How to predict response to a vitamin D dose – RCT
Environmental, personal and genetic determinants of response to vitamin D supplementation in older adults
J of Clinical Endocrenology and Metabolism, DOI: http://dx.doi.org/10.1210/jc.2013-4101, Published Online: April 02, 2014
Mary Waterhouse 1, Bich Tran12, Bruce K Armstrong3, Catherine Baxter1, Peter R Ebeling24, Dallas R English5, Val Gebski6, Christine Hill1, Michael G Kimlin27, Robyn M Lucas8, Alison Venn9, Penelope M Webb1, David C Whiteman12, and Rachel E Neale12
1Population Health Division, QIMR Berghofer Medical Research Institute;
2Centre for Research Excellence in Sun and Health;
3Sydney School of Public Health, University of Sydney;
4University of Melbourne and Western Health, Victoria;
5 Melbourne School of Population and Global Health, University of Melbourne and Cancer Epidemiology Centre, Cancer Council Victoria;
6NHMRC Clinical Trials Centre, Sydney Medical School, University of Sydney;
7AusSun Research Laboratory, Queensland University of Technology;
8National Centre for Epidemiology and Population Health, The Australian National University;
9Menzies Research Institute Tasmania.
Context and Objective:
Suboptimal vitamin D status can be corrected by vitamin D supplementation, but individual responses to supplementation vary. We aimed to examine genetic and non-genetic determinants of change in serum 25-hydroxyvitamin D [25(OH)D] following supplementation.
Design and participants:
We used data from a pilot randomised controlled trial in which 644 adults aged 60–84 years were randomly assigned to monthly doses of placebo, 30,000 IU, or 60,000 IU vitamin D3 for 12 months. Baseline characteristics were obtained from a self-administered questionnaire. Eighty-eight single nucleotide polymorphisms (SNPs) in 41 candidate genes were genotyped using Sequenom MassArray technology. Serum 25(OH)D levels before and after the intervention were measured using the Diasorin Liaison platform immunoassay. We used linear regression models to examine associations between genetic and non-genetic factors and change in serum 25(OH)D levels.
Results:
Supplement dose and baseline 25(OH)D level explained 24% of the variability in response to supplementation. BMI, self-reported health status and ambient UVR made a small additional contribution. SNPs in CYP2R1, IRF4, MC1R, CYP27B1, VDR, TYRP1, MCM6 and HERC2 were associated with change in 25(OH)D level, although only CYP2R1 was significant after adjustment for multiple testing. Models including SNPs explained a similar proportion of variability in response to supplementation as models that included personal and environmental factors.
Conclusion:
Stepwise regression analyses suggest that genetic variability may be associated with response to supplementation, perhaps suggesting that some people might need higher doses to reach optimal 25(OH)D levels, or that there is variability in the physiologically normal level of 25(OH)D.
Summary VitaminDWiki
RCT used 30,000 or 60,000 IU monthly (which is not much) for 12 months
Tried to model the blood response to the dose which was given
Considered baseline blood level, genes, BMI, Health status, UltraViolet/Sunshine
Failed to consider such things as
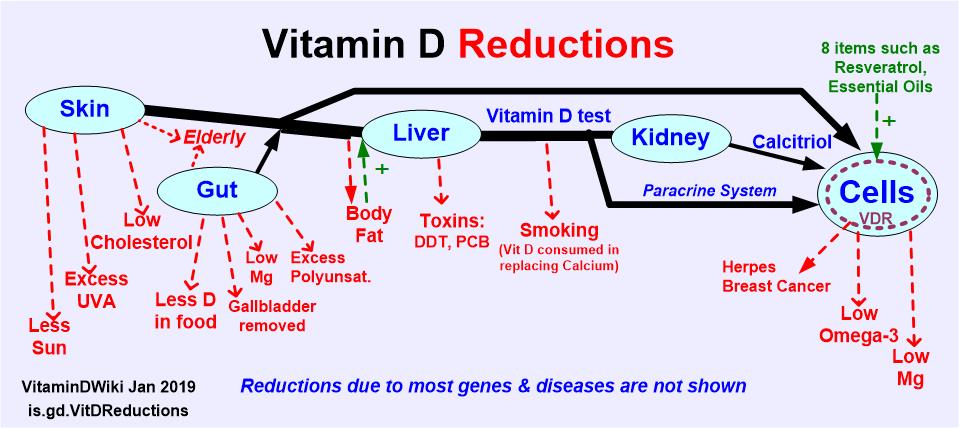
Skin color which reduces UV benefit
Low cholesterol in diet, so not as much benefit from UV/sunshine
Excess toxins such as DDT, PCB, Alcohol
Health problems which consume Vitamin D
Health problems which reduce the response of Vitamin D consumed
- Especially problems of the Liver and Kidney
Cofactors such as Magnesium and Omega-3
What time of day the vitamin D was taken
What was eaten with the vitamin D
Amount of Vitamin A in diet (too much vitamin A blocks vitamin D)
There are much better indicators of obesity than BMI
Smoking – known to reduce dose/response by 20%
Amount of vitamin D in diet: 6X more vitamin D in animal products than previously realized
Recent surgery/trauma – which consumes a lot of vitamin D
Drugs being taken which reduce vitamin D levels - statins, chemotherapy, etc.
Depression
Get a lot of sunshine thru a window (UVA distroys some Vitamin D created by UVB)
See also VitaminDWiki
Gut-Friendly Vitamin D far better dose response for those with poor guts
Increasing the ratio of mono to poly fats increased Vitamin D levels by 6 ng – RCT Aug 2011
Model has 80 percent chance of predicting vitamin D levels to within 10 ng – Feb 2012
Response to vitamin D dose, overview of 25 studies - Feb 2014 with summary chart
Vitamin D reduced so low that Victorian age diseases are returning which has the following chart