Parkinsons' disease and MRI white matter in brain
White matter hyperintensities in Parkinson's disease: do they explain the disparity between the postural instability gait difficulty and tremor dominant subtypes? Jan 2013
PLoS One. 2013;8(1):e55193. doi: 10.1371/journal.pone.0055193. Epub 2013 Jan 31.
Herman T, Rosenberg-Katz K, Jacob Y, Auriel E, Gurevich T, Giladi N, Hausdorff JM.
BACKGROUND:
Brain white matter hyperintensities (WMHs) commonly observed on brain imaging of older adults are associated with balance and gait impairment and have also been linked to cognitive deficits. Parkinson's disease (PD) is traditionally sub-classified into the postural instability gait difficulty (PIGD) sub-type, and the tremor dominant (TD) sub-type. Considering the known association between WMHs and axial symptoms like gait disturbances and postural instability, one can hypothesize that WMHs might contribute to the disparate clinical sub-types of patients with PD.
METHODS:
110 patients with PD underwent a clinical evaluation and a 3T MRI exam. Based on the Unified Parkinson Disease Rating Scale, the patients were classified into motor sub-types, i.e., TD or PIGD, and scores reflecting PIGD and TD symptoms were computed. We compared white matter burden using three previously validated methods: one using a semi-quantitative visual rating scale in specific brain regions and two automated methods.
RESULTS:
Overall, MRI data were obtained in 104 patients. The mean WMHs scores and the percent of subjects with lesions in specific brain regions were similar in the two subtypes, p = 0.678. The PIGD and the TD scores did not differ even when comparing patients with a relatively high burden of WMHs to patients with a relatively low burden. Across most of the brain regions, mild to moderate correlations between WMHs and age were found (r = 0.23 to 0.41; p<0.021). Conversely, no significant correlations were found between WMHs and the PIGD score or disease duration. In addition, depressive symptoms and cerebro-vascular risk factors were similar among the two subtypes.
CONCLUSIONS:
In contrast to what has been reported previously among older adults, the present study could not demonstrate any association between WMHs and the PIGD or TD motor sub-types in patients with PD.
PMID: 23383104
PDF is attached at the bottom of this page
Cerebral white matter hyperintensity in Parkinson's disease: a major risk factor for mild cognitive impairment. - July 2013
Parkinsonism Relat Disord. 2013 Jul;19(7):680-3. doi: 10.1016/j.parkreldis.2013.03.008. Epub 2013 Apr 24.
Kandiah N, Mak E, Ng A, Huang S, Au WL, Sitoh YY, Tan LC.
Author information
BACKGROUND:
Mild cognitive impairment (MCI) and dementia contribute to a poor quality of life among patients with PD. The influence of cerebral ischemia as a risk factor for MCI in PD has not been adequately investigated. To address this issue, we examined the influence of the volume and distribution of white matter hyperintensity (WMH) as a risk factor for MCI in early PD.
METHODS:
Prospective study of patients with early idiopathic PD. All patients had baseline MRI-FLAIR, clinical assessment and detailed neuropsychological evaluation. Data on demographics, vascular risk factors, cognitive performance and WMH volumes were analyzed.
RESULTS:
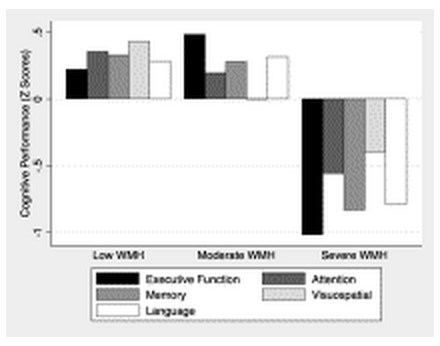
91 patients; mean age 64.9 years, mean education of 10.5 years. 24 patients fulfilled the Movement Disorder Society criteria for MCI and were classified as PD-MCI while the rest were classified as PD with no cognitive impairment (PD-NCI). Patients with PD-MCI and PD-NCI did not differ in Hoehn & Yahr staging. PD-MCI patients had a higher prevalence of diabetes mellitus, hypertension and hyperlipidemia. PD-MCI patients had significantly greater volume of periventricular (6.04 ml vs. 2.66 ml, p = 0.001) and deep subcortical WMH (2.16 vs.1.44, p = 0.002). Regional WMH was significantly greater among PD-MCI in the frontal, parietal and occipital regions. Logistic regression analyses demonstrated WMH to be associated with PD-MCI independent of age, education, and vascular risk factors. Increasing WMH volume was associated with lower performance on executive function, memory and language.
