Independent and Synergistic Associations of Biomarkers of Vitamin D Status With Risk of Coronary Heart Disease
Arteriosclerosis, Thrombosis, and Vascular Biology. 2017;37:2204-2212, Sept 7, 2017, https://doi.org/10.1161/ATVBAHA.117.309548
Lu Qi, Wenjie Ma, Yoriko Heianza, Yan Zheng, Tiange Wang, Dianjianyi Sun, Eric B. Rimm, Frank B. Hu, Edward Giovannucci, Christine M. Albert, Kathryn M. Rexrode, JoAnn E. Manson
Poor Vitamin D Binding Protein is more associated with dark skin than Heart Disease
Wonder how many of the participants in this study had dark skin
- Vitamin D-binding protein and vitamin D status of black Americans and white Americans – Nov 2013
- Bioavailable Vitamin D is the same blacks and whites, but measured vit D is not – Oct 2014
- Blacks have lower vitamin D levels, but OK active vitamin D levels (VDBP) - Feb 2015
Cardiovascular category listing has 507 items along with related searches
Genetics category listing contains the following
332 articles in the Genetics category
see also
- Vitamin D Receptor has
512 items
- Vitamin D Binding Protein = GC has
176 items
- CYP27B1 has
60 items
- CYP24A1 in title of 34+ items
- CYP2R1 25+ items
- Calcidiol has
46 items
- Calcitriol has
56 items
- Topical Vitamin D
- Nanoemulsion Vitamin D may be a substantially better form
- 1289 genes changed with higher doses of Vitamin D - RCT Dec 2019
- CYP3A4 (7 as of Dec 2022)
- Getting Vitamin D into your body

Vitamin D blood test misses a lot
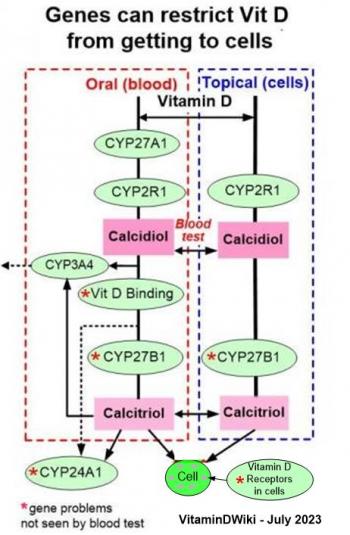
- Vitamin D from coming from tissues (vs blood) was speculated to be 50% in 2014, and by 2017 was speculated to be 90%
- Note: Good blood test results (> 40 ng) does not mean that a good amount of Vitamin D actually gets to cells
- A Vitamin D test in cells rather than blood was feasible (2017 personal communication) Commercially available 2019
- However, test results would vary in each tissue due to multiple genes
- Good clues that Vitamin D is being restricted from getting to the cells
1) A vitamin D-related health problem runs in the family
especially if it is one of 51+ diseases related to Vitamin D Receptor
+2) Slightly increasing Vitamin D shows benefits (even if conventional Vitamin D test shows an increase)
+3) DNA and VDR tests - 120 to 200 dollars $100 to $250
+4) PTH bottoms out ( shows that parathyroid cells are getting Vitamin d)
Genes are good, have enough Magnesium, etc.
+4) Back Pain
probably want at least 2 clues before taking adding vitamin D, Omega-3, Magnesium, Resveratrol, etc
- The founder of VitaminDWiki took action with clues #3&4
See also PubMed
- Race and Vitamin D Binding Protein Gene Polymorphisms Modify the Association of 25-Hydroxyvitamin D and Incident Heart Failure: The ARIC (Atherosclerosis Risk in Communities) Study. May 2015 free PDF online
- Impact of polymorphism rs7041 and rs4588 of Vitamin D Binding Protein on the extent of coronary artery disease Sept 2017, Results were not statistically significant
Objective—To comprehensively evaluate the independent associations and potential interactions of vitamin D–related biomarkers including total and bioavailable 25-hydroxyvitamin D (25OHD), VDBP (vitamin D binding protein), and parathyroid hormone (PTH) with risk of coronary heart disease (CHD).
Approach and Results—We prospectively identified incident cases of nonfatal myocardial infarction and fatal CHD among women in the Nurses’ Health Study during 20 years of follow-up (1990–2010). Using risk-set sampling, 1 to 2 matched controls were selected for each case. The analysis of 25OHD and PTH included 382 cases and 575 controls; the analysis of VDBP included 396 cases and 398 controls. After multivariate adjustment, plasma levels of total 25OHD, bioavailable 25OHD, and PTH were not significantly associated with CHD risk.
VDBP was associated with a lower CHD risk with an extreme-quartile odds ratio of 0.60 (95% confidence interval, 0.39–0.92; P trend=0.02). When examining the biomarkers jointly, a significant, inverse association between 25OHD and CHD was observed among participants with higher PTH levels (P for interaction=0.02).
