Deaths after Cancer Surgery higher in blacks (probably low vitamin D)
Changes in Racial Disparities in Mortality After Cancer Surgery in the US, 2007-2016
JAMA Netw Open. 2020;3(12):e2027415. doi:10.1001/jamanetworkopen.2020.27415
Miranda B. Lam, MD, MBA1,2; Katherine Raphael, BA1; Winta T. Mehtsun, MD, MPH1,3; et alJessica Phelan, MA1; E. John Orav, PhD4,5; Ashish K. Jha, MD, MPH1,4; Jose F. Figueroa, MD, MPH1,6
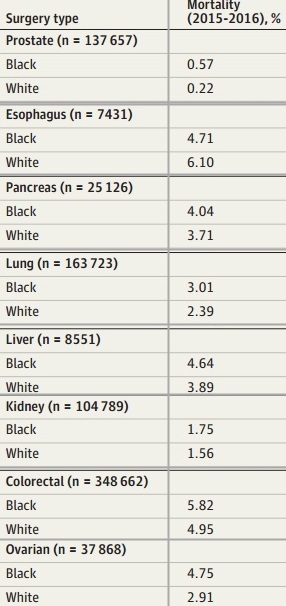
subset of table
📄 Download the PDF from VitaminDWiki
Importance Racial disparities are well documented in cancer care. Overall, in the US, Black patients historically have higher rates of mortality after surgery than White patients. However, it is unknown whether racial disparities in mortality after cancer surgery have changed over time.
Objective To examine whether and how disparities in mortality after cancer surgery have changed over 10 years for Black and White patients overall and for 9 specific cancers.
Design, Setting, and Participants In this cross-sectional study, national Medicare data were used to examine the 10-year (January 1, 2007, to November 30, 2016) changes in postoperative mortality rates in Black and White patients. Data analysis was performed from August 6 to December 31, 2019. Participants included fee-for-service beneficiaries enrolled in Medicare Part A who had a major surgical resection for 9 common types of cancer surgery: colorectal, bladder, esophageal, kidney, liver, ovarian, pancreatic, lung, or prostate cancer.
Exposures Cancer surgery among Black and White patients.
Main Outcomes and Measures Risk-adjusted 30-day, all-cause, postoperative mortality overall and for 9 specific types of cancer surgery.
Results A total of 870 929 cancer operations were performed during the 10-year study period. In the baseline year, a total of 103 446 patients had cancer operations (96 210 White patients and 7236 Black patients). Black patients were slightly younger (mean [SD] age, 73.0 [6.4] vs 74.5 [6.8] years), and there were fewer Black vs White men (3986 [55.1%] vs 55 527 [57.7%]). Overall national mortality rates following cancer surgery were lower for both Black (−0.12%; 95% CI, −0.17% to −0.06% per year) and White (−0.14%; 95% CI, −0.16% to −0.13% per year) patients. These reductions were predominantly attributable to within-hospital mortality improvements (Black patients: 0.10% annually; 95% CI, −0.15% to −0.05%; P < .001; White patients: 0.13%; 95% CI, −0.14% to −0.11%; P < .001) vs between-hospital mortality improvements. Across the 9 different cancer surgery procedures, there was no significant difference in mortality changes between Black and White patients during the period under study (eg, prostate cancer: 0.35; 95% CI, 0.02-0.68; lung cancer: 0.61; 95% CI, −0.21 to 1.44).
Conclusions and Relevance These findings offer mixed news for policy makers regarding possible reductions in racial disparities following cancer surgery. Although postoperative cancer surgery mortality rates improved for both Black and White patients, there did not appear to be any narrowing of the mortality gap between Black and White patients overall or across individual cancer surgery procedures.
