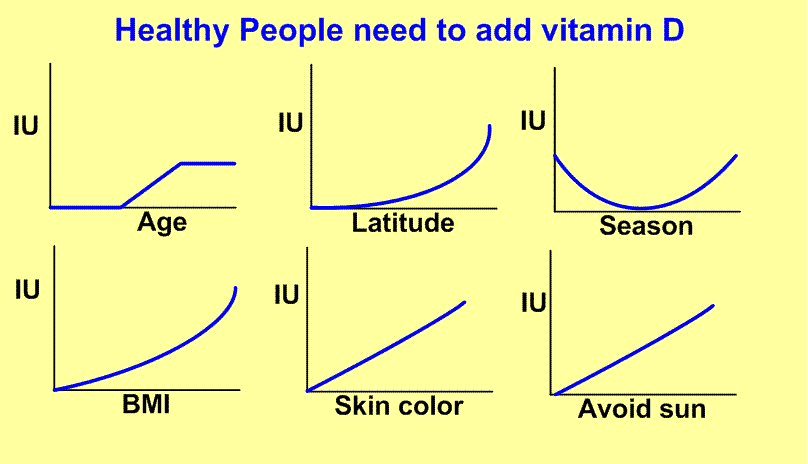
Response to Vitamin D supplementation
Factors Affecting 25-Hydroxyvitamin D Concentration in Response to Vitamin D Supplementation
Nutrients 2015, 7(7), 5111-5142; doi:10.3390/nu7075111
Hajar Mazahery and Pamela R. von Hurst P.R.vonHurst@massey.ac.nz
Institute of Food Science and Technology-School of Food and Nutrition, Massey University,
Auckland 0632, New Zealand; E-Mail: h.mazahery@hotmail.com
Sun exposure is the main source of vitamin D. Due to many lifestyle risk factors vitamin D deficiency/insufficiency is becoming a worldwide health problem. Low 25(OH)D concentration is associated with adverse musculoskeletal and non-musculoskeletal health outcomes. Vitamin D supplementation is currently the best approach to treat deficiency and to maintain adequacy. In response to a given dose of vitamin D, the effect on 25(OH)D concentration differs between individuals, and it is imperative that factors affecting this response be identified. For this review, a comprehensive literature search was conducted to identify those factors and to explore their significance in relation to circulating 25(OH)D response to vitamin D supplementation. The effect of several demographic/biological factors such as baseline 25(OH)D, aging, body mass index(BMI)/body fat percentage, ethnicity, calcium intake, genetics, oestrogen use, dietary fat content and composition, and some diseases and medications has been addressed. Furthermore, strategies employed by researchers or health care providers (type, dose and duration of vitamin D supplementation) and environment (season) are other contributing factors. With the exception of baseline 25(OH)D, BMI/body fat percentage, dose and type of vitamin D, the relative importance of other factors and the mechanisms by which these factors may affect the response remains to be determined.
Sections of PDF
Basal 25(OH)D Concentration
BMI or Body Fat Percentage
Aging
Ethnicity
Dietary Calcium Intake
Genetic Background
Oestrogen Use
Dietary Fat Content and Fat Composition
Diseases and Medications
Type of Vitamin D; D3 vs. D2
Dosing Regimen: Dose, Duration
Season
Conclusions (extracted from PDF)
The relationship between 25(OH)D concentration and vitamin D supplementation is not straightforward and is influenced by a large number of factors. Some of these factors such as basal 25(OH)D concentration are well documented. Evidence is emerging for others such as BMI/body fat% and season, while for calcium intake, dietary fat content and composition, and genetics the evidence is either mixed or in its infancy. The mechanisms by which these factors may affect the response are not well understood. Accordingly, there is an urgent need for more well-designed studies:
(1) to establish the significance of these factors;
(2) to identify other unknown factors;
(3) to determine the mechanistic pathways by which these factors may exert their roles and
(4) to strengthen our knowledge and understanding to inform the dose of supplementation required.
It should be noted that increasing 25(OH)D concentration alone is not meaningful if it is not accompanied by improved clinical outcomes, or at least biomarkers. Clinical trials investigating the impact of improving vitamin D status on various health and disease outcomes are also warranted. Finally, chronic diseases are multifactorial in origin and many variables that contribute to the development of these diseases, such as unhealthy dietary habits, aging and physical inactivity, are risk factors for vitamin D deficiency [109]. Therefore even if widespread vitamin D status is optimized, various chronic diseases will continue to occur, but the risk will be lower.
One of many tables in the PDF

📄 Download the PDF from VitaminDWiki
See also VitaminDWiki
Reasons for low response to vitamin D
- has the following chart, and a long table - which has many more reason than in this study