A woman who has ZERO Vitamin D in her blood, even with supplementation
Vitamin D–Binding Protein Deficiency and Homozygous Deletion of the GC Gene
March 21, 2019
N Engl J Med 2019; 380:1150-1157 DOI: 10.1056/NEJMoa1807841
Clark M. Henderson, Ph.D., Susan L. Fink, M.D., Ph.D., Hanan Bassyouni, M.D., Bob Argiropoulos, Ph.D., Lindsay Brown, Ph.D., Thomas J. Laha, M.T. (A.S.C.P.), Konner J. Jackson, B.S., Raymond Lewkonia, M.B., Ch.B., Patrick Ferreira, M.B., B.S., Andrew N. Hoofnagle, M.D., Ph.D., and Julien L. Marcadier, M.D.
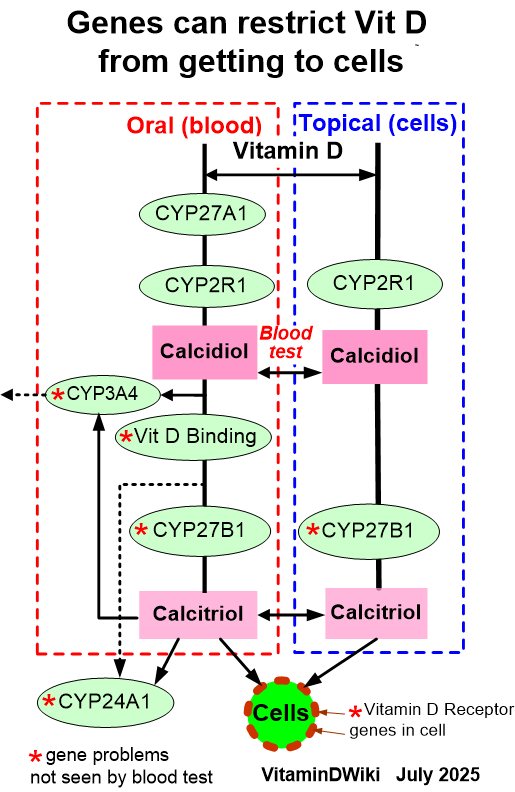 This study appears to be unaware of the right-hand pathway
---
1. See also VitaminDWiki
The following are cases where there is a poor Vitamin D binding protein
The woman has an extreme case, ZERO VDBP
* Vitamin D Binding Protein category listing has ** items *
* Poor Vitamin D response 4X more likely if poor Vitamin D binding proteins - July 2019
* Vitamin D Nutrigenomics - High, Medium, and Low Responders - March 2019
* Poor Vitamin D binding had 30 percent less response to Vitamin D (50,000 IU weekly) – Feb 2019
* Vitamin D and critical illness – many questions and unknowns (DBP etc)– Dec 2018
* Ear infections in children 3X more likely if poor vitamin D binding protein – July 2018
* Response to Vitamin D varies with Vitamin D Binding Protein gene – RCT May 2018
* Hypothesis – Bipolar disorder diagnose based on results of vitamin D-binding protein test – March 2018
This study appears to be unaware of the right-hand pathway
---
1. See also VitaminDWiki
The following are cases where there is a poor Vitamin D binding protein
The woman has an extreme case, ZERO VDBP
* Vitamin D Binding Protein category listing has ** items *
* Poor Vitamin D response 4X more likely if poor Vitamin D binding proteins - July 2019
* Vitamin D Nutrigenomics - High, Medium, and Low Responders - March 2019
* Poor Vitamin D binding had 30 percent less response to Vitamin D (50,000 IU weekly) – Feb 2019
* Vitamin D and critical illness – many questions and unknowns (DBP etc)– Dec 2018
* Ear infections in children 3X more likely if poor vitamin D binding protein – July 2018
* Response to Vitamin D varies with Vitamin D Binding Protein gene – RCT May 2018
* Hypothesis – Bipolar disorder diagnose based on results of vitamin D-binding protein test – March 2018
A 58-year-old woman with debilitating ankylosing spondylitis who was born to consanguineous parents was found to have an apparent severe vitamin D deficiency that did not respond to supplementation . Liquid chromatography–tandem mass spectrometry showed the absence of circulating vitamin D–binding protein, and chromosomal microarray confirmed a homozygous deletion of the group-specific component (GC) gene that encodes the protein. Congenital absence of vitamin D–binding protein resulted in normocalcemia and a relatively mild disruption of bone metabolism, in this case complicated by severe autoimmune disease.
(Funded by the National Institutes of Health and the University of Washington.)
Part of the description at Medical Express
First case of person without the protein needed to transport vitamin D identified
"The idea has always been that without its binding protein, vitamin D couldn't get to the cells where it's needed. Our findings call that into question," says Dr. Julien Marcadier, MD, a clinical assistant professor in the departments of medical genetics and paediatrics at the Cumming School of Medicine and senior author of the paper. "To our surprise, she's maintained normal calcium levels despite having no measurable vitamin D. This tells us that the vitamin D she has in her system does in fact get to its target cells, though how exactly that happens is still unknown."
This is the first reported case of a human without vitamin D binding protein. The woman, who does not wish to be identified, is now taking vitamin D at a dose of 2,000 IU per day and has not suffered any recent fractures. She continues to work with her health-care team as they try to better understand the role of vitamin D binding protein.
