Autistic teens have lower levels of vitamin D than siblings or parents
Vitamin D in the General Population of Young Adults with Autism in the Faroe Islands.
J Autism Dev Disord. 2014 Jun 14. [Epub ahead of print]
Kočovská E1, Andorsdóttir G, Weihe P, Halling J, Fernell E, Stóra T, Biskupstø R, Gillberg IC, Shea R, Billstedt E, Bourgeron T, Minnis H, Gillberg C.
1Gillberg Neuropsychiatry Centre, Institute of Neuroscience and Physiology, Sahlgrenska Academy, University of Gothenburg, Kungsgatan 12, 411 19, Göteborg, Sweden, eva.kocovska@gnc.gu.se.
Vitamin D deficiency has been proposed as a possible risk factor for developing autism spectrum disorder (ASD). 25-Hydroxyvitamin D3 (25(OH)D3) levels were examined in a cross-sectional population-based study in the Faroe Islands. The case group consisting of a total population cohort of 40 individuals with ASD (aged 15-24 years) had significantly lower 25(OH)D3 than their 62 typically-developing siblings and their 77 parents , and also significantly lower than 40 healthy age and gender matched comparisons. There was a trend for males having lower 25(OH)D3 than females. Effects of age, month/season of birth, IQ, various subcategories of ASD and Autism Diagnostic Observation Schedule score were also investigated, however, no association was found. The very low 25(OH)D3 in the ASD group suggests some underlying pathogenic mechanism.
PMID: 24927807
All groups had suboptimal vitamin D - the autistic teens had the lowest
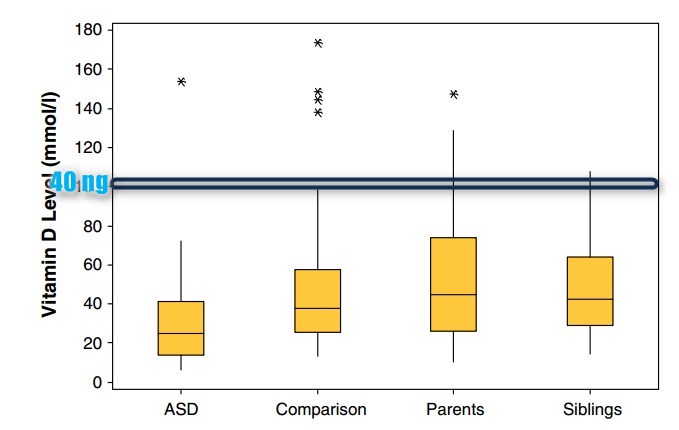
Matrix of vitamin D levels for each group
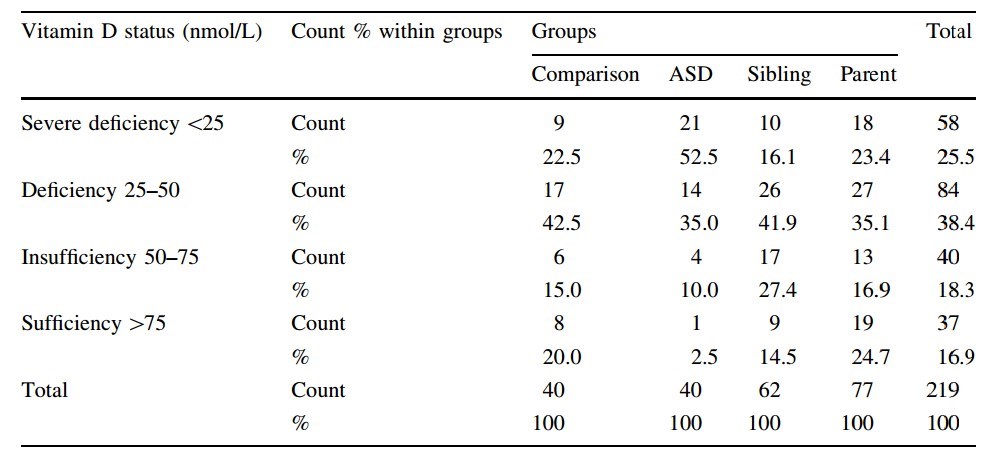
Discussion (extracted from PDF)
This first-ever population-based study of vitamin D in ASD showed significantly lower levels in young adolescents/ adults with ASD than in their siblings and parents, and also than healthy comparisons.
Our findings are consistent with those of several studies published since 2010, although some of these had methodological problems e.g., no comparison group or a problematic comparison group (Nseir et al. 2012; Kocovska et al. 2012a, b) (see Appendix).
The finding that 80 % of the comparison group (which can be considered representative of the general population in the Faroe Islands) were in the 'deficient/insufficient' range and 22.5 % in the 'severely deficient' range (<25 nmol/L-<10 ng/mL) that is indicative of the risk of osteomalacia/rickets (Holick 2007), adds to the mosaic of perceived global vitamin D deficiency in various regions of the world. It is of note that the levels of 25(OH)D3 found in ASD participants of the present study from the Faroe Islands are even lower than those in other regions (see Appendix). It might be that the severity of this region's climate and its high Northern latitude, both diminishing the production of vitamin D by UVB rays, cannot be compensated for by a diet albeit rich in large oily fish.
The only other report on vitamin D levels in the Faroe Islands was the Faroese elder study (Dalgard et al. 2010) that found the median 25(OH)D3 concentration of 47.6 (29.8-64.8) nmol/L and a small seasonal variation in the 25(OH)D3 levels in Faroese elders, with a winter nadir of 42.6 nmol/L and a summer peak of 56.5 nmol/L (females 51.0 nmol/L; males 44.6 nmol/L). Our study found a similarly small, insignificant seasonal variation in our ASD group corresponding to the season of blood sampling.
