Vitamin D blood levels of Canadians
by Teresa Janz and Caryn Pearson Health Statistics Division, January 2013
PDF is attached at the bottom of this page
Highlights
Just over two-thirds of Canadians (68%) had blood concentrations of vitamin D over 50 nmol/L—a level that is sufficient for healthy bones for most people. About 32% of Canadians were below the cut-off.
Children aged 3 to 5 had the highest rates above the cut-off (89%), while the 20- to 39-year-olds had the lowest (59%).
A minority of Canadians (34%) took a supplement containing vitamin D, but a larger percentage of those taking supplements were above the cut-off (85%), compared with non-supplement users (59%).
About 40% of Canadians were below the cut-off in winter, compared with 25% in the summer.
On average, females had a higher concentration of vitamin D in their blood than males.
Vitamin D plays an important role in bone growth and maintenance because it helps the body absorb calcium and phosphorus.12 In children, low levels of vitamin D can cause rickets, a condition characterized by soft bones and skeletal deformities. In adults, low levels of vitamin D can lead to osteoporosis (decreased bone mass), which also increases the risk of fractures. Some research suggests that adequate vitamin D may have benefits, such as lowering the risk of breast and colorectal cancer3,4, cardiovascular disease in men5, and multiple sclerosis.6 However, the research supporting the benefits of vitamin D, other than for bone health, is still inconclusive.7
This article explores factors associated with vitamin D blood levels, using data from Cycle 2 of the Canadian Health Measures Survey (CHMS). In particular, it examines how vitamin D levels differ depending on one's age, sex, supplement use, milk consumption, season of sun exposure, and body mass index (BMI).
- Cycle 2 Data for the Canadian Health Measures Survey (CHMS) were collected from August 2009 to November 2011.
- This survey collects direct physical measures of health (e.g., blood) and asks questions about health from the Canadian population aged 3 to 79.
The CHMS collected blood samples from Canadians that measured the plasma 25-hydroxyvitamin D [25(OH)D] concentrations in nanomoles per litre (nmol/L) that reflect the number of molecules per litre of blood. The concentration of 25(OH)D reflects vitamin D levels in the blood from food, supplements, and sun exposure.7
What does this mean for bone health?
The following categories describe the amount of vitamin D in the blood relative to bone health, as suggested by the Institute of Medicine (IOM).
The categories were developed through a comprehensive review of scientific studies.7
- Above vitamin D cut-off: refers to those who have vitamin D blood levels at or above 50 nmol/L.
- Most Canadians are considered to have sufficient levels of vitamin D for bone health at this level.
- This is compatible with vitamin D intakes that meet the Recommended Dietary Allowance.7
- Below vitamin D cut-off: refers to those who have vitamin D blood levels lower than 50 nmol\L.
- Some, but not all, people with vitamin D blood levels between 30 and 50 nmol/L are potentially at risk of inadequacy relative to bone health.
- Canadians who are classified as 'deficient' (who have blood levels below 30 nmol/L) are also included in this cut-off.
- Deficiency: refers to those with vitamin D blood levels below 30 nmol/L. Canadians may be at risk of deficiency relative to bone health below this level.
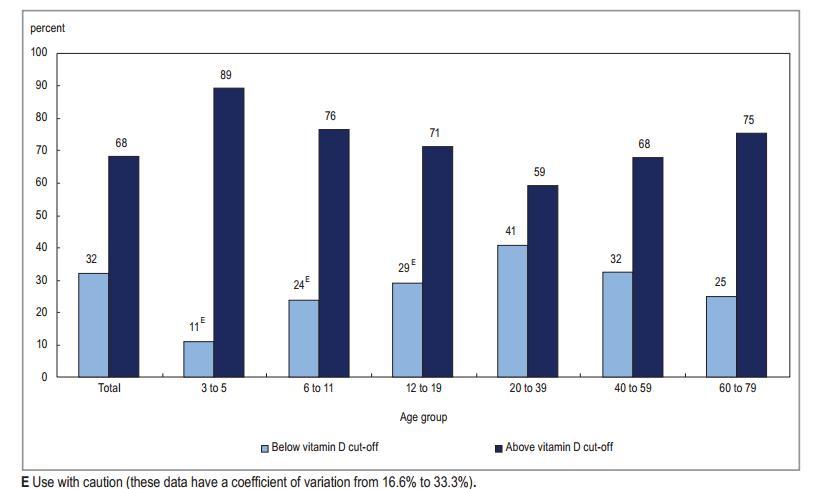
Just over two-thirds of Canadians (68%) had vitamin D blood levels above the cut-off, according to Cycle 2 data from the CHMS (Chart 1). Conversely, about one third (32%) had concentrations of vitamin D below the cut-off, this rate also includes those who were vitamin D deficient- - 10%14 of Canadians were deficient.