CONCLUSIONS:
WMH is an important risk factor for PD-MCI independent of vascular risk factors. PD patients with WMH should be regularly screened for MCI.
Copyright © 2013 Elsevier Ltd. All rights reserved.
PMID: 23623194
White Matter Hyperintensities Successfully Differentiate Parkinson's Disease Patients with and without Cognitive Impairment Feb 2013
P06 Non-Alzheimer's Disease Neuroimaging Neurology February 12, 2013; 80(Meeting Abstracts 1): P06.050
Jennifer Goldman1, John Ebersole2, Bryan Bernard3, Bichun Ouyang4, Christopher Goetz5, Leyla DeToledo-Morrell6 and Glenn Stebbins7
1 Neurological Sciences Rush University Medical Center Chicago IL
2 Internal Medicine St. Francis Hospital Evanston IL
3 Neurological Sciences Rush University Medical Center Chicago IL
4 Neurological Sciences Rush University Medical Center Chicago IL
5 Neurological Sciences Rush University Medical Center Chicago IL
6 Neurological Sciences Rush University Medical Center Chicago IL
7 Neurological Sciences Rush University Medical Center Chicago IL
OBJECTIVE: To examine the relationship of white matter hyperintensities (WMH) and cognitive impairment in Parkinson's Disease (PD).
BACKGROUND: Cerebral WMH detected on magnetic resonance imaging (MRI) brain scans are associated with cognitive impairment in the elderly and in Alzheimer's disease. Less is known, however, about the contributions of WMH to PD mild cognitive impairment (PD-MCI) and PD dementia (PDD).
DESIGN/METHODS: 98 PD subjects underwent clinical and neuropsychological evaluations and MRI brain scans (1.5T GE Signa). A blinded rater measured WMH on FLAIR sequences using the Scheltens scale. Subjects were classified as cognitively normal (PD-NC), PD-MCI, or PDD using published Movement Disorder Society criteria for PD-MCI and PDD.
RESULTS: PD-NC (n=29), PD-MCI (n=44), and PDD (n=25) subjects did not differ in age, education, or vascular risk factors. Demented subjects had significantly longer PD duration and worse motor function. Total WMH scores differed among the cognitive groups (p=0.01) with significantly greater WMH burden in PDD compared to PD-NC subjects. Cerebral localization of WMH differed among the cognitive groups, with respect to periventricular and deep WMH (p=0.005 and p=0.03, respectively) but not basal ganglia or infratentorial regions. Periventricular WMH load was greatest in PDD, followed by PD-MCI, and least in PD-NC subjects, thereby differentiating PDD from PD-NC subjects (p=0.01) and PD-MCI from PD-NC subjects (p=0.02). Additionally, deep WMH were significantly greater in PDD compared to PD-NC subjects (p=0.02). Specifically, deep WMH located in the parietal lobe, differed among the cognitive groups (p=0.01), whereas other lobar regions did not. Moreover, the parietal lobe WMH distinguished PDD from PD-NC subjects (p=0.01) and PD-MCI from PD-NC subjects (p=0.02).
CONCLUSIONS: Increased WMH burden in PD is associated with worse cognitive status, regardless of age or vascular risk factors. Periventricular and deep WMH, especially in the parietal lobe, differentiate the cognitive groups, and thus, may serve as markers of cognitive decline in PD.
Supported by: K23NS060949, Parkinson's Disease Foundation.