Unlike in the Meguid (2010) and Gong (2014) studies our group with the most severe diagnosis of autism had the highest levels of vitamin D (30.30 nmol/L; p = 0.3). This could be partially explained by the fact that 9 out of 11 individuals with autism diagnoses were blood sampled during the summer holidays while for the two other diagnoses there was a greater variability in season of sampling.
The slight over-representation of spring births among the ASD group (32.5 %) and corresponding lowest level of vitamin D in this group (median 13.8 nmol/L ; p = 0.17) is interesting and warrants follow up. A hypothetical explanation as to why ASD cases born in the spring had the lowest 25(OH)D3 status in adolescence could be that low maternal 25(OH)D3 levels led to epi-genetic processes at the CYP24A1 gene . This gene encodes the 24-hydroxylase that degrades calcitriol and 25(OH)D3 is subject to epigenetic regulation (methylation) during neonatal life (Novakovic et al. 2009): epi-genetic marking and silencing of the CYP24A1 gene could occur due to low maternal vitamin D levels preventing 25(OH)D3 from reaching a level that adequately supports CNS development. Further investigation of this potential mechanism may be of interest. To date the Faroese population generally has not been supplementing with vitamin D, even in pregnancy (apart from ordinary multivitamins with no more than 400 IU of cholecalciferol or ergoclaciferol per day), and the use of solaria in the Faroe Islands is also rare.
The trend towards lower levels of vitamin D in males in ASD and sibling groups presented another interesting finding. There are no acknowledged sun exposure differences between males and females among Faroese adolescents. Dalgard's Faroese elder study also reported that female gender was associated with higher 25(OH)D3 levels (Dalgard et al. 2010). Previous research has demonstrated various gender differences in vitamin D metabolism (Spach and Hayes 2005; Orton et al. 2006; Novakovic et al. 2009; Feldman et al. 2011). Thus, future research is warranted, as it would shed light on this phenomenon.
Here we only aimed at cross-sectional comparison of vitamin D levels and we did not investigate mechanisms involved in the differences found. It can be expected that both diet and availability of UVB rays can influence vitamin D levels. We did not measure calcium, parathyroid hormone (PTH), or phosphate, which might reveal more about the nature of the deficiency either from inadequate sun exposure and/or inadequate dietary intake (Holick 2007). An individual's underlying hormonal imbalance could also play a role (Cannell and Grant 2013; Holick 2007; Feldman et al. 2011). The apparatus regulating the hormone calcitriol (e.g. vitamin D receptors, vitamin D binding protein, associated enzymes) is all under genetic control and might exacerbate environmentally determined low vitamin D status or amplify its consequences to elevate ASD risk (Fu et al. 2009; Ahn et al. 2010; Hiraki et al. 2013). Thus future research is expected to shed light on a possible role of genetic factors. We intend to follow up and treat the diagnosed hypovitaminosis D among participants with ASD and try to obtain further information on the origin of low vitamin D status.
We have no evidence regarding the direction of causality as the blood samples of our ASD group were drawn when they were 15-24 years of age. The low vitamin D levels in the ASD group could be either a result of autism impacting on a family/child's lifestyle and/or diet (indoor activities, selective eater, etc.) or the underlying biology of autism altering the metabolism of vitamin D in some way or vitamin D deficiency itself contributing to the patho-genesis of ASD. As all groups were exposed to low levels of sunlight, the very low 25(OH)D3 in the ASD group suggests some other underlying pathogenic mechanism may be involved.
Children with Williams syndrome very often have high 25(OH)D3 levels in early infancy due to a single gene mutation, which also involves abnormal vitamin D metabolism (Feldman et al. 2011; Stamm et al. 2001). It would be interesting to explore whether altered vitamin D metabolism could also be involved in the development of autism. One of the supportive features for causality is biological mechanism (Hennekens et al. 1987).
High 'Body Mass Index' (BMI) has been associated with vitamin D deficiency (Holick 2007). We did not have exact BMI values available for either of our comparison groups. In our ASD group, eight participants (20 %) were noted by diagnosing clinicians as overweight/obese. Thus, this factor itself does not offer an exhaustive explanation for our overall result.
An increasing body of research indicates that ASD may be associated with a variety of complex immune dysregu-lations, including autoimmunity, and may have a neuro-immunecomponent (Cannell and Grant 2013; Mostafa and AL-Ayadhi 2012; Gentile et al. 2013). Thus, future investigation utilizing a combination of genetic, epigenetic, and mechanistic studies of this complex interplay between autism, vitamin D deficiency, steroid metabolism, and autoimmunity will be desirable.
Faroe Islands are just North of 60th latitude
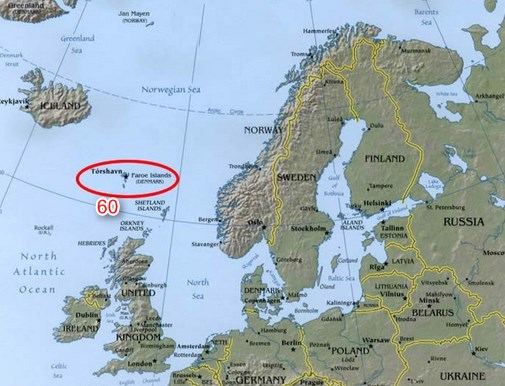
PDF is attached at the bottom of this page
See also VitaminDWiki
Most Autism Risk factors are associated with low vitamin D - March 2014
Autism treated by Vitamin D: Dr. Cannell - video June 2013 includes many reasons why he believes Autism is related to Vitamin D
{include}
