Pancreatic cancer risk of death reduced 19 percent by Vitamin D – meta-analysis
20% less likely to survive Pancreatic Cancer if poor Vitamin D Receptor - Aug 2018
The vitamin D receptor gene as a determinant of survival in pancreatic cancer patients: Genomic analysis and experimental validation.
PLoS One. 2018 Aug 14;13(8):e0202272. doi: 10.1371/journal.pone.0202272. eCollection 2018.
Innocenti F1, Owzar K2,3, Jiang C3, Etheridge AS1, Gordân R2, Sibley AB3, Mulkey F3, Niedzwiecki D3, Glubb D1, Neel N1, Talamonti MS4, Bentrem DJ5, Seiser E1, Yeh JJ1, Van Loon K6, McLeod H7, Ratain MJ8, Kindler HL8, Venook AP6, Nakamura Y8, Kubo M9, Petersen GM10, Bamlet WR10, McWilliams RR10.
PURPOSE:
Advanced pancreatic cancer is a highly refractory disease almost always associated with survival of little more than a year. New interventions based on novel targets are needed. We aim to identify new genetic determinants of overall survival (OS) in patients after treatment with gemcitabine using genome-wide screens of germline DNA. We aim also to support these findings with in vitro functional analysis.
PATIENTS AND METHODS:
Genome-wide screens of germline DNA in two independent cohorts of pancreatic cancer patients (from the Cancer and Leukemia Group B (CALGB) 80303 and the Mayo Clinic) were used to select new genes associated with OS. The vitamin D receptor gene (VDR) was selected, and the interactions of genetic variation in VDR with circulating vitamin D levels and gemcitabine treatment were evaluated. Functional effects of common VDR variants were also evaluated in experimental assays in human cell lines.
RESULTS:
The rs2853564 variant in VDR was associated with OS in patients from both the
Mayo Clinic ( HR 0.81 , 95% CI 0.70-0.94, p = 0.0059) and
CALGB 80303 ( HR 0.74 , 0.63-0.87, p = 0.0002).
rs2853564 interacted with high pre-treatment levels of 25-hydroxyvitamin D (25(OH)D, a measure of endogenous vitamin D) (p = 0.0079 for interaction) and with gemcitabine treatment (p = 0.024 for interaction) to confer increased OS. rs2853564 increased transcriptional activity in luciferase assays and reduced the binding of the IRF4 transcription factor.
CONCLUSION:
Our findings propose VDR as a novel determinant of survival in advanced pancreatic cancer patients. Common functional variation in this gene might interact with endogenous vitamin D and gemcitabine treatment to determine improved patient survival. These results support evidence for a modulatory role of the vitamin D pathway for the survival of advanced pancreatic cancer patients.
📄 Download the PDF from VitaminDWiki
Pancreatic Cancer Meta-analysis June 2017
Plasma 25-hydroxyvitamin D levels, vitamin D intake, and pancreatic cancer risk or mortality: a meta-analysis
Oncotarget. 2017 Jun 29. doi: 10.18632/oncotarget.18888.
Zhang X1, Huang XZ1, Chen WJ1, Wu J1, Chen Y2, Wu CC1, Wang ZN3.