The percentage of Canadians above the vitamin D cut-off across all age groups resembles a U-shape—highest among young children and seniors and lowest for ages 20 to 39 (Chart 1). The youngest children (aged 3 to 5) had the highest rates above the cut-off (89%), while the 20- to 39-year-olds had the lowest (59%).
Beyond examining a single cut-off, variations in average blood levels by age and sex provide more information about who is getting enough vitamin D.
The youngest and oldest age groups had levels of vitamin D that were notably higher than the national average of 64 nmol/L. The average level of vitamin D for 3- to 5-year olds was 74 nmol/L, while the average was 67 nmol/L for those aged 6 to 11, and 70 nmol/L for 60- to 79-year-olds.
Overall, the average blood level for females (67 nmol/L) was higher than males (61 nmol/L). The largest sex differences were seen among children aged 6 to 11 and adults aged 20 to 39. Among children aged 6 to 11, males had higher average blood levels of vitamin D (72 nmol/L) than females (63 nmol/L). This was the only age group where males had higher levels than females. The average vitamin D blood level for males aged 20 to 39 was 55 nmol/L, while it was 66 nmol/L for females—a sex difference of 11 nmol/L.
Chart 1 Percentage of Canadians > and < 50nmol/L, by age group
What else may be linked with higher blood levels of vitamin D?
The age and sex differences in blood levels of vitamin D may, to some extent, be related to how people in these groups obtain their vitamin D. For example, people can obtain vitamin D naturally from a few foods, including egg yolks and fatty fish such as mackerel or salmon.
The focus of the remainder of the article will be on other sources of vitamin D. Specifically, attention will be given to supplement use, milk consumption and sun exposure- - and how they may be related to vitamin D blood levels. A possible link between body mass index (BMI) and vitamin D is also explored.
Supplement use
Vitamin D supplements are recommended for people over the age of 50 given that the body's ability to produce vitamin D from sun exposure declines with age.8 Supplements are also recommended for breast-fed infants as a preventative measure against rickets.1 Previous research shows that those who do not take vitamin D supplements have double the rate of vitamin D deficiency than those who take supplements.8
10
According to CHMS Cycle 2 data, 34% of Canadians took a supplement containing vitamin D within the month before they were surveyed. Supplements include any prescription or over-the-counter medication, herbal product, botantical oil, vitamin or mineral that contain vitamin D. More females (41%) took supplements than males (28%). In terms of age, supplement intake was highest among 3- to 5-year-olds and 40- to 79-year-olds; and lowest among those aged 12 to 39.
Overall, a higher percentage of Canadians who took supplements containing vitamin D had blood concentrations above the cut-off (85%) compared to those who did not take supplements with vitamin D (59%).
Among supplement users, young children aged 3 to 5 (97%) and older Canadians aged 60 to 79 (93%), had the highest rates above the cutoff compared with the national average (85%). Of any age group taking supplements, 20- to 39-year-olds had the smallest percentage above the cut-off at 75%.
Cycle 2 data from the CHMS shows a relationship between diagnosis of osteoporosis and vitamin D. Females aged 50 and older with osteoporosis had higher levels of vitamin D (82 nmol/L) than those without osteoporosis (68 nmol/L). This may be because a recommended treatment for osteoporosis is to increase the intake of vitamin D and calcium, typically by taking supplements.9 In Cycle 2, 70% of those diagnosed with osteoporosis reported taking supplements with vitamin D.
Osteoporosis and vitamin D
Osteoporosis is a disease leading to a loss of bone mass accompanied by increased risk of bone fragility and fracture.9 The condition primarily affects older people, mainly women.
Past research10 shows that 19% of women and 3% of men over 50 reported being diagnosed with osteoporosis by a health professional. Rates were higher with age—of those 71 or older, 31% of women and 6% of men had been diagnosed.
Canadians who reported a diagnosis of osteoporosis were more likely to be taking supplements than those not diagnosed. Among those aged 50 and older 27% of men and 44% of women took vitamin D supplements at least once in the previous month. However, among those diagnosed with osteoporosis, 38% of men and 57% of women took vitamin D supplements. 10
Milk consumption
Adding vitamin D to cow's milk and margarine is mandatory in Canada as a preventative measure against rickets, osteomalacia, and osteoporosis.11 It is also added to some foods such as: goat's milk, fortified plant-based beverages (such as fortified soy beverages), and calcium-fortified orange juice.1
According to Cycle 2 of the CHMS, 75% of those who consumed milk once or more a day had levels of vitamin D above the cut-off, compared with 60% of those who had milk less than once a day.