The odds ratio (95% confidence interval) comparing the highest quartile of 25OHD to lowest was 0.43 (0.23–0.82; P trend=0.003) when PTH levels were above population median (35.3 pg/mL), whereas among the rest of participants the corresponding odds ratio (95% confidence interval) was 1.28 (0.70–2.36; P trend=0.43).
Conclusions—Our data suggest that higher 25OHD levels were associated with a lower CHD risk when PTH levels were high, whereas no association was observed for participants with low PTH levels. VDBP but not bioavailable 25OHD was independently associated with lower CHD risk.
Publisher wants $35 for the PDF
Heart Disease 40 percent more likely in women having poor Vitamin D Binding Protein – Sept 2017
4001 visitors, last modified 26 Oct, 2017,
Printer Friendly
Follow this page for updates
This page is in the following categories (# of items in each category)
Genetics category listing contains the following
see also
- Vitamin D Receptor has
512 items - Vitamin D Binding Protein = GC has
176 items - CYP27B1 has
60 items - CYP24A1 in title of 34+ items
- CYP2R1 25+ items
- Calcidiol has
46 items - Calcitriol has
56 items - Topical Vitamin D
- Nanoemulsion Vitamin D may be a substantially better form
- 1289 genes changed with higher doses of Vitamin D - RCT Dec 2019
- CYP3A4 (7 as of Dec 2022)
- Getting Vitamin D into your body
Vitamin D blood test misses a lot
- Vitamin D from coming from tissues (vs blood) was speculated to be 50% in 2014, and by 2017 was speculated to be 90%
- Note: Good blood test results (> 40 ng) does not mean that a good amount of Vitamin D actually gets to cells
- A Vitamin D test in cells rather than blood was feasible (2017 personal communication) Commercially available 2019
- However, test results would vary in each tissue due to multiple genes
- Good clues that Vitamin D is being restricted from getting to the cells
1) A vitamin D-related health problem runs in the family
especially if it is one of 51+ diseases related to Vitamin D Receptor
+2) Slightly increasing Vitamin D shows benefits (even if conventional Vitamin D test shows an increase) +3) DNA and VDR tests - 120 to 200 dollars $100 to $250 +4) PTH bottoms out ( shows that parathyroid cells are getting Vitamin d)Genes are good, have enough Magnesium, etc.
+4) Back Painprobably want at least 2 clues before taking adding vitamin D, Omega-3, Magnesium, Resveratrol, etc
- The founder of VitaminDWiki took action with clues #3&4
See also PubMed
- Race and Vitamin D Binding Protein Gene Polymorphisms Modify the Association of 25-Hydroxyvitamin D and Incident Heart Failure: The ARIC (Atherosclerosis Risk in Communities) Study. May 2015 free PDF online
- Impact of polymorphism rs7041 and rs4588 of Vitamin D Binding Protein on the extent of coronary artery disease Sept 2017, Results were not statistically significant
Objective—To comprehensively evaluate the independent associations and potential interactions of vitamin D–related biomarkers including total and bioavailable 25-hydroxyvitamin D (25OHD), VDBP (vitamin D binding protein), and parathyroid hormone (PTH) with risk of coronary heart disease (CHD).Approach and Results—We prospectively identified incident cases of nonfatal myocardial infarction and fatal CHD among women in the Nurses’ Health Study during 20 years of follow-up (1990–2010). Using risk-set sampling, 1 to 2 matched controls were selected for each case. The analysis of 25OHD and PTH included 382 cases and 575 controls; the analysis of VDBP included 396 cases and 398 controls. After multivariate adjustment, plasma levels of total 25OHD, bioavailable 25OHD, and PTH were not significantly associated with CHD risk.
VDBP was associated with a lower CHD risk with an extreme-quartile odds ratio of 0.60 (95% confidence interval, 0.39–0.92; P trend=0.02). When examining the biomarkers jointly, a significant, inverse association between 25OHD and CHD was observed among participants with higher PTH levels (P for interaction=0.02).
The odds ratio (95% confidence interval) comparing the highest quartile of 25OHD to lowest was 0.43 (0.23–0.82; P trend=0.003) when PTH levels were above population median (35.3 pg/mL), whereas among the rest of participants the corresponding odds ratio (95% confidence interval) was 1.28 (0.70–2.36; P trend=0.43).Conclusions—Our data suggest that higher 25OHD levels were associated with a lower CHD risk when PTH levels were high, whereas no association was observed for participants with low PTH levels. VDBP but not bioavailable 25OHD was independently associated with lower CHD risk.
Publisher wants $35 for the PDF
Heart Disease 40 percent more likely in women having poor Vitamin D Binding Protein – Sept 2017Printer Friendly Follow this page for updates4001 visitors, last modified 26 Oct, 2017, This page is in the following categories (# of items in each category) - Vitamin D Binding Protein = GC has