Medical use of antibiotics increased 36 percent globally in a decade
Global antibiotic consumption 2000 to 2010: an analysis of national pharmaceutical sales data
Lancet Aug 2014,. DOI: http://dx.doi.org/10.1016/S1473-3099(14)70780-7
Thomas P Van Boeckel, PhD, Sumanth Gandra, MD, Ashvin Ashok, MPP, Quentin Caudron, PhD, Prof Bryan T Grenfell, PhD, Prof Simon A Levin, PhD, Prof Ramanan Laxminarayan
 The TOP articles in Antibiotics, probiotics and Vitamin D are listed here:
{category}
The TOP articles in Antibiotics, probiotics and Vitamin D are listed here:
{category}
Increase use of antibiotics
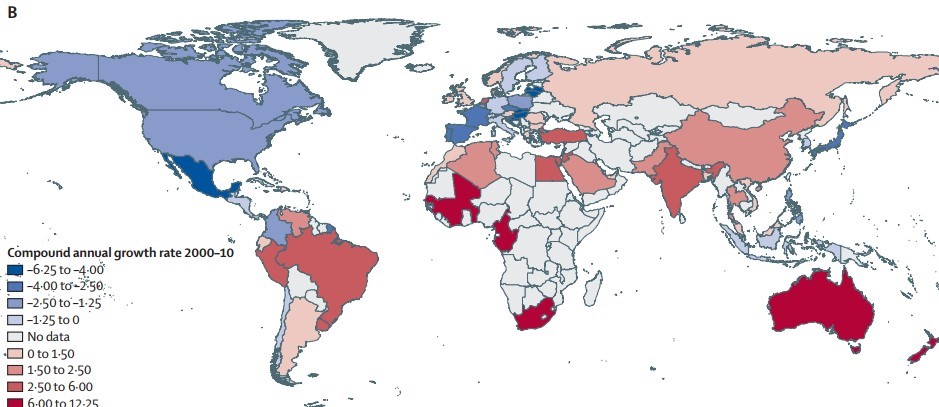
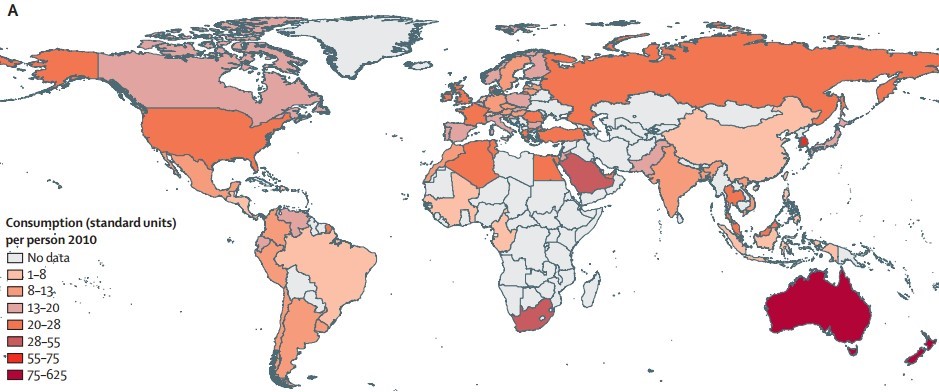
Use of antibiotics in 2010
Background
Antibiotic drug consumption is a major driver of antibiotic resistance. Variations in antibiotic resistance across countries are attributable, in part, to different volumes and patterns for antibiotic consumption. We aimed to assess variations in consumption to assist monitoring of the rise of resistance and development of rational-use policies and to provide a baseline for future assessment.
Methods
With use of sales data for retail and hospital pharmacies from the IMS Health MIDAS database, we reviewed trends for consumption of standard units of antibiotics between 2000 and 2010 for 71 countries. We used compound annual growth rates to assess temporal differences in consumption for each country and Fourier series and regression methods to assess seasonal differences in consumption in 63 of the countries.
Findings
Between 2000 and 2010, consumption of antibiotic drugs increased by 36% (from 54 083 964 813 standard units to 73 620 748 816 standard units). Brazil, Russia, India, China, and South Africa accounted for 76% of this increase. In most countries, antibiotic consumption varied significantly with season. There was increased consumption of carbapenems (45%) and polymixins (13%), two last-resort classes of antibiotic drugs.
Interpretation
The rise of antibiotic consumption and the increase in use of last-resort antibiotic drugs raises serious concerns for public health. Appropriate use of antibiotics in developing countries should be encouraged. However, to prevent a striking rise in resistance in low-income and middle-income countries with large populations and to preserve antibiotic efficacy worldwide, programmes that promote rational use through coordinated efforts by the international community should be a priority.
Funding
US Department of Homeland Security, Bill & Melinda Gates Foundation, US National Institutes of Health, Princeton Grand Challenges Program.