Chart 2 Average vitamin D blood levels, by milk consumption, by age group
Those who consumed milk once or more a day also had a higher average vitamin D level (68 nmol/L) than Canadians who consumed milk less than once a day (59 nmol/L). Of those who consumed milk once or more a day, 3- to 5-year-olds and 60- to 79-year-olds had the highest average vitamin D levels of all age groups (Chart 2). These two groups also had high rates of supplement use.
Sun exposure
Vitamin D is unique because it can be made by the body through exposure to sunlight while most vitamins need to be ingested. That is why it is commonly known as the 'sunshine vitamin.’
The body's ability to produce vitamin D is affected by factors such as latitude (distance from the sun), season, time of day, cloud cover, smog, clothing coverage, and sunscreen use. Skin pigmentation is also linked to vitamin D levels. Melanin in the skin evolved as an effective natural sunscreen. Those with darker skin pigment, or more melanin, have more difficulty producing vitamin D from the sun.2
The body's ability to produce vitamin D from the sun also declines with age. For example, a person aged 70 makes, on average, 25% of the vitamin D that a 20-year-old makes when exposed to the same amount of sunlight.2
Chart 3 Percentage of Canadians at selected vitamin D levels, by season
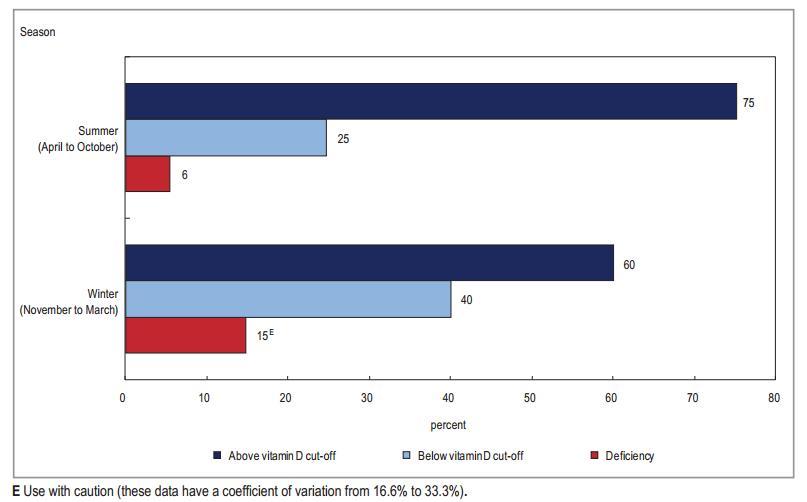
Geography is also a factor—during the winter months in Canada and other countries in the northern hemisphere, there are fewer ultraviolet B (UVB) photons reaching the earth. This means that very little, if any, vitamin D is produced by the body in the winter.2 According to CHMS Cycle 2 data, 40% of Canadians had concentrations of vitamin D below the cutoff in winter, compared with 25% in summer
(Chart 3).
Body mass index
Similar to previous research,12 Cycle 2 of the CHMS suggests a link between body mass index (BMI) and vitamin D. Children and adults who were overweight or obese generally had lower average vitamin D blood levels than those who were normal or underweight.
Body mass index (BMI) is the ratio of a person's weight, in kilograms, by their height in meters squared (kg/m2). It is useful for classifying body weight and identifying obesity. Adult BMI ranges are different than those for children and adolescents to account for growth-rate variations among youth.13
According to Cycle 2 data, 69% of Canadian children and adolescents—aged 5 to 17—were normal weight or thin, and 31% were overweight or obese. Among adults, about 40% were normal or underweight; 34% were overweight and 26% were obese.
Vitamin D blood levels for obese adults were significantly lower than overweight and normal/underweight adults (Chart 4). However, there were no notable differences between the overweight and normal/ underweight adults. One exception was found in the 18 to 39 age group. For this age group, there were no significant differences in average vitamin D blood levels across any of the three BMI categories.
Chart 4 Average vitamin D levels of adults, by age group and body mass index category
Children aged 5 to 11 and adolescents aged 12 to 17 who were thin or normal weight had significantly higher average vitamin D levels (67 nmol/L) than those who were overweight or obese (61 nmol/L). Despite lower average vitamin D blood levels, 68% of overweight or obese youth still have vitamin D levels above the cut-off.
Summary
According to measurements taken during Cycle 2 of the CHMS from 2009 to 2011, most Canadians had levels of vitamin D at or above 50 nmol/L, a level sufficient for healthy bones for most people. In particular, children aged 3 to 11, and seniors aged 60 to 79 had blood concentrations of vitamin D higher than the national average. Furthermore, despite a reduced likelihood of vitamin D production year-round, Canadians generally had levels of vitamin D in their blood above the cut-off.
Teresa Janz and Caryn Pearson are analysts with the Health Statistics Division.
