Ischemic stroke 17 X more likely if low vitamin D
Vitamin D deficiency is associated with acute ischemic stroke, C-reactive protein, and short-term outcome.
Metab Brain Dis. 2017 Apr;32(2):493-502. doi: 10.1007/s11011-016-9939-2
Alfieri DF1, Lehmann MF2, Oliveira SR1, Flauzino T1, Delongui F1, de Araújo MC3, Dichi I4, Delfino VD4, Mezzaroba L5, Simão AN5, Reiche EM6.
Modified Rankin Scale (mRS) three-months later
The aim of this study was to investigate whether vitamin D deficiency (VDD) is associated with acute ischemic stroke, inflammatory markers, and short-term outcome. 168 acute ischemic stroke patients and 118 controls were included. The modified Rankin Scale (mRS) was applied up to 8 h of admission (baseline) and after three-months follow-up, and blood samples were obtained up to 24 h of admission to evaluate serum levels of 25-hydroxivitamin D [25(OH)D] and inflammatory markers. Vitamin D levels classified the individuals in sufficient (VDS ≥ 30.0 ng/mL), insufficient (VDI 20.0-29.9 ng/mL), and deficient (VDD < 20.0 ng/mL) status.
Patients had lower levels of 25(OH)D, higher frequency of VDD (43.45% vs. 5.08%, OR: 16.64 , 95% CI: 5.66-42.92, p < 0.001), and higher inflammatory markers than controls (p < 0.05).
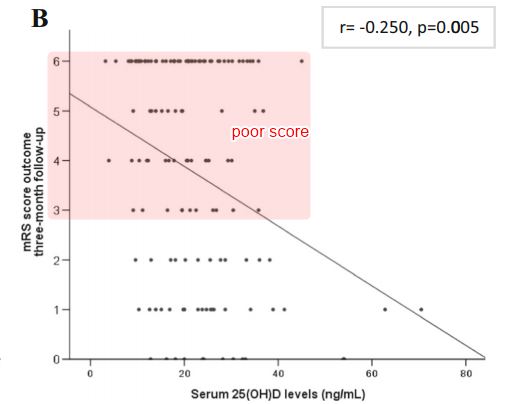
Patients with VDD showed increased high sensitivity C-reactive protein (hsCRP) levels than those with VDS status (p = 0.043); those with poor outcome presented with lower 25(OH)D levels than those with good outcome (p = 0.008); moreover, 25(OH)D levels were negatively correlated with mRS after three-months follow-up (r = -0.239, p = 0.005). The associations between VDD and higher hsCRP levels and between 25(OH)D levels and poor outcome at short-term in acute ischemic stroke patients suggest the important role of vitamin D in the inflammatory response and pathophysiology of this ischemic event.
📄 Download the PDF from VitaminDWiki
VitaminDWiki – Stroke category contains
{include}
Stroke Meta-analysis
{category}
23+ VitaminDWiki Stroke pages have ISCHEMIC OR ISCHAEMIC in the title
This list is automatically updated
{LIST()}