📄 Download the PDF from VitaminDWiki
Pancreatic cancer MORTALITY
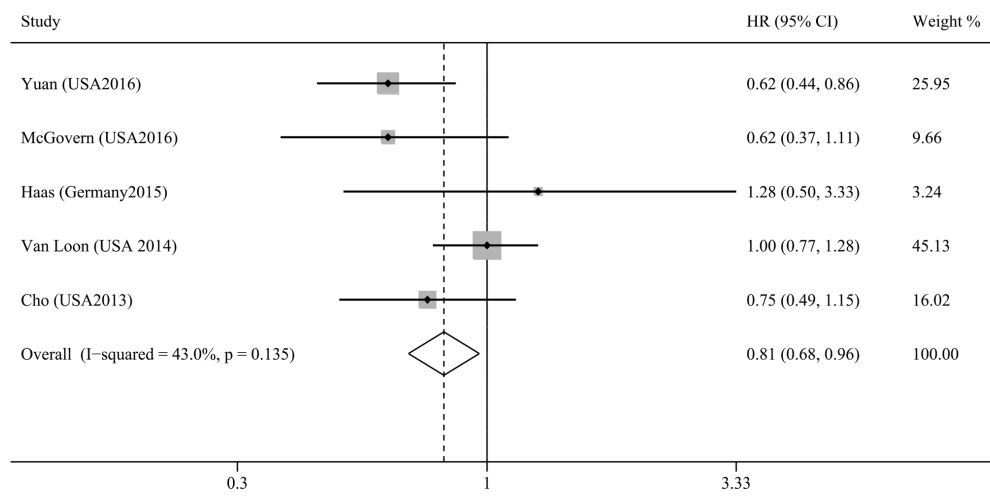
Pancreatic cancer INCIDENCE
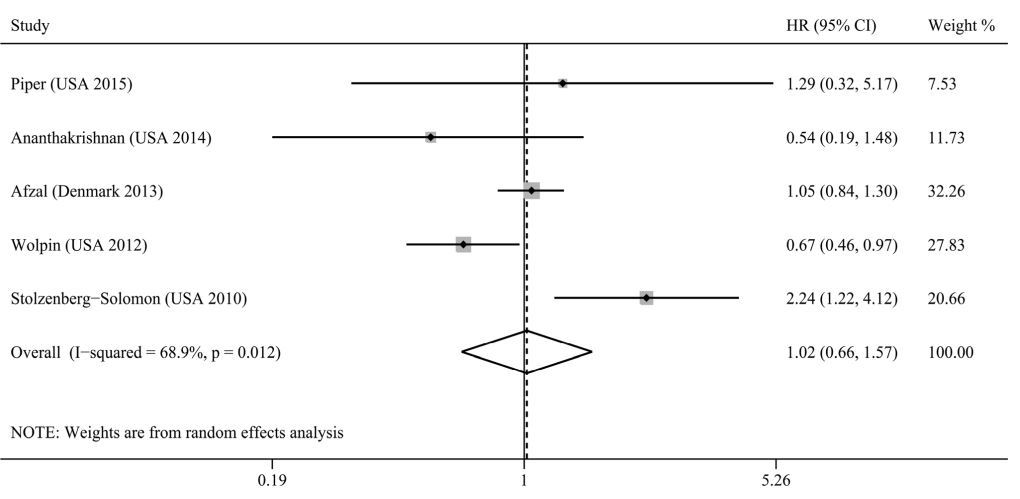
BACKGROUND:
The associations between vitamin D status, including plasma 25-hydroxyvitamin D [25(OH)D] levels and vitamin D intake, and pancreatic cancer risk and mortality are inconsistent. The aims of this study are to evaluate the antitumor and therapeutic effects of vitamin D status for pancreatic cancer patients.
METHODS:
A literature search for relevant studies was conducted using PubMed and Embase databases. Risk ratio (RR), hazard ratio (HR), and 95% confidence interval (CI) were used as the effect measures. All statistical analyses were performed using Stata software 12.0.
RESULTS:
Our results indicated that high plasma 25(OH)D levels were inversely associated with pancreatic cancer mortality without significant heterogeneity (HR=0.81, 95% CI=0.68-0.96). However, high plasma 25(OH)D levels could not reduce pancreatic cancer risk (RR=1.02, 95% CI=0.66-1.57). Moreover, vitamin D intake was also not associated with pancreatic cancer risk (RR=1.11, 95% CI=0.67-1.86)
Conclusions: Our results indicate that high plasma 25(OH)D levels were significantly associated with improved survival in pancreatic cancer patients. However, there were no significant associations between vitamin D intake or plasma 25(OH)D levels and pancreatic cancer risk.
PMID: 28733547 DOI: 10.18632/oncotarget.18888
