the US Department of Agriculture database. Am J Clin Nutr 87:1092S-1096S, 2008
US Department of Agriculture, Agricultural Research Service, 2009; USDA National Nutrient Database for Standard Reference, Release 22—Nutrient Data Laboratory. http://www.ars.usda.gov/ba/bhnrc/ndl
Heaney RP, Davies KM, Chen TC, et al: Human serum 25-hydroxycholecalciferol response to extended oral dosing with cholecalciferol. Am J Clin Nutr 77:204-210, 2003
Vieth R, Chan PC, MacFarlane GD: Efficacy and safety of vitamin D3 intake exceeding the lowest observed adverse effect level. Am J Clin Nutr 73:288-294, 2001
Vieth R: Vitamin D and cancer mini-symposium: The risk of additional vitamin D. Ann Epidemiol 19:441-445, 2009
Armas LA, Hollis BW, Heaney RP: Vitamin D2 is much less effective than vitamin D3 in humans. J Clin Endocrinol Metab 89:5387-5891, 2004
Hathcock JN, Shao A, Vieth R, et al: Risk assessment for vitamin D. Am J Clin Nutr 85:6-18, 2007
Holick MF: Optimal vitamin D status for the prevention and treatment of osteoporosis. Drugs Aging 24:1017-1029, 2007
Chapuy MC, Preziosi P, Maaner M, et al: Prevalence of vitamin D insufficiency in an adult normal population. Osteoporosis Int 7:439-443, 1997
Heaney RP, Dowell MS, Hale CA, et al: Calcium absorption varies within the reference range for serum 25-hydroxyvitamin D. J Am Coll Nutr 22:142-146, 2003
Crew KD, Shane E, Cremers S, et al: High prevalence of vitamin D deficiency despite supplementation in premenopausal women with breast cancer undergoing adjuvant chemotherapy. J Clin Oncol 27:2151-2156, 2009
Fabian CJ, Kimler BF, Phillips T, et al: Levels of 25-hydroxy-vitamin D in pre-menopausal women at high risk for development of breast cancer. Cancer Res 69:5079, 2009 (suppl 2)
Caniggia A, Lore` F, di Cairano G, et al: Main endocrine modulators of vitamin D hydroxylases in human pathophysiology. J Steroid Biochem 27:815-824, 1987
Gilad LA, Bresler T, Gnainsky J, et al: Regulation of vitamin D receptor expression via estrogen-induced activation of the ERK 1/2 signaling pathway in colon and breast cancer cells. J Endocrinol 185:577-592, 2005
Clemens TL, Adams JS, Henderson SL, et al: Increased skin pigment reduces the capacity of skin to synthesize vitamin D3. Lancet 1:74-76, 1982
Worstman J, Matsuoka LY, Chen TC, et al: Decreased bioavailability of vitamin in obesity. Am J Clin Nutr 72:690-693, 2000
Matsuoka LY, Ide L, Wortsman J, et al: Sunscreens suppress cutaneous vitamin D3 synthesis. J Clin Clin Endocrinol Metab 64:1165-1168, 1987
Webb AR, Kline L, Holick MF: Influence of season and latitude on the cutaneous synthesis of vitamin D3: Exposure to winter sunlight in Boston and Edmonton will not promote vitamin D3 synthesis in human skin. J Clin Endocrinol Metab 67:373-378, 1988
Matsuoka LY, Wortsman J, Dannenberg MJ, et al: Clothing prevents ultraviolet-B radiation-dependent photosynthesis of vitamin D3. J Clin Endocrinol Metab 75:1099-1103, 1992
Agarwal KS, Mughal MZ, Upadhyay P, et al: The impact of atmospheric pollution on vitamin D status of infants and toddlers in Delhi, India. Arch Dis Child 87:111-113, 2002
Glerup H, Mikkelsen K, Poulsen L, et al: Hypovitaminosis D myopathy without biochemical signs of osteomalacic bone involvement. Calcif Tissue Int 66:419-424, 2000
Plotnikoff GA, Quigley JM: Prevalence of severe hypovitaminosis D in patients with persistent, nonspecific musculoskeletal pain. Mayo Clin Proc 78:1463-1470,2003
Khan QJ, Reddy PS, Kimler BF, et al: Effect of vitamin D supplementation on serum 25-hydroxy vitamin D levels, joint pain, and fatigue in women starting adjuvant letrozole treatment for breast cancer. Breast Cancer Res Treat 119:111-118, 2010
Lee P, Greenfield JR, Seibel MJ, et al: Adequacy of vitamin D replacement in severe deficiency is dependent on body mass index. Am J Med 122:1056-1060,2009
Nilsson IL, Zedenius J, Yin L, et al: The association between primary hyperparathyroidism and malignancy: Nationwide cohort analysis on cancer incidence after parathyroidectomy. Endocr Relat Cancer 14:135-140, 2007
Fabian CJ: If vitamin D prevents breast cancer, how does it do it, and how much does it take? Am Soc Clin Oncol Ed Book 71-74, 2009