References
Health Canada. Vitamin D and Calcium: Updated Dietary Reference Intakes. March 22, 2012. Available at: http://www.hc-sc.gc.ca/fn-an/ nutrition/vitamin/vita-d-eng.php. Accessed July 30, 2013.
Holick M. Sunlight and vitamin D for bone health and prevention of autoimmune diseases, cancers and cardiovascular disease. Am J Clin Nutr. 2004;80(suppl):1678S-1688S.
Lin J, Manson J, Lee IM, et al. Intakes of calcium and vitamin D and breast cancer risk in women. Archives of International Medicine. 2007;167(10):1050-1059.
Gorham E, Garland C, Garland F, et al. Optimal vitamin D status for colorectal cancer prevention: a quantitative meta analysis. American Journal of Preventative Medicine. 2007;32(3):210-216.
Giovannucci E, Liu Y, Hollis B. 25-Hydroxyvitamin D and risk of myocardinal infarction in men: a prospective study. Archives of Internal Medicine. 2008;168(11):1174-1180.
Ramagopalan S, Maugeri N, Handunnetthi L, et al. Expression of the multiple sclerosis-assoicated MGC class ll allele HLA-DRB1*1501 is regulated by vitamin D. PLoS Genetics. 2009;5(2).
Dietary reference intakes for calcium and vitamin D. Washington, DC: Institute of Medicine; 2010.
Whiting S, Langlois K, Vatanparast H, et al. The vitamin D status of Canadians relative to the 2011 dietary reference intakes: an examination in children and adults with and without supplement use. Am J Clin Nutr. 2011;94(1):128-135.
Rizzoli R, Boonen S, Brandi M, et al. The role of calcium and vitamin D in the management of osteoporosis. Bone. 2008; 42:246-249.
Garriguet D. Bone health: Osteoporosis, calcium and vitamin D. Health Reports. September 2011;22(3):1-8.
Canadian Food Inspection Agency. "Chapter 9 vitamin addition," Dairy products inspection manual. 2012. Available at: http://www.inspection.gc.ca/ english/fssa/dailai/man/proman/ch9e.shtml. Accessed August 13, 2012.
McGill A, Stewart J, Lithander F, et al. Relationships of low serum vitamin D3 with anthropometry and markers of the metabolic syndrome and diabetes in overweight and obesity. Nutrition Journal. 2008;7(4).
Roberts K, Shields M, Groh M, et al. Overweight and obesity in children and adolescents: Results from the 2009 to 2011 Canadian Health Measures Survey. Health Reports. September 2012; 23(3):3-6.
This statistic should be used with caution (this data has a coefficient of variation from 16.6% to 33.3%).
See also VitaminDWiki
Canada and Vitamin D items
Half of Quebec kids had less than 20 ng of vitamin D – Milk and movement did not help – Mar 2011
90 percent of Canadian youth less than 30 ng vitamin D – Oct 2010
Many vitamin D articles and videos by Schwalfenberg in Canada
90 % of Swiss men have less than 30 ng of vitamin D in the winter – Nov 2012
90 % of young health care professionals had less than 30 ng of vitamin D – Nov 2011
87 % of Tennessee general medicine patients had less than 32 ng of vitamin D – Jan 2011
82 % of Swedes did not have the recommended amount of vitamin D – Feb 2011
Vitamin D is the most common nutritional deficiency worldwide – Best Practice BMJ Dec 2012
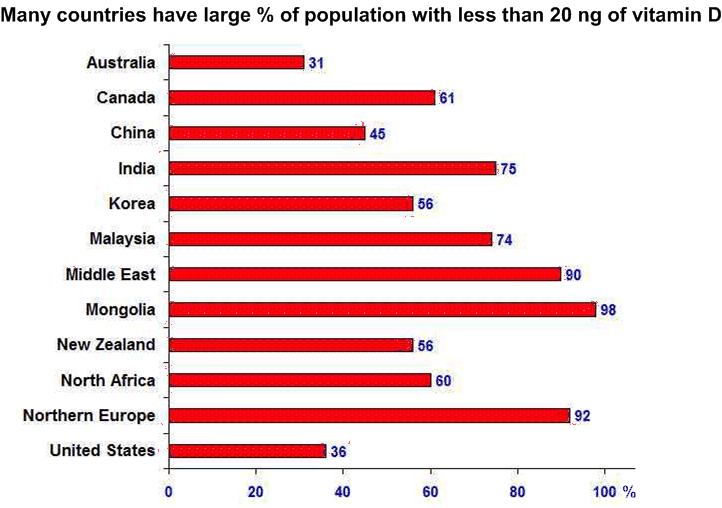
Vitamin D levels in healthy populations around the globe – Aug 2012 which has the following chart