Poor Bladder Cancer survival associated with poor Vitamin D receptor
Expression of Vitamin D Receptor (VDR) Positively Correlates with Survival of Urothelial Bladder Cancer Patients
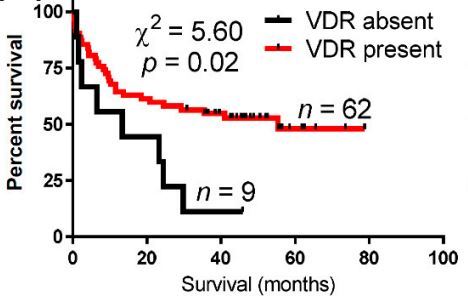
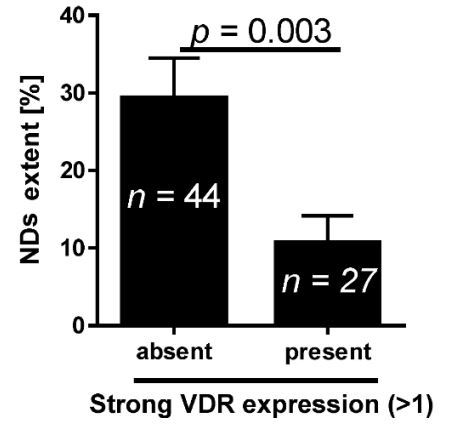
NDs = Non–classic differentiations
Int. J. Mol. Sci. 2015, 16, 24369-24386; doi:10.3390/ijms161024369
Wojciech Jóźwicki 1,2, jozwickiw@co.bydgoszcz.pl;, Anna A. Brożyna 1,2, Jerzy Siekiera 3 and Andrzej T. Slominski 4,5
Department of Tumour Pathology and Pathomorphology, Nicolaus Copernicus University Collegium Medicum in Bydgoszcz, Bydgoszcz 85-796, Poland; E-Mail: anna.brozyna@cm.umk.pl
Department of Tumour Pathology and Pathomorphology, Oncology Centre-Prof. Franciszek Lukaszczyk Memorial Hospital, Bydgoszcz 85-796, Poland
Department of Urology, Oncology Centre-Prof. Franciszek Lukaszczyk Memorial Hospital, Bydgoszcz 85-796, Poland; E-Mail: siekieraj@co.bydgoszcz.pl
Departments of Dermatology and Pathology, University of Alabama at Birmingham, Birmingham, AL 35294, USA; E-Mail: aslominski@uabmc.edu
Department of Veteran Affairs (VA) Medical Center, Birmingham, AL 35294, USA
📄 Download the PDF from VitaminDWiki
Vitamin D3 shows tumoristatic and anticancer effects by acting through the vitamin D receptor (VDR), while hydroxylation of 25-hydroxyvitamin D3 at position 1a by CYP27B1 is an essential step in its activation. The expression of both the VDR and CYP27B1 has been found in many normal and cancer tissues, but there is a lack of information about its expression in human bladder cancers. The aim of the present research was to examine whether the expression of the VDR and CYP27B1 in bladder cancer was related to the prognostic markers and disease outcome. We analyzed VDR and CYP27B1 in samples of tumor and normal tissues obtained from 71 urinary bladder cancer patients. The highest VDR immunostaining was found in normal epithelium and was significantly lower in bladder cancer cells (p < 0.001 with Mann-Whitney Utest). VDR expression was lowest in more advanced (pT2b-pT4) (p = 0.005 with Mann-Whitney U test) and metastasizing cancers (p < 0.05 and p = 0.004 with Mann-Whitney U test for nuclear and cytoplasmic VDR immunostaining, respectively). The lack of cytoplasmic and nuclear VDR was also related to shorter overall survival (for cytoplasmic VDR immunolocalization 13.3 vs. 55.3 months of survival, HR = 1.92,p = 0.04 and for nuclear VDR immunostaining 13.5 vs. 55.3 months of survival, HR = 2.47, p = 0.002 with Mantel-Cox test). In cases with the lack of high cytoplasmic VDR staining the non-classic differentiations (NDs) was observed in higher percentage of tumor area. CYP27B1 expression was lower in cancer cells than in normal epithelial cells (p = 0.03 with Mann-Whitney U test), but its expression did not correlate with tumor stage (pT), metastasizing, grade, mitotic activity or overall survival. In conclusion, expression of the VDR and CYP27B1 are deregulated in urothelial bladder cancers. Although our results showing a relationship between the decreased VDR expression and prognostic markers and survival time indicate potential usefulness of VDR as a new indicator of a poorer prognosis, further studies are needed in different patient cohorts by independent groups to validate this hypothesis. We also suggest that vitamin D-based therapies may represent an adjuvant strategy in treatment for bladder cancers expressing VDR.
Conclusions (from PDF)
In summary, VDR and CYP27B1 expression was down-regulated in urothelial bladder cancers in comparison to normal tissue. There was a strong relationship between VDR expression and the biology and stage of bladder cancers, with a lack of such correlation for CYP27B1. Urothelial bladder cancer progression and decrease of overall survival were linked with a reduction in VDR expression. These results have potential clinical implications in that a decreased VDR expression may predict a poorer prognosis, as demonstrated by the lower overall survival in our study. VDR expression can also be a potential prognostic marker in urothelial bladder cancer patients. The lack of correlation between VDR expression and some histological markers of malignancy such as mitotic activity and tumor grade and lack of correlation with CYP27B1 indicate a more complex role of the VDR signaling in the biology of bladder cancer that may include involvement of the new vitamin metabolites activating alternative pathways. The differences in VDR expression in bladder cancer suggest that vitamin D-based therapies may represent a promising previously unexplored strategies of bladder cancer treatment.
