Hypothesis: A hospital diarrhea epidemic caused vitamin D deficiency
Vitamin D deficiency: A potential risk factor for Clostridium difficile infection
This article was published in the following Dove Press journal: Risk Management and Healthcare Policy 5 October 2012
Dima Youssef 1 William B Grant 2 Alan N Peiris 3,4
1 Department of Internal Medicine, Division of Infectious Diseases,
2 Sunlight, Nutrition and Health Research Center, San Francisco, CA USA;
3 Department of Medicine, Mountain Home VAMC,
4 Department of Medicine, East Tennessee State University, Johnson City, Tennessee, USA
In the July 3, 2012 issue of the journal of Risk Management and Healthcare Policy, Martinez et al present a nice review on Clostridium difficile (C. difficile) infections.1 The different manifestations of this challenging disease along with the high cost and burden on the health care system were discussed. While the authors did an admirable job in discussing traditional risk factors, they do not mention vitamin D deficiency.
Vitamin D deficiency has reached a pandemic status.2 Vitamin D has an important role in boosting the innate immunity, and thus preventing infections.3 We have recently reviewed the potential role of vitamin D in the prevention of hospital acquired infections.4 In a veterans study, vitamin D deficiency in patients with C. difficile was associated with significantly increased total costs and fee-based consultation. The deficient patients had five times higher costs than the non-deficient patients.5 Most cells have vitamin D receptors and vitamin D has a plethora of actions leading to boosting innate immunity including increased oxidative burst of macrophages and enhancing neutrophil motility and phagocytic function, T cell activation and increased expression of antimicrobial peptides, such as cathelicidin, and beta-defensins. While awaiting additional confirmatory studies of the antimicrobial effects of vitamin D, there are sufficient benefits including better intensive care unit outcomes,6 for the authors to include a vitamin D replete state as a part of their therapeutic approach. Vitamin D is inexpensive and has the potential to tilt the balance in favor of patients with this devastating infection.
Acknowledgments
This material is the result of works supported with resources and the use of facilities at the Mountain Home VAMC. The contents of this report do not reflect the position of the US government and the Department of Veterans Affairs.
Correspondence: Dima Youssef Quillen College of Medicine, East Tennessee State University, Department of Internal Medicine, Division of Infectious Diseases, Box 70622, VAMC Bldg Dogwood Ave, Johnson City, TN 37614, USA Email estecina@hotmail.com
Disclosure
WBG receives funding from the UV Foundation (McLean, VA), Bio-Tech Pharmacal (Fayetteville, AR), the Vitamin D Council (San Luis Obispo, CA), the Vitamin D Society (Canada), and the Sunlight Research Forum (Veldhoven).
References
Martinez FJ, Leffler DA, Kelly CP. Clostridium difficile outbreaks: prevention and treatment strategies. RiskManagHealthc Policy. 2012;5:55-64. (PDF attached at bottom of this page)
Holick MF. Vitamin D deficiency. NEngl J Med. 2007;357(3):266-281.
Youssef DA, Miller CW, El-Abbassi AM, et al. Antimicrobial implications of vitamin D. Dermatoendocrinol. 2011;3(4):220-229. On-line full text
Youssef D, Ranasinghe T, Grant WB, Peiris AN. Vitamin D's potential to reduce the risk of hospital-acquired infections. Dermatoendocrinol. Apr/May/Jun 2012;4(2):1-9. In VitaminDWiki
Youssef D, Bailey B, El Abbassi A, et al. Healthcare costs of Staphylococcus aureus and Clostridium difficile infections in veterans: role of vitamin D deficiency. Epidemiol Infect. 2010;138(9):1322-1327.
Matthews LR, Ahmed Y, Wilson KL, Griggs DD, Danner OK. Worsening severity of vitamin D deficiency is associated with increased length of stay, surgical intensive care unit cost, and mortality rate in surgical intensive care unit patients. Am J Surg. 2012;1(204):37—43.
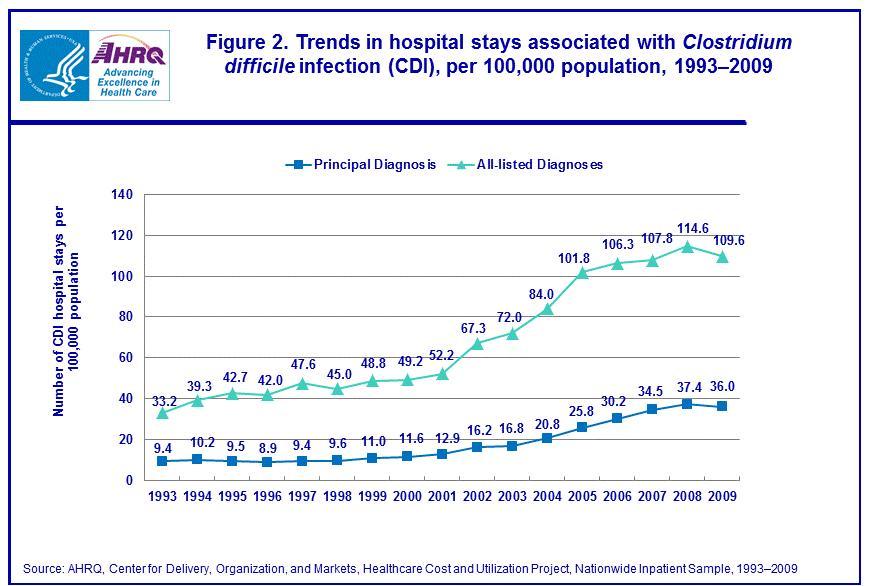
AHRQ graph shows the extent of the epidemic
Almost 4X increase
CDI dot COM
People in good health usually do not get CDI. Increased risk is associated with:
Prolonged use of broad spectrum antibiotics such as cephalosporins and clindamycin
Advanced age (Usually over 65)
Gastrointestinal surgery
Immunologically compromised
See also VitaminDWiki
Superbug (Clostridium difficile) 4.7X more of a problem if low vitamin D – Sept 2013
How to reduce hospital infections with vitamin D – April 2012 David McCarthy
ICU surgical patients with low vitamin D stayed longer and had more sepsis – Dec 2011
Vitamin D's potential to reduce the risk of hospital-acquired infections – May 2012
Staph infection reduced 50 percent when have more than 30 ng of vitamin D – Aug 2011
Septic patients vitamin D so low that small changes did not matter – June 2011
VA found less testing for vitamin D resulted in increased health costs – Jan 2012
Vitamin D might reduce military costs for UC and CD – June 2011
Superbug (Clostridium difficile) Infections strongly associated with low vitamin D - many studies
Hospital stay 6 days longer for nursing home residents with low vitamin D – Oct 2011
