Oral Vitamin D, the lung microbiome and Tuberculosis
The lung microbiome, vitamin D, and the tuberculous granuloma: A balance triangle
Microbial Pathogenesis, Volume 131, June 2019, Pages 158-163. https://doi.org/10.1016/j.micpath.2019.03.041
📄 Download the PDF from Sci-Hub via VitaminDWiki
Highlights
Granuloma formation in tuberculosis involves multiple cell interactions which are affected by commensals in the lung.
It is possible that lung microbiota changes could affect tuberculous granuloma dynamics.
VD plays a key role in the immune response to Mtb, granuloma formation, and intestinal and lung microbiome modulation.
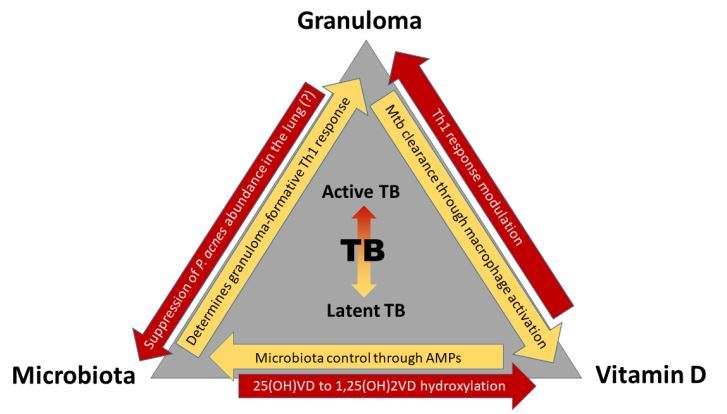
These three variables interact with each other in TB, determining the outcome of infection and progression of disease.
Mycobacterium tuberculosis (Mtb) has the extraordinary ability to persist for decades within granulomas in the human host. These histopathological structures involved in both protection and pathogenesis, are subject to various influences from the host systemically and through micro-niche environments. Despite the fact that vitamin D (VD) has a key role in macrophage activation and mycobacterial clearance in the early stages of Mtb infection, the overall role of VD in granuloma maintenance or functionality has been scarcely studied. VD deficiency has long time been known to influence on gut microbiota composition, and recent studies have shown that it can also impact on respiratory microbiome. The human microbiota plays an important role in pathogen colonization resistance, and it has been proposed to play a potential role in TB pathogenesis.
In this article, we have reviewed current knowledge on the interaction between VD, the lung microbiome and TB, and propose mechanisms by which the tuberculous granuloma's outcome could be modulated by these two factors. The determinants of the final fate of lung granulomas are still unclear, and deciphering the underlying drivers of Mtb infection outcome within those structures is of critical importance.
